Research Article - (2022) Volume 10, Issue 5
Comparison of Outcome of Endoscopic Septoplasty versus Endoscopic Septoplasty with Inferior Turbinoplasty Using Microdebrider
Thrupthi S*, Rajasekar MK and Jayapreetha
*Correspondence: Thrupthi S, Department of ENT, Sree Balaji Medical College and Hospital, Chrompet, Chennai, Tamil Nadu, India, Email:
Abstract
Nasal obstruction is one of the common symptoms that patients present with to the ENT surgeon. The most common causes of nasal obstruction are deviated nasal septum and inferior turbinate hypertrophy. The development of new diagnostic and therapeutic materials has helped to a variable extent to understand the various anatomical abnormalities or any pathologies. Diagnostic nasal endoscopy is done preoperatively. Patient can undergo turbinate reduction procedures as a treatment option for inferior turbinate hypertrophy. In this study we will be comparing the outcome of endoscopic septoplasty versus endoscopic septoplaty done along with inferior turbinoplasty using a microdebrider.Keywords
Nasal obstruction, Inferior turbinoplasty, MicrodebriderIntroduction
Breathing is an individual's most basic need for survival. It has an impact not only on an individual's survival but also on his or her productivity. Breathing difficulties can be caused by abnormalities ranging from the tip of the nose to the terminal bronchioles.
Nasal obstruction is one of the common symptoms that patients present with to the ENT surgeon. The development of new diagnostic and therapeutic materials has helped to a variable extent to understand the various anatomical abnormalities or any pathology. Symptoms maybe disproportionate to the actual findings. I will be discussing the management of nasal obstruction in my study.
The most common causes of nasal obstruction are deviated nasal septum and inferior turbinate hypertrophy. Many patients complain of persisting nasal obstruction after undergoing septoplasty as a treatment for deviated nasal septum. It is usually due to the presence of a hypertrophied inferior turbinate. Diagnostic nasal endoscopy is done preoperatively to show the difficulty in the first pass which maybe caused due to the deviated nasal septum as well as inferior turbinate hypertrophy. Temporary management of turbinate reduction can be done using modern pharmacological agents. It is temporary as the nasal obstruction is bound to occur after the stoppage of medical treatment. Alternatively patient can undergo turbinate reduction procedures as a treatment option for inferior turbinate hypertrophy [1]. The chances of crusting, atrophic rhinitis is high with total turbinectomy but nevertheless it relieves nasal obstruction immediately. The other procedures which can be done for turbinate reduction are:
These are the resection procedures
1. Partial inferior turbinectomy
2. Subtotal inferior turbinectomy
3. Turbinate submucous resection
4. Inferior turbinoplasty with power
Non-resection procedures include
1. Turbinate out fractioning
2. Chemical turbinate cauterization
3. Cryotherapy
4. Surface and submucosal electrocautery
5. Radiofrequency ablation
6. Coblation assisted turbinoplasty
7. LASER assisted turbinoplasty
My study is about the added benefits of microdebrider assisted turbinoplasty when it is done alongwith septal correction procedures [2].
The study's goals and objectives
The purpose of this study was to compare the outcomes of endoscopic septoplasty and endoscopic septoplasty combined with microdebrider assisted inferior turbinoplasty by
• Comparing symptomatic improvement in the various groups.
• Comparing the postoperative complication rates in the control and test groups.
Materials and Methods
Aim: To compare the outcomes of endoscopic septoplasty and endoscopic septoplasty combined with inferior turbinoplasty assisted by a microdebrider.
December 2017 to November 2019 Study Period.
Criteria for inclusion
• Age 20 to 45 years old, both sexes.
• Patients with a deviated nasal septum, inferior turbinate hypertrophy, and nasal obstruction symptoms.
• The patient gives his or her consent to participate in the study.
• The patient is willing to undergo surgery [3].
Exclusion criteria
• Patients over the age of 45 and those under the age of 20 are excluded.
• Patients who have a history of allergic reactions or other symptomatology.
• Patients who are unable to undergo surgery.
Investigations
A complete history with systemic examination and complete examination of ear, nose and throat including anterior and posterior rhinoscopy [4].
• Diagnostic nasal endoscopy.
• CT paranasal sinuses.
• Preop and post op questionnaire.
• Routine pre-operative investigations (complete blood counts, renal function tests, etc.)
Case presentation
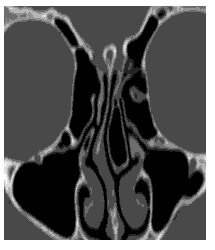
The prospective study was conducted at Sree Balaji Medical College and Hospital, Chennai. The patients who came to the ENT op with symptoms of deviated nasal septum and inferior turbinate hypertrophy both clinically and radiologically were studied after taking the inclusion criteria into careful consideration (Figure 1).
Figure 1: CT PNS.
It was essentially a double-blind prospective randomised control study in which all patients in the even number were assigned to septoplasty plus inferior turbinoplasty and all patients in the odd number were assigned to septoplasty alone [5].
General anaesthesia was preferred to do the procedure. Approximately 3-4 ml was injected into the sub-mucosa of both the inferior turbinates and the submucoperichondrial layer of the nasal septum. For surface decongestion of the nasal mucosa along with topical decongestion, cotton patties which was soaked in 4% lignocaine with adrenaline was used. For general anaesthesia, a 1:20000 concentration adrenaline is used for surface anaesthesia and a 1:200000 adrenaline solution as injection is used to prevent excess intraoperative bleeding. Septoplasty is performed with a zero degree Hopkins endoscope following infiltration and a Freer's incision on the nasal septum on the side of caudal displacement of the nasal septum, (Figure 2).
Figure 2: Mucoperichondrial and mucoperiosteal flaps.
This is followed by raising the mucoperichondrial and mucoperiosteal flaps on the same side of the incision. Then incision is made at the bony cartilaginous junction of the nasal septum and the opposite side of the mucoperiosteum is elevated (Figure 3).
Figure 3: Septal spur.
Septal spur with the deviated septum is removed using a Ballenger swivel knife. Mucoperichondrial and mucoperiosteal flaps are repositioned and sutured [6]. A vertical incision is made in the anterior aspect of the inferior turbinate after infiltrating it using a zero degree Hopkins rigid endoscope.
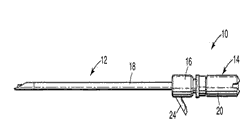
Figure 4: Turbinoplasty blade size 2.9 mm.
Then a microdebrider with a straight blade is inserted into the incision and along the medial aspect of the inferior turbinate the submucosal soft tissue is debrided out. A submucosal tunnel is created along the medial aspect of the inferior turbinate [7].
Hemostasis is achieved by placing cotton patties. Once hemostasis is achieved, nasal packing is done with gauze soaked in 1:20000 adrenalines. Nasal packs are removed after 24 hours (Figure 5).
Figure 5: Microdebrider assisted turbinoplasty.
Preoperatively and 3 months postoperatively the patients were given a questionnaire and asked to score the symptoms and improvement in lifestyle. SNOT-20 (sinonasal outcome test-20) original research, which was published in the journal of otorhinolaryngology, head and neck surgery (2007).
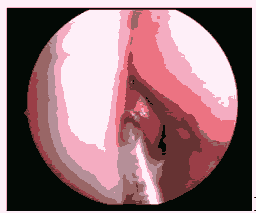
Modifications were done in the original SNOT-20 scoring system to satisfy the needs of our study. Five parameters were used for the analysis of nasal symptoms like irritability, nose block, facial pain, reduced concentration and difficulty in falling asleep (Figure 6).
Figure 6: Post op DNE left side with adequate first pass.
If the first pass is inadequate it means that either the scope cannot be passed to visualize the choana or the scope will be passed with great difficulty whereas adequate first pass indicates that the scope can be passed easily to visualize the choana [8].
Results and Discussion
A sample size of 100 patients were considered for the study out of which 50 patients underwent septoplasty alone and considered as the control group and the rest underwent septoplasty with inferior turbinoplasty using a microdebrider as considered to be the test group.
Out of the 50 patients who were taken as the test group, 23 patients underwent bilateral turbinoplasty, 18 had left turbinoplasty and 9 of them underwent right turbinoplasty along with septoplasty. The groups were randomized into test and control groups [9]. The improvement in symptoms and post objective diagnostic nasal endoscopy were considered at the end of 3 months which is better in the test group as compared to the control group to consider this study a success (Table 1).
Table 1: Total symptom score.
| Total Symptom Score | Preoperative Total | Postoperative Total | Difference | P Value | |
|---|---|---|---|---|---|
| Score | Score | Paired t Test | |||
| Endoscopic septoplasty | Mean | 12.38 | 8.12 | 4.26 | <0.001 |
| SD | 1.72 | 1.62 | |||
| Endoscopic septoplasty with inferior turbinoplasty | Mean | 13.58 | 3.18 | 10.4 | |
| SD | 1.79 | 0.9 | |||
On analysis of endoscopic septoplasty vs. endoscopic septoplasty with inferior turbinoplasty-pre-operative vs. post-operative total symptom score distribution table, it was evident that the difference in mean pre-operative vs. post-operative total symptom score is 4.26 score points in endoscopic septoplasty and 10.40 score points in endoscopic septoplasty with inferior turbinoplasty group (p=<0.001) [10].
Discussion
In patients with a deviated nasal septum and inferior turbinine hypertrophy, the study compared the outcomes of septoplasty and septoplasty with inferior turbinoplasty utilising a microdebrider. According to the inclusion and exclusion criteria, patients were accepted into the study. Patients with allergy symptoms or symptoms that were connected to allergies were excluded from the trial. Patients with co-morbid conditions were excluded from the study.
There was a 36.3% improvement in the control group who underwent only septoplasty as compared to the test group who underwent septoplasty and turbinoplasty with a 77% improvement in symptoms. Patients were taken as the control and test group by randomization. The study is a double blinded study.
Total Symptom Score
In our study the difference in mean pre-operative vs. post-operative total symptom score in endoscopic septoplasty with inferior turbinoplasty group compared to endoscopic septoplasty group was meaningfully high and significant. Increased mean pre-operative vs. postoperative difference in total symptom score in endoscopic septoplasty with inferior turbinoplasty group compared to endoscopic septoplasty (mean increased difference of 6.14 score points, 59% higher)
Our patients were followed up for a period of 3-6 months. The patients who underwent septoplasty with inferior turbinoplasty had no crusting or atrophic changes. In November 1999, expert’s did a similar study on 120 patients and came to a conclusion that “microdebrider assisted submucous resection of inferior turbinates” is safe to achieve turbinate reduction in patients with nasal obstruction which is caused due to turbinate hypertrophy. Crusting can be prevented by preservation of mucosa. It also helps in early healing. Using of a microdebrider helps in precise tissue removal and reducing the size of the inferior turbinate.
A study which was conducted by experts on 29 patients with chronic hypertrophic rhinitis was treated with endoscopic inferior turbinoplasty and an average increase in nasal airflow was observed. There was no permanent synechaie or atrophic change which is similar to our study.
Experts observed that there was a 91% improvement in the nasal obstruction as compared to 100% improvement in our study. They also proved that powered endoscopic turbinoplasty alongwith endoscopic septoplasty or sinus surgery is a surgical option for disease clearance. Another study which was done by group of experts did observe that there was a satisfactory improvement in nasal obstruction post septoplasty with inferior turbinectomy.
In 2010, experts published a study that showed that inferior turbinate surgery has positive outcomes, and we found that the test group used fewer decongestants and other medicines postoperatively than the control group. As a result, patients with turbinate hypertrophy who do not respond to conventional treatment should consider inferior turbinate surgery.
Ilium P did a study on 45 patients in 1993 and concluded that there was no subjective improvement from inferior turbinoplasty on the opposite side of the septal deviation whereas in our study there is a symptomatic improvement when septoplasty is combined with inferior turbinoplasty.
Conclusion
Cases of deviated nasal septum with symptoms of nasal obstruction were treated surgically by both septoplasty and submucous resection of septum. Nowadays septoplasty and Submucous resection of septum is combined with inferior turbinoplasty for better outcome. Precise tissue removal can be done in inferior turbinoplasty using a microdebrider with the help of endoscope as the visualization is better. Inferior turbinoplasty is advised as in our study there is an excellent improvement in the symptoms postoperatively as observed during follow up in patients undergoing septoplasty with inferior turbinoplasty as compared to the control group who underwent only septoplasty.
References
- Lee CF, Chen TA. Power Microdebrider Assisted Modification of Endoscopic Inferior Turbinoplasty: A Preliminary Report. Chang Gung Med J 2004; 27:359-365.
- Huang TW, Cheng PW. Changes in Nasal Resistance and Quality Of Life after Endoscopic Microdebrider-Assisted Inferior Turbinoplasty in Patients with Perennial Allergic Rhinitis. Arch Otolaryngol Head Neck Surg 2006; 132:990-993.
[Cossref] [Google Scholar] [Indexed]
- Wormald PJ. Powered Inferior Turbinoplasty and Endoscopic Septoplasty. Endoscopic sinus surgery: Anatomy, three dimensional reconstruction, surgical technique. 2008; 19-26.
- Serrano E, Percodani J, Woisard V, et al. Efficacy of Partial Inferior Turbinectomy in the Treatment of Nasal Obstruction, Retrospective Study Apropos of 71 Patients. In Annales D'otolaryngologie et de Chirurgie Cervico Faciale: Bulletin de la Societe D'otolaryngologie des Hopitaux de Paris 1996; 113:379-383.
- Baroody F, Naclerio RM. A Review of the Anatomy and Physiology of the Nose. Alexandria (VA): Amer Acad Otolaryngology Head Neck Surgery. 1990.
- Courtiss EH, Gargan TJ, Courtiss GB, et al. Nasal Physiology. Ann Plast Surg. 1984; 11:214-223.
[Cossref] [Google Scholar] [Indexed]
- Hasegawa M, Kern EB. The Human Nasal Cycle. Mayo Clin Proc 1977;52:28-34.
[Cossref] [Google Scholar] [Indexed]
- Alberti PW. Applied Surgical Anatomy of the Maxillary Sinus. Otolaryngol Clin North Am 1976; 9:3-20.
[Cossref] [Google Scholar] [Indexed]
- Lang J. Clinical Anatomy of the Nose, Nasal Cavity, and Paranasal Sinuses. NY: Thieme. 1989.
[Cossref]
- Libersa C, Laude M, Libersa J. The Pneumatization of the Accessory Sinuses of the Nasal Fossae during Growth. Anat Clin 1981; 2:265.
Author Info
Thrupthi S*, Rajasekar MK and Jayapreetha
Department of ENT, Sree Balaji Medical College and Hospital, Chrompet, Chennai, Tamil Nadu, IndiaCitation: Thrupthi S, Rajasekar MK, Jayapreetha. Comparison of Outcome of Endoscopic Septoplasty with Inferior Turbinoplasty using Microdebrider. J Res Med Dent Sci, 2022, 10 (5):17-21.
Received: 23-Feb-2022, Manuscript No. 41492; , Pre QC No. 41492; Editor assigned: 25-Feb-2022, Pre QC No. 41492; Reviewed: 11-Mar-2022, QC No. 41492; Revised: 24-Apr-2022, Manuscript No. 41492; Published: 02-May-2022