Research - (2022) Volume 10, Issue 7
Camouflage Treatment of Skeletal Class III Malocclusion Associated with Anterior Mandibular Displacement, Deep Over Closure and Crowding
Umi Mardhiyyah Mat Ali1* and Khairil Aznan Mohamed Khan2
*Correspondence: Umi Mardhiyyah Mat Ali, Orthodontic Unit, School of Dental Sciences, Universiti Sains Malaysia, Health Campus, 16150, Kubang Kerian Kelantan, Malaysia, Email:
Abstract
This case report illustrates the successful of non-extraction orthodontic camouflage treatment in an adult patient with skeletal Class III malocclusion associated with anterior mandibular displacement, deep overclosure, and moderate crowding on the upper arch. The treatment involved the usage of protraction archwire and lower removable appliance with a posterior bite plane. The procedure entails eliminating the displacement to restore the mandible's natural functional position and relieving crowding without compromising the periodontium, with good anchoring control of the molars. At the end of treatment, the improvement of the occlusal relationship was achieved with a good facial profile and reduction of chin prominence.
Keywords
Class III malocclusion, Camouflage treatment, Mandibular displacement
Introduction
The prevalence of malocclusion varies across country, ethnicity, and race. For an Angle Class III malocclusion, a high prevalence rate has been reported in the Malaysian population, especially in Malay races [1]. In skeletal Class III patient, the sagittal issue appears exacerbated when combined with mandibular displacement due to incisal interference. The skeletal appearance of a patient becomes prominent when the mandible slides forward during maximum intercuspation to avoid premature contact. Another impact of anterior mandibular displacement, also known as pseudo-class III, is an increase in reverse over jet and a decrease in anterior face height [2]. Hence, anterior mandibular displacement could be one of the prognostic indicators for orthodontic camouflage in Class III malocclusion [3]. Proclination of the maxillary incisors and retroclination of the mandibular incisors are common orthodontic camouflage treatments that improve overall occlusion. However, they worsen the profile by increasing apparent chin prominence and significantly compromising smile esthetics [4]. Therefore, active clockwise rotation of the mandible is anticipated during dental compensation to improve facial convexity and chin prominence [5]. This case report illustrates the successful orthodontic camouflage treatment in an adult patient with skeletal Class III malocclusion associated with anterior mandibular displacement, deep overclosure, and moderate crowding on the upper arch. The treatment involved the usage of protraction archwire and lower removable appliance with a posterior bite plane.
Case Presentation
An 18-year-old Malay female was referred to the Orthodontics Department, Faculty of Dentistry, Universiti Kebangsaan Malaysia. Her main complaint was the unaesthetic appearance of her front teeth and under bite. She reported being in good general health with no history of systemic disease. The initial extraoral examination revealed mesofacial features with a concave profile and facial symmetrical (Figure 1). The intraoral examination showed moderate crowding on the upper arch, mild crowding on the lower arch, anterior cross bite with reverse over jet (-2mm) and increased overbite (50%). The upper midline shifted to the right by 3 mm. Canine relationship Class II ¼ unit bilaterally and molar relationship Class I bilaterally (Figure 2). However, during a functional examination, the patient has premature contact and interference of the anterior teeth in retruded contact position (RCP) (Figure 3). Anterior mandibular displacement was present when patient was in maximum interdigitation or intercuspal position (ICP).
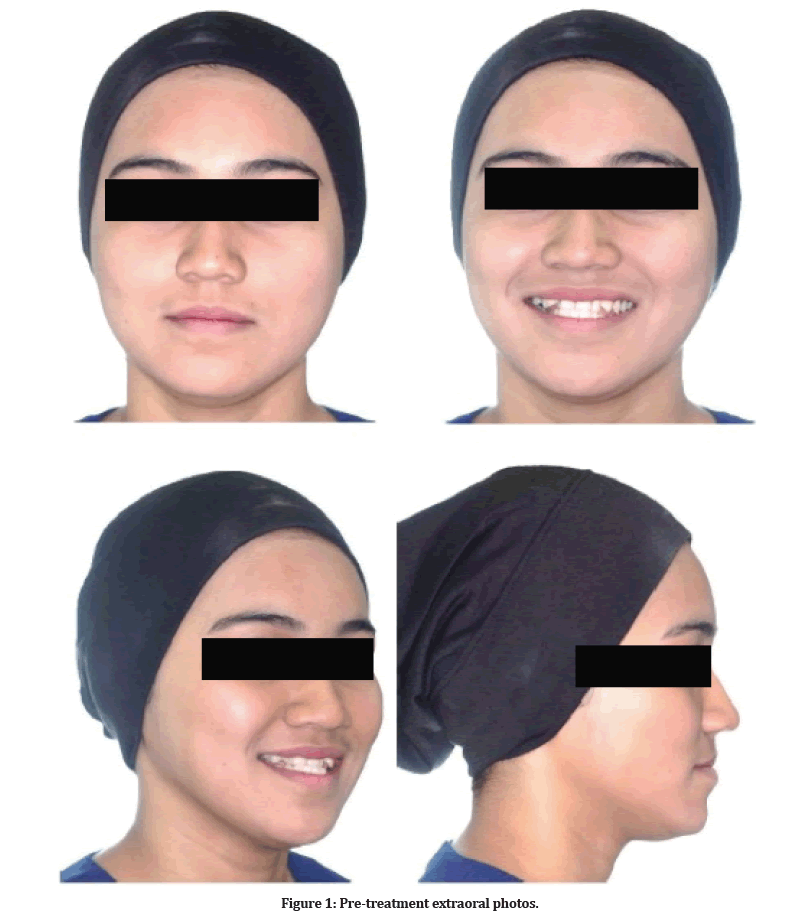
Figure 1: Pre-treatment extraoral photos.
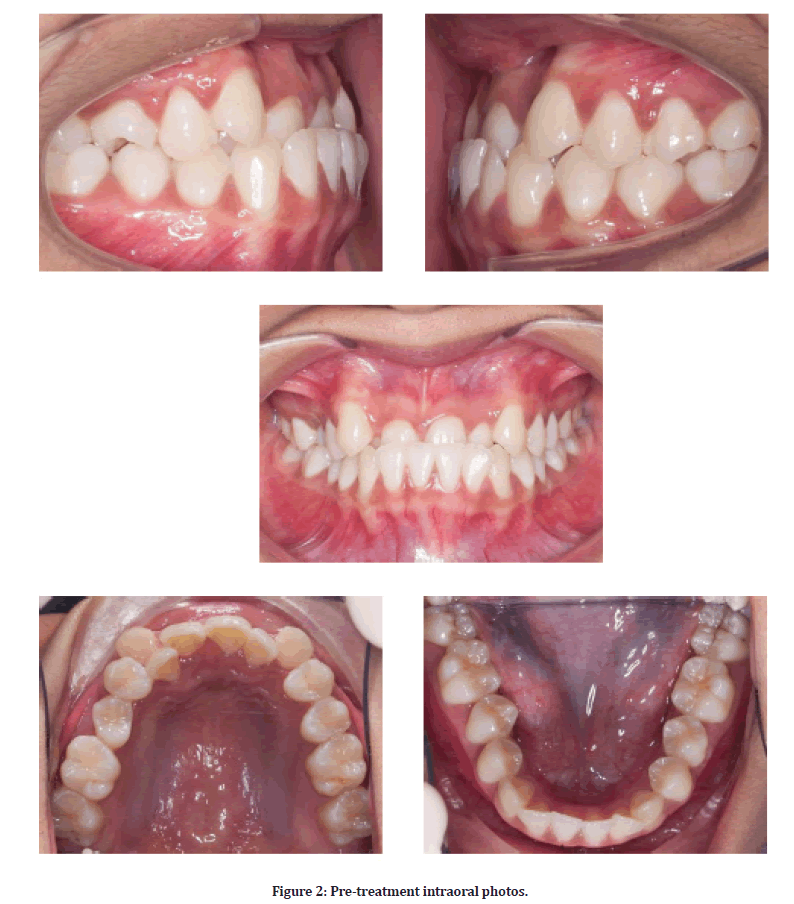
Figure 2: Pre-treatment intraoral photos.
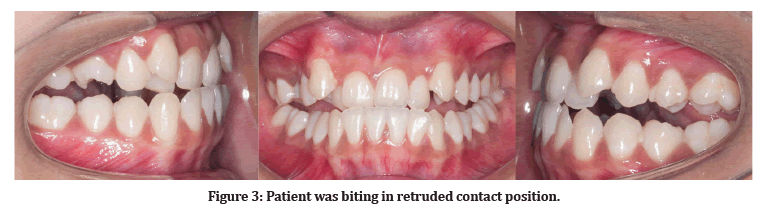
Figure 3: Patient was biting in retruded contact position.
The lateral Cephalometric analysis showed that the value of SNA (85°) and SNB (87°) represent the prognathic maxilla and mandible. However, this was not the true representation of the mandible as the patient exhibited anterior mandibular displacement where the B point had been moved forward. Patient has a moderate Class III skeletal pattern as reflected by her reduced ANB of -2° (Figure 4 and Table 1).
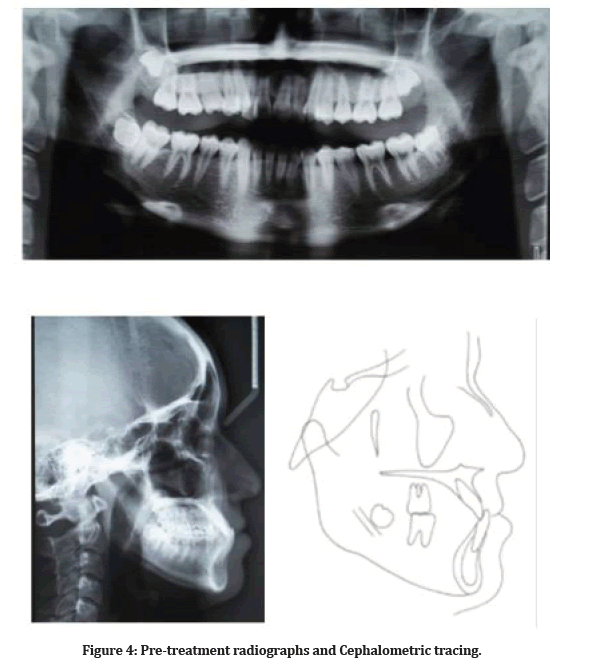
Figure 4: Pre-treatment radiographs and Cephalometric tracing.
Treatment objectives
The objectives of the treatment were (1) Eliminate the anterior mandibular displacement and achieve a good skeletal relationship (2) Relief crowding on both arches (3) Improve soft tissue balance and smile aesthetics, (4) Establish stable functional occlusion.
Treatment plan and alternatives
The patient was informed about several treatment options. Non-extraction, camouflage orthodontic treatment was chosen for this patient, with maxillary expansion using a protraction archwire and a lower removable appliance with posterior bite plane to disocclude front teeth during upper tooth protraction. Another treatment plan was extraction and surgical intervention, as this approach will correct the sagittal discrepancy. However, the patient refused to accept the plan due to the additional cost burden, the need to undergo surgery, and the potential risks.
Treatment process
Treatment was initiated with alignment of upper arch first, bonded-up with pre-adjusted edgewise fixed appliances (MBT prescription), 0.022”x0.028” arch wire slot (American Orthodontics). No bracket was put on tooth 12 and 22. Initial archwire inserted was 0.014” nickel-titanium (NiTi) (Figure 5A). Lower removable appliance with posterior bite plane was issued to allow disocclusion on anterior segment during alignment phase (Figure 5B). After the alignment, 0.018” stainless steel wire was used with Omega loop constructed mesial to upper first molars bilaterally. Protraction of labial segments was done by activating the loops (Figure 5C). Creating the space for palatally displaced 12 and 22 was done by NiTi open coil spring, interproximal stripping from canine to canine, and also space gain when derogating upper second premolar tooth (Figure 5D). At 10 months, lower arch was bonded up and 0.014” NiTi archwire with cinch back was placed. During this time, interproximal stripping also done on lower anterior teeth to gain some space to align lower incisors. Towards the end of treatment, diagonal elastic was used to correct the centerline (Figure 5E and 5F). After 26 months, the upper and lower fixed appliances were removed. Upper and lower Hawley retainers were fitted and instruction for full time wear for the first 6 months and nighttime wear for the next 6 months was given to patient.
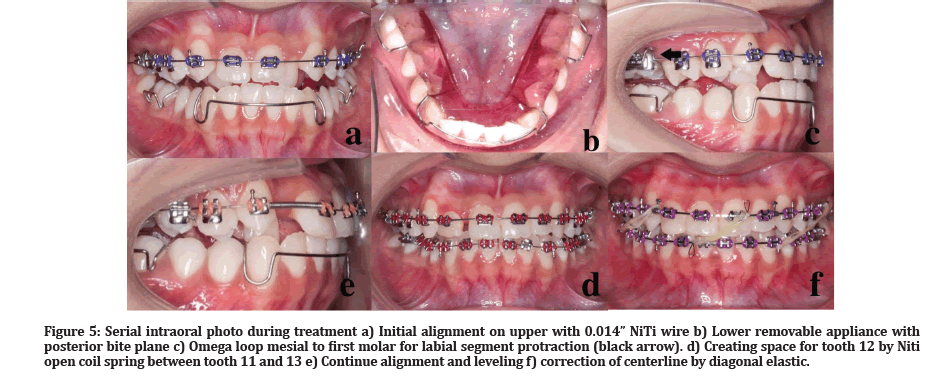
Figure 5: Serial intraoral photo during treatment a) Initial alignment on upper with 0.014” NiTi wire b) Lower removable appliance with posterior bite plane c) Omega loop mesial to first molar for labial segment protraction (black arrow). d) Creating space for tooth 12 by Niti open coil spring between tooth 11 and 13 e) Continue alignment and leveling f) correction of centerline by diagonal elastic.
Treatment result
Facial aesthetic was improved. The slight protrusion of the upper lip and decreased nasolabial angle was expected after proclination of the upper incisors however this gave good support to the upper teeth. Improvement of facial aesthetics makes her profile more pleasing (Figure 6). For smile aesthetics, the result showed that the smile arc followed the curvature of the lower lip. This case finished with a good upper incisal display at rest and smiling. Minimal skeletal growth occurred throughout treatment, possibly due to remodeling of the skeletal structure (Figure 7). The moderate skeletal III pattern has improved as the SNB changed after the elimination of anterior displacement. The postured forward B point during pre-treatment showed that it was not a true skeletal discrepancy (Table 1).
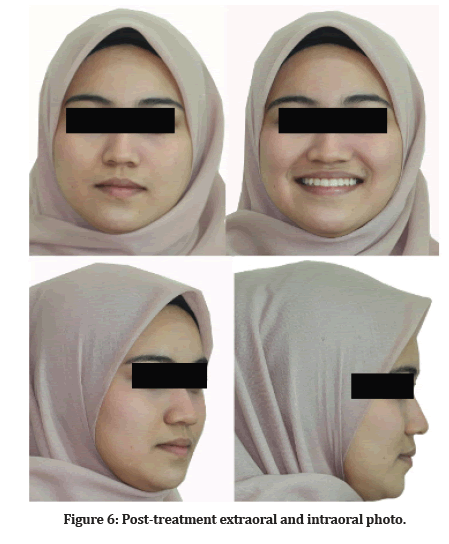
Figure 6: SPost-treatment extraoral and intraoral photo.
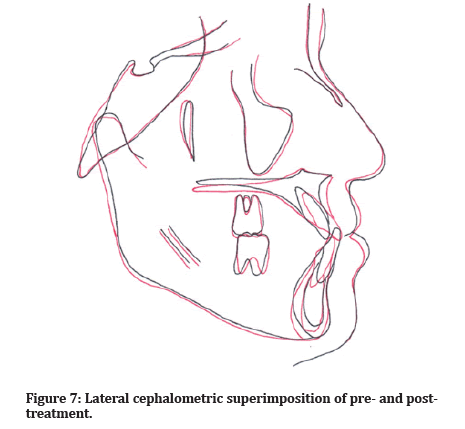
Figure 7: Lateral cephalometric superimposition of pre- and post-treatment.
| Variable | Pre-tx | Post-tx |
| SNA | 85° | 86° |
| SNB | 87° | 84° |
| ANB | -2° | 2° |
| MMPA | 26° | 27° |
| Face height ratio | 53% | 55% |
| SN to maxillary plane | 5° | 5° |
| Upper incisor to maxillary plane | 113° | 120° |
| Lower incisor to mandibular plane | 85° | 85° |
| Interincisal angle | 136° | 125° |
| Wits appraisal | -3 mm | -1 mm |
| Lower incisor to APo line | 5 mm | 2 mm |
Table 1: Cephalometric summary.
This is a camouflage case whereby the reversed over jet was corrected by protraction of upper incisors. Even though the upper incisors inclination changed more than average value, they are still within the envelope of the bone, keeping good healthy gingiva margin and clinically look upright and good lip support. A Class I incisor and canine relationship with positive overbite and over jet has been established. Upper and lower molars remained static and maintained a Class I molar relationship. Lower midline finished 0.5mm to the right of the mid-sagittal plane, which was acceptable. Overall good alignment of the upper and lower arch was achieved. Tooth 12 was built-up with composite resin due to severe attrition. Upper and lower Hawley retainer were planned to achieve good settling after debonding. The treatment is expected to be stable as over jet and overbite are adequate to maintain the correction.
Discussion
Correct diagnosis of a pseudo-class III malocclusion has an impact on orthodontic treatment strategy. In growing patients, evaluation and correction of the pseudo-Class III malocclusion should be done early, especially during the developmental stage. If uncorrected, this condition normally leads to a skeletal problem during adulthood due to the impact of muscles on mandibular growth [6]. Ideally, surgical approach will be proposed to correct severe Class III dental and skeletal discrepancies in adults, initiated by pre-surgical orthodontic for dental decompensation and arch coordination. In this case, the patient exhibits Class III dental and skeletal malocclusion, with pre-existing premature contact on anterior teeth. During maximum intercuspation, the mandible displaces anteriorly, exacerbating the severity of Class III malocclusion in this patient. Therefore, distinguishing between pseudo-Class III and actual skeletal Class III was critical in developing an appropriate treatment approach.
As a result, rather than using a surgical technique, dental camouflage treatment was planned in consideration of the limitations revealed by previous study [7]. The common camouflage option for Class III malocclusion was to extract upper second premolars and lower first premolars. This option will improve the proclination of upper incisor as well as relieve the crowding on the upper arch. However, extraction of premolars would worsen the facial profile with prominent chin, especially on the lower arch. Therefore, a non-extraction was considered to improve soft tissue balance and smile aesthetics.
The lower removable appliance with posterior bite plane was constructed to disocclude the anterior teeth during establishment of positive overjet. This type of appliance was chosen considering the deep overbite of 50%, thus around 4mm thickness of the posterior block needed to fully eliminate the occlusal interference on the anterior teeth [8]. The discrepancy between intercuspal position (ICP) and retruded contact position (RCP) improved when the mandible returns to its natural functional position without any forward movement when using the bite plane. The effect also to eliminate the neuromuscular response that the mandible had learned to produce when there were occlusal interferences [9]. The mandible was rotated clockwise to improve the face convexity and chin prominence, as well as the occlusal relationship.
The alignment and sagittal correction of the anterior cross bite was the first step in the treatment. The anterior segment was protracted using a protraction archwire with omega loops and anchorage reinforcement from the molars. During a few visits, the omega loop was also activated to further protract the anterior segments until positive over jet was established. After cross bite elimination, lower arch was bonded up and interproximal stripping on upper and lower was planned to gain some space to relieve the crowding. Lower incisors inclination remained the same throughout treatment, meanwhile upper incisors inclination increase to the upper limit of 120° [7] to the cranial base. All orthodontic tooth movement is accomplished with no negative effects on the periodontium detected. For retention, Hawley retainer was prescribed to allow further occlusal settling of posterior teeth. The overbite, over jet correction and good posterior intercuspation are sufficient for maintaining the correction and stability without any extra retention regime [10].
Conclusion
In this case report, it was shown that Class III malocclusion associated with anterior mandibular displacement and deep overclosure can be effectively treated with good diagnosis and treatment planning. Elimination of the anterior cross bite by proclination of upper anterior teeth and achieved correct functional occlusion in the beginning of treatment is crucial before proceeding with lower arch alignment.
References
- Elfseyie M, Hassan MIA, Al-Jaf NMA. Prevalence of malocclusion and occlusal traits of Malay adults (18-23 years) in Shah Alam, Malaysia. Int J Dent Res 2020; 5:81â??5.
- Reyes A, Serret L, Peguero M, et al. Diagnosis and treatment of pseudo-class III malocclusion. Case Rep Dent 2014; 2014:1â??6.
- Cobourne M, DiBiase A. Handbook of Orthodontics. Elsevier Ltd; 2016.
- Ngan P, Moon W. Evolution of class III treatment in orthodontics. Am J Orthod Dentofac Orthop 2015; 148:22â??36.
- Jang W, Shin C, Hwang S, et al. Nonsurgical treatment of an adult with a skeletal Class III malocclusion combined with a functional anterior shift, severely over closed vertical dimension, and a reverse smile. Am J Orthod Dentofac Orthop 2020; 157:561â??570.
- Santos-Pinto A Dos, Paulin RF, Melo ACM. Pseudo-class III treatment with reverse traction: Case report. J Clin Pediatr Dent 2001; 25:267â??74.
- Burns NR, Musich DR, Martin C, et al. Class III camouflage treatment: What are the limits? Am J Orthod Dentofac Orthop 2010; 137:9.e1-9.e13.
- Singh G, Gupta H, Rathi A, et al. The use of bite raisers in orthodontic treatment-A review of literature. Acta Sci Dent Sci 2021; 5:219â??28.
- Alogaibi YA, Al-Fraidi AA, Alhajrasi MK, et al. Correction of a class III malocclusion with a functional shift and severe crowding. Case Rep Dent 2020; 2020.
- https://www.bos.org.uk/Portals/0/Public/docs/Membership/clinicalguidelinesretentionfinalversionaugust2013.pdf
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Author Info
Umi Mardhiyyah Mat Ali1* and Khairil Aznan Mohamed Khan2
1Orthodontic Unit, School of Dental Sciences, Universiti Sains Malaysia, Health Campus, 16150, Kubang Kerian Kelantan, Malaysia2Discipline of Orthodontics, Centre for Family Oral Health, Faculty of Dentistry, Universiti Kebangsaan Malaysia Jalan Raja Muda Abdul Aziz, 50300 Kuala Lumpur, Malaysia
Received: 23-Jun-2022, Manuscript No. JRMDS-22-67757; , Pre QC No. JRMDS-22-67757(PQ); Editor assigned: 27-Jun-2022, Pre QC No. JRMDS-22-67757(PQ); Reviewed: 12-Jul-2022, QC No. JRMDS-22-67757; Revised: 15-Jul-2022, Manuscript No. JRMDS-22-67757 (R); Published: 22-Jul-2022
