Research - (2021) Volume 9, Issue 11
An Unusual Case of Recurrent Fever
Abhilash Nair*, Padma V, Rameez Raja, Murugaraj, Sarath Bhaskar S, Saketh Ramineni and Kannan Meera Devi
*Correspondence: Abhilash Nair, Department of General Medicine, Sree Balaji Medical College and Hospital, India, Email:
Abstract
A fever is a part of your body’s natural defenses system. Your immune system is the part of your body that works to fight off illnesses. When this system is triggered, your body’s temperature heats up. Typically, your average body temperature should be around 98.6° Fahrenheit (or 37° Celsius). A fever is a temperature of 100.4° Fahrenheit or higher. If you take a child’s temperature orally or axillary (armpit), you might get a reading that’s up to one degree off. To get the most accurate temperature reading, take the child’s temperature rectally. A recurring fever is a fever that happens multiple times over a period of time. These fevers can sometimes be described as episodic, meaning that they come and go. A recurrent fever is one that comes back in a pattern. For example, your young child or toddler could have a fever every month. This type of fever is typically seen in young children, usually under age 5 (infants and toddlers in particular). The increased temperature lasts for a few days and then goes away for a stretch of time. The child is healthy and acts normally in between fevers. Recurrent fever is one of the main symptoms of a collection of conditions called periodic fever syndromes. These are diseases that cause a person — typically a child — to have a fever in a spaced out pattern over time, without having a virus or bacterial infection.
Keywords
Recurrent fever, Bacterial infection, Periodic fever syndrome
Case Report
A 71-year-old male, known case of T2DM/SHTN on regular treatment came with complains of fever for 5 days which was high grade, intermittent, gradual in onset, associated with chills and rigors. He complained of evening rise of temperature, generalized body ache and headache. There was no history of vomiting/loose stools. No history of burning micturition/cold/cough was there. There was no history suggestive of decreased urine output and no history of loss of consciousness or altered sensorium. No abdominal pain or chest pain was there. There was no shortness of breath on lying flat or any attack of severe shortness of breath and coughing at night. No history of significant weight loss. His bowel and bladder were regular, appetite reduced and reduced sleep. He was known case of Type 2 Diabetes Mellitus o regular treatment with SFUs and Metformin. He was a known case of systemic Hypertension on regular treatment with ACE Inhibitors and Calcium Channel Blockers. He was known to have similar episodes in the past for which he used to get admitted. He was an active smoker with an average smoke exposure of 18 pack-years (range, 5-32). There was no family history of similar complaints.
Examination
On examination patient was moderately built and nourished. He was conscious, oriented and a febrile. There was no pallor, icterus, cyanosis, clubbing, lymphadenopathy or edema. Cardiovascular system examination was normal and S1 and S2 was heard, no murmurs were present. Respiratory system examination showed bilateral air entry present with fine crept in left infraclavicular area. CNS examination didn’t reveal any further significant findings and per abdomen examination did not reveal any anomaly like tenderness or organomegaly. His Blood Pressure was 130/80mmHg, Respiratory Rate was 96bpm. Capillary Blood Glucose was 175mg/dl and his saturation was 89% at room air
Investigations
He was provisionally diagnosed as Fever for evaluation probably viral in origin. All routine investigations were sent. His WBC was 7520cells/cumm, ESR was 47mm at 1 hour, platelet was 1.27lakh cell/mm, Haemoglobin was 12.6gm/dl, and PCV was 35.7. His Renal function test values were nearly normal with serum Creatine at 1.2, Serum Urea at 28. Serum Sodium and Serum Potassium were nearly normal at 133mEq/L and 4.9mEq/L respectively. His Liver Function Test was found to be normal.
His Dengue serology values were negative for NS1, IgG and IgM Antibodies. Alpha-1 antitrypsin levels were normal.
Radiology
ECHO showed Tachycardia (probably due to fever) mild AR with a normal LV function. HRCT showed consolidation with few fibrotic strands involving posterior segment of bilateral lower lobes suggestive of infectious aetiology.
Multiple lung cysts in bilateral lung fields and bilateral mild pleural effusion with thickening were present.
Management
Even post admission he had fever spikes for two days with a maximum temperature of 102.2F.On day 2 patient developed breathlessness.
The ABG showed type 1 respiratory failure with increased lactate levels. Patient was shifted to ICU for 2 days.
He was managed with antibiotics, anti-hypertensive, anti-diabetics, and nebulisation and mucolytic.
Cardiology opinion was taken and nil intervention was advised for his side as he had a normal LV function.
He was suspected to have a lower respiratory tract infection. HRCT was advised for him in view of recurrent lung infections.
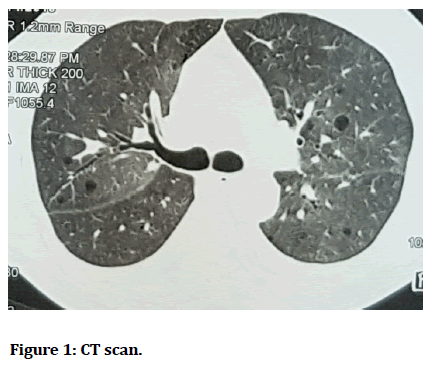
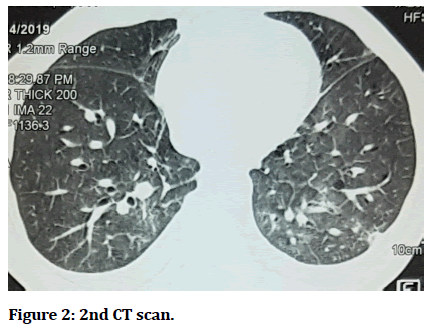
HRCT showed multiple lung cysts with lower lobe consolidation. Antibiotics were given for 5 days and the patient gradually improved and was discharged at request (Figures 1 and Figure 2).
Figure 1:CT scan.
Figure 2:2nd CT scan.
Follow up
Patient is under regular follow up.
Discussion
Cystic lung diseases often are multiple and are air filled lucencies surrounded by discrete walls in radiography and pathologically have a fibrous or epithelial outer wall. Various causes of lung cyst are existing like amyloidosis, congenital e.g. Brit Hogg Dube Syndrome, bronchopulmonary dysplasia, hypersensitivity pneumonitis, fungal causes like coccidioidomycosis, lymphoid inertial pneumonia, smoking related, staphylococcal pneumonia or primary and metastatic tumours e.g. lung adenocarcinoma etc. It is generally low attenuating area on high resolution computed tomography with normal lung around it. There are many lucencies that mimic cyst but are not a true cyst e.g. bullae, blebs, bronchiectasis, cavity and pneumatoceles etc. a true cyst wall will be less than 2mm. in thickness.
Sometimes patients with cystic lesions of lung may be asymptomatic and may thus be discovered incidentally on imaging. They may present with dyspnoea, cough, spontaneous pneumothorax, pleural effusion or any other on specific complaints. A thorough clinical and radiological examination is important in fixing the diagnosis. Various clues may be appreciated in history itself like history of underlying systemic disease like tuberous sclerosis complex or Sjogren syndrome, may point towards to a diagnosis of possible lymphangioleiomyomatosis or lymphoid interstitial pneumonia. A strong family history of renal cancer or pneumothorax may point towards Birt Hogg Dube Syndrome.
Lymphangioleiomyomatosis exclusively affects females and are mostly associated with tuberous sclerosis and is unlikely to be seen in a non-smoker. Pulmonary Langerhans cell histiocytosis is mostly seen in younger populations. HRCT helps in detailed characterization of the appearance and distribution of the cysts as well as identification of accompanying features.
Broadly Lung cysts may be divided into five specific categories on the basis of their location, number, distribution, and associated CT findings. These categories include: (1) sub pleuralcysts (solitary or multifocal) (2) parenchyma cysts without associated high-resolution CT scan findings (solitary or multiple) (3) parenchyma cysts seen in association with nodules; and (4) parenchyma cysts seen in association with ground-glass attenuation. These categories are arbitrary, in the sense,a disorder may be included in more than one category. An example of such a scenario occurs with PLCH which may present as a diffuse cystic involvement of the lungs with nodules or may have no radiographic abnormalities [1-6].
High end imaging like the HRCT can produce image with great detail and in different orientations and thus are important in diagnostic evaluation. It precisely defines the walls, extent, and distribution of lucent lung lesions, and it will also generate high-quality coronal and sagittal image reconstructions. Images obtained by using this technique are especially valuable for illustrating the relationship between cysts and peripheral airways. Treatment depends on the respective conditions. Solitary cysts may be easier to remove than multiple cysts. It is done if the patient is symptomatic and his daily life is affected.
References
- Gupta N, Vassallo R, Wikenheiser-Brokamp KA, et al. Diffuse cystic lung disease. Part II. Am J Respiratory Critical Care Med 2015; 192:17-29.
- Hansell DM, Bankier AA, MacMahon H, et al. Fleischner Society: Glossary of terms for thoracic imaging. Radiology 2008; 246:697.
- Anupam Kumar, Robert M Kotoff. Diagnostic approach to the adult with cystic lung disease. Topic 2020.
- Koba T, Arai T, Kitaichi M, et al. Efficacy and safety of transbronchial lung biopsy for the diagnosis of lymphangioleiomyomatosis: A report of 24 consecutive patients. Respirology 2018; 23:331-338.
- McCormack FX, Gupta N, Finlay GR, et al. Official American thoracic society/Japanese respiratory society clinical practice guidelines: Lymphangioleiomyomatosis diagnosis and management. Am J Respiratory Critical Care Med 2016.
- Koyama M, Johkoh T, Honda O, et al. Chronic cystic lung disease: diagnostic accuracy of high-resolution CT in 92 patients. Am J Roentgenol 2003; 180:827–835.
Author Info
Abhilash Nair*, Padma V, Rameez Raja, Murugaraj, Sarath Bhaskar S, Saketh Ramineni and Kannan Meera Devi
Department of General Medicine, Sree Balaji Medical College and Hospital, IndiaCitation: Abhilash Nair, Padma V, Rameez Raja, Murugaraj, Sarath Bhaskar S, Saketh Ramineni, Kannan Meera Devi, An Unusual Case of Recurrent Fever, J Res Med Dent Sci, 2021, 9(11): 263-265
Received: 06-Oct-2021 Accepted: 15-Nov-2021