Research - (2021) Volume 9, Issue 5
A Comparative Study on Left Ventricular Mass in Hypertensive Patients with and Without Type 2 Diabetes Mellitus
Daya Sindhu Krishna, S Palaniandavan, T Manivel and G Jagan*
*Correspondence: G Jagan, Department of General Medicine, Sree Balaji Medical College and Hospital Affiliated to Bharath Institute of Higher Education and Research, Chennai, Tamil Nadu, India, Email:
Abstract
Objectives: Hypertension and Diabetes- a worldwide burden is a major risk factor for cerebro-vascular accident and is the most modifiable factor in cardiovascular diseases.
Methods: This is a prospective cross-sectional study conducted in Sree Balaji Medical College and Hospital. 50 patients with hypertension alone for more than 5 years ,50 patients with diabetes and hypertension for more than 5 years were considered the study population and those not suffering from any cardiac disease of were taken as control. All patients were above the age of 30 years.
Results: There is significant statistical correlation between age group and left ventricular mass in hypertension with diabetes group (p =0.015). There is significant statistical correlation with both males(p<0.000) and females (p<0.000) with respect to left ventricular mass in hypertension and diabetes population. Females were at higher chances of having increased left ventricular mass compared to males based on chi square value. There was significant statistical correlation between BMI and left ventricular mass (p<0.004).
Conclusion: The study shows that there is increased left ventricular mass in females with hypertension and diabetes mellitus when compared to females with hypertension alone but not in males.
Keywords
Left ventricular mass, Hypertension, Type -2 Diabetes mellitus, Echocardiography, Penn formula
Introduction
Hypertension being a major risk factor for cerebro- vascular accidents, cardiovascular disease has significant morbidity and mortality. Hypertension causes 7.5million deaths globally which accounts to about 57 million disability adjusted life years (DALYs). The prevalence of hypertensive patients globally above the age of 25 had risen by 40% by 2008. According to the WHO survey in 2008, the number of people with uncontrolled hypertension rose from 600 million in 1980 to nearly 1 billion in 2008 [1,2].
Echocardiography has become an especially important tool in the management of hypertension. Although ECG is useful in identifying left ventricular hypertrophy, it is not overly sensitive. The LVH criteria for left ventricular hypertrophy was 7%-35% in moderate hypertrophy and 10% - 50% in severe hypertrophy. Therefore, echocardiography is considered the preferred tool for the assessment of left ventricular hypertrophy and M-mode technique is the gold standard test.
Diabetes mellitus refers to “A group of common metabolic disorders that share the phenotype of hyperglycemia. The metabolic dysregulation associated with DM causes secondary pathophysiologic changes in multiple organ systems that impose a tremendous burden on individuals with diabetes as well as on the health care system” [3-5]. The prevalence of diabetes according to WHO survey has risen from 108 million in 1980 to 422 million in 2014. In 2015, an estimated 1.6 million deaths were directly caused by diabetes.
Another 2.2 million deaths were attributable to high blood glucose in 20121 [6].
Diabetes mellitus predisposes to cardiovascular diseases. In diabetes mellitus, insulin resistance, high HbA1c and dysautonomia leads to increased left ventricular mass. All these factors lead to increased morbidity and mortality in diabetic individuals when compared to non–diabetics [7].
Materials and Methods
Selection of subjects
Patients with hypertension alone and patients with both hypertension and diabetes mellitus of more than 30 years attending the hypertension outpatient department of Sree Balaji Medical College. The selected patients should be on regular treatment not on cardiac remodeling drugs like angiotensin converting enzyme inhibitors and aldosterone antagonists. Control groups with more than 30 years without diabetes mellitus and hypertension.
Inclusion criteria
✓ All patients > 30 yrs of age with hypertension of duration > 5yrs on regular treatment.
✓ Patients >30 yrs of age with hypertension and diabetes mellitus >5yrsduration on regular treatment.
✓ Healthy controls of >30yrs of age.
Exclusion criteria
✓ Coronary Artery Disease 2. Valvular Heart Disease.
✓ Chronic Kidney Disease of non-diabetic origin.
✓ Obesity.
✓ Cardiomyopathies.
Setting: Sree Balaji Medical College and Hospital.
Study design: Prospective Cross-sectional study
Period of study: 1 year from April 2017 to March 2018.
Sample size: 150 subjects (50 Hypertensive cases+50 Cases of both hypertension and diabetes + 50 controls).
Both cases and controls are investigated by following measures:
✓ Proper history and past medical history and demographic details were collected.
✓ General examination, Vitals monitoring includes blood pressure and pulse rate.
✓ Body Mass Index.
✓ Fasting and Post-prandial Blood Sugar
✓ Complete hemogram.
✓ Blood Urea, Serum Creatinine and Serum Electrolytes Urine analysis.
✓ Serum Total Cholesterol, Serum Triglyceride levels.
✓ Electrocardiography.
✓ Chest X-Ray.
✓ 2-Dimensional Echocardiography.
Echocardiography
By using trans-thoracic 2-Dimensional echocardiographic method, the following left ventricular dimensions are measured by M-mode technique using the parasternal long axis view just above/at the tip of the papillary muscle level.
Results
This study was done in the Department of General Medicine at Sree Balaji Medical College and Hospital, Chennai to compare left ventricular mass in hypertension with diabetes and hypertension without diabetes and compare them with control. In this present study among 50 systolic hypertension cases 3.3% were in the age group of less than 45 years, 10.7% were in the age group of 46 -55 years, 6% of the cases were between 56 -65 years, 6.7% in the age range of 66-75 years and 6.7% were found to be above 75 years of age. Likewise, among 50 patients with hypertension and Diabetes Mellitus (DM) 5.3% were below 45 years of age, 6% were in the age group of 46 -55 years, 7.3% of the cases were between 56-65 years, 6.7% in the age range of 66 -75 years and 8% were found to be above 75 years of age.
Among the control group 6.7% of the study participants were below 45 years of age, 6.7% were in the age group of 46-55 years, 3.3% were between age range of 56-65 years, 6.7% in the age group of 66 -75 years and the rest 10% were in the age group of more than 75 years (Table 1).
Table 1: Age group wise distribution of study participants.
| Age group | Group | |||
|---|---|---|---|---|
| SHTN | HTN+DM | Control | Total | |
| <45 years | 5 (3.3) | 8 (5.3) | 10 (6.7) | 23 (15.3) |
| 46-55 years | 16(10.7) | 9(6.0) | 10(6.7) | 35(23.3) |
| 56-65 years | 9(6.0) | 11(7.3) | 5(3.3) | 25(16.7) |
| 66-75 years | 10(6.7) | 10(6.7) | 10(6.7) | 30(20.0) |
| >75 years | 10(6.7) | 12(8.0) | 15(10.0) | 37(24.7) |
There was statistical significance between the severity of left ventricular mass and the age group among cases in this study. With normal left ventricular mass and the age group among cases and control there was statistical significance with p value 0.021. There was statistically significant correlation found between mild left ventricular mass and age group among cases and controls. (p value 0.015). Statistical significance was not found between moderate and severe form of left ventricular mass and age groups in HT and HT+DM group although, there was increased incidence of left ventricular mass in HT+DM with age (Figure 1).
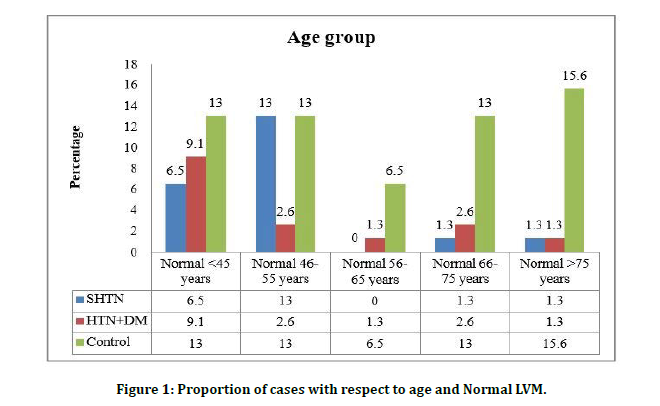
Figure 1: Proportion of cases with respect to age and Normal LVM.
Among 50 patients in the systolic hypertension cases 28 were females and 22 were males. In hypertension with DM cases 30 were females and 20 were males. Among the control group 23 participants were females and 27 participants are male (Table 2 and Figure 2).
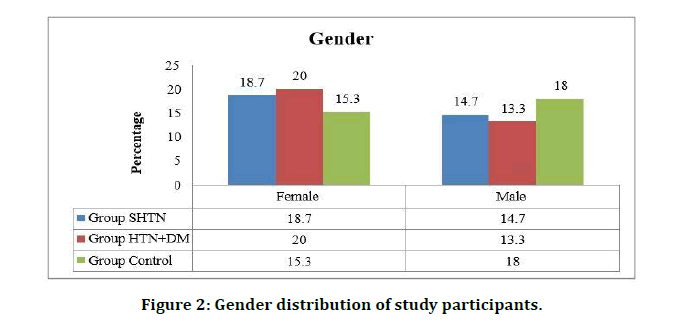
Figure 2: Gender distribution of study participants.
Table 2: Gender distribution of study participants.
| Gender | Group | |||
|---|---|---|---|---|
| SHTN | HTN+DM | Control | Total | |
| Female | 28(18.7) | 30(20.0) | 23(15.3) | 81(54.0) |
| Male | 22(14.7) | 20(13.3) | 27(18.0) | 69(46.0) |
Among the female patients with systolic hypertension 8.6% were normal, 7.4% had mild left ventricular mass, 6.2% and 12.3% had moderate and severe form of left ventricular mass respectively. In female patients with HTN and DM there were 7.4%,3.7% , 3.7% and 22.2% of cases with normal, mild ,moderate and severe left ventricular mass respectively. Among female control group 25.9% were normal and 1.2% of each was found to have mild and moderate left ventricular mass. In this current study there was high statistical correlation found for gender and the left ventricular mass. Among female gender and left ventricular mass among cases and control there was statistical significance with p value <0.000 and between male gender and left ventricular mass the p value was found to be statistically significant (p value<0.000). Females were at higher chances of having LVM compared to males on the basis of chi square value (Table 3 and Figure 3).
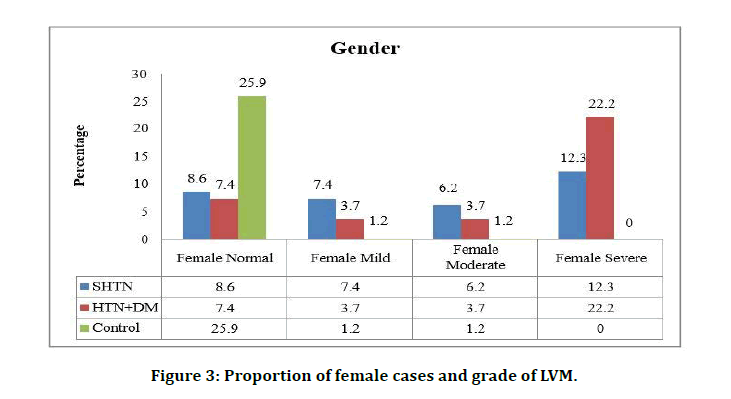
Figure 3: Proportion of female cases and grade of LVM.
Table 3: Proportion of cases with respect to gender and LVM.
| Gender | Lv mass | SHTN | HTN+DM | Control | Chi sq | P-value |
|---|---|---|---|---|---|---|
| Female | Normal | 7(8.6) | 6(7.4) | 21(25.9) | 37.6 | .000* |
| Mild | 6(7.4) | 3(3.7) | 1(1.2) | |||
| Moderate | 5(6.2) | 3(3.7) | 1(1.2) | |||
| Severe | 10(12.3) | 18(22.2) | 0(0.0) | |||
| Male | Normal | 10(14.5) | 7(10.1) | 26(37.7) | 24.2 | .000* |
| Mild | 1(1.4) | 3(4.3) | 1(1.4) | |||
| Moderate | 3(4.3) | 3(4.3) | 0(0.0) | |||
| Severe | 8(11.6) | 7(10.1) | 0(0.0) |
*Significant
Body mass index was found to be normal in 20.7% of the systolic hypertension cases and 10% of the hypertension patients were overweight and 2.7% were obese. Among the HTN and DM group 16% were normal, 9.3% were overweight and 8% were found to be obese. In the control group 30.7% participants were having normal BMI, 2.7% were overweight and no case of obesity was recorded (Figure 4).
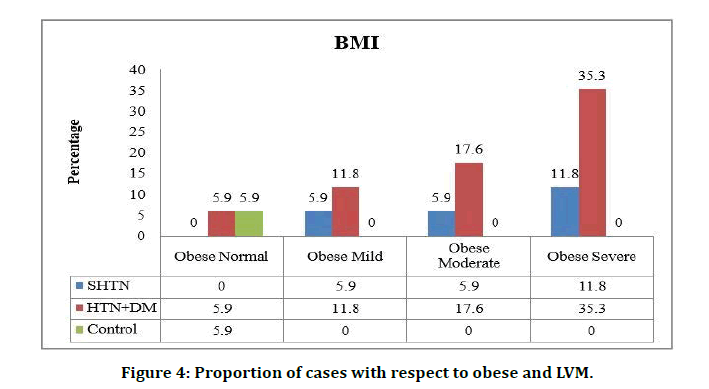
Figure 4: Proportion of cases with respect to obese and LVM.
Among 50 SHTN cases 11.3% were normal, 4.7% had mild left ventricular mass, 5.3% had moderate mass and 12% cases had severe left ventricular mass. In patients with HTN and DM 8.7% were normal, 4% had mild left ventricular mass, 4% had moderate and 16.7% had severe left ventricular mass. Among the 50 controls 31.3% were normal, 1.3% had mild left ventricular mass, 0.7% had moderate mild left ventricular mass.
In this present study among 50 SHTN cases 32 patients had Grade 1 Diastolic Dysfunction (DD) and in 50 patients with HTN and DM 37 had Grade 1 Diastolic Dysfunction. Among the control group 7 patients had Grade 1DD (Table 4 and Figure 5).
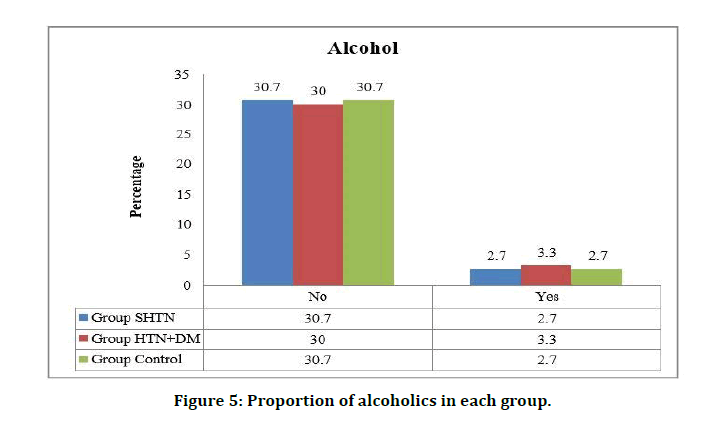
Figure 5: Proportion of alcoholics in each group.
Table 4: Proportion of cases with grade 1 DD in each group.
| Grade1DD | Group | |||
|---|---|---|---|---|
| SHTN | HTN+DM | Control | Total | |
| Absent | 18(12.0) | 13(8.7) | 43(28.7) | 74(49.3) |
| Present | 32(21.3) | 37(24.7) | 7(4.7) | 76(50.7) |
Among the 4 alcoholics in SHTN group 1 patient had severe left ventricular mass and in HTN+DM group of 5 alcoholics 2 had mild and 2 had moderate left ventricular mass. There was not statistical significance between alcoholics and LV mass (p =0.084) (Figure 6).
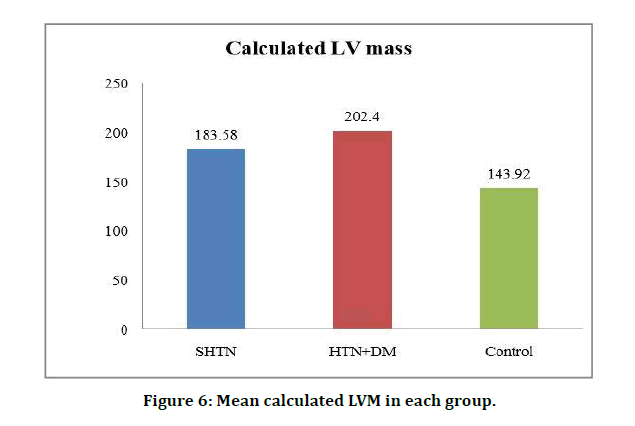
Figure 6: Mean calculated LVM in each group.
Discussion
In our study, we studied 150 subjects (50 -HT only, 50- HT+DM, 50-Controls without HT and DM) and the left ventricular mass of the three groups were compared. The minimum age of the cases and controls was 30 years and maximum age was 88 years. There is significant statistical correlation between the severity of the left ventricular mass and the age group in this study. Statistical significance was found between mild left ventricular mass and age group among the study population (P value is 0.015). Statistical significance was not found between moderate and severe form of left ventricular mass and age groups in HT+DM and HT only group, although there was an increased incidence of higher left ventricular mass in HT+DM group with age [8].
There is high significant statistical correlation between female (p<0.000) cases in HT+DM group and in males (p<0.000) in HT+ DM group. Females were at a higher chance of having increased left ventricular mass compared to males based on chi square value. Among cases with HT+DM there is increased prevalence of overweight (30.3%) and obesity (35.3%). There was high statistical significance between BMI and let ventricular mass (p value was <0.0001). There was high statistical significance for overweight and increased left ventricular mass among cases (p value 0.004). It was noted that the left ventricular mass was more in HT+DM group when compared to the HT only group [9,10]. There was high statistical correlation between the mild increase in left ventricular mass ( p value 0.003) and the duration of illness and moderate increase in left ventricular mass ( p value 0.004) and duration of illness. Severe increase in left ventricular mass was not found statistically significant although, as the duration of illness increased, there was increased incidence of severe increase in left ventricular mass in HT+DM group when compared to the HT only group [11,12].
There was high statistical correlation between increased left ventricular mass and Grade 1 diastolic dysfunction (p<0.000) in HT+DM group when compared to the HT only group. There was significant statistical correlation between left ventricular mass and menopause ( p value 0.000). In our study, women with menopause are associated to have a higher left ventricular mass. There was significant increase in left ventricular mass in female with menopause in the HT+DM group when compared to the HT only group females with menopause [13-15].
While comparing LV mass between these three groups (HT, HT+DM, Control) there is significant statistical correlation between three groups. But while comparing the two groups (HT, HT+DM), the difference of LV mass was found to be higher in HT+DM group than compared to HT only group [16].
There was no significant difference in the left ventricular mass in males in both DM+HT and HT only group. In females, there was an increase in left ventricular mass in DM+HT group when compared to HT only group. Increase in duration of diabetes and hypertension also increases the left ventricular mass and among females, there was an increased incidence of higher left ventricular mass in women who have attained menopause in HT+DM group when compared to the HT only group Alexander Tenenbaum and their colleagues studied 550 hypertensives (314 men, 246 women), 200 of them (108 men, 92 women) were having type 2 diabetes mellitus [17]. It was found that females with DM+HT had higher prevalence of increased left ventricular mass when compared to males. The Augsburg family study showed that there w a s increase in left ventricular mass in women with diabetes.
Conclusion
Type- 2 Diabetes Mellitus being a multi system disease is associated with increased cardiovascular morbidity and mortality. In the present study, we studied 150 subjects (50-HT only, 50- HT+DM, 50-Controls without HT and DM) and the left ventricular mass of the three groups were compared. The data was analysed and compared between the groups and the following observations were made. As the age increases, there is increase in left ventricular mass. It is predominantly found in HT+DM group when compared to the HT only group.
Females with HT+DM had increase in left ventricular mass when compared to females with HT alone. Females were at a higher chance of having an increased left ventricular mass when compared to males. There was increase in left ventricular mass in HT+DM group when compared to the HT only group.
Thus, increased left ventricular mass is an important cause for cardiovascular morbidity and mortality. Females with diabetes and hypertension in menopause should be managed aggressively for reduction of left ventricular mass.
Funding
No funding sources.
Ethical Approval
The study was approved by the Institutional Ethics Committee.
Conflict of Interest
The authors declare no conflict of interest.
Acknowledgements
The encouragement and support from Bharath Institute of Higher Education and Research, Chennai is gratefully acknowledged. For provided the laboratory facilities to carry out the research work.
References
- Mathers CD, Loncar D. Projections of global mortality and burden of disease from 2002 to 2030. PLoS medicine. 2006; 3:e442.
- Collins R, McMahon S. Blood pressure, antihypertensive drug treatment and the risks of stroke and of coronary heart disease. Br Med Bull 1994; 50:272-298.
- Wild S, Roglic G, Greene A, et al. Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care 2004; 27:1047-1053.
- International Diabetes Federation: Diabetes Atlas 2003. Brussels, International Diabetes federation 2003
- Pearson AC, Pasierski T, Labovitz AJ. Left ventricular hypertrophy, diagnosis, prognosis and management. Am Heart J 1991; 121:148-155.
- Lee KW, Lip GYH. Haemostasis, thrombosis and vascular biology unit, university department of medicine, city hospital, Birmingham, UK. J Human Hypertension 2003; 17:299–304.
- Ribeiro-Filho FF, Rosa EC, Faria NA, et al. Abdominal obesity, insulin resistance and hypertension: impact on left ventricular mass and function in women. Arq Bras Endocrinol Metab 2000; 44:64 -71.
- Den Hond E, Celis H, Vandenhoven G, et al. Determinants of white-coat syndrome assessed by ambulatory blood pressure or self-measured home blood pressure. Blood Pressure Monitoring 2003; 8:37-40.
- Laks MM. Norepinephrine, the producer of myocardial cellular hypertrophy and/or necrosis and/ or fibrosis. Am Heart J 1977; 94:394-399.
- Mulvany MJ, Aalkjaer C. Structure and function of small arteries. Physiol Rev 1990; 70:921-961.
- Sadoshima JI, Izumo S. Molecular characterization of angiotensin IIinduced hypertrophy of cardiac myocytes and hyperplasia of cardiac fibroblasts. Circ Res 1993; 73:413–423.
- Baker KM, Aceto JF. Angiotensin II stimulation of protein synthesis and Cell growth in chick hearts cells. Am J Physiol 1990; 258:H610 –H618.
- Schunkert H, Sadoshima JI, Cornelius T, et al. Angiotensin II–induced growth responses in isolated adult rat hearts: Evidence for load-independent induction of cardiac protein synthesis by angiotensin II. Circulation Res 1995; 76:489-497.
- Olsen MH, Wachtell K, Hermann KL, et al. Is cardiovascular remodeling in patients with essential hypertension related to more than high blood pressure? A LIFE substudy. Am Heart J 2002; 144:530-537.
- Shigematsu Y, Hamada M, Ohtsuka T, et al. Left ventricular geometry as an independent predictor for extracardiac target organ damage in essential hypertension. Am J Hypertension 1998; 11:1171-1177.
- Troy BL, Pomb J, Rackley E. Measurement of LV wall thickness mass by echo. Circulation 1971; 25:602.
- Levy D, Garrison RJ, Savage DD, et al. Prognostic implications of echocardiographically determined left ventricular mass in the Framingham Heart Study. New England J Med 1990; 322:1561-1566.
Author Info
Daya Sindhu Krishna, S Palaniandavan, T Manivel and G Jagan*
Department of General Medicine, Sree Balaji Medical College and Hospital Affiliated to Bharath Institute of Higher Education and Research, Chennai, Tamil Nadu, IndiaCitation: Daya Sindhu Krishna, S Palaniandavan, T Manivel, G Jagan, A Comparative Study on Left Ventricular Mass in Hypertensive Patients with and Without Type 2 Diabetes Mellitus, J Res Med Dent Sci, 2021, 9 (5):207-213.
Received: 22-Mar-2021 Accepted: 21-May-2021 Published: 31-May-2021
