Research - (2021) Volume 9, Issue 6
A Comparative Study of Suicidal Behavior in Adolescents and Adults Attending Psychiatry OPD in a Tertiary Care Hospital
*Correspondence: S Nambi, Department of Psychiatry, Sree Balaji Medical College & Hospital Affiliated to Bharath Institute of Higher Education and Research, India, Email:
Abstract
Suicidal behaviors are thoughts or tendencies that put a person at higher risk of committing suicide. It is an act of intentionally terminating one’s own life. To study the intent of suicide in adults and adolescents based on the socioeconomic status, on the abuse of substances. To study the intent of suicide in adults and adolescents based on any psychiatric illness, and the severity of the disorder. To study the suicidal behavior in adults and adolescents based on the history of deliberate self-harm. To compare the results between the two group.
Keywords
Suicidal behavior, Adolescents, Psychiatry, OPD.
Introduction
Human destructive behavior has many determinants. In considering animal models of human behaviour, one cannot propose that similar behaviors necessary have the same causation in human being. Human suicidal behavior has always been a source of dread and wonder to mankind. All suicidal people are not death seekers. Some attempt to communicate pain, to reduce isolation, to avoid consequences of social status change, seek revenge, and convey a whole lot of other meaning which are essentially individualistic. Suicide is a major health problem, with a far reaching socioeconomic, political, and emotional consequences. Southeast Asia accounts for roughly 40% of the estimated 800000 annual suicidal deaths [1].
In India suicide has more death than AIDS related (62000 in 2016) and maternal death (4500 in 2015) [2,3]. Historically, Ramayana and Mahabharata have recorded instances of suicide.
Suicidal behaviors as such are classified into three categories: suicidal ideation, suicide plan or intent and suicide attempts. As per Data from World Health Organization indicated that approximately one million people worldwide die by suicide each year. This corresponds to one death every 40 by suicide. The Suicide attempts and suicidal ideation are far more common. The number of suicides attempts, exceeds by 20 times the number of deaths by suicide.
According to WHO, an estimate for the year 2020, approximately 1.53 million people will die by suicide and10 to 20 times more people will attempt suicide worldwide. These estimates represent on average one death every 20 s and one attempt every one to two seconds.
According to World Health Organization (WHO) and the Latest Burden of Disease Estimation, suicide is a major public health problem in highincome countries and is an emerging problem in low as well as middle-income countries where poor psychiatric services are available. The global rate of suicide is estimated to be 11.6 per 100,000 inhabitants per year. Suicide accounts for 1.4% of total mortality and 15% of injury mortality [1,2].
Suicide rates have increased by an alarming 60% over the last 50 years and the increase has been particularly marked in developing countries. As a whole people with a mental illness face statistically higher risk of suicide. Although it is generally accepted that, 10% of people with mental illness commit suicide during their lifetime and approximately 90 percent of suicide cases meet criteria for psychiatric disorders, particularly major depression, substance use disorders, cluster B personality disorders and schizophrenia, most of them can be either extended or are even preventable.
Although much research showed suicide and suicidal behaviors are more common in high income countries, it is also increasing currently in low- and middle-income countries because of various reasons. Suicide and suicidal behaviors are higher in those who are divorced/separated/ widowed, being female, younger, single, and less educated. Complete suicide is more common in males whereas nonfatal suicidal behaviors are more common among females.
Among mental disorders, major depressive disorder is the strongest predictors of suicide and suicidal behaviors. The other mental disorders like schizophrenia, bipolar disorders, and anxiety disorders are risk factors for suicidal behaviors. Substance use disorders and substance co- morbidity are also the predictors of suicide and suicidal behaviors. From substance use disorders; alcohol use disorders, tobacco and other illicit drug use and cigarette smoking are the predictors of suicide and suicidal behaviors.
It has been suggested that the annual suicide rate could be 6 to 9 times the official rate. There has been less work in systemic profiling of risk factor in developing countries compared to the developed counterparts.
Materials and Methods
30 adults and 30 adolescents attending the outpatient department in the Department of Psychiatry, and also patient referred from Intensive Care Unitin SBMCH.
Cross sectional descriptive study done with outpatient attending SBMCH psychiatry department as well as those referred from ICU. A sample of 60 patients (30 adolescent and 30 adult) screened for various psychiatric diagnosis as per the ICD 10 and suicidal behavior, detailed assessment, and comparison of suicidal behavior. After getting the informed consent, the socio demographic and clinical details are taken down as according to the semi structured proforma developed especially for this study.
The patients are administered the following scales:
✓ GHQ.
✓ HAMD.
✓ 3BECK’S suicidal intentscale.
Results and Discussion
All parameters were compared between adults and adolescents.
Descriptive analysis: Descriptive analysis was carried out by mean and standard deviation for quantitative variables, frequency, and proportion for categorical variables. Data was also represented using appropriate diagrams like bar diagram, pie diagram and boxplots.
The association between marital status, SES, prevalence of depression, GHQ, suicidal intent, medical co morbidities and adults/adolescents was assessed by cross tabulation and comparison of percentages. Chi square test was used to test statistical significance. P value<0.05 was considered statistically significant. IBM SPSS version 22 was used for statistical analysis (Figure 1).
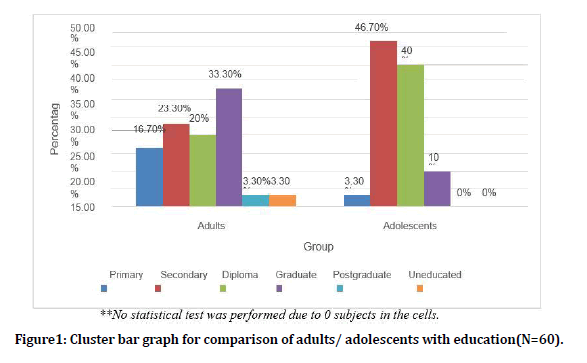
Figure 1. Cluster bar graph for comparison of adults/ adolescents with education(N=60).
Socio economic status
Among the adults 14 (46.7%) belonged to Lower middle, 10 (33.3%) belonged to upper middle, 5 (16.7%) belonged to upper, 1 (3.3%) belonged to lower socio-economic status. Among the adolescents 16(53.3%) belonged to lower middle, 13 (43.3%) belonged to upper middle and only one subject belonged to working class (Figure2).
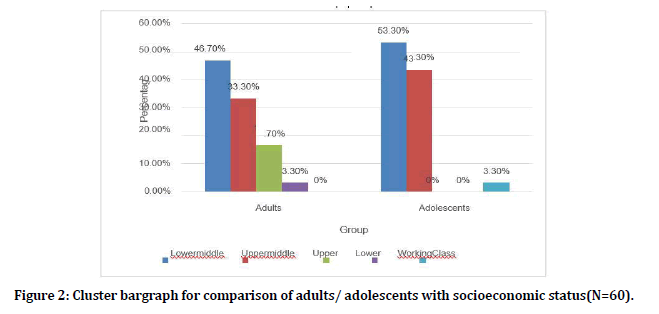
Figure 2. Cluster bargraph for comparison of adults/ adolescents with socioeconomic status(N=60).
Past psychiatry history
The data were collected with history from patients and family members. Among the adults 12 (40%) had past psychiatry history. Among the adolescents 7 (23.3%) had Past psychiatry history. The difference between past psychiatry history and group was statistically not significant. (P value 0.165) (Figure3).
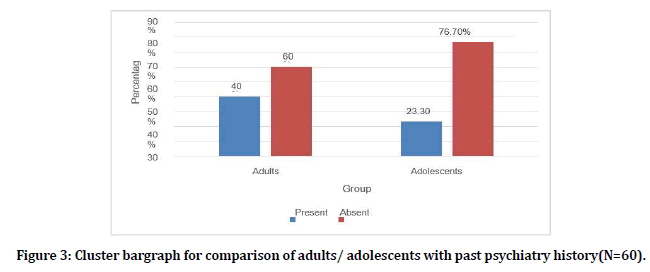
Figure 3. Cluster bargraph for comparison of adults/ adolescents with past psychiatry history(N=60).
Substance use/abuse
Among the adults6 (20.0%) were used Alcohol, 4 (13.3%) were used Alcohol/ nicotine, 1 (3.3%) were used Cannabis/ alcohol, 2 (6.7%) used nicotine. Among the adolescents 1 (3.3%) used Alcohol/ nicotine, 1 (3.3%) used Cannabis, 1 (3.3%) used Heroin, cannabis and 6 (20.0%) used Nicotine (Figure 4).
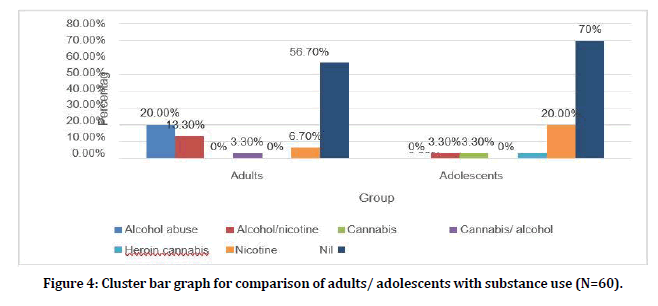
Figure 4. Cluster bar graph for comparison of adults/ adolescents with substance use (N=60).
Among the adults 8 (26.7%) were deliberated to self- harm. Among the adolescents 11 (36.7%) was deliberated to self-harm. There was no statistically significant difference indeliberate self-harm present between adults and adolescents. (P value 0.405) (Figures 5 and 6).
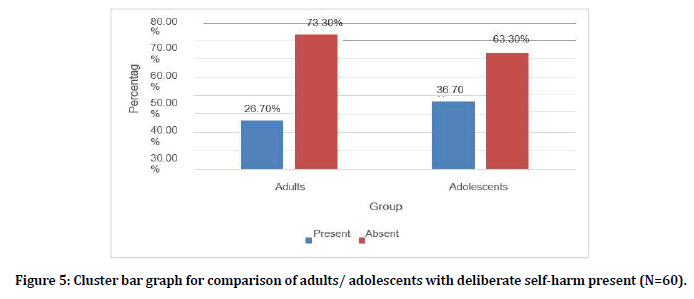
Figure 5. Cluster bar graph for comparison of adults/ adolescents with deliberate self-harm present (N=60).
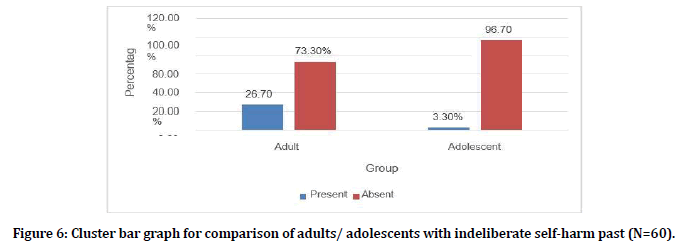
Figure 6. Cluster bar graph for comparison of adults/ adolescents with indeliberate self-harm past (N=60).
Prevalence of depression
Depression was assessed by using the Hamilton Depression Rating scale. Scores were recorded. 0-7 indicates no depression, 8 -13 indicates mild depression, 14-18 indicates moderate depression, 19 -22 indicates severe and >23 indicates very severe depression.
Among the adults7 (23.3%) had mild depression, 18 (60%) had moderate depression, 5 (16.7%) had severe depression. Among the adolescents 16 (53.3%) had mild depression, 13 (43.3%) had moderate depression, 1 (3.3%) had severe depression. There was statistically significant difference in Prevalence of depression between adults and adolescents. (P value 0.030) (Figure 7).
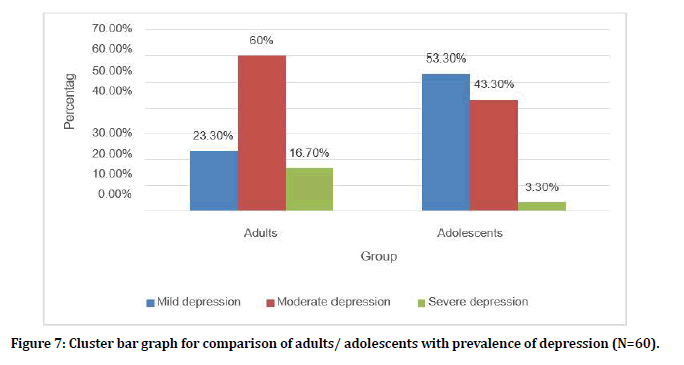
Figure 7. Cluster bar graph for comparison of adults/ adolescents with prevalence of depression (N=60).
Beck’s suicidal intent scale
The suicidal intent in the attempted subjects was assessed using the Beck’s Suicidal Intent Scale. The score asper the scales were, 15 -19 low intent, 20 -28 medium intent, 29+ high intent. Among the adults5 (16.7%) had low suicidal intension, 4 (13.3%) had medium intension, 1 (3.3%) had high intension. Among the adolescents 2 (6 .7%) had low suicidal intension and 8 (26.7%) had medium intension (Figure 8).
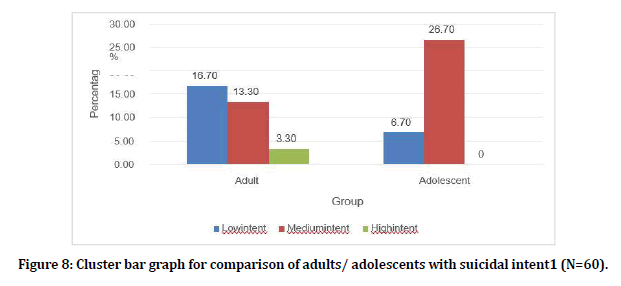
Figure 8. Cluster bar graph for comparison of adults/ adolescents with suicidal intent1 (N=60).
Among the people belonged to lower middle SES 2 (14.3%) had low intent, 2 (14.3%) had medium intent. Among the people belonged to upper middle 3(30%) had low intent and 1 (10%) had medium intent. Among the people belonged to upper SES 1 (20%) had medium intent and1(20%) had high suicidal intent (Figure 9).
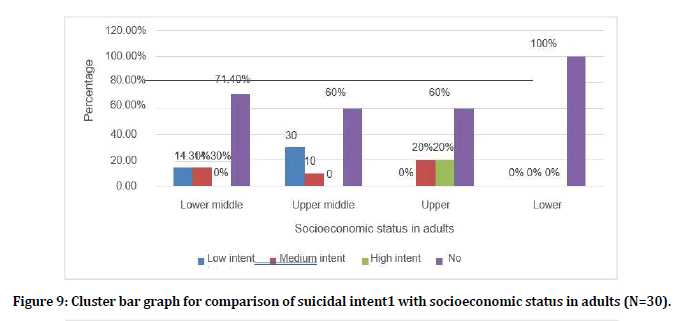
Figure 9. Cluster bar graph for comparison of suicidal intent1 with socioeconomic status in adults (N=30).
Among the people who had Alcohol abuse 2 (33.3%) had low suicidal intent, 1 (16.7%) had medium intent and 1 (16.7%) had high intent. (Figure 10).
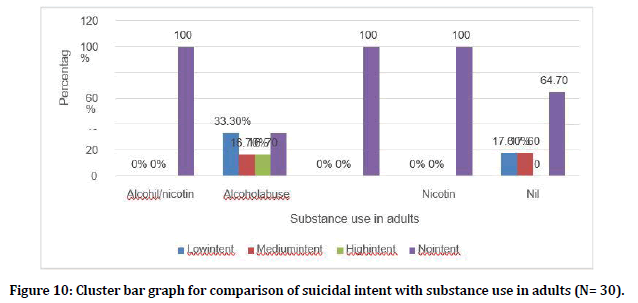
Figure 10. Cluster bar graph for comparison of suicidal intent with substance use in adults (N= 30).
Among the people with past psychiatric history 2 (16.7%) had medium suicidal intent, 1(8.3%) had high intent in adults (Figure 11).
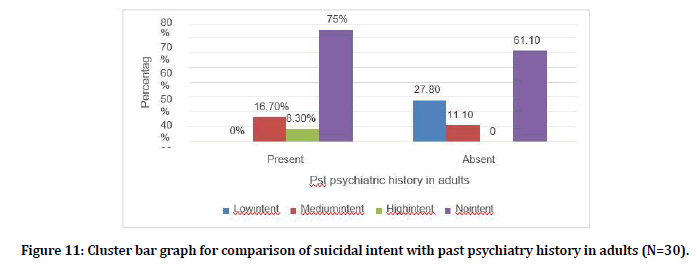
Figure 11. Cluster bar graph for comparison of suicidal intent with past psychiatry history in adults (N=30).
Among the people belonged to lower middle SES 1 (6.3%) had low suicidal intent, 6 (37.5%) medium intent. Among the people belonged to upper middle 1(7.7%) had low suicidal intent, 2 (15.4%) had medium suicidal intent (Figure 12).
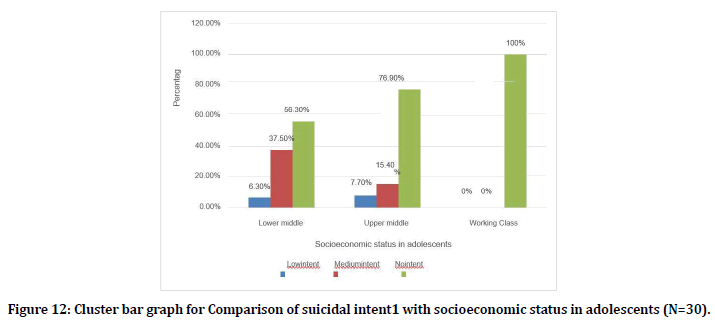
Figure 12. Cluster bar graph for Comparison of suicidal intent1 with socioeconomic status in adolescents (N=30).
Among the people who had Alcohol/ nicotine1 (100%) had low suicidal intent, among the people who had cannabis 1 (100%) had medium intent, among the people who had nicotine 1 (16.7%) had medium suicidal intent (Figure 13). Among the people with past psychiatric history only 1 (14.3%) person had medium suicidal intent in adolescents (Figure 14). Among the people with deliberate self-harm past in adults 2 (25%) had low intent, 3 (37.5%) had medium intent and 1 (12.5%) high intent (Table 1 and Figure 15).
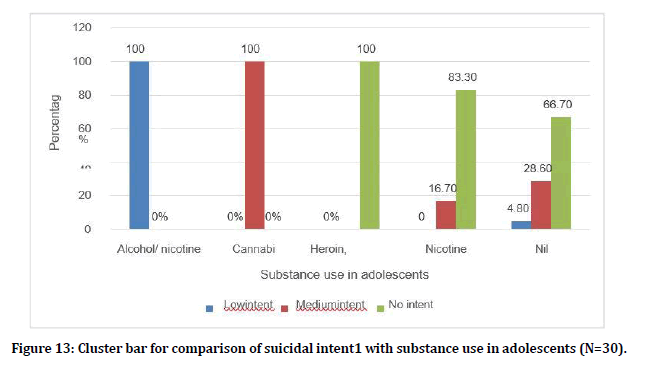
Figure 13. Cluster bar for comparison of suicidal intent1 with substance use in adolescents (N=30).
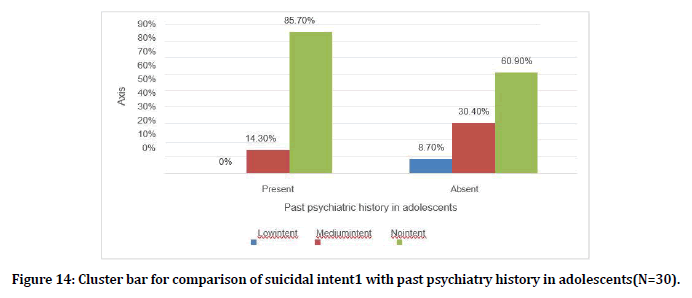
Figure 14. Cluster bar for comparison of suicidal intent1 with past psychiatry history in adolescents(N=30).
| Deliberate self-harm past | Suicidal intent | |||
|---|---|---|---|---|
| Low intent | Medium intent | High intent | No intent | |
| Present (N=8) | 2 (25%) | 3 (37.5%) | 1 (12.5%) | 2 (25%) |
| Absent (N=22) | 3 (13.6%) | 1 (4.5%) | 0 (0%) | 18 (81.8%) |
Table 1: Comparison of suicidal intent with deliberate self-harm past in adults (N=30).
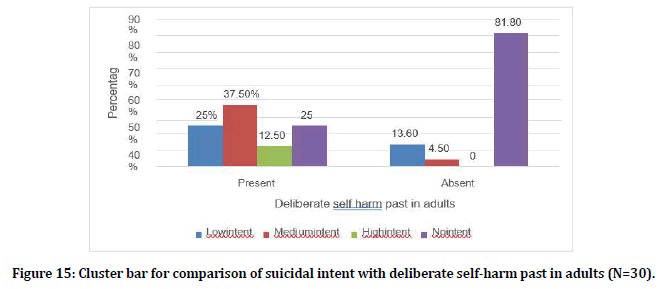
Figure 15. Cluster bar for comparison of suicidal intent with deliberate self-harm past in adults (N=30).
Figure 16 represents the comparison of suicidal intent with deliberate self-harm past in adolescents. Figure 17 comparison of suicidal intent with deliberate self-harm present in adults. Figure 18 represents comparison of suicidal intent with deliberate self-harm present in adolescents.
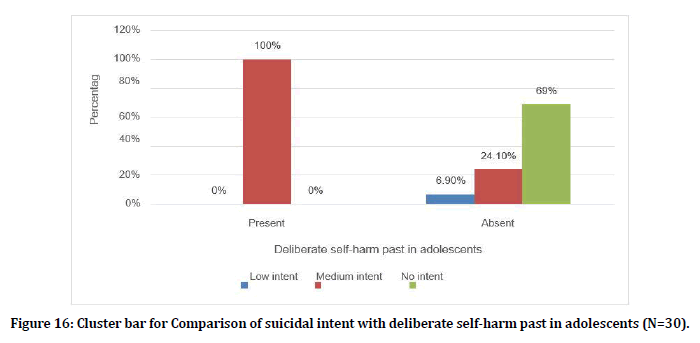
Figure 16. Cluster bar for Comparison of suicidal intent with deliberate self-harm past in adolescents (N=30).
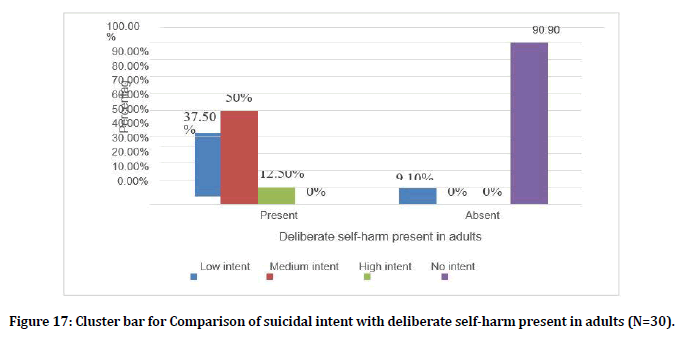
Figure 17. Cluster bar for Comparison of suicidal intent with deliberate self-harm present in adults (N=30).
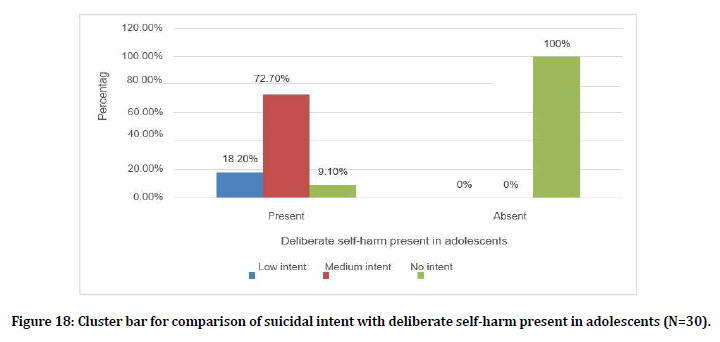
Figure 18. Cluster bar for comparison of suicidal intent with deliberate self-harm present in adolescents (N=30).
In the study done, the prevalence of suicidal behavior in the form of deliberate self-harm is present in about 26.7% in adult and 36.7% in adolescent. The study is similar to previous study done in Singapore and reported a total of 58.8% DSH in outpatients attending psychiatry clinic. The suicidal intent in the study which is assessed according to the Beck’s Suicidal Intent scale shows adult having a low intent of 16.7%, medium intent of13.3 and high intent of 3.3%. In adolescent the intent of low was 6.7% and medium was 26.7%. The total of the two group came up to low intent of 23.4% and medium intent of 40%.
The study was also a hospital-based study. The result was a low intent of 26.76% and medium of 31.4%. The study assessed the socio-economic status of the participants and accordingly the presence of the upper middle and the lower middle were more prominent. The prevalence of suicidal intent in adult is more on the upper middle as compared to the low middle class. The included subjects were 46.7% and 33.3% lower and upper middle class respectively.
The study assessed the prevalence of psychiatric illness in the patient and in this, among adults, depression was the main prevalence which was 40% and followed by bipolar which is 16.7%. This is like the study by Jain et al, which had 67.3% of The study assessed the prevalence of psychiatric illness in the patient and in this, among adults, depression was the main prevalence which was 40% and followed by bipolar which is 16.7%. This is like the study by Jain et al, which had 67.3% of
The study also assesses the prevalence of substance abuse in adult and adolescent. And the distribution of the suicidal intent as according to the consumption of substance of abuse. In this study, in adult’s alcohol use/ abuse and alcohol Along with nicotine are the forerunners. They contribute about, 20 %and 13.3% respectively. This is like the study of Jung M. J et al. a study conducted in Korea. They recorded a value of high suicide intent in alcoholic and medium to low in both alcohol and nicotine addict. In adolescent the main substance of abuse is nicotine.
In this study the comparison done with the suicidal intent in adult and Adolescent regarding the various parameters are considered. The various factors that come into play are the complaints of psychiatric disorder like depression, bipolar, schizophrenia and anxiety etc.
The distribution of the disorders according to this study, where the study Group are taken into consideration are, depression-66.7%, bipolar- 23.4%, schizophrenia-16.6%, anxiety-20%. This is like the previous study in which the common cause for attempted suicideis due to depression accounts for 65%, anxiety accounts for 31%.
In this study, most of the attempted suicide are those below the age of 30, in this again the adolescent age group have more suicidal behavior as compared to adult. This study is like the study by Hedge et al, where the suicide attempters were less than 44 years of age.
According to this study, the distribution of the male: female ratio is 46.7:53.3. This signifies the increasing rate of distress as well as the increase ideation in female as compared to male. The study also reports of higher suicidal intent in those with psychiatric illness as compared to “normal” individuals. This is like previous studies which identified the presence of stressful life events and psychiatric illness as one of the reasons for attempting suicide. This study evaluated cases attempting suicide but a comparative finding where almost all cases have some form of psychiatric illness and life events [4-30].
Conclusion
This is a tertiary care general hospital-based study to assess the prevalence of suicidal behavior in adults and adolescents. The result suggested the higher suicidal behavior in individuals who have previously made an attempt. This applies more for adults as compared to adolescent. Suicidal behavior as well as suicidal intent is seen more in the lower middle class. The data finding was 43.8% in the lower middleclass.
This study also suggested the presence of increased suicidal behavior in adults using substances, out of which alcohol abuse is more common. Suicidal behavior is much more common in adolescents who have combined dependence of alcohol and nicotine. The data finding was 66.7%. Both adolescents and adults who have psychiatric illness mostly major depressive disorder, followed by bipolar affective disorder, schizophrenia and anxiety have more suicidalintent.26% of adults and 36% of adolescents have made at least one attempt of deliberate self-harm in previous month. Compared to adolescents, adults who have previous history of attempted suicide are more prone to attempt/commit suicide.
Funding
No funding sources.Ethical Approval
The study was approved by the Institutional Ethics Committee.Conflict of Interest
The authors declare no conflict of interest.Acknowledegements
The encouragement and support from Bharath University, Chennai is gratefully acknowledged. For provided the laboratory facilities to carry out the research work.
References
- https://www.who.int/mental_health/suicide-prevention/world_report_2014/en/#:~:text=It%20aims%20to%20increase%20awareness,in%20a%20multisectoral%20public%20healt
- https://www.unaids.org/sites/default/files/media_asset/unaids-data-2018_en.pdf
- https://www.who.int/reproductivehealth/publications/monitoring/maternal-mortality-2015/en/
- https://www.goodreads.com/book/show/9185990-bhagavad-gita
- https://ncrb.gov.in/en/accidental-deaths-suicides-india-adsi
- https://ncrb.gov.in/en/accidental-deaths-suicides-in-india
- Bhugra D. Sati: A type of nonpsychiatric suicide. Crisis 2005; 26:73-77.
- Hornby AS. Oxford Advanced learner's dictionary of current english oxford: Oxford University Press 1995.
- Neeleman J, Halpern D, Leon D, et al. Tolerance of suicide, religion and suicide rates: an ecological and individual study in 19 Western countries. Psychol Med 1997; 27:1165-1171.
- Lemperiere T. A better approach to mood disorders? Symposium. J Psychiatr Bio Clin Therapeutics 1995; 21:1-67.
- Durkheim E. Le Suicide. Paris: PUF 1990.
- https://archive.org/details/AHistoryOfClassicalSociology_573
- Hendin H. Psychotherapy and suicide. Am J Psychother 1961; 35:469 -480.
- Farberow NL, Shneidman E. The cry for help. New York: McGraw Hill,1961.
- Kaplan HI, Sadock BJ. Comprehensive textbook of psychiatry. III Ed. Baltimore: Williams &Wilkins, 1981.
- Jena S, Sidhartha T. Non-fatal suicidal behaviors in adolescents. Indian J Psychiatry 2004; 46:310-318.
- Narang RL, Mishra BP, Nitesh M. Attempted suicide in Ludhiana. Indian J Psychiatry 2000; 42:83-87.
- Osvath P, Voros V, Fekete S. Life events and psychopathology in a group of suicide attempters. Psychopathology 2004; 37:36-40.
- Overholser JC, Normen WH, Miller IW. Life stress and social supports in depressed inpatients. Behavioural Med 1990; 16:125-132.
- Rudd MD. An integrative model of suicidal ideation. Suicide and Life-Threatening Behaviour 1990; 20:16-30.
- Philps DP, Lesyna K, Paight DJ. Suicide and the media: Research and policy implications. In: DiekstraR, et al. Eds. Assessment and prevention of suicide. New York: Guilford Press, 1992.
- Singh G, Kaur H. Hand book of presumptive stressful life events scale. Agra: National Psychological Corporation1983.
- Holmes TH, Rahe RH. The social adjustment rating scale. J Psychosom Res 1967; 11:213
- Weissman MM. The epidemiology of suicide attempts. 1960 to 1971. Arch Gen Psychiatry 1974; 30:737.
- WHO. Prevention of suicide. Public Health Paper: No. 35. Geneva: World Health Organisation 1968.
- Beck AT, Davis JH, Frederick CJ, et al. Classification and nomenclature. In: Resnik HLP, Hathorne BC, Eds., Suicide prevention in the seventies, government printing office, Washington, 1972; 7-12.
- https://store.samhsa.gov/sites/default/files/d7/priv/sma16-4935.pdf
- Gajalakshmi V, Peto R. Suicide rates in rural Tamil Nadu, South India: Verbal autopsy of 39000 deaths in 1997-98. Int J Epidemiol 2007; 36:203-207.
- Hagnell O, Rorsman B. Suicide in the Lund by study: A controlled prospective investigation of stressful life events. Neuropsychobiol 1980; 6:319-332.
- Patel V, Chatterji S, Chisholm D, et al. Chronic diseases and injuries in India. Lancet 2011; 377:413-428.
Author Info
Department of Psychiatry, Sree Balaji Medical College & Hospital Affiliated to Bharath Institute of Higher Education and Research, Chennai, Tamil Nadu, IndiaCitation: Heigrujam Jina, S Nambi, A Comparative Study of Suicidal Behavior in Adolescents and Adults Attending Psychiatry OPD in a Tertiary Care Hospital, J Res Med Dent Sci, 2021, 9 (6):529-538.
Received: 03-Apr-2021 Accepted: 27-Apr-2021
