Research Article - (2021) Volume 9, Issue 12
Comparison of Progress of Labour with Maternal and Fetal Outcome with and Without Epidural Analgesia
*Correspondence: K. Saraswathi, Department of Obstetrics and Gynecology, Affiliated to Bharath Institute of Higher Education and Research, Chennai, Tamil Nadu, India, Email:
Abstract
In our study, 100 parturients in active labour (4cms) were selected according to inclusion and exclusion criteria stated in the methodology. Progress of Labour was plotted in both the groups with the help of Partogaph.periodically maternal vitals and fetal heart sounds were monitored. Duration of labour,mode of delivery,maternal complications, newborn apgars at 1 min and 5 mins and NICU admissions were compared. Duration of first stage and third stage is not affected by by epidural. Duration of second stage of labour is prolonged by epidural compared to the control group. Epidural analgesia is a safe,and,effective method of pain relief during labour.It is a boon to the parturating mothers. However the women randomised to epidural group had impact over the labour to some extent.Keywords
Anesthesia, RBC, HBB, Hydroxyurea, TurmericIntroduction
Pregnancy and motherhood is a major milestone in the life of a female which change her position in the family and the society giving more self confidence and independence. Child birth is a painful process and pain relief during labour has always been associated with myths and controversies. Several groups of people think that God has made this process painful and no interference should be done in it 1• However, from the early days several methods including primitive use of rings, neck less,distraction, and counter stimulation have been used to relieve labour pain. In modern era various nonpharmacological and pharmacological methods are being practiced for labour analgesia. Use of labour analgesia has gained wide spread popularity ever since the three famous women, Fanny Longfellow wife of famous American poet Henry Wadsworth Longfellow (1847), Emma Darwin wife of Charles Darwin the eminent Naturalist, and Queen Victoria wife of Prince Albert (1853) not only accepted but strongly endorsed the use of analgesia during birth process 1. The delivery of the infant into the arms of a conscious and pain free mother is one of the most exciting and rewarding moments in medicine'- More Pain relief in labour has always been surrounded with myths and controversies. Hence, providing effective and safe analgesia during labour has remained an ongoing challenge. Historically, the era of obstetric anaesthesia began with James Young Simpson, when he administered ether to a woman with a deformed pelvis during childbirth. His concept of "etherization of labour" was strongly condemned by critics! The religious debate over the appropriateness of anaesthesia for labour1 continued till 1853, when John Snow administered chloroform to Britain's Queen Victoria during the birth of her eighth child, Prince Leopold.2
JY Simpson also proposed that "Medical men may oppose for a time the super-induction of anesthesia in parturition, but they will oppose it in vain; for certainly our patients themselves will force use of it upon the profession. The whole question is, even now, one merely of time." This time came in the 1950s, when neuraxial techniques were introduced for pain relief in labour and, during the last two decades,3 there have been several advances that lead to comprehensive and evidence-based management of labour pain. Modern neuraxial labour analgesia reflects a shift in obstetrical anaesthesia, thinking away from a simple focus on pain relief towards a focus on the overall quality of anesthesia4. The International Association for the Study of Pain (IASP) declared 2007-2008 as the "Global Year against Pain in Women - Real Women, Real Pain." The focus was to study both acute pain and chronic pain in women. Labour pain was found to be a good study model for treating acute pain. Increasing knowledge of the physiology and pharmacotherapy of pain and the development of obstetric anaesthesia as a subspecialty has improved the training in obstetric anaesthesia, leading to an overall improvement in the quality of labour pain relief. In many countries today, the availability of regional analgesia for labour is considered a reflection of standard obstetric care. According to the 2001 survey, the epidural acceptance is up to 60% in the major maternity centres of the US. In our country, the awareness is still lacking and, except few centres that run a comprehensive labour analgesia programme, the national awareness or acceptance of pain-relieving options for women in labour virtually does not exist.
Material and method
This study was conducted in sree balaji medical college and hospital on 100 parturients, based on inclusion and exclusion criteria, after obtaining permission from the ethical committee. This was A single centre, cross sectional study, consisted 100 patients (sample size) Group I (Epidural analgesia) n=50 Group II (No analgesia) n=50. The inclusion criteria included parturient mothers with Singleton pregnancy, vertex presentation, Uncomplicated pregnancy, Willingness for epidural analgesia, Anaesthetist fitness for epidural analgesia. The patients with Patient refusal, Uncooperative patient, Pregnancy with other co-morbid conditions such as Elderly Gravida, grand multipara, Untreated coagulopathy or patient on any anticoagulant therapy, Neurologic or neuromuscular diseases, Thrombocytopenia, Infection at the injection site, Refractory hypotension, Allergy to local anesthetics and epidural set were excluded from the study. The study conducted after Institutional Ethical Committee approval and informed written consent on 100 full term parturient women of ASA status I and II who fits in inclusion criteria. Each participant in active labour with cervical dilatation at 4 cm will be randomized into two groups, in which group I receives epidural analgesia and group II receives no analgesia. The study group will be preloaded with 500ml of ringer lactate solution. PR, BP, RR of the mother and FHR is monitered for both the groups. Then Epidural infusion using bupivacaine 0.125% will be given by qualified anesthesiologists in L2-3 or L3-4 interspace. The catheter taped in place in all group I patients and monitored throughout labour. Passive descent was encouraged during second stage of labour. Third stage of labour is managed actively. Progression of labour is monitered with the help of partograph. Newborn apgar score recorded. The visual analogue pain scale (0-l00mm scale :0 = no pam , 100 = worst pam ever)was measured at the peak of contractions before and 5,10,20,and 30minutes administration of the epidural analgesia at an hourly intervals. Our primary outcome consists of the duration of labour, Mode of delivery, requirement for oxytocin augmentation, fetal and maternal outcome.
Results
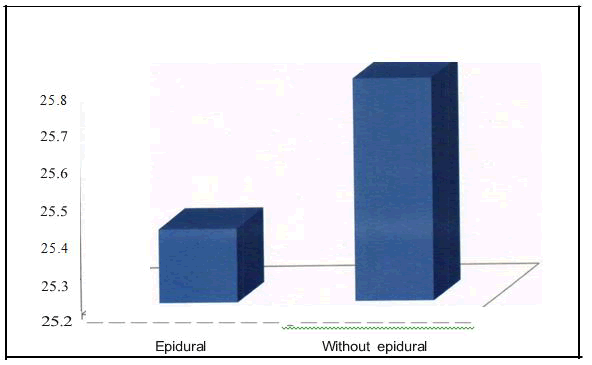
Table 1 showed the average age of the parturients in years. The average age in group I was 25.4 years and in group II was 25.8 years which falls in the age group of 20-35 years .
| Group | Mean (years) | S.D. |
|---|---|---|
| I | 25.4 | 2.7543 |
| II | 25.8 | 3.2343 |
Table1: Mean Age Distribution.
Figure 1: Mean age distribution.
Table 2 showed parity in both group. More of primiparous women prefered epidural than multiparous women.
| Parity | Group I | percentage | Group II | percentage |
|---|---|---|---|---|
| prumpara | 29 | 0.58 | 22 | 0.44 |
| Multipara | 21 | 0.42 | 28 | 0.56 |
| Total | 50 | 1 | 50 | 1 |
Table2: Parity of parturients.
Figure 2 : Parity of Patients.
Table 3 showed the average duration of 1st stage of labour. In Group !,average duration first stage of labour in primi was 4.17 hrs and in multi it was 2.57hrs.Total mean duration in group I was 6.74hrs(S.D.=l.7821). In Group II average duration in primi was 4.73hrs and in multi it was j:.89hrs.Total mean duration in Group II was 6.62hrs (S.D.=2.3585). Epidural had no impact on the I stage of labour, but, (p> 0.05) which is not significant.
| Group | Primi (hours) | Multi (hours) | Total Mean (hours) |
|---|---|---|---|
| I | 4.17 | 2.57 | 6.74 |
| II | 4.73 | i .89 | 6.62 |
Table3: Mean for Duration of I stage labour.
Figure 3 : Mean duration of 1st stage of labour.
Table 4 showed the average duration of 2nd stage of labour. In Group I average duration of primi in Group 1 was 17.247mins and in multi it was 6.883mins.Total mean duration of IInd stage of labour was 24.13 mins(S.D.=202559) . In Group II average duration in primi was13.732mins and in multi it was 7.233mins.Total mean duration being 20.965min(S.D.=17.0441). The p value is 0.0383 (< 0.05) which is significant. Epidural analgesia had impact on the II stage of labour.
| Group | Primi (minutes) | Multi (minutes) | Total Mean (minutes) |
|---|---|---|---|
| I | 17.247 | 6.883 | 24.13 |
| II | 13.732 | 7.233 | 20.965 |
Table4: Mean for Duration of II stage labour.
Figure 4 : Mean duration of 2nd stage of labour.
Table 5 shows the mean duration of 3rd stage of labour. In group I, average duration in primi was 3.79mins and in multi it was 2.69mins. Total mean duration was 6.48 mins ( S.D.= 1.474l)ln Group 11,average duration in primi was 3.82mins and in multi it was 2.56mins.total mean duration being 6.38 mins (S.D.=1.7010), p value is 0.740 (> 0.05) which was not significant. The Epidural has no impact on the III stage of labour.
| Group | Primi(minutes) | Multi(minutes) | Mean (minutes) | S.D. |
|---|---|---|---|---|
| I | 3.79 | 2.69 | 6.48 | 1.4741 |
| II | 3.82 | 2.56 | 6.38 | 1.701 |
Table5: Mean for Duration of III stage labour.
Figure 5: Mean duration of 3rd stage of labour.
Table 6 showed the incidence of instrumental delivery. In Group I 9/50(14%) parturients had instrumental delivery. Among which 6 were primi and 3 were multi .In Group II 5/50(10%). Among which 3 were primi and 2 were multi. p value was 0.03481 (< 0.05) which is significant. Epiduralanalgesiahad animpactmthemcreasem instrumental delivery.
| GROUPI | GROUP II | |
|---|---|---|
| Primi | 6 | 3 |
| Multi | 3 | 2 |
| 9/50 (14%) | 5/50(10%) |
Table6: Incidence of instrumental delivery.
Figure 6: Incidence of instrumental Delivery.
Table 7 showed the incidence of caesarean delivery. In Group I,5 out of 50 parturients(l0%) underwent LSCS. Among which 4 were primi and 1 was multi.whereas in Group II 4/50(8%) of the parturients underwent LSCS.Among which 3 were primi and 1 was multi. p value is 0.481 (> 0.05) which is not significant. Epidural analgesia does not increase the rate of caesarean section.
| GROUPI | GROUP II | |
|---|---|---|
| Primi | 4 | 3 |
| Multi | 1 | 1 |
| Total | 5/50(10%) | 4/50(8%) |
Table7: Incidence of cesarean delivery.
Figure 7: Incidence of caesarean delivery.
Table 8 showed the indication for caesarean section. In Group I 5/50(10%) underwent LSCS of which 3/5(60%) (2 primis and 1 multi)were due to fetal distress and 2/5 (40%)(2 primis) were due to cervical dystocia. In Group II 4/50 underwent LSCS of which 2/4(50%)(primi- 1,multi-1) were due to fetal distress and rest 2/5(50%)(22 primis) due to cervical dystocia.
GROUPI |
GROUP II |
|
|---|---|---|
Fetal distress |
3/5 (60%) (Primi-2 Multi-I) |
2/4 (50%) (Primi-1 Multi-I) |
Cervical dystocia |
2/5 (40%) (Primi-2 Multi-0) |
2/4 (50%) (Primi-2 Multi-0) |
Table8: Indication for cesarean section.
Figure 8: Indication for cesarean section
Table 9 showed the requirement of oxytocin augumentation of labour. In Group I, 62%(31 out of 50)women required oxytocin augumentation among whom 20 were prirni and 11 were multi. In Group II 52 %(26 out of 50) required oxytocin augumentation among whom 22 were prirni and 4 were multi. The p value is 0.0399 (< 0.05) which is significant. Epidural analgesia increased the need of oxytocin augmentation of labour.
| Parity | GROUPI | GROUP II |
| Prirni | 20 | 22 |
| Multi | 11 | 4 |
| Total | 31/50 (62%) | 26/50 (52%) |
Table9: Need for oxytocin augumentation of labour.
Figure 9: Need for oxytocin augumentation
Table 10 showed the incidence of complications. In Group I 4 (8%) and in Group II 5 (10%) had nausea &vomiting.In both Groups, 2 (4%) had PPH. Rest of the women (82%
| Complications | Group I | Percentage | Group II | Percentage |
|---|---|---|---|---|
| N&V | 4 | 0.08 | 5 | 0.1 |
| PPH | 2 | 0.04 | 2 | 0.04 |
| Maternal Hypotension | 0 | 0 | 0 | 0 |
| Total | 50 | 100 | 50 | 100 |
Table10: Maternal complications and side effects.
Figure 10: Complication
Table 11 showed the fetal outcome in both the groups. In group I 2 babies had apgar < 7 at lminute. In group II 1 baby had apgar < 7 at 1 minute. In both the groups there was 1 baby who had apgar <7 at 5 minutes and required NICU admission. Epidural had impact on apgar scores and NICU admissions.
| Outcome | Group I | Group II | P value |
|---|---|---|---|
| Apgar<7 at 1 min | 2 | 1 | P=0.06589 |
| Apgar<7 at 5 min | 1 | 1 | P=l |
| NICU admission | 1 | 1 | P=l |
Table11: Fetal outcome.
Figure 11: Fetal outcome.
Table 12 showed the incidence of different types of PPH. In Group I , two parturients in total suffered PPH of which one was a primipara who had traumatic PPH due to instrumental delivery and the other was a multiparous woman who had atonic PPH. In Group II both the parturients were multiparous and they suffered atonic PPH.
| Causes | GROUPI | GROUP II |
|---|---|---|
| Traumatic | 1/2 (primi) | 0 |
| Atonic | 1/2 (multi) | 2(multi) |
Table12: Cause for post partum hemorrhage.
Figure 12 : Incidence of postpartum hemorrhage
Table 13 showed the visual analogue score. In group I, 48 out of 50(96%) among whom 27 were primi and 21 were multi had no pain,, and rest 2 out of 50 (4%) (both were primis) had moderate pain. In group II 29 out of 50 (58%) among whom 2 were primi and 27 were multi who had moderate pain and 21 out of 50 (42%) among whom 20 were primi and lwas multi who had severe pam.
| Score | Group I | Group II |
|---|---|---|
| No pain(< 4) | Primi- 27, Multi- 21 Total-48 (96%) | 0 |
| Moderate pain (5,6,7) | Primi- 2, Multi- 0 Total-2 (4%) | Primi- 2, Multi- 27 Total-29 (58%) |
| Severe pain (8,9,10) | 0 | Primi- 20, Multi- 1 Total-21 (42%) |
Table13: Visual Analogue Scale.
Figure 13: Visual Analogue Scale
Discussion
Labour and child birth are natural events. Child birth an event of joy and satisfaction turns into a harrowing experience for some mothers due to labour pain.Labour and child birth,the normal and physiological process, produce significant pam, reqmrmg appropriate pam management. A varietyof anaesthesia techniques are used in conduct of normal labour. The ideal labour analgesic technique should be effective, safe for the mother and the foetus, should provide consistent, predictable rapid onset of analgesia in all stages of labour, should be devoid of motor blockade and preserve the stimulus for expulsive efforts required during the second stage of labour8. It is now well recognized that the only consistently effective method of pain relief in labour is lumbar epidural analgesia. Epidural anaesthesia the most frequently used method of pain control is reliable and preferred method of analgesia forever 60% hospitalized women in developed countries. An epidural anaesthesia is a procedure used to make a woman more comfortable during labour. The use of this technique allows the patient to be fully awake, even mobile making her participate in all aspects of the birth process. Epidural anaesthesia along with an experienced anaesthesiologist, a dedicated obstetrician and a trained mid-wife team can convert the painful labour into a less stressful event9.
In our present study, 100 parturient awaiting deliveries were chosen. 50 of the parturients received epidural analgesia at the time of active labour (4-5cm) as suggested by ACOG (ACOG statement in 2000- Evaluation of Cesarean delivery) and the progress of labour was continuously monitered with . The help of program along with periodical monitoring of fetal heart rate and the mothers vitals. Rest of the 50 parturients were not given labour analgesics and they were taken for control group. The parameters observed in our study were the effects of epidural analgesia over duration of labour,incidence of instrumental delivery,cesarean section, need for oxytocin augmentation ,complications,neonatal apgar score and NICU admissions.
In our study,epidural catheter was secured at greater cervical dilatation (4-5 ems) .The mean duration of first stage of labour appears to be slightly higher in the study group compared to control group ,but it is not statistically significant .Our study correlates with all the studies other than the meta-analysis conducted by Halpern9 (1998), in which he reported that Epidural analgesia was associated with a prolongation of the first stage of labor by an average of 42 minutes .This could be because, with the help of partogram,we have identified the parturients with poor cervical dilatation at an early stage and have augmented the labour with oxytocin.
In our present study, the duration of second stage of labour was prolonged compared to the control group,which is statistically significant. This is because when women do not feel the urge,pushing is more difficult for the women . Our study results correlates with the meta-analysis conducted by Cochrane collaboration 2011 and Halpern SH: More over according to meta-analysis conducted by Robyn M. Brancato! 200810, passive descent [The practice involves allowing the woman to delay pushing until she feels the urge to push or the head is visible at the vaginal introitus (delayed pushing)], increases a woman's chance of having a spontaneous vaginal birth, decreases risk of having an instrument assisted deliveries, decreases pushing time( prolonged pushing increase the incidence of fetal and maternal acidosis ). ACOG (2003) does recommend considering operative delivery when 3 hours have elapsed for a nullipara with analgesia and 2 hours for a multipara with analgesia11. In present study, the Duration of third stage of labour is similar to that of control group.
We found that incidence of instrumental delivery was significantly increased compared to control group. Although there is a significant increase in instrumental delivery, we were able to avoid some number of instrumental deliveries by following passive descent technique.
Present study shows that, epidural analgesia does not have any significant impact over incidence of cesarean delivery. And the indication for LSCS -3/5 is due to fetal distress and 2/5 is due to cervical dystocia. This is contradictory to the study by Thorp15 (1998) in which he reported an increase in number of LSCS in parturients with epidural analgesia because of dystocia (17 percent in the epidural group).This discrepancy was because we have identified the lag in the cervical dilatation in early stage and rectified it with oxytocin augumentation. In our study,the patients in the studygroup ,required significantly more oxytocin augumentation.this is supported by Merril and Zlatnik16 1999 who has reported that Length of labor, the primary outcome, was shortened with high dose oxytocin.
Cochrane Colloboration16 has conducted a meta-analysis on Epidural Versus non epidural analgesia in 2011, and reported that there is significant risk of Maternal hypotension associated with epidural analgesia. In present study, all parturients in the study group were preloaded with 500ml of Ringer's lactate solution before establishing the block, in order to decrease the incidence of hypotension following sympathetic blockade. So none of the patients in the study group reported Hypotension.This is supported by Vincent17 1998.
Our study shows that there were no significant effect of epidural over PPH.in either of the groups only two of the cases had PPH.in the study group among the two women, Multiparous had Atonic PPH for which her multiparity could have contributed for the atonicity.whereas in the other women who was a primi and had an instrumental delivery which in turn resulted in Traumatic PPH. Here Epidural analgesia contributed indirectly to the incidence postpartum haemorrhage by increasing the incidence of Instrumental delivery.our study is supported by a study conducted by Gilbert.
Our study shows that Epidural has no effect over Apgar score at birth and NICU admission. The 1 NICU admission was also due to cord around the neck rather than due any other complications associated with epidural analgesia (prolonged second stage, Matemal hypotension etc.,).
Limitation And SuggestionsAlthough this study was limited with time constrain, manual-steps process but it was good to establish such a study in Saudi Arabia where SCD affects many patients particularly in Eastern and South Western areas.
Further studies are recommended to identify the specific compounds of different parts of these herbs that pharmacologically cause their therapeutic activity. Moreover, dose and additive effects as well as drug-interactions are suggested in future evaluation. In addition, in vivo researches with more objective, practical and validated advanced techniques are recommended, also, to correlate all of that with the disease phenotypes in multicentre analysis on larger cohort groups to provide more understanding of the beneficial effects of such plant products.
Conclusion
Encouraging passive descent during second stage allows more number of spontaneous vaginal birth,and reduces the incidence of instrumental deliveries to some extent. This increases the duration of second stage of labour without affecting the fetal or maternal outcome. It requires little augmentation of labour to reduce the incidence of cesarean section due to cervical dystocia. These benifits should be made available to the women considering pain relief in labour.The decision about whether to have an epidural should then be made in consultation between the woman and her family.
AcknowledgementsThe encouragement and support from Bharath Institute of Higher Education and Research, Chennai, Tamil Nadu, India is gratefully acknowledged for providing the laboratory facilities to carry out the research work.
Declaration Of Conflict Of InterestThe authors declare no conflict of interest.
FundingNo funding sources.
Ethical ApprovalThe study was approved by the Institutional Ethics Committee.
References
- Snow J. On the administration of chloroform during parturition. Assoc Med J 1853;1:500.
- Salinas Lieberman E, O'donoghue C. Unintended effects of epidural analgesia during labor: a systematic review. Am J Obstet Gynecol 2002;186:31-68.
- Eltzschig HK, Lieberman ES, Camann WR. Regional anesthesia and analgesia for labor and delivery. N Engl J Med 2003;348:319-332.
- Rosen MA. Nitrous oxide for relief of labor pain: a systematic review. Am j obstet gynecol 2002;186:110-126.
- Cokic Brancato RM, Church S, Stone PW. A meta-analysis of passive descent versus immediate pushing in nulliparous women with epidural analgesia in the second stage of labor. J Obstet, Gynecol Neon Nurs 2008;37:4-12..
Author Info
Department of Obstetrics and Gynecology, Affiliated to Bharath Institute of Higher Education and Research, Chennai, Tamil Nadu, IndiaCitation: R. Ramya, K. Saraswathi Comparison of Progress of Labour with Maternal and Fetal Outcome with and Without Epidural Analgesia, J Res Med Dent Sci, 2021, 9(9): 1-8
Received: 01-Dec-2021 Accepted: 15-Dec-2021 Published: 22-Dec-2021