Research - (2021) Volume 9, Issue 1
An Update on Urinary Tract Infection
V Naveen Kumar and Chitralekha Saikumar*
*Correspondence: Chitralekha Saikumar, Department of Microbiology, Sree Balaji Medical College and Hospital, Bharath Institute of Higher Education and Research, India, Email:
Abstract
Urinary tract infections are the commonest infection encountered in the community. In females, 1-3% schoolgirls are commonly affected by UTI and then markedly with the onset of sexual activity and it is the most common among women between 20-50 years of age. In males, acute asymptomatic infections occur in first year of life often in association with urologic abnormalities; thereafter UTI’s are unusual in male patients under the age of 50.
Keywords
UTI, Urinary tract disease, E. coli, Klebsiella pneumonia, Urethritis, Cystitis, Prostatitis
Introduction
Urinary tract disease has been depicted since antiquated occasions with the principal reported portrayal in the Ebers Papyrus dated to 1550 BC1.
It was depicted by Egyptians as "Sending forward warmth from the bladder 2. The principal instance of UTI was recorded by John Arden in Britain. Later in 1863, Pasteur has perceived pee as a decent culture media for microorganisms and related the nearness of microscopic organisms in the pee to manifestations, yet next to no advance was made in investigating the relationship until quantitative evaluations of the quantity of microbes in the pee of patients with urinary tract contamination were done by numerous creators. In 1995, Quantitative bacterial tallying more than 105 microorganisms for every ml was viewed as ture or critical bacteriuria by Kass et al. idea [1-4]
The anti-toxin time of Goodman and Gillman began with the disclosure of penicillin by Alexander Fleming in 1928. As indicated by Patricia A Bradford (2001)4 rise of protection from β lactam antibiotics started even before the first β-Lactam penicillin was created [5-8]. The first β-Lactam anti-infection was recognized in E. coli preceding the arrival of penicillin in medicinal practice. Numerous genera of gram-negative microorganisms have a normally happening chromosomally intervened β lactamase. These catalysts are thought to have developed from penicillin restricting protein with which they give some grouping homology. In the mid- 1940s saved by the requirement for hostile to bacterial operators in World War II penicillin was found not exclusively to fix disease yet in addition to have low poisonous quality. This advanced the assistant quest for comparative enemy of microbial specialists. Immediately after the penicillin got accessible for treatment; compounds ready to pulverize penicillin named penicillinases were identified in E. coli.
Datta et al. [5] portrayed the first plasmid interceded β lactamase in Gram negative microbes; TEM-1 was depicted in the mid- 1960s. According to Mederos et al. [6], the TEM- 1 protein was initially found in a solitary strain of E. coli disconnected from a blood culture from a patient named Temoniera in Greece, thus the Designation TEM [9-11].
Mendell et al7 clarified another regular plasmid interceded β lactamse found in Klebsiella pneumonia and E. coli; SHV1 (for sulfhdryl variable). The SHV 1 β-lactamase is chromosomally encoded in most of detaches in Klebsiella however is typically plasmid intervened in E.coli.
Numerous new β-lactam anti-toxins have been built up that were explicitly intended to be impervious to the hydrolutic activity of β lactamases. To defeat the β-lactamase intervened obstruction against penicillin delivered by Gram negative microorganisms, expansive range antiinfection agents like penicillin and ampicillin were acquainted with clinical practice in 1950s. In the year 1960s the first era cephalosporin arrived at the market. The expansive range penicillin and the first era cephalosporin remained the first line of treatment for right around 20 years. With each new class of β lactam anti-infection agents that have been utilized to treat patients, another β lactamase develops. This reason protection from all class of medications. One of the new class was Oximino-cephalosporin which turned out to be generally utilized for the treatment of genuine disease because of Gram negative microscopic organisms in 1980s. Protection from third era expanded range β-lactam anti-infection agents due to β-lactamases rose rapidly. As a result of increment range of movement against the Oximino-cephalosporins the chemicals were called Extended range β lactamases (ESBL). Today more than 150 distinctive ESBLs have been depicted.
Classification of urinary tract infection (UTI)
Lower UTI
Urethritis: Infection of the urethra which presents as dysurea and increased frequency of urination
Cystitis: Infection of the urinary bladder with features of dysurea, frequency, urgency, and supra pubic tenderness.
Acute urethral syndrome: Youthful explicitly dynamic ladies with dysurea, recurrence and desperation however yield life form < 105CFU/ ml
Prostatitis: Inection of the prostate.
Upper UTI
Pyelonephritis: inflammation of the kidney, parenchyma, calyx and pelvis caused by bacterial infection.
Urethritis: Rare, usually due to tuberculosis.
Types of UTI
Uncomplicated UTI alludes to contamination in a fundamentally and neurologically typical urinary tract.
Complicated UTI alludes to contamination in a urinary tract with useful or basic variations from the norm.
Relapses repeat of bacteriuria with the equivalent contaminating small scale life forms that was available before treatment was begun because of tirelessness of the living being in the urinary tract
Reinfection Recurrence of bacteria with microorganisms different from the original infective bacteria.
Asymptomatic bacteriuria Isolation of significant count of bacteria from a person without signs and symptoms of UTI.
Epidemiology of urinary tract infection
Urinary tract infections are the commonest infection encountered in the community. In females, 1-3% schoolgirls are commonly affected by UTI and then markedly with the onset of sexual activity and it is the most common among women between 20-50 years of age. In males, acute asymptomatic infections occur in first year of life often in association with urologic abnormalities; therafter UTI’s are unusual in male patients under the age of 50.
Pathogenesis of urinary tract infection (Figure 1) Route of Infection
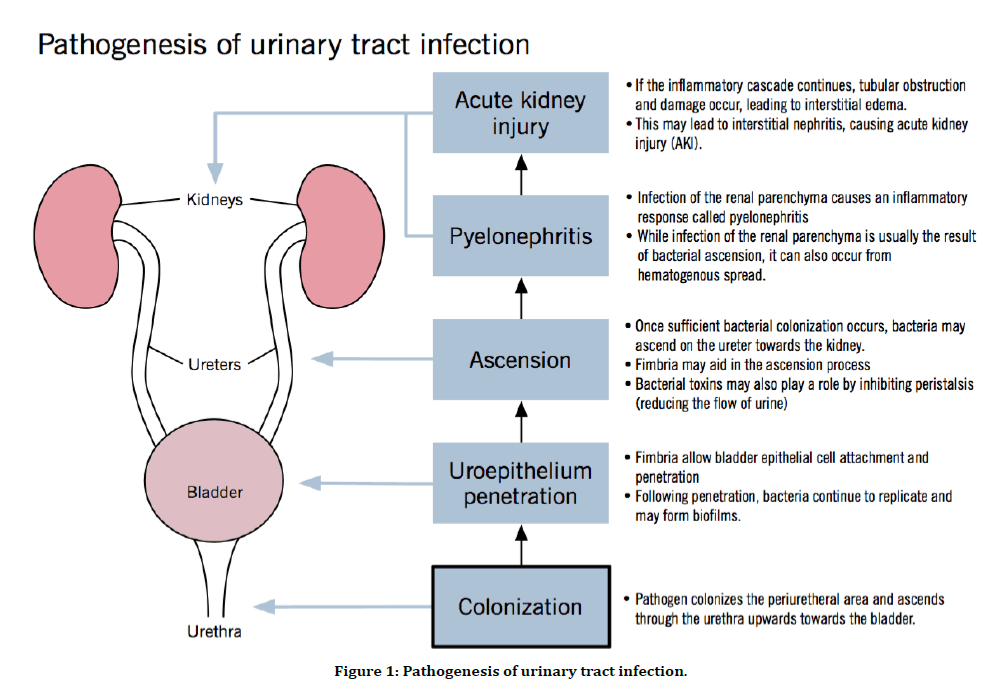
Figure 1. Pathogenesis of urinary tract infection.
Urine is a sterile fluid. The bacteria can invade and cause UTI via two major routes.
Ascending route.
Descending route.
Ascending route is the commonest route of infection in females. Catherterization and cystoscopy can cause UTI in both males and females by ascending route. Descending route of infection is caused by hematogenous spread as result of bacteremia.
Host defence against UTI
Urine is inhibitory to anaerobic bacteria and the low pH, high osmolarity, high organic acid content and constant flushing action of urine inhibit the bacterial colonization.
Valve like membranes at the junction of the bladder and ureter that prevents back flow of urine.
Immune system- Lipopolysaccharide of bacteria activates the host cell and release cytokines such as TNF α and TNF γ, activation of complement system.
Tamm-Horsfall protein or uromucoid serves as anti-adhesion factor by binding to E. coli, expressing type I fimbriae.
Defensins-group of small antimicrobial peptides produced by macrophages, neutrophils and cells in the urinary tract and attached to the bacterial cell eventually kill the bacteria.
Predisposing factors
The Following factors help in the development of UTI
Any variation from the norm of the urinary tract that impedes or eases back the progression of pee for instance Tumor, stricture and in men developed prostate can discourage the pee stream and make contamination hard to treat.
UTI happen in little level of newborn children because of inborn anomaly that requires medical procedure.
People on Immuno suppressive state like Diabetes Mellitus.
UTI is more common in females because of short urethra that opens into the moist introitus which is colonized by bacteria. For many women sexual intercourse precipitates UTI. Women using Diaphragm or spermicides as a contraceptive measure are likely to develop UTI than other forms of contraception.
Pregnant ladies are increasingly vulnerable to UTI's because of check to pee stream brought about by hormonal changes and furthermore because of weight on the urinary tract.
Post-menopausal women due to estrogen deficiency and with uterus prolapsed
Patients with Neurogenic bladder like spinal line damage, sexually transmitted disease, numerous sclerosis and diabetes mellitus or bladder diverticulum.
Conclusion
Virulence Factors for E. coli
Fimbria which binds on uroepithelium persists within the urinary tract. Three types are Type “S” fimbriae, Type “P” fimbriae and Type “D” fimbriae. Others are Toxins-haemolysin, siderophores. Uropathogenic strain specific proteins, protections, TIR domain containing proteins (tcp C) intimin, Colonising factor-CFA I, II and III.
Ethical Clearance
Nil.
Source of Funding
Self-funded.
Conflict of Interest
Nil.
References
- Al-Achi A. An introduction to botanical medicines, history science, use and dangers. Praeger publishers 2008; 126.
- Wilson J. Topley and Wilsons principles of bacteriology, virology and immunity. London Arnold 1990; 198.
- Kass E. Asymptomatic infections of the urinary tract. Trans Assoc Am Physicians 1955; 69:56-63.
- Bradford PA. Extended-spectrum β-lactamases in the 21st century: Characterization, epidemiology, and detection of this important resistance threat. Clin Microbiol Reviews 2001; 14:933-951.
- Datta N, Kontomichalou P. Penicillinase synthesis controlled by infectious R factors in Enterobactericeae. Nature 1965; 208:239-244.
- Mederios AA. Beta-Lactamases. Br Med Bull 1984; 40:18-27.
- Mandell Gerald L, Bennet John E. Principles and practice of infectious disease. 4th Edn 214-217.
- Mandell Gerald L, Bennet John E. Principles and practice of infectious disease. 6th Edn 2006; 1:242-905.
- Stamm Walter E. UTI pyelonephritis and prostatitis chapter 269. In : Harrison’s textbook of Internal Medicine 17th Edn 2005; 1820-1825.
- https://evolve.elsevier.com/cs/product/9780323354820?role=student
- Foxman B, Brown P. Epidemiology of UTI transmission and Risk factor incidence and costs. Infect Dis Clin N Am 2003; 17:222-241.
Author Info
V Naveen Kumar and Chitralekha Saikumar*
Department of Microbiology, Sree Balaji Medical College and Hospital, Bharath Institute of Higher Education and Research, Chennai, IndiaCitation: V Naveen Kumar, Chitralekha Saikumar, An Update on Urinary Tract Infection, J Res Med Dent Sci, 2021, 9 (1): 279-282.
Received: 09-Dec-2020 Accepted: 04-Jan-2021
