Research - (2021) Volume 9, Issue 8
Assessment of Motor Function of Phrenic Nerve in Type 2 Diabetes Mellitus Patients
*Correspondence: LM Sweety, Department of Physiology, Sree Balaji Medical College & Hospital Affiliated to Bharath Institute of Higher Education and Research, India, Email:
Abstract
Chronic Hyperglycemia in type 2 diabetic patients leads to phrenic nerve damage. Like other peripheral nerves phrenic nerve also gets affected and the magnitude of neuropathy is related to the duration of disease. Moreover this study has proved that phrenic neuropathy is the cause for restrictive lung disease in type 2 diabetes mellitus.
Keywords
Phrenic neuropathy, HyperglycemiaIntroduction
Diabetes Mellitus (DM) comprises of a common metabolic disorder that has the phenotype of increase blood sugar level. The metabolic deregulation associated with this causes secondary pathophysiologic changes in multiple organ system that causes some serious abnormalities on health.one such is affecting the lung function. Several studies have also said that lung becomes the target organ of DM. Reduced pulmonary function is mainly reported due to hyperglycemia. As the diaphragm of lungs are supplied by phrenic nerves respirator muscles receives the signals from these nerve impulse and any impairment of these muscles will reflect in retard pulmonary functions, which is reported to be common in DM. Hence this aims to evaluate the phrenic neuropathy in patients with type 2 diabetes mellitus [1-5].
Methodology
Patients of age group 35-55 were chosen for the study. Blood parameters such as glycosylated hemoglobin level (HbAlc), fasting and post prandial blood sugar levels. Was assessed were subjected to do pulmonary function test and motor nerve conduction of median and phrenic nerve .Motor phrenic conduction (MPN) Motor median nerve (MMN) studies were done.
Results
Figure 1 shows that the bar diagrams of the glycaemic index namely glycosylated haemoglobin and their comparison with duration of disease. The HbAlc values increases along with duration of disease. Figure 2 represents the bar diagram of the glycaemic indices namely fasting and post prandial blood sugar and their comparison with duration of disease. It can be clearly observed that as duration progresses the glycaemic status worsen.
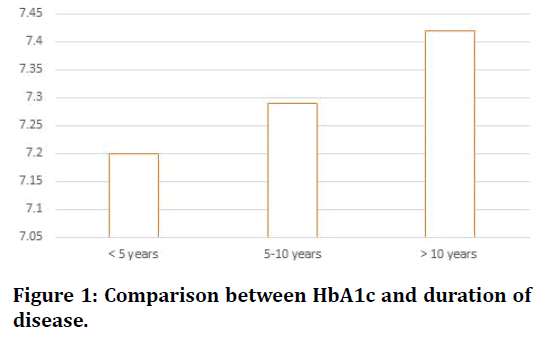
Figure 1. Comparison between HbA1c and duration of disease.
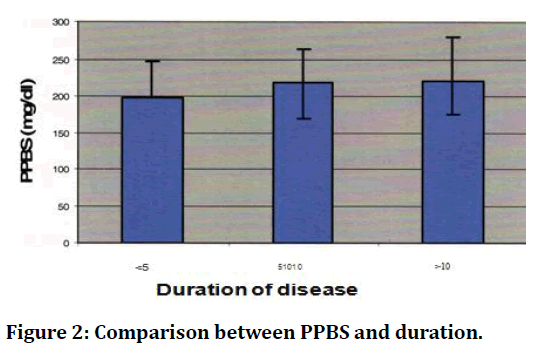
Figure 2. Comparison between PPBS and duration.
Table 1 shows the latency, amplitude, latency difference between wrist and elbow and nerve conduction velocity on right side of median nerve in diabetic patients of varying duration. All the values have been expressed in mean ± standard deviation. It is evident that as duration of disease progresses the latency increases whereas the amplitude and nerve conduction velocity decreases. Correlation between left motor median nerve conduction velocity and duration of diabetes mellitus. It can be observed that there exist a significant negative correlation between left side motor median nerve conduction velocity and duration of illness.
| Duration | Latency (ms) | Amplitude(mv) | Latency Diff (ms) | Conduction Velocity (ms) | ||
|---|---|---|---|---|---|---|
| Wrist | Elbow | Wrist | Elbow | |||
| < 5 years | 2.91 ± 0.66 | 7.1 ± 0.6 | 5.8 ± 3.9 | 4.7 ± 4.1 | 4.21 ± 0.38 | 49.9 ± 5.5 |
| 5 - 10 years | 3.1 ± 0.6 | 7.5 ± 0.9 | 6 ± 3.3 | 4.7 ± 2.4 | 4.4 ± 0.5 | 48.7 ± 5 |
| > 10 years | 4.5 ± 1.8 | 9.04 ± 2 | 2.48 ± 2.4 | 2.19 ± 2.4 | 4.5 ± 0.3 | 47.9 ± 3.6 |
Table 1: Right side motor median nerve conduction study in diabetic patients of varying duration.
Discussion and Conclusion
The latency of MPN conduction was increased in all the diabetic patients of varying duration; however the increase was significant in left side. As Hyperglycemia of the patients worsen, the latency of the MPN conduction increases. Our is in par with previous studies which has proved that Hyperglycemia, can alter the nerve function. It has been proved that restrictive pattern of lung disease in DM is due to Increase blood sugar level that leads pulmonary dysfunction. We evaluated the motor nerve conduction of both side median nerve and phrenic nerve, pulmonary function test of forty five type 2 diabetic patients (male - 15; female-30). We divided the patients into three groups depending upon the duration of illness as <5 years duration, 5-10 years duration and >10 years duration. Both the side motor conduction of the phrenic nerve showed decrease in the amplitude and increase in latency. There was a gradual decrease in the nerve conduction velocity of phrenic nerve as duration of the disease progressed. This proves that like other peripheral nerves phrenic nerve also gets affected in diabetes. From this study it was found that chronic Hyperglycemia in type 2 DM leads to phrenic nerve damage. Phrenic nerve gets affected and becomes the cause for restrictive lung disease in type 2 DM [6-10].
References
- Guyton AC, Hall JE. Text book of Medical Physiology. 11th Ed 2006; 972.
- Mohan V, Sandeep S, Deepa R, et al. Epidemiology of type 2 diabetes: Indian scenario. Indian J Med Res 2007; 125:217-230.
- Doaa Hanafy Mahmoud, Magdy Helmy Megallaa. Study of the short term impact of intensive glycemic control on nerve conduction in type 2 diabetic patients. Alexandria Bulletin 2009; 45:119-124.
- Tkac I, Bril V. Glycemic control is related to the electrophysiologic severity of diabetic peripheral sensorimotor polyneuropathy. Diabetes Care 1998; 21:1749-52.
- Macklem PT. The act of breathing. In: Roussos, Edn. The thorax. New York: Marcel Dekker, 1995; 445-54.
- Younes M, Remmers J. Control of tidal volume and respiratory frequency. In: Hornbein TF, Edn. Lung biology in health and disease: Regulation of breathing. New York: Marcel Dekker, 1981; 621-71.
- Berger AJ. Control of breathing. In: Murray J, Nadel J, Eds. Textbook of respiratory medicine. New York: WB Saunders,1988; 49-166.
- Goldman MD. Lung dysfunction in diabetes. Diabetes Care 2003; 26:1915-8.
- Hsia CC. Recruitment of lung diffusing capacity: Update of concept and application. Chest 2002; 122:1774-83.
- Meo SA, Al-Drees AM, Arif M, et al. Lung function in type 2 Saudi diabetic patients. Saudi Med J 2006; 27:338-343.
Author Info
Department of Physiology, Sree Balaji Medical College & Hospital Affiliated to Bharath Institute of Higher Education and Research, Selaiyur, Chennai, Tamil Nadu, IndiaCitation: LM Sweety, Assessment of Motor Function of Phrenic Nerve in Type 2 Diabetes Mellitus Patients, J Res Med Dent Sci, 2021, 9(8): 124-125
Received: 16-Jul-2021 Accepted: 10-Aug-2021
