Research - (2021) Volume 9, Issue 6
Clinical Spectrum of Acute Kidney Injury in ICU Patients
Vedula Rama Aditya Chainulu and V Padma*
*Correspondence: V Padma, Department of General Medicine, Sree Balaji Medical College & Hospital Affiliated to Bharath Institute of Higher Education and Research, Chennai, Tamil Nadu, India, Email:
Abstract
To study and analyse the demography, etiology and several clinical and biochemical risk factors contributing to development of AKI in ICU patients. Assessment of prior comorbid conditions, septicemia, oliguria and Renal Function Tests with outcome, severity of AKI. We observed that sepsis is the leading cause of AKI in ICU admissions. We observed that there is highly significant correlation of presence of sepsis and oliguria with the outcome of AKI (p<0.01) We observed a significant correlation between the values of Urea, Creatinine and eGFR with the outcome of AKI. We also observed that there is no significant correlation betw
Keywords
Oligouria, Septicemia, Chronic kidney disease, Acute kidney injury
Introduction
Acute Kidney Injury (AKI) is a complex condition that manifests in a number of clinical scenarios with it manifestations ranging from modest plasma creatinine escalation to anuric renal failure.It is often underrecognized and has severe consequences. Recent epidemiological studies show the wide variation in etiology and risk factors [1-5], identify the increased mortality associated with this disease (especially when dialysis is required) [6-9], and indicate a relationship to the subsequent development of chronic kidney disease (CKD) and development of dialysis dependence [10–13].
Emerging evidence suggests that even minor serum creatinine changes are associated with higher in-patient mortality [14]. Over the past decades, AKI has been the focus of extensive clinical and basic research. A major limitation has been the absence of a niversally recognized definition of AKI. Despite significant progress in understanding the biology and mechanism of AKI in animal models, there has been limited translation of this knowledge into improved patient management and outcomes. Acute Kidney Injury Network (AKIN) is an independent collaborative network of experts selected by the participating societies to represent their field of expertise as well as their sponsoring organization. AKIN seeks to promote global, interdisciplinary and intersocietal partnerships to ensure success in the area of AKI and achieve the best results for patients with or at risk of AKI [15-17].
Materials and Methods
Place: Intensive Care Unit, Sree Balaji Medical College and Hospital, Chennai.
Design: Observational Study
Sample Size: 100 (one hundred)
Study Population: The study will be conducted in inpatients of ICU in Sree Balaji Medical College and Hospital.
Inclusion Criteria: All patients admitted to ICU with AKI and those who developed AKI after admission to ICU.
Exclusion Criteria: Patients with pre-existing renal disease and with renal transplant. Patients with abnormal kidney size and abnormal cortico-medullary differentiation
A detailed history, physical examination and lab investigations including CBC, RFT, Renal USG, urine analysis was done. Blood culture and sensitivity, Leptospirosis serology, smear for MP / MF, imaging studies and other investigations were done as and when warranted clinically.
Results
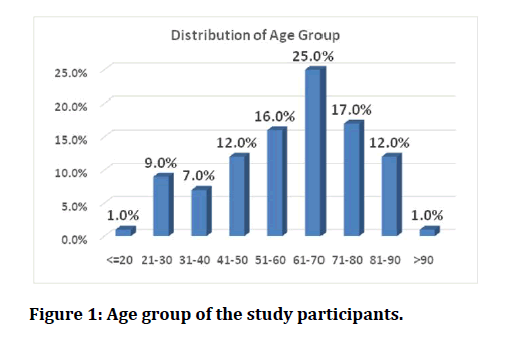
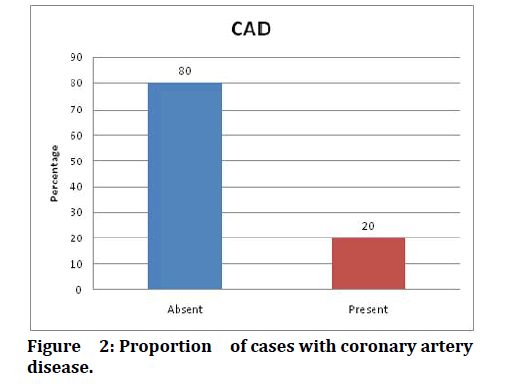
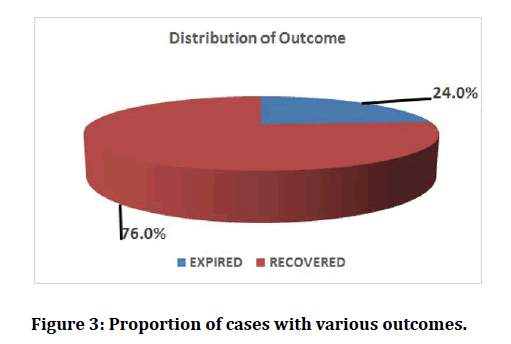
In this study among 100 participants with Acute Kidney Injury 1 % of the participants were below 20 years of age, 9% of the participants were between 21 -30 years of age. In the age range of 31-40 years 7% of the participants were recorded on this study, 12% of the AKI patients were between 41-50 years of age, 16% of the participants were between 51-60 years of age, 25% of the participants were of the age group of 61-70 years and above 70 years there were 30% of patients in this study (Figure 1). Among the 100 Acute Kidney Injury patients 42 of them (42%) were found to have Diabetes Mellitus (Table 1). In the current study 38% of the participants were found to have Hypertension (Table 2). Coronary Artery Disease was found in 20% of the study participants with Acute Kidney Injury (Figure 2). In this present study, 40% of the study participants had sepsis whereas 60% of the AKI patients do not have sepsis (Table 3). Oliguria was recorded among maximum of 62% of the study patients and for 38% of the patient’s oliguria was absent (Table 4). In this study, on analysing the outcome, it was found that 24% of the population with AKI have expired, and the rest of the patients have survived, either having fully recovered or with variable levels of residual renal insults sub clinically (Figure 3).
Figure 1: Age group of the study participants.
Figure 2: Proportion of cases with coronary artery disease.
Figure 3: Proportion of cases with various outcomes.
Table 1: Proportion of cases with diabetes mellitus.
| Diabetes mellitus | Percentage |
|---|---|
| Absent | 58 |
| Present | 42 |
| Total | 100 |
Table 2: Proportion of cases with hypertension.
| Hypertension | Percentage |
|---|---|
| Absent | 62 |
| Present | 38 |
| Total | 100 |
Table 3: Proportion of cases with Sepsis.
| Sepsis | Percentage |
|---|---|
| Absent | 60 |
| Present | 40 |
| Total | 100 |
Table 4: Proportion of cases with oliguria.
| Oliguria | Percentage |
|---|---|
| Absent | 38 |
| Present | 62 |
| Total | 100 |
Upon analysing the values of the renal function tests, the mean values of:
Serum Urea was 104.99 mg/dl,
Serum Creatinine was 2.891 mg/dl and eGFR was 27.88 ml/min/1.73m2 (Table 5).
Table 5: Mean values of Biochemical indices in the study population.
| Urea (mg/dl) | Creat (mg/dl) | eGFR (ml/min/1.73m2) | |
|---|---|---|---|
| Mean | 104.99 | 2.891 | 27.88 |
| Std Error | 4.760220159 | 0.15569 | 1.42065 |
In our study we analysed the peak Serum Urea and Creatinine values of each of the patients during their course of stay in the ICU.
It was found that the mean urea value in the study population was 104.99 mg/dl and mean creatinine value was 2.891 mg/dl. Among the expired patients, the mean urea was 150.63 mg/dl and among the survivors, the mean urea was 90.58 mg/dl. Further, in the present study, upon analysis of estimated Glomerular Filtration Rate (eGFR) which is a useful point of care tool to determine kidney function, it was found that the mean eGFR was 27.88 mL/min/1.73 m2.
Among the expired patients, the mean eGFR was 14.33 mL/min/ 1.73 m2 whereas in patients who survived, the mean eGFR was 32.16 mL/min/1.73 m2 (Table 6).
Table 6: Outcome based analysis of biochemical indices.
| Outcome | N | Mean | Std. Deviation | Std. Error Mean | |
|---|---|---|---|---|---|
| Urea | Expired | 24 | 150.63 | 55.677 | 11.365 |
| Recovered | 76 | 90.58 | 34.111 | 3.913 | |
| Creat | Expired | 24 | 4.73 | 1.88 | 0.384 |
| Recovered | 76 | 2.31 | 0.828 | 0.095 | |
| eGFR | Expired | 24 | 14.33 | 7.9 | 1.613 |
| Recovered | 76 | 32.16 | 13.038 | 1.496 |
Applying the student’s t -test, showed that the difference between the outcome based mean values of Urea, Creatinine and eGFR between the expired and survived population were statistically significant (Table 7). This study has shown that among 40 patients with sepsis, 18 patients expired (p<0.001) and sepsis was hence found to be an indicator of higher mortality rates than those without sepsis. Mortality due to septicemia was observed to be 75% (Table 8).
Table 7: Student’s t-test applied to the biochemical indices.
| Levene's Test for Equality of Variances | t-test for Equality of Means | ||||||
|---|---|---|---|---|---|---|---|
| F | Sig. | t | df | Sig. (2-tailed) | Mean Difference | Std. Error Difference | |
| Urea | 17.374 | 0 | 6.375 | 98 | 0 | 60.046 | 9.418 |
| (mg/dl) | 4.996 | 28.652 | 0 | 60.046 | 12.02 | ||
| Creat (mg/dl) | 44.327 | 0 | 8.894 | 98 | 0 | 2.424 | 0.273 |
| 6.13 | 25.874 | 0 | 2.424 | 0.395 | |||
| eGFR (mL/min/ 1.73 m2) | 7.43 | 0.008 | -6.327 | 98 | 0 | -17.825 | 2.817 |
| -8.104 | 64.87 | 0 | -17.825 | 2.199 | |||
Table 8: Sepsis outcome.
|
Outcome |
Total |
||||
|---|---|---|---|---|---|
|
Expired |
Recovered |
||||
| Sepsis | Present | Count | 18 | 22 | 40 |
| % Within Sepsis | 45.00% | 55.00% | 100.00% | ||
| % Within Outcome | 75.00% | 28.90% | 40.00% | ||
| % Of Total | 18.00% | 22.00% | 40.00% | ||
| Absent | Count | 6 | 54 | 60 | |
| % Within Sepsis | 10.00% | 90.00% | 100.00% | ||
| % Within Outcome | 25.00% | 71.10% | 60.00% | ||
| % Of Total | 6.00% | 54.00% | 60.00% | ||
| Total | Count | 24 | 76 | 100 | |
| % Within Sepsis | 24.00% | 76.00% | 100.00% | ||
| % Within Outcome | 100.00% | 100.00% | 100.00% | ||
| % of Total | 24.00% | 76.00% | 100.00% | ||
Among the 62 patients in our study who were oliguric, 24 patients (38.7%) expired, which is statistically significant (p<0.05). Among the 24 patients in our study that expired, all 24 patients were found to have oliguria (100%) (Table 9).
Table 9: Oliguria outcome.
| Outcome | Total | ||||
|---|---|---|---|---|---|
| Expired | Recovered | ||||
| Oliguria | Present | Count | 24 | 38 | 62 |
| % Within Oliguria | 38.70% | 61.30% | 100.00% | ||
| % Within Outcome | 100.00% | 50.00% | 62.00% | ||
| % Of Total | 24.00% | 38.00% | 62.00% | ||
| Absent | Count | 0 | 38 | 38 | |
| % Within Oliguria | 0.00% | 100.00% | 100.00% | ||
| % Within Outcome | 0.00% | 50.00% | 38.00% | ||
| % Of Total | 0.00% | 38.00% | 38.00% | ||
| Total | Count | 24 | 76 | 100 | |
| % Within Oliguria | 24.00% | 76.00% | 100.00% | ||
| % Within Outcome | 100.00% | 100.00% | 100.00% | ||
| % Of Total | 24.00% | 76.00% | 100.00% | ||
Discussion
AKI is a kidney disease that is potentially fatal but reversible. Due to its climatic and geographic heterogeneity and variable quality of medical care, etiology, and course, the analysis varies in different parts of the world and also within India. 100 patients have been analyzed in our research. There were 52 males and 48 females. The mean age was 59.5 years. In the sixth to eighth decade, the highest number of cases were reported. Mehta et al., in her study analysed a sample population which had 59% males and 41% were females with mean of 59.5years. 46 Sepsis was found to be the leading cause of Acute Kidney Injury in the current study (40%) as has been time and again proven by multiple studies [18].
This study has shown that among 40 patients with sepsis, 18 patients expired (p<0.001) and sepsis was hence found to be an indicator of higher mortality rates than those without sepsis. Mortality due to septicemia was observed to be 75%. This was identical to the findings of Qutub HO 3, Saeed IA48 in their three yearlong prospective study (1996 to 1999) in which sepsis emerged as the leading cause of Acute Kidney Injury and also a major contributor for mortality [19,20]. They also stated that prevention of sepsis would improve the prognosis of patients who got admitted into ICU due to any other cause. In another study conducted by Agarwal et al 49 at CMC Vellore in 2004, similar observations were made in pediatric population vis-a-vis septicemia. It was found that mortality due to septicemia was 83% among ICU patients who had Acute Kidney Injury and was a major contributor to morbidity and mortality. In our sample population, oliguric AKI was predominant (62 percent) compared to non-oliguric AKI, which was in line with Muthusethupathi et al's research in 1999.2 Oliguria is a very important parameter in renal injury and was the single most important predictor of mortality in many studies. Among the 62 patients in our study who were oliguric, 24 patients (38.7%) expired, which is statistically significant (p<0.05). Among the 24 patients in our study that expired, all 24 patients were found to have oliguria. Macedo et al 50 in their prospective study in 2011 found out that oliguria for more than 12 hours or oliguria for 3 or more episodes were associated with higher mortality [21-23].
In our study we analysed the peak Serum Urea and Creatinine values of each of the patients during their course of stay in the ICU. It was found that the mean urea value in the study population was 104.99 mg/dl and mean creatinine value was 2.891 mg/dl. Among the expired patients, the mean urea was 150.63 mg/dl and among the survivors, the mean urea was 90.58 mg/dl. Applying the student’s t-test, showed that the difference between the two values is significant. Similarly, the mean creatinine among the expired patients was 4.73 mg/dl, whereas that among the survivors was 2.31 mg/dl, the difference of which was again found to be statistically significant using student’s t -test. There has been limited research pertaining to peak levels of urea and creatinine and their effect upon the outcome [24]. However, in 2013 it is found that patients with tage 1 AKI (increase in serum creatinine either 0.3 mg / dl or 50% regardless of the final serum creatinine) and <=1.5 mg/dl peak serum creatinine had a very good survival, comparable to that of non-AKI patients.
In the present study, upon analysis of estimated Glomerular Filtration Rate (eGFR) which is a useful point of care tool to determine kidney function, it was found that the mean Egfr was 27.88 mL/min/1.73 m2. Among the expired patients, the mean eGFR was 24 mL/min/ 1.73 m2 whereas in patients who survived, the mean eGFR was 76 mL/min/1.73 m2. Upon applying the student’s t -test, it was found that the difference between these two mean values was significant. It is in line with the research findings of Suk et al52 whose study concluded that the eGFR cut-off level for in-hospital mortality was 56 mL / min/1,73 m 2. EGFR < 56 mL / min/1.73 m2 had an odds ratio of 2.5 (95 percent confidence interval, 1.6 –4.0) for mortality by multivariate logistic regression [25-27]. Our study also reiterated the point that though the presence of comorbid conditions like Diabetes, Hypertension and Coronary Artery Disease poses increased risk for development of AKI, they are not associated with increased mortality risk in patients admitted for/with AKI as has been established previously by many extensive studies like that of Mehta et al 53 in India and Schwilk et al54 in Europe. However, although outside the scope of this study, it is worthwhile to mention that in a retrospective study involving more than 500 patients, Mariana et al 55 in 2012 showed that though the chronic comorbidities like Diabetes, Hypertension and Coronary Artery Disease do not have any immediate mortality risk but positively affect the long-term survival rates in patients who have recovered from AKI [28,29].
Conclusion
At the end of the study 24 patients expired and 76 patients survived. We observed that the risk of developing AKI was more in advanced age group (>60 years) with no gender predilection. We observed that sepsis is the leading cause of AKI in ICU admissions. We observed that there is highly significant correlation of presence of sepsis and oliguria with the outcome of AKI (p<0.01) We observed a significant correlation between the values of Urea, Creatinine and eGFR with the outcome of AKI. We also observed that there is no significant correlation between the presence of comorbid conditions like Diabetes, Hypertension and Coronary Artery Disease with the outcome of AKI (p>0.05).
Funding
No funding sources.
Ethical Approval
The study was approved by the Institutional Ethics Committee.
Conflict of Interest
The authors declare no conflict of interest.
Acknowledgements
The encouragement and support from Bharath University, Chennai is gratefully acknowledged. For provided the laboratory facilities to carry out the research work.
References
- Mehta RL, Pascual MT, Soroko S, et al. Program to improve care in acute renal disease (PICARD). Spectrum of acute renal failure in the intensive care unit: The PICARD experience. Kidney Int 2004; 66:1613 -21.
- Palevsky PM. Epidemiology of acute renal failure: The tip of the iceberg. Clin J Am Society Nephrol 2006; 1:6-7.
- Ympa YP, Sakr Y, Reinhart K, et al. Has mortality from acute renal failure decreased? A systematic review of the literature. Am J Med 2005; 118:827-32.
- Metnitz PG, Krenn CG, Steltzer H, et al. Effect of acute renal failure requiring renal replacement therapy on outcome in critically ill patients. Critical Care Med 2002; 30:2051-8.
- Liangos O, Wald R, O’Bell JW, et al. Epidemiology and outcomes of acute renal failure in hospitalized patients: A national survey. Clin J Am Society Nephrol 2006; 1:43-51.
- Clermont G, Acker CG, Angus DC, et al. Renal failure in the ICU: Comparison of the impact of acute renal failure and end-stage renal disease on ICU outcomes. Kidney Int 2002; 62:986-96.
- Thakar CV, Worley S, Arrigain S, et al. Influence of renal dysfunction on mortality after cardiac surgery: Modifying effect of preoperative renal function. Kidney Int 2005; 67:1112-1119.
- Druml W. Long term prognosis of patients with acute renal failure: is intensive care worth it?. Intensive Care Med 2005; 31:1145-7.
- Liano F, Junco E, Madero R, et al. The spectrum of acute renal failure in the intensive care unit compared with that seen in other settings. Kidney Int 1998; 16-24.
- Mehta RL, Pascual MT, Soroko S, et al. Diuretics, mortality, and nonrecovery of renal function in acute renal failure. JAMA 2002; 288:2547-53.
- Chertow GM, Burdick E, Honour M, et al. Acute kidney injury, mortality, length of stay, and costs in hospitalized patients. J Am Society Nephrol 2005; 16:3365-70.
- Lassnigg A, Schmidlin D, Mouhieddine M, et al. Minimal changes of serum creatinine predict prognosis in patients after cardiothoracic surgery: A prospective cohort study. J Am Society Nephrol 2004; 15:1597-605.
- Levy MM, Macias WL, Vincent JL, et al. Early changes in organ function predict eventual survival in severe sepsis. Critical Care Med 2005; 33:2194-201.
- McCullough PA, Soman SS. Contrast-induced nephropathy. Critical Care Clin 2005; 21:261-80.
- Praught ML, Shlipak MG. Are small changes in serum creatinine an important risk factor?. Current Opinion Nephrol Hypertension 2005; 14:265-70.
- Hoste EA, Clermont G, Kersten A, et al. RIFLE criteria for acute kidney injury are associated with hospital mortality in critically ill patients: A cohort analysis. Critical Care 2006; 10:R73.
- Pisoni R, Wille KM, Tolwani AJ. The epidemiology of severe acute kidney injury: From BEST to PICARD, in acute kidney injury: New concepts. Nephron Clin Pract 2008; 109:188–191.
- https://kdigo.org/wp-content/uploads/2016/10/KDIGO-2012-AKI-Guideline-English.pdf
- Kellum JA, Bellomo R, Ronco C. Definition and classification of acute kidney injury. Nephron Clin Pract 2008; 109:c182–7.
- Bywaters EG, Beall D. "Crush injuries with impairment of renal function. Br Med J 1941; 1:427–33.
- Al-Homrany M. Epidemiology of acute renal failure in hospitalized patients: Experience from southern Saudi Arabia. East Mediterr Health 2003;1061–1067.
- Vukusich A, Alvear F, Villanueva P, et al. Epidemiology of severe acute renal failure in Metropolitan Santiago. Rev Med Chil1 2004; 32:1355–1361.
- Ostermann M, Chang RW. Acute kidney injury in the intensive care unit according to RIFLE. Critical Care Med 2007; 35:1837-43.
- Andreoli P. Are children with a history of acute kidney injury at risk of later kidney disease? Nature Clin Practice Nephrol 2006; 439-42.
- Hoste EA, Bagshaw SM, Bellomo R, et al. Epidemiology of acute kidney injury in critically ill patients: the multinational AKI-EPI study. Intensive Care Med 2015; 41:1411-23.
- Muthusethupathi MA, Shivakumar S, Suguna R, et al. Leptospirosis in Madras: A clinical and serological study. J Assoc Physicians India 1995; 43:456– 458.
- Qutub HO, Saeed IA. Acute renal failure in intensive careunit. Saudi Med J 2001; 22:999-1003.
- Agarwal I, Kirubakaran C, Markandeyulu V. Clinical profile and outcome of acute renal failure in South Indian children. J Indian Med Assoc 2004; 102:353-354.
- Pereira MB, Zanetta DM, Abdulkader RC. The real importance of pre-existing comorbidities on long-term mortality after acute kidney injury. PLoS One 2012; 7:e47746.
Author Info
Vedula Rama Aditya Chainulu and V Padma*
Department of General Medicine, Sree Balaji Medical College & Hospital Affiliated to Bharath Institute of Higher Education and Research, Chennai, Tamil Nadu, IndiaCitation: Vedula Rama Aditya Chainulu, V Padma, Clinical Spectrum of Acute Kidney Injury in ICU Patients, J Res Med Dent Sci, 2021, 9(6): 168-176
Received: 01-Apr-2021 Accepted: 17-Jun-2021 Published: 24-Jun-2021