Research - (2020) Volume 8, Issue 6
Clinical and Anti-Inflammatory Effect of Curcumin Oral Gel as Adjuncts in Treatment of Periodontal Pocket
Hayder Thabit Farhood* and Basma Ghafori Ali
*Correspondence: Hayder Thabit Farhood, Department of Periodontics, College of Dentistry, University of Baghdad, Iraq, Email:
Abstract
Background: The periodontal disease is among the most popular medical situations which might affect humans. Periodontal pocket that is known as a pathologically extended gingival sulcus which is one of most essential clinical characteristics of the periodontal disease. The scaling, the root planning and the polishing are the golden ordinary procedures for the management. An adjunct to scaling and root planning has been introducing as curcumin. Curcumin possess antioxidant, anti-inflammatory, and anti-microbial properties.
Aim/ Objectives: To estimate the effectiveness of sub gingival application of curcumin oral gel as adjuncts for the SRP in the management of (5–7 mm) periodontal pockets on clinical periodontal parameters. plaque index, gingival index, bleeding on probing pocket depth and relative attachment level.
Materials and Methods: 20 patients of both gender and aged from 21 to 45 years. The patients with periodontitis (stage II/III, grade A-C) and pockets depth 5-7mm bilateral of upper jaw only which randomly selected. Split mouth technique followed, one side consider as control group sites that receive SRP alone, the other side marked as test group side that receive twice application of curcumin oral gel as adjunct to SRP with one week interval. Plaque and gingival indices were recorded on three visits while bleeding on probing, probing pocket depth and relative attachment level were measured for each patient at baseline, and 1-month interval.
Results: For intra group ,in the 3rd visit, means of PLI, GI, PPD, and RAL presented statistical significant decrease in test and control sites compared with baseline visit, but no statistical significant differences in these parameters in the 3rd visit between test and control sites (Inter group). Bleeding on probing in test sites group was significantly decreased in the 3rd visit compared with baseline visit, but in control sites group no statistical significant change in the 3rd visit compared with baseline visit.in inter group comparison a statistical significant differences in BOP between test and control sites.
Conclusion: Curcumin shows a potent effect in improving the outcomes of clinical parameters when compared with SRP. Curcumin can be a promising adjunctive therapeutic agent; it showed a good capability in influencing the gingival health by assessing the clinical parameters
Keywords
Anti-inflammatory, Curcumin gel, Periodontal pocket
Introduction
Periodontal pocket that is known as a pathologically extended gingival sulcus which is one of most essential clinical characteristics of the periodontal disease [1]. The aim of the periodontal management that is to stop inflammation, avoid infection to the underlying tissue, and generate favorable circumstances for healing and renewal of the periodontal tissue [2]. Scaling and root planning it is a keystone for the periodontal management and goals for destroying the plaque accumulation that enhance the developing and progressing of the periodontitis [3].
The antibiotic and the non-steroidal antiinflammatory medicines have been studied as adjunct for periodontal treatment. Until now, such medications are associated with systemic alteration, antimicrobial resistance and gastrointestinal intolerance [4-6].
Researchers find that bacteria which lead to the periodontal infections can be inhibited with using of phytotherapeutic agents. Therefore, there is a marked attention in the improvement of phytotherapeutic agents as an adjunct for the periodontal treatment [7].
Polyphenols are the group of the phytochemicals which are substantial source to the antioxidants. Between polyphenols that most broadly utilized agent is turmeric, which is an ancient spice extracted of rhizome of Curcuma longa, an eternal plant which is part from Zingiberacae (ginger) family.
Turmeric has a sort of compounds including the demethoxycurcumin, curcuminoid consist of curcumin, and bisdemethoxycurcumin [8]. Curcumin possess antioxidant, antiinflammatory, anti-carcinogenic, antimicrobial, astringent properties [9].
Mechanical treatment when joined with locally deliver system such as the curcumin oral gel decreases microorganisms and clinical parameters also improve in comparison to SRP alone [10].
Aim/Objectives
For comparing the effectiveness of the curcumin oral gel as an adjunctive for sub gingival scaling and root planing with the effects accomplished by using sub gingival scaling and root planing only for treating of (5–7 mm) the periodontal pocket on the clinical periodontal Parameters: Plaque index, gingival index, bleeding on probing, probing pocket depth and relative attachment level.
Materials and Methods
Study design/sample
This a clinical random split mouth interventional study was conducted from November 2019 to March 2020 at Al Hayderia general hospital in al- Najaf city/Iraq. The study approved by ethical committee/college of Dentistry/University of Baghdad, follow the guidelines of Helsinki and Tokyo for humans (reference no. 135619 in 2/12/2019). A total of 20 Iraqi patients aged 21-45 years, 9 males and 11 females who encountered the eligibility criteria were precipitated in this study for the non-surgical treatment of periodontitis (stage II/III, grade A-C) with pocket depth (PPD) 5-7 mm. A total of 40 sites were treated.
Inclusion criteria
Patients with periodontitis (stage II/III, grade A-C) with pocket depth (PPD) 5-7 mm.
No history of any systemic condition.
Patients able to follow the required instructions.
Willing to sign an informed consent form.
Did not receive any antibiotic therapy and periodontal therapy in the last 2 months.
Exclusion criteria
Patients with systemic disease that may affect the periodontal tissue.
Smokers and tobacco users.
Pregnant and lactating women.
Patients refused to write an informed consent form and uncooperative ones who refused to follow the required instructions.
Patients taking certain medications that may influence periodontal health status.
Patients with overhang filling.
Procedure
A total of 20 Iraqi patients aged 21-45 years, 9 males and 11 females who encountered the eligibility criteria were precipitated in this study for management of periodontitis non surgically. From each patient (2) sites were selected per patient in upper jaw. One site (control) selected randomly and received SRP only, the other site is (test site) received curcumin gel in addition to SRP (Curenext oral gel®, Abbott heath care, Abbott Health, Mumbai, Mh, India, each gm gel contains curcuma longa extract (Rhizome) 10.00 mg). A split mouth technique was followed and the study was conducted in four visit: patient preparation visit (performing supragingival scaling, impression for stent construction for reliability in measuring RAL, and motivation and oral hygiene instructions), baseline visit day 0 (measuring the clinical parameters: PLI (plaque index), GI (gingival index), BOP (bleeding on probing), PPD (probing pocket depth) and RAL (relative attachment level), performing SRP, and placing the curcumin gel in test pocket only and covering pockets by periodontal pack), second visit after one week (removing the pack, measuring PLI and GI, and second application of gel) and third visit after one month (measuring clinical parameters: PLI GI, BOP, PPD, and RAL (Figure 1).
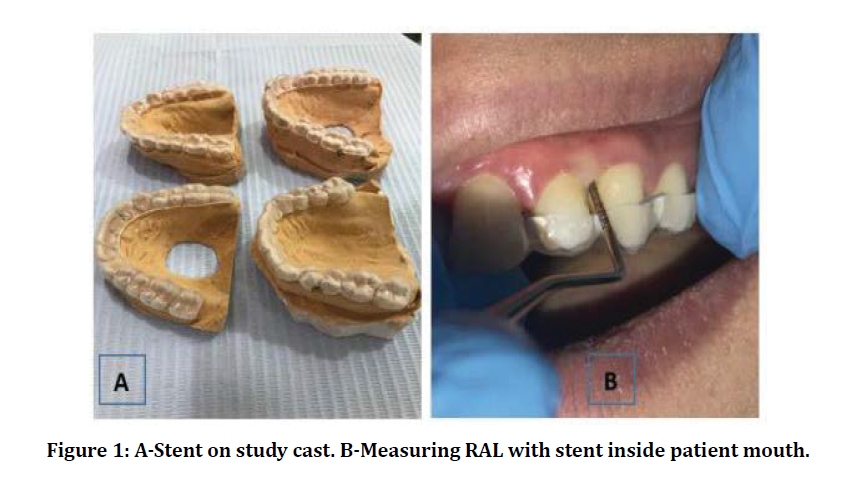
Figure 1: A-Stent on study cast. B-Measuring RAL with stent inside patient mouth.
Results
First visit (Baseline)
Table 1 reveal mean ± SE of PLI, GI, PPD, and RAL at base line visit in both test and control sites group. Means of PLI (1.400 versus 1.350), GI (1.950 versus 2.000), PPD (5.550 versus 5.300) and RAL (8.300 versus 8.100) respectively. Statistically anon significant differences appeared regarding these periodontal parameters between test and control side groups.
| Variables | Groups | T | P value | ||||
|---|---|---|---|---|---|---|---|
| Test | Control | ||||||
| Mean | ±SE | Mean | ±SE | ||||
| PLI | 1.4 | 0.152 | 1.35 | 0.15 | 0.234 | 0.816 | NS |
| GI | 1.95 | 0.088 | 2 | 0 | 0.567 | 0.574 | |
| PPD | 5.55 | 0.153 | 5.3 | 0.128 | 1.252 | 0.218 | |
| RAL | 8.3 | 0.179 | 8.1 | 0.161 | 0.831 | 0.411 | |
Table 1: The descriptive and statistical test of periodontal parameters between test and control site groups in the baseline visit.
Regarding BOP parameter for both test and control sites at the baseline visit a non-significant association appear using Chi square test between bleeding on probing score 0 and score 1 in both groups as in Table 2. Among the 20 test sites eighteen with score 1 BOP and the rest two with score 0.
| Groups | Chi square | P value | Total | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Test | Control | ||||||||
| N. | % | N. | % | N. | % | ||||
| BOP | 1 | 18 | 90 | 18 | 90 | 0 | 1 [NS] | 36 | 90 |
| 0 | 2 | 10 | 2 | 10 | 4 | 10 | |||
Table 2: Comparison between bleeding on probing in the baseline level in each study group.
In the 2nd and 3rd visits
Plaque index (PLI)
Tables 3 and 4 intra group comparison presented with non-statistical significant change in Means of PLI in the 2nd visit compared with the baseline data for both test and control sites intra group (1.550 versus 1.400, P=.419; and 1.550 versus 1.350, P=0.330 respectively). Also, for intergroup comparison, no-statistically significant difference in the 2nd visit between test and control sites (1.550 versus 1.550, P=1.000 respectively).
| Groups | T test | P value | |||||
|---|---|---|---|---|---|---|---|
| Test | Control | ||||||
| Mean | ± SE | Mean | ± SE | ||||
| PLI1 | 1.4 | 0.152 | 1.35 | 0.15 | 0.234 | 0.816 | NS |
| PLI2 | 1.55 | 0.17 | 1.55 | 0.17 | 0 | 1 | |
| PLI3 | 0.3 | 0.105 | 0.15 | 0.082 | 1.125 | 0.267 | |
Table 3: Comparison between PLI in the baseline level, 2nd, and 3rd visits between study groups.
| Groups | Mean | ± SE | Paired T test | P value | |
|---|---|---|---|---|---|
| Test | PLI1 | 1.4 | 0.152 | 0.825 | 0.419 NS |
| PLI2 | 1.55 | 0.17 | |||
| PLI1 | 1.4 | 0.152 | 6.85 | 0.000 HS | |
| PLI3 | 0.3 | 0.105 | |||
| PLI2 | 1.55 | 0.17 | 7.804 | 0.000 HS | |
| PLI3 | 0.3 | 0.105 | |||
| Control | PLI1 | 1.35 | 0.15 | 1 | 0.330 NS |
| PLI2 | 1.55 | 0.17 | |||
| PLI1 | 1.35 | 0.15 | 6.99 | 0.000 HS | |
| PLI3 | 0.15 | 0.082 | |||
| PLI2 | 1.55 | 0.17 | 8.304 | 0.000 HS | |
| PLI3 | 0.15 | 0.082 | |||
Table 4: Comparison between PLI in the 2nd and 3rd visits and baseline level change in each group.
In the 3rd visit, means of PLI presented statistical high significant decrease in test and control sites intra group compared with 2nd and baseline visit (0.300 versus 1.550 and 1.400, P=0.000; and .150 versus 1.550 and 1.350, P=0.000 respectively).
But for inter group comparison no-statistically significant differences in the 3rd visit regarding PLI in test and control sites (0.300 versus 0.150, P=0.267respectively).
Gingival index (GI)
For intra group comparisons between GI in the 2nd and 3rd visits with baseline level in each study group. Means of gingival index presented no statistically significant change in the 2nd visit compared with the baseline data for both test and control sites (2.150 versus 1.950, P=0.214; and 2.200 versus 2.000, P=0.214 respectively). In the 3rd visit, means of GI presented highly statistical significant decrease in test and control site compared with 2nd and baseline visit (1.050 versus 2.150 and 1.950, P=0.000; and 1.250 versus 2.200 and 2.000, P=0.000 respectively) (Tables 5 and 6). Intergroup comparisons reveal no-statistical significant differences in the GI scores in 2nd visit between test and control sites (2.150 versus 2.200, P=0.828 respectively). GI scores also presented with no statistical significant differences in the 3rd visit between test and control sites (1.050 versus 1.250, P=0.083 respectively).
| Groups | T | P value | |||||
|---|---|---|---|---|---|---|---|
| Test | Control | ||||||
| Mean | ± SE | Mean | ± SE | ||||
| GI1 | 1.95 | 0.088 | 2 | 0 | 0.567 | 0.577 | NS |
| GI2 | 2.15 | 0.167 | 2.2 | 0.156 | 0.219 | 0.828 | |
| GI3 | 1.05 | 0.05 | 1.25 | 0.099 | 1.798 | 0.083 | |
Table 5: Comparison between GI in the baseline, 2nd and 3rd visits between study groups.
| Groups | Mean | ± SE | Paired T test | P value | |
|---|---|---|---|---|---|
| Test | GI1 | 1.95 | 0.088 | 1.285 | 0.214 NS |
| GI2 | 2.15 | 0.167 | |||
| GI1 | 1.95 | 0.088 | 9 | 0.000 HS | |
| GI3 | 1.05 | 0.05 | |||
| GI2 | 2.15 | 0.167 | 6.85 | 0.000 HS | |
| GI3 | 1.05 | 0.05 | |||
| Control | GI1 | 2 | 0 | 1.285 | 0.214 NS |
| GI2 | 2.2 | 0.156 | |||
| GI1 | 2 | 0 | 7.55 | 0.000 HS | |
| GI3 | 1.25 | 0.099 | |||
| GI2 | 2.2 | 0.156 | 6.19 | 0.000 HS | |
| GI3 | 1.25 | 0.099 | |||
Table 6: Comparison between GI in the 2nd and 3rd visits and baseline level in each study group.
Pocket depth
The intra group comparison between pocket depth in the baseline and 3rd visits in each study group is shown in Table 7. Means of pocket depth presented high statistical decrease in the 3rd visit compared with baseline pocket depth in test and control sites (3.500 versus 5.550, p=0.000; and 3.775, versus 5.300, p=0.000, respectively).
| Groups | T | P value | ||||
|---|---|---|---|---|---|---|
| Test | Control | |||||
| Mean | ± SE | Mean | ± SE | |||
| PPD1 | 5.55 | 0.153 | 5.3 | 0.128 | 1.252 | 0.218 NS |
| PPD3 | 3.5 | 0.136 | 3.775 | 0.152 | 1.351 | 0.185 NS |
| Paired T test | 12.076 | 12.99 | ||||
| P value | 0.000 HS | 0.000 HS | ||||
Table 7: Inter and intra group comparison between pocket depth in the baseline and 3rd visits.
Intergroup comparison, means of PPD in the 3rd visit, presented no-statistically significant differences in test and control sites (3.500 versus 3.775, P=0.185 respectively).
Relative attachment level
The intra group comparison between RAL in the baseline and 3rd visits in each study group is shown in Table 8. Means of RAL presented statistical high significant decrease in the 3rd visit compared with that in baseline for test and control sites (7.325 versus 8.300, P=0.000; and 7.400 versus 8.100, P=0.000 respectively).
| Groups | T | P value | ||||
|---|---|---|---|---|---|---|
| Test | Control | |||||
| Mean | ± SE | Mean | ± SE | |||
| RAL1 | 8.3 | 0.179 | 8.1 | 0.161 | 0.831 | 0.411 |
| RAL3 | 7.325 | 0.132 | 7.4 | 0.172 | 0.345 | 0.732 |
| Paired T test | 9.831 | 8.304 | ||||
| P value | 0.000 HS | 0.000 HS | ||||
Table 8: Intra and inter group comparison between RAL in the baseline and 3rd visits.
In the 3rd visit and for, intergroup comparison means of RAL presented no statistically significant change in test and control sites (7.325 versus 7.400, P=0.732 respectively).
Bleeding on probing
Table 9 shows the comparison between BOP in the 3rd visit with baseline level in each study group. In test group BOP presents with highly significant decrease in 3rd visit compared to the baseline data (P=0.000). But in the control sites group, no statistically significant association (P=0.063) in the 3rd visit compared with baseline data. But intergroup comparison in the 3rd visits revealed statistical high significant association between test and control sites (P=0.000 versus P=0.063 respectively).
| Index1 | Groups | Chi square | P value | Total | |||||
|---|---|---|---|---|---|---|---|---|---|
| Test | Control | ||||||||
| N. | % | N. | % | N. | % | ||||
| BOP1 | 1 | 18 | 90 | 18 | 90 | 0 | 1 NS | 36 | 90 |
| 0 | 2 | 10 | 2 | 10 | 4 | 10 | |||
| Total | 20 | 100 | 20 | 100 | 40 | 100 | |||
| BOP3 | 1 | 1 | 5 | 13 | 65 | 15.824 | 0 | 14 | 35 |
| 0 | 19 | 95 | 7 | 35 | HS | 26 | 65 | ||
| Total | 20 | 100 | 20 | 100 | 40 | 100 | |||
| MC Nemar’s Test | P value | 0.000HS | 0.063 NS | ||||||
Table 9: Comparison between bleeding on probing in the 3rd visit and baseline level in each study group.
Discussion
This study showed that curcumin gel as adjunctive treatment can make a significant reduction in means of all clinical periodontal parameters from baseline to 30 days in both test and control sites.
On intra group, the PLI presented no statistical significant change in the 2nd visit (after one week) compared with baseline data for both test and control sites which was due to the use of periodontal pack that increased the plaque accumulation, but PLI presented statistical significant decrease in the test and control sites in 3rd visit (after one moth) compared with baseline visit this due to SRP can reduce the pathogenicity of the plaque by the disruption of the biofilms with removing of the retentive factor, and its maintained with personal consistent oral hygiene commitment.
On intra group, GI presented no statistical significant change in the 2nd visit (after one week) compared with baseline data for both test and control sites which was due to the use of periodontal pack that increased the PLI and subsequently increase GI, but in the 3rd visit (after one month), means of GI presented statistical significant decrease in test and control sites compared to 2nd and baseline visit, this was because of removal of plaque and irritant factors that lead to decrease the gingival inflammation.
On inter group, no statistically significant difference was noticed in GI in the test and control sites at baseline visit this was due to few number of times of gel application, these results were agreeing with the researches of Behal et al. in the 2nd visit of their follow up after one moth that achieved clinical trial for comparing the influence of 2%, whole curcumin oral gel along with the scaling and root planning with the influence accomplished by using scaling and root planning alone [11] and Bhatia et al. in 2nd visit of their follow up after one month, the results of this study after one month in test and control sites PLI (0.48 versus 0.55, p=0.183 respectively) which statistically non-significant difference between the test and control sites inter group. At the end of the observation period, there were significant improvements in the clinical parameters of periodontitis, including reduction in pocket depth and bleeding, and gain in clinical attachment levels in both groups but with more pronounced improvement in the test group [12]. But our study disagrees with results of Anuradha BR et al. that treated 30 patients with pocket depth of 5 to7 mm affecting 2 nonadjacent sites. The clinical parameters were recorded on day 0, 30 and 45 days. after one month in test and control sites statistically significant differences were presented for PLI and GI [9].
The pocket depth presented statistical significant decrease in the 3rd visit compared with baseline pocket depth in test and control sites and this was because of the power of SRP that lead to removal of calculus with inflamed tissue and smoothing the surfaces of the hard tissue with exposing of heathy tissue which enhance the reattachment of periodontal fibers and resolution of the inflammation which lead to the shrinkage of the soft tissue.
In the 3rd visit, means of pocket depth presented no statistical significant differences in test and control sites (intergroup) and to present statistical significant different this may need more time for follow up and increase number of time of gel application.
The RAL presented statistically significant decrease in the 3rd visit compared with baseline data within test and control sites this is partialy due to gaining in clinical attachment and to the formation of long junctional epithelium.
In the 3rd visit, means of RAL presented no statistically significant change between test and control sites this because of short period of follow up and few numbers of times of gel application. Reduction of pocket depth and CAL gain can be obtained by appropriate SRP [13-15] and that was homogenous with our results. Our result was agreeing with research of Anuradha et al. [9] and research of Behal et al. [11].
However, our result was disagreeing with researches of Gottumukkala et al. which treating twenty three patients that have non‑adjacent pockets with depth (PPDs) ≥ 5mm with CU, CHX and positive control irrigation groups, the results of this study after one month in test and control sites PPD (2.70 versus 4.30, p<0.01 respectively) statistically significant difference was presented between the test and control sites [13] and Bhatia et al. At the end of the observation period, there were significant improvements in the clinical parameters of periodontitis, including decrease in pocket depth and bleeding, and clinical attachment gain levels in the both groups, but with more pronounced improvement in the test group [12].
The BOP, in test group was significantly decreased in the 3rd visit in comparison with baseline data (P=0.000) the change was 85% and this because of anti-inflammatory effect of curcumin gel. But no statistically significant change in the bleeding on probing within control sites group (P=0.063) in the 3rd visit compared with baseline data, the change was 25%. The results concluded that (BOP) can be irrelevant to SRP. Furcation involvement and the type of tooth involved alter the BOP response to treatment. Single rooted teeth showed to be much more responsive to treatment regarding BOP when compared to multirooted teeth [16].
In the 3rd visits, were statistically significant difference was presented between test and control sites groups (P=0.000 versus P=0.063 respectively) this was because of use of antiinflammatory agent (curcumin gel) in test sites group. Our result was agreeing with the result of Gottumukkala et al. [13] and disagree with the result of Bhatia et al. in 2nd visit of their follow up after one month [12].
There are two recent studies the 1st one was conducted by Harleen Kaur et al. that Evaluated the effect of the curcumin oral gel as adjunctive for the scaling and the root planing in the treatment of the periodontitis, based on clinical, and biochemical, parameters. Carried out on 30 patients with the pocket depth, ≥ 5mm affecting 4 sites at least. The study clarified minor adjunct advantage of the curcumin oral gel for decreasing of the “gingival inflammation” for a little duration of time. However, the improving in the other clinical parameters were also larger for subjects managed with curcumin oral gel and the result was not different statistically from these managed with SRP only [17]. This study was in parallel line with our study in clinical parameters and the 2nd study was conducted by Kepu V Raghava et al. that evaluated the effectiveness of the curcumin oral gel as a drug deliver locally post scaling and root planning, and its influence on the clinical parameters. Assessment of (PLI), (GI), PPD, and CALs were done in the baseline and the 4th week. Results were revealed there were a statistically significant decrease in PLI and probing depth in the test group in comparison with the control group. CAL improved but the result was not statistically significant [18]. This study was contradicted with our study in PLI and PPD but like our study in CAL.
Conclusion
Curcumin shows a potent effect in improving the outcomes of clinical parameters when compared with SRP. The medication significantly improved BOP.
Curcumin can be a promising adjunctive therapeutic agent; it showed a good capability in influencing the gingival health by assessing the clinical parameters. This therapeutic agent presents a significant effect on PPD, CAL, PLI and GI and although its influence on these parameters were not significant when compared with SRP but it was prominent on PPD and CAL than conventional therapy.
References
- Newman MG, Takei H, Klokkevold PR, et al. Carranza's clinical periodontology. 13th Edn 2018; 1710-1712.
- Vitt A, Gustafsson A, Ramberg P, et al. 2019. Polyhexamethylene guanidine phosphate irrigation as an adjunctive to scaling and root planing in the treatment of chronic periodontitis. Acta Odontologica Scandinavica 2019; 77:290-295
- Liaw A, Miller C, Nimmo A. Comparing the periodontal tissue response to non‐surgical scaling and root planing alone, adjunctive azithromycin, or adjunctive amoxicillin plus metronidazole in generalized chronic moderate‐to‐severe periodontitis: a preliminary randomized controlled trial. 2019; 64:145-152
- Palombo EA. Traditional medicinal plant extracts and natural products with activity against oral bacteria: potential application in the prevention and treatment of oral diseases. Evidence-Based Complementary Alternative Med 2011.
- Zandbergen D, Slot DE, Cobb CM, et al. The clinical effect of scaling and root planing and the concomitant administration of systemic amoxicillin and metronidazole: A systematic review. J Periodontol 2013; 84:332-351.
- Buommino E, Scognamiglio M, Donnarumma G, et al. Recent advances in natural product-based anti-biofilm approaches to control infections. Mini Reviews Med Chem 2014; 14:1169-1182.
- Pai PG, Dayakar MM, Nath AR, et al. Phytotherapeutics in the management of periodontal disease-A review. J Res Dent Sci 2019; 10:82.
- Lawande SA. Therapeutic applications of turmeric (Curcuma longa) in dentistry: A promising future. J Pharm Biomed Sci 2013; 27: 586-591.
- AnuradhaB R, Yendluri Durga Bai, et al. Evaluation of anti-inflammatory effects of curcumin gel as an adjunct to scaling and root planning. J Int Oral Health 2015; 7:90-93.
- Deevaraj SD, Neelakantan P. Curcumin-pharmacological actions and its role in dentistry. Asian J Pharm Res Health Care 2014; 6:19-22.
- Behal R, Mali AM, Gilda SS, et al. Evaluation of local drug-delivery system containing 2% whole turmeric gel used as an adjunct to scaling and root planing in chronic periodontitis: A clinical and microbiological study. J Indian Soc Periodontol 2011; 15:35-38.
- Bhatia M, Urolagin SS, Pentyala KB, et al. Novel therapeutic approach for the treatment of periodontitis by curcumin. J Clin Diagnostic Res 2014; 8:65-69.
- Gottumukkala SN, Koneru S, Mannem S, et al. Effectiveness of sub gingival irrigation of an indigenous 1% curcumin solution on clinical and microbiological parameters in chronic periodontitis patients: A pilot randomized clinical trial. Contemporary Clin Dent 2013; 4:186-191.
- Hung HC, Douglass CW. Meta-analysis of the effect of scaling and root planing, surgical treatment and antibiotic therapies on periodontal probing depth and attachment loss. J Clin Periodontol 2002; 29:975–986.
- Herrera D. Scaling and root planning is recommended in the nonsurgical treatment of chronic periodontitis. J Evid Base Dent Pract 2016; 16:56-58.
- Van der Weijden GA, Dekkers GJ, Slot DE. Success of non-surgical periodontal therapy in adult periodontitis patients: A retrospective analysis. Int J Dent Hyg 2019; 17:309-317.
- Kaur H, Grover V, Malhotra R, et al. Evaluation of curcumin gel as adjunct to scaling and root planing in management of periodontitis- Randomized clinical and biochemical investigation. Randomized Controlled Trial 19:171-178.
- Raghava KV, Sistla KP, Narayan SJ, et al. Efficacy of curcumin as an adjunct to scaling and root planing in chronic periodontitis patients: A randomized controlled clinical trial. 2019; 20:842-846.
Author Info
Hayder Thabit Farhood* and Basma Ghafori Ali
Department of Periodontics, College of Dentistry, University of Baghdad, IraqCitation: Hayder Thabit Farhood, Basma Ghafori Ali, Clinical and Anti-Inflammatory Effect of Curcumin Oral Gel as Adjuncts in Treatment of Periodontal Pocket, J Res Med Dent Sci, 2020, 8 (6): 83-90.
Received: 19-Aug-2020 Accepted: 16-Sep-2020
