Research - (2021) Volume 9, Issue 1
Coronavirus Disease 2019 (Covid-19): Dentists Perception towards the Pandemic: A Questionnaire Based study
Manjari Chaudhary and Uma Maheswari TN*
*Correspondence: Uma Maheswari TN, Department of Oral Medicine, Saveetha Dental College and Hospitals, Saveetha Institute of Medical and Technical Sciences (SIMATS), Saveetha University Tamilnadu, India, Email:
Abstract
The epidemic of coronavirus disease 2019 (COVID-19), originating in China has become a global health challenge due to its spread worldwide. The World Health Organization announced that the outbreaks of the novel coronavirus have constituted a global health emergency. As of April 11, 2020, COVID-19 is affecting 210 countries and territories around the world and 2 international conveyances. The health care workers are at high risk especially the dentist community as the risk of cross infection is high between patients and dental practitioners. Strict and effective infection control protocols are urgently needed to prevent the virus from further spreading and to help control the epidemic situation. The aim of the study was to assess the general perception of the Dentist community in India towards pandemic Covid-19 and the measures taken by them for protection against SARS-CoV2. A study was conducted in form of a questionnaire, made with help of Google form, comprising 13 questions, circulated via social media like WhatsApp and Facebook to the various dentists residing in different states of India. The responses were recorded, and the representation was in the form of aggregated results. In this questionnaire study, 165 dentists working in different states of India responded to 13 compulsory questions. This study helps us to know that more awareness among the dentist community should be created and further steps to be taken to improve the infection prevention and control methods among dentists both in dental institution and in dental practice.
Keywords
COVID-19, Dentist, Pandemic, SARS-CoV2
Introduction
On January 8, 2020, Chinese Center for Disease Control and Prevention officially declared that novel coronavirus was as the causative pathogen of COVID-19 [1]. The current outbreak of the novel coronavirus SARSCoV-2 (coronavirus disease 2019; previously 2019- nCoV), epicenter in Hubei Province of the People’s Republic of China, has spread to many other countries and reached worldwide. The epidemics of coronavirus disease 2019 (COVID19) started in December 2019 and have become a public health problem in China and other countries around the world [2]. On 30th January 2020, the World Health Organisation (WHO) Emergency Committee had announced a global health emergency because of the continuously growing cases at Chinese and international locations [3]. The case detection rate is changing daily and can be tracked in almost real time on the website provided by Johns Hopkins University [4]. Professor Lauren Gardner at Johns Hopkins University in the US built the interactive dashboard with her graduate student Ensheng Dong to capture all confirmed COVID-19 cases, fatalities and recoveries and other forums. In February 2020, the largest mortality and morbidity rate was seen in China compared to other Asian countries, in Europe and North America.
COVID-19 and its uproar
Viral etiology
As per the recent research, SARSCoV-2 is like SARS-CoV and Middle East Respiratory Syndrome coronavirus (MERS-CoV), its zoonotic, with Chinese horseshoe bats (Rhinolophus sinicus) considered to be origin [5,6] and pangolins as the most likely intermediate host as described by The Chinese Preventive Medicine Association 2020. Coronaviruses are enveloped, positive single-stranded large RNA viruses. Coronaviruses were first described in 1966 by Tyrell and Bynoe [7]. Based on their morphology as spherical virions with a core shell and surface projections resembling a solar corona, they were termed corona viruses (Latin: Corona=crown). Four subfamilies, namely alpha-, beta, gamma and delta corona viruses exist. Alpha and beta corona viruses apparently originate from mammals, particularly from bats and gammaand delta-viruses originate from pigs and birds. The genome size varies between 26 kb and 32 kb. Among the seven subtypes of corona viruses that can infect humans, the beta-coronaviruses may cause severe disease and fatalities, whereas alpha-coronaviruses cause asymptomatic or mildly symptomatic infections [8,9].
Source of transmission
A seafood market in Wuhan, China is the source of place for SARS-CoV-2 which apparently succeeded in making its transition from animals to humans. Patients with symptomatic COVID-19 have been considered the main source of transmission. Asymptomatic patients and patients in their incubation period are also carriers of SARS-CoV-2 [5,10]. Due to this, its control is extremely challenging, as it is difficult to identify and quarantine these patients in time, which can result in an accumulation of SARS-CoV-2 in communities as per The Chinese Preventive Medicine Association 2020. Patients in the recovering phase are a potential source of transmission that remains to be proved [10].
Incubation period
On an average, the incubation period of COVID-19 has been estimated at 5 to 6 days. There is evidence that it could be if 14 days. This duration has been accepted for medical observation and quarantine of potentially exposed persons [11,12].
Who is at high risk of infection?
People of all ages are generally susceptible to this new infectious disease. However, those who are in close contact with patients with symptomatic and asymptomatic COVID-19, including health care workers and other patients in the hospital, are at higher risk of SARS-CoV-2 infection. In the early stage of the epidemic, in an analysis of 138 hospitalized patients with COVID-19 in Wuhan, 57 (41%) were presumed to have been infected in hospital, including 40 (29%) health care workers and 17 (12%) patients hospitalized for other reasons [13]. On February 14, 2020, a total of 1,716 health care workers in China were infected with SARS-CoV-2, consisting of 3.8% affected patients nationally, 6 of that group who have died. As of now, on 10th April 2020, coronavirus cases are 1,607,595 and deaths are 95,785 worldwide. In India, total cases are 6771 and deaths are 228. But the data for health care workers being infected in the hospital in India is yet unknown. Thus, it is important for the health care workers to take utmost care when dealing with confirmed or susceptible Covid-19 cases.
Methods of infection control and safe clinical practice in a dental setup
As per World Health Organization (WHO) 2020, SARS-CoV-2 can persist on surfaces for a few hours or up to several days, depending on the type of surface, the temperature, or the humidity of the environment. This reinforces the need for good hand hygiene and the importance of thorough disinfection of all surfaces within the dental clinic. Effective Infection Control Protocols Hand hygiene has been considered the most critical measure for reducing the risk of transmitting microorganism to patients [14]. Dental apparatus could be contaminated with various pathogenic microorganisms after use or become exposed to a contaminated clinic environment. Thereafter, infections can occur through the puncture of sharp instruments or direct contact between mucous membranes and contaminated hands [15].
In dental colleges/clinics/hospitals of India
On 17th March 2020, the Dental Council of India (DCI) in addition to Ministry of Health & Family Welfare, Government of India had issued an advisory to the dentists and all the Dental Colleges of the Country regarding the precautionary and preventive measures to prevent spreading of Novel Coronavirus (COVID-19). The advisory stated that all the faculty and students at the dental colleges are barred from using Biometric Attendance instead opting for manual attendance. Classes, seminars, workshops, conferences, camps etc. are suspended. Clinical procedures involving aerosol generation (Air rotor/ Ultrasonic Scalers) are avoided/ minimized for the time being and only emergency procedures were performed. Disposal gloves to be used routinely as usual. Staff and doctors are asked to avoid touching their face specially the ear, nose and mouth. Every patient who entered and exited the clinic will be provided hand sanitizers. The waiting room/clinic including the handles and doors as well as dental chairs and other surfaces will be wiped several times in a day with alcohol-based disinfectant. Thorough medical & travel history of each patient were recorded before any clinical procedures. Patients should be scrubbed with Isopropyl alcohol extra orally. Pre-procedural rinse with Povidone Iodine is recommended. Wearing of N95 or at least 3 ply masks and suitable head caps, eyewear and face shield is recommended. Fumigation of clinics periodically is advised.
On March 15, 2020, an article was published in New York Times by Lazaro Gamio on ‘The Workers Who Face the Greatest Coronavirus Risk.’ The article was about the people with jobs that put them in physical contact with many others considered to be at higher risk of becoming sick. The vertical position of each bubble measures of how often workers in each profession are exposed to disease and infection. The horizontal position measures of how close people are to others during their workdays. The graph depicts that the Health care workers are at the greatest risk — they can encounter diseases and infections daily and typically work near one another and their patients.
Therefore, our study aims to know the general perception of the Dentist community in India towards pandemic Covid-19 and the measures taken by them for protection against SARS-CoV2.
Materials and Methods
A study was conducted in form of a questionnaire, made with help of Google form, comprising 13 questions, circulated via social media like WhatsApp and Facebook to the various dentists residing in different states of India. The responses were recorded, and the representation was in the form of aggregated results.
The personal information like the age, gender and the state in which the applicant is residing in was recorded. The details about the qualification like whether the applicant is an undergraduate or a postgraduate were asked.
Questions about their current work profile like whether they are attached to the dental institution or a dental clinic or both and also about the years of work experience was recorded. The applicant was also asked about the number of patients he/she is attending in his/her clinic or dental institution during this lockdown, and what complaint of the patient are they addressing? Whether the dentist is dealing with pain cases, emergency cases or all cases.
The applicant was also asked whether he/she feels that whether the dentist community is at the higher risk of contacting the covid-19 disease and what precautionary measures one has to take when dealing with patients who have come to them for the treatment and also how are they protecting their family from not getting infected after they return from the clinic. For example, sterilization of the equipment, disinfectants for cleaning the work area, hand washing with soap and water or use of hand sanitizers and following the disposal of the Biowaste as per the Covid-19 guidelines.
Results and Discussion
In this questionnaire study, 165 dentists working in different states of India responded. Out of which 61.8% dentist were females and 38.2% were males (Figure 1) with 68.2 % were below the age of 30 years whereas 24.2% of the dentists belonged to 30- 40 years age range (Figure 2) The undergraduates (Bachelor of Dental Surgery) dominated the study with 52.1% of the all the dentists taking part in this questionnaire study as shown in Figure 3. The dentists were either attached to the dental institute or had a private practice/ clinic or both (Figure 4) 71.5% of dentists having less than 5 years of work experience (Figure 5).
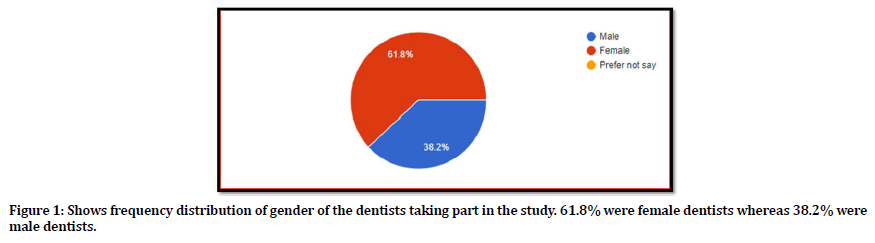
Figure 1. Shows frequency distribution of gender of the dentists taking part in the study. 61.8% were female dentists whereas 38.2% were male dentists.

Figure 2. Shows frequency distribution of age of the dentists taking part in the study. 69.1% (blue) of the dentists were below 30 years of age.
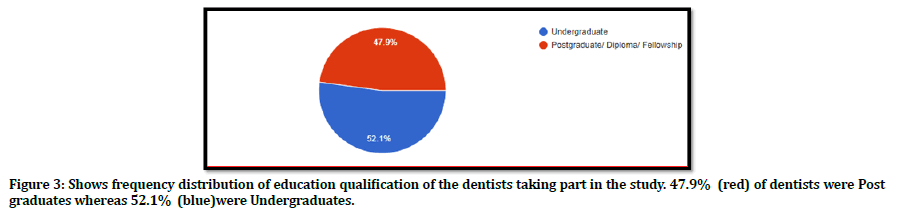
Figure 3. Shows frequency distribution of education qualification of the dentists taking part in the study. 47.9% (red) of dentists were Post graduates whereas 52.1% (blue)were Undergraduates.
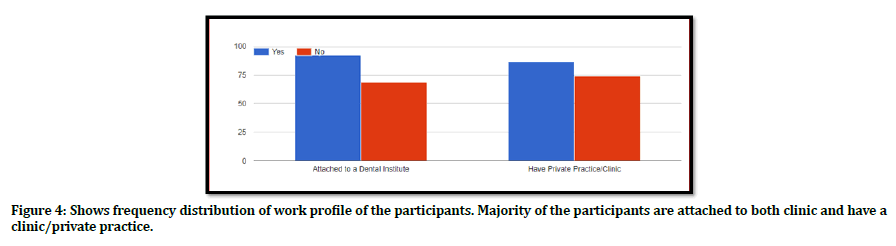
Figure 4. Shows frequency distribution of work profile of the participants. Majority of the participants are attached to both clinic and have a clinic/private practice.
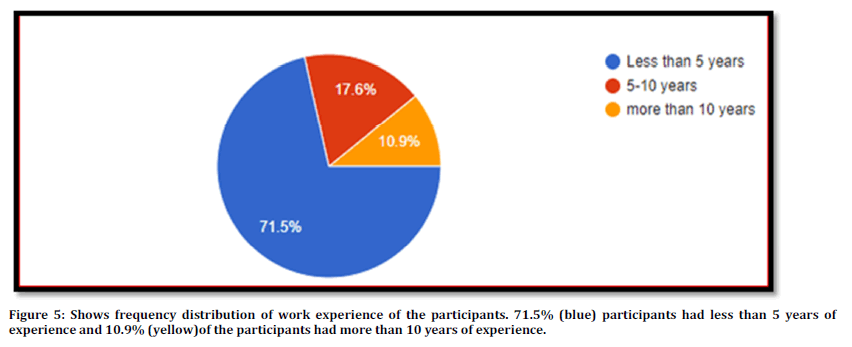
Figure 5. Shows frequency distribution of work experience of the participants. 71.5% (blue) participants had less than 5 years of experience and 10.9% (yellow)of the participants had more than 10 years of experience.
Figure 6 shows the distribution of the participants according to their states they are residing in; this pandemic was maximum in Maharashtra followed by Tamil Nadu. 96.3% dentist participants believed that they were at the higher risk of contracting Covid-19 disease whereas, 3.7 % dentists still believed that they weren’t at higher risk of contracting the disease or were unsure about it (Figure 7)
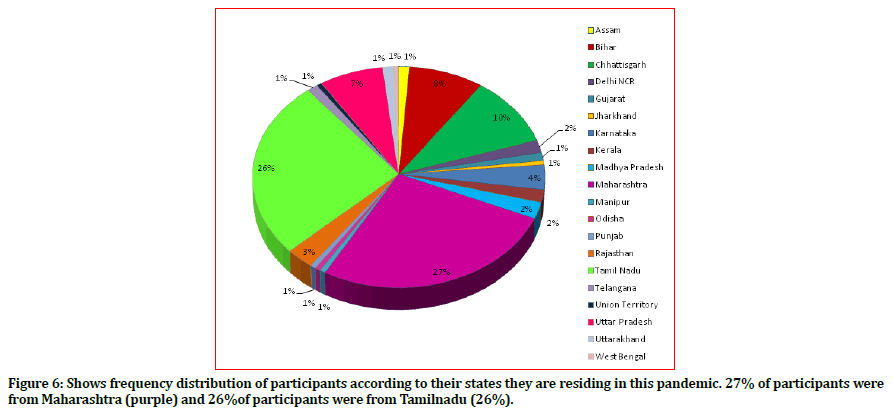
Figure 6. Shows frequency distribution of participants according to their states they are residing in this pandemic. 27% of participants were from Maharashtra (purple) and 26%of participants were from Tamilnadu (26%).
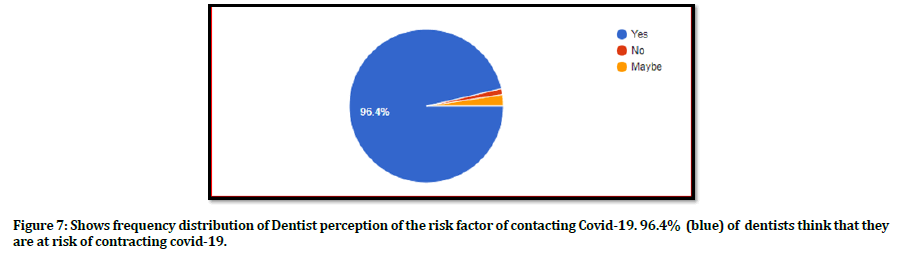
Figure 7. Shows frequency distribution of Dentist perception of the risk factor of contacting Covid-19. 96.4% (blue) of dentists think that they are at risk of contracting covid-19.
The participants were asked about the patients they were attending in the clinic or in the dental institution every day, in this pandemic. 52. 8% of the participants said that they were attending zero patients whereas 8.7% of the participants were attending more than 10 patients every day as shown in Figure 8, with 20 % of patients visiting dentists with chief complaints of pain and 58.8% of cases as emergency cases (Figure 9). Figure 10 shows the precautionary measures taken by the participants at their workplace. They were asked about the use of thermal scanners to check the temperature of the patients visiting them. About 55 of the study participants don’t use the thermal scanners for their patients. More than 150 of the study participants asked about the travel history of the patients visiting them and avoided crowing of the patients in the clinic or waiting area, that is they followed social distancing.
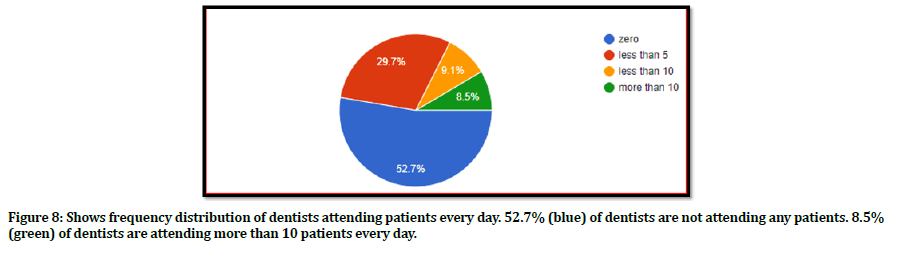
Figure 8. Shows frequency distribution of dentists attending patients every day. 52.7% (blue) of dentists are not attending any patients. 8.5% (green) of dentists are attending more than 10 patients every day.
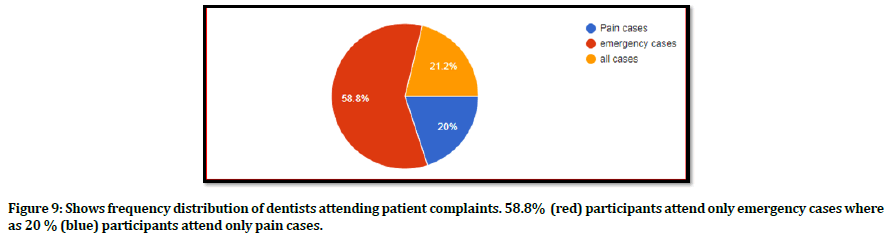
Figure 9. Shows frequency distribution of dentists attending patient complaints. 58.8% (red) participants attend only emergency cases where as 20 % (blue) participants attend only pain cases.
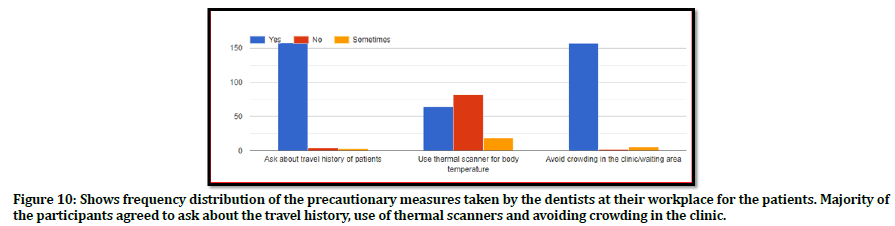
Figure 10. Shows frequency distribution of the precautionary measures taken by the dentists at their workplace for the patients. Majority of the participants agreed to ask about the travel history, use of thermal scanners and avoiding crowding in the clinic.
Figure 11 shows the precautionary measures taken by the participants at their workplace for themselves. More than 150 participants accepted that they use gloves at all the times when dealing with patients. About 100 participants said that they use a N95 mouth mask, eyewear/face shield whereas approximately 55 participants said that they use a gown when dealing with patients.
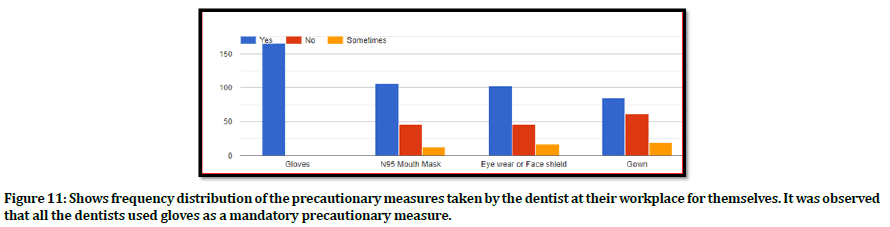
Figure 11. Shows frequency distribution of the precautionary measures taken by the dentist at their workplace for themselves. It was observed that all the dentists used gloves as a mandatory precautionary measure.
Figure 12 shows the sterilization and infection control methods taken by the study participants at the workplace. More than 150 study participants follow use of hand sanitizer/hand wash and disinfectants for cleaning the work area before and after every procedure and sterilizes the equipment after every procedure whereas approximately 120 study participants follow biowaste disposal as per Covid-19 guidelines.
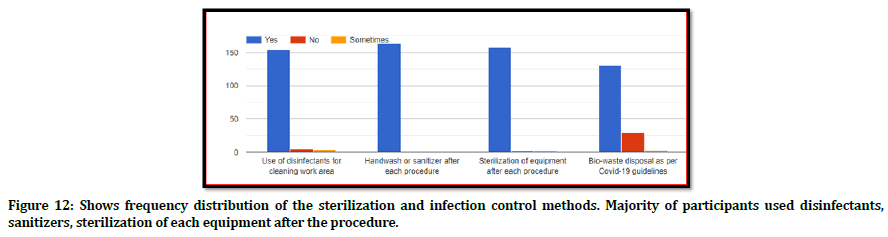
Figure 12. Shows frequency distribution of the sterilization and infection control methods. Majority of participants used disinfectants, sanitizers, sterilization of each equipment after the procedure.
Figure 13 shows the measures taken by the study participants in protecting the family from infection after coming home from work. 36% of the study participants take a bath after coming home from work. 16% wash their hands and feet immediately whereas 47% of the study participants both take a bath and wash their hands and feet immediately after coming home from work.
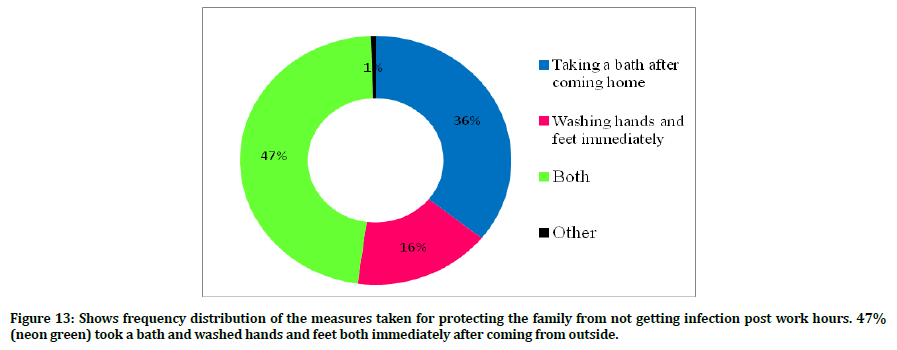
Figure 13. Shows frequency distribution of the measures taken for protecting the family from not getting infection post work hours. 47% (neon green) took a bath and washed hands and feet both immediately after coming from outside.
Conclusion
The study helps us to conclude that we, the dentist community should follow the instructions and recommendations from the World Health Organization, Control for Disease Center for both infection prevention and control during the pandemic situation. The dentist community like other health care professionals has a higher risk of contracting various infections which may prove fatal. Creating awareness and further steps to be taken to improve the infection prevention and control methods among dentists both in dental institutions and in dental practice.
Acknowledgment
We would like to thank Saveetha Dental College for providing us with the opportunity to conduct this study.
Author Contributions
Both the authors have discussed the results and contributed to the final manuscript.
Conflict of Interest
Nil.
References
- Li Q, Guan X, Wu P, et al. Early transmission dynamics in Wuhan, China, of novel coronavirus–infected pneumonia. New England J Med 2020; 382:1199-1207.
- Phelan AL, Katz R, Gostin LO. The novel coronavirus originating in Wuhan, China: challenges for global health governance. JAMA 2020; 323:709-710.
- Velavan TP, Meyer CG. The COVID‐19 epidemic. Tropical Med Int Health 2020; 25:278–280.
- Johns Hopkins C. Coronavirus 2019-nCoV global cases. Center for Systems Science and Engineering, Johns Hopkins University 2019.
- Chan JF, Yuan S, Kok KH, et al. A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: A study of a family cluster. Lancet 2020; 395:514-523.
- Lu R, Zhao X, Li J, et al. Genomic characterisation and epidemiology of 2019 novel coronavirus: Implications for virus origins and receptor binding. The Lancet 2020; 395:565-574.
- Tyrrell DA, Bynoe ML. Cultivation of viruses from a high proportion of patients with colds. The Lancet 1966; 1:76–77.
- Shu Y, McCauley J. GISAID: Global initiative on sharing all influenza data – from vision to reality’, Eurosurveillance 2017; 22:30494.
- Zhou P, Yang XL, Wang XG, et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 2020; 579:270–273.
- Rothe C, Schunk M, Sothmann P, et al. Transmission of 2019-nCoV infection from an asymptomatic contact in Germany. New England J Med 2020; 382:970-971.
- Backer JA, Klinkenberg D, Wallinga J. Incubation period of 2019 novel coronavirus (2019-nCoV) infections among travellers from Wuhan, China, 20--28 January 2020. Eurosurveillance. European Centre for Disease Prevention and Control 2020; 25:2000062.
- Li ZY, Meng LY. Prevention and control of novel coronavirus infection in department of stomatology. Chinese J Stomatol 2020; 55:217–222.
- Wang D, Hu B, Hu C, et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus–infected pneumonia in Wuhan, China. JAMA 2020; 323:1061-1069.
- Larson EL, Early E, Cloonan P, et al. An organizational climate intervention associated with increased handwashing and decreased nosocomial infections. Behavioral Med 2000; 26:14-22.
- Kohn WG, Harte JA, Malvitz DM, et al. Cover story guidelines for infection control in dental health care settings—2003. J Am Dent Assoc 2004; 135:33-47.
Author Info
Manjari Chaudhary and Uma Maheswari TN*
Department of Oral Medicine, Saveetha Dental College and Hospitals, Saveetha Institute of Medical and Technical Sciences (SIMATS), Saveetha University Tamilnadu, Chennai, IndiaCitation: Manjari Chaudhary, Uma Maheswari TN, Coronavirus Disease 2019 (Covid-19): Dentists Perception Towards the Pandemic: A Questionnaire Based study, J Res Med Dent Sci, 2021, 9 (1): 267-273.
Received: 23-Sep-2020 Accepted: 28-Dec-2020
