Case Report - (2022) Volume 10, Issue 1
Delayed Development of Mandibular Second Premolar: Review and 7 Years follow up Case Report
*Correspondence: Zain Hafiz, Department of Pediatric Dentistry and Orthodontics, College of Dentistry, King Saud University, Riyadh, Saudi Arabia, Email:
Abstract
Hypodontia defined as the congenital absence of one or more permanent teeth and the delay in tooth formation is considered a milder presentation of tooth agenesis. In this case report, a case of 12.5 years old girl with delayed formation of a mandibular left second premolar for which she was followed up for 7 years. The mandibular left second premolar was congenitally missing at the initial radiographic examination when the patient was 5.5 years. At the age of 7.5 years, in the recall visit, an unexpected ontogenesis of the mandibular left second premolar took place. The initial treatment plan with the orthodontist was modified and new treatment options were discussed. It was concluded that pediatric dentist and orthodontist should follow up their growing patients with congenitally missing second premolars until the age of 7 years or even later and schedule them for a regular recall radiographic examination to confirm the diagnosis before finalizing the treatment plan.
Keywords
Congenitally missing, Second premolar, Delayed odontogenesis, Growing patients
Introduction
Directing the eruption and development of the primary, mixed, and permanent dentitions is an important part of oral and dental care for all pediatric dental patients. This will aid in the development of an acceptable occlusion of permanent dentition which is stable functionally and esthetically. Achieving occlusal harmony and function and dentofacial esthetics is usually based on early diagnosis and successful early intervention of developing malocclusions [1-4]. Dentists specially orthodontists and pediatric dentists are responsible for the diagnosis, prevention, interception, treatment and referrals (if needed) of malocclusions of the teeth and abnormalities of the surrounding structures [5].
Hypodontia is an inherited condition diagnosed when 1 or more permanent teeth are developmentally missing. Its prevalence is 3.5% to 6.5% [6,7]. The frequently congenitally missing teeth are third molars (wisdom teeth), secondly, mandibular second premolars followed by the maxillary lateral incisors [6,8]. Furthermore, the prevalence of second premolars to be congenitally missing is 3% [9-13]. Shafi et al. examined 1100 OPG’s for children 6-14 years who attended the College of Dentistry, King Khalid University in Saudi Arabia to determine the prevalence of congenitally missing premolars. They found that the prevalence for congenitally missing premolar was seen more in females (59.4%) than males (40.6%) and that the frequently congenitally missing premolar was the lower 2nd premolar followed by the upper 2nd premolar in both female and male participants [14].
Tooth agenesis may be represented as late tooth formation [15-17]. Mineralization of the premolars starts in the majority of the cases at the age of 1.5-2 years for first premolars and 2-2.5 years for second premolars [18,19]. Ravn et al. radiographically examined 104 children who were 3-7 years of age. The participants appeared to have no visible one or more tooth germs mesial to the first permanent molar. The areas with apparent tooth agenesis were radiographically re-examined. After 16-24 months re-examination of the same areas was done, and the two examinations were compared to each other. Their study confirmed that the 2nd premolar can show delayed development with greater chance to occur in the maxilla than in the mandible [20]. Memmott et al. reported a case of a late agenesis of a maxillary second premolar. The patient was examined radiographically when she was 11 years old and the premolar was diagnosed to be congenitally missing. The maxillary second premolar developed when the patient was between the ages 12-16 years. Moreover, the premolar was discovered when the patient was 17 years of age and came for a recall visit complaining of intermittent discomfort in the upper left area. The panoramic radiograph showed the upper left second premolar was developing [21]. As well, Becakci et al. presented a case of a female with a lower second premolar late formation and she was followed up for eight and a half years. At 8 years of age, her initial radiographic examination revealed congenitally absent second premolars. Unexpectedly, after a year and during the orthodontic intervention, formation of a right second premolar was interpreted during the recall radiographic examination.
The treatment plan was modified and implanted successfully [22]. Moreover, Ying at al. (2020) treated a case of a 16 years old Asian adolescent whose bilateral upper second premolar germs were at Nolla's 6 stage as it appears on the panoramic radiograph.
They reported that it is unusual that tooth germs of the maxillary second premolar to be developed after 11 years of age. In addition, they concluded that to limit the chance of misdiagnosis, clinicians should consider the possibility of the delayed tooth development if a tooth germ doesn’t appear in the initial radiographs of a child [23].
Based on the reported cases in the literature on the delayed development of maxillary and mandibular second premolars, the clinician who finds no evidence of developing second premolars in pediatric patient older than age 6 may formulate a treatment plan that would consider the tooth congenitally missing [24].
Additionally, there are several reports in the literature of an apparent initial lack of radiographic evidence of developing second premolars; clinicians should follow up the pediatric patient at age 8, 10, or even 13 and radiographically examine the patient for any developing second premolars [24-26].
This clinical article will report the late development of mandibular left second premolar in a 12 years old female patient.
Patient presentation
Medical and dental history
A twelve-year-old healthy female reported to the pediatric dental clinic with the chief complaint of pain and discomfort in the lower left back teeth region.
The patient is a regular patient at the pediatric dentistry clinic since she was 5 years of age and she regularly attends her follow up sessions.
In 2013 at the age of 5.5 the patient came to the pediatric dental clinic complaining of eruption of lower frontal adult teeth.
Intraoral examination showed that the permanent mandibular central incisors were erupting lingual to the primary mandibular central incisors.
In addition, panoramic radiograph was requested, and radiographic interpretation showed that #35 is congenitally missing (Figure 1).
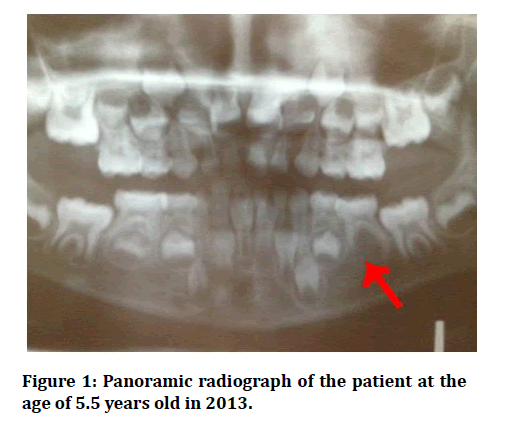
Figure 1: Panoramic radiograph of the patient at the age of 5.5 years old in 2013.
The family and medical history of the child patient regarding missing teeth was significant since the father has bilateral congenitally missing mandibular second premolars. The other teeth were of normal color, size and shape. In 2015 the patient came for a follow up visit and she was 7 years old. The panoramic radiograph showed stage 3 left mandibular second premolar development based on Nolla’s development stages [27]. In addition, since the parent of the child refused to take panoramic radiograph without the thyroid collar covering her child neck, the quality of the radiograph was reduced, however it was still considered as diagnostic (Figure 2).
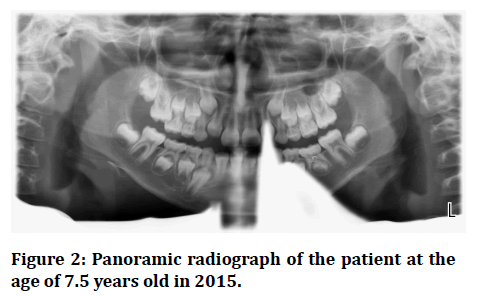
Figure 2: Panoramic radiograph of the patient at the age of 7.5 years old in 2015.
Follow up panoramic radiographic examination of the patient have been done on the years 2016 (Figure 3), 2017 (Figure 4), 2018 (Figure 5).
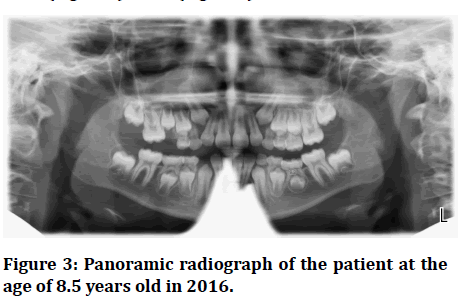
Figure 3:Panoramic radiograph of the patient at the age of 8.5 years old in 2016.
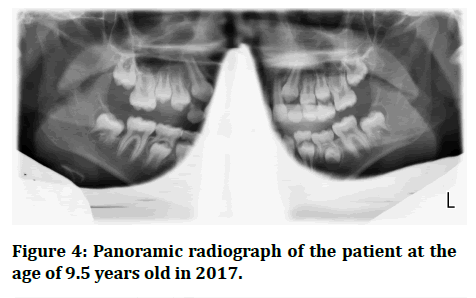
Figure 4:Panoramic radiograph of the patient at the age of 9.5 years old in 2017.
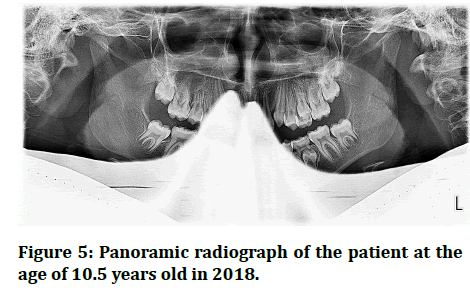
Figure 5:Panoramic radiograph of the patient at the age of 10.5 years old in 2018.
In 2020, the patient attended her recall visit complaining of pain triggered with pressure on the left lower back tooth. Intraoral examination showed #75 pinkish in color and mobile (Figure 6). When the crown of #75 was remove it came out in two pieces (Figure 7). After 2 months a panoramic radiograph was requested and showed that the left mandibular second premolar has erupted but in a rotated position (Figure 8).
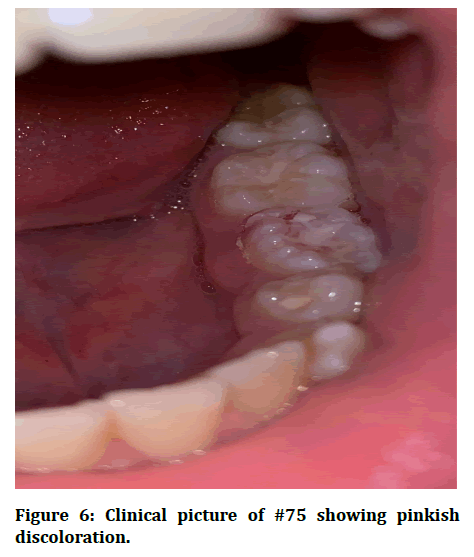
Figure 6:Clinical picture of #75 showing pinkish discoloration.
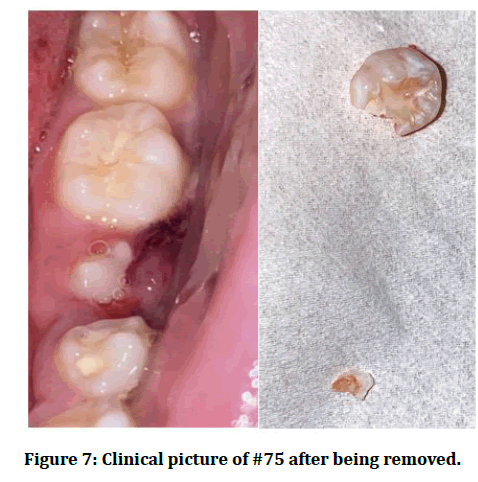
Figure 7:Clinical picture of #75 after being removed.
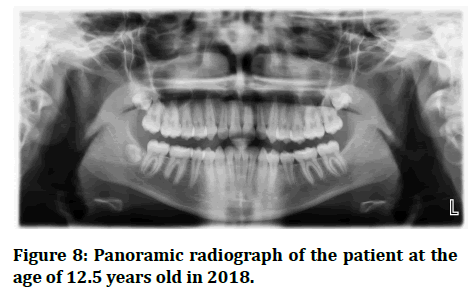
Figure 8:Panoramic radiograph of the patient at the age of 12.5 years old in 2018.
Additionally, the patient was referred to the orthodontic clinics and was examined by an orthodontist. Two options were discussed by the orthodontist: (1) either leaving the tooth as it is in its rotated position since it doesn’t interfere with the function, esthetic and oral health of the adolescent, (2) or if the patient planned to correct the position of the left mandibular second premolar when its root is fully formed and closed, orthodontic treatment will be done to correct its rotated position. Moreover, in a routine radiographic examination for the patient’s younger male sibling who’s aged 7 years, it was discovered that the sibling has left mandibular second premolar that seems to be congenitally missing. However, based on his older sister’s case the patient will be regularly followed up to confirm this diagnosis.
Discussion
Several studies have reported that lower second premolars have the most variations in differentiation and calcification stages after third molars in permanent dentition [28,29]. Usually, second premolars calcify when the child is 2-2.5 years old, and the crown is completely formed when the child is 6-8 years old. It’s not uncommon for the mandibular second premolars to show delayed calcification starting at the age of 5-6 years old [20,30]. Moreover, the agenesis of second premolar is commonly confirmed when the child is at the age of 8-9 years [22]. In the present case, initial panoramic radiograph examination showed that the left mandibular second premolar was assumed congenitally missing when the female pediatric patient was 5.5 years old who has a family history in which her father has bilateral congenitally missing mandibular second premolars. However, during the follow up visits of the patient when she was 7.5 years old, it was observed on the panoramic radiograph that she has delayed development of left mandibular second premolar.
Based on the initial assessment in the first visit including significant family history of congenitally missing mandibular second premolars, development of the contralateral right mandibular second premolar and knowing that the mandibular second premolar is the most frequently congenitally missing tooth following third molars, it was not expected that the late formation of the mandibular second premolar would occur in an almost 6-yearold pediatric patient.
Moreover, when the patient was 6 years old, the orthodontist formulated an initial treatment plan: (1) either keep the primary left mandibular second molar until all permanent teeth are fully erupted, then extraction of #75 and space closure using conventional orthodontic treatment, (2) or when the patient is 18 years old, #75 will be extracted and implant will be placed in the mandibulae second premolar place. Whereas, this initial orthodontic treatment plan was changed as the late formation of the left mandibular second premolar took place in the follow up visit when the patient was 7.5 years old.
Different treatment choices would be considered for patients with congenitally missing second premolars. Treatment considerations are based on: (a) the age of the patient, (b) the developmental stage for the adjacent teeth, (c) and the status of the primary tooth including the tooth’s condition regarding root resorption and infraocclusion. As the patient becomes 9 years old, treatment options become less. Spontaneous closure of the space might not be a valid choic [31]. Svedmyr (1983) advised the removal of the retained primary second molar before the first permanent molar erupts allowing a spontaneous closure of the space [32]. However, Berstrom (1977) and Rolling (1980) reported that it is not possible to confirm the absence of the second premolars before the age of 9 [28,33]. In addition, spontaneous space closure takes place, if the second premolar removal was done before the completion of the mandibular first permanent molar root development and before the emergence of the second permanent molar [34]. However, in a few cases, such as the one reported here, the treatment options were modified as the second premolar started its delayed formation and was left under observation to assure it erupts in its normal space. Delayed tooth development is a mild representation of tooth agenesis [15-17].
Although congenitally missing teeth is occasionally caused by environmental factors, like an infection (e.g. rubella), various dental traumatic injuries, chemotherapy or radiotherapy, or disturbed innervations of the jaw, most of the cases of hypodontia have genetic reasons [35,36]. Furthermore, by the end of the primary dentition phase which is estimated to be 5-6 years of age, 28 permanent tooth buds with various stages of calcification are usually present within the alveolar bones, except for the third molars that start to calcify by the age of 9 years. During this age (5-6 years old), panoramic radiographs often show 48 teeth, which are the 20 erupted primary teeth and the 28 permanent successors buds in various stages of odontogenesis. In the literature, it has been reported that second premolars start calcifying between 2 and 3 years of age [18]. However, in most cases it has been reported that the odontogenesis of second premolars starts at 3 or 3.5 years of age, with more variability than the rest of the permanent teeth [20]. Based on that, diagnosing the agenesis of lower second premolars should not be done before the child is 6-7 years old as was found in this case where the mandibular left second premolar started to calcify after the age of 7 years. This results from the “apparent tooth agenesis” in which the premolar is found developing, often in a later stage [21,26,37].
In addition, the transcription factor genes MSX1 and PAX9 were the genes that firstly recognized for tooth agenesis that is not related to syndromes [38,39]. It is reported that these genes have an effect on third molars, however, it was found that the higher frequency of agenesis was highly associated with mutations in MSX1 than in PAX9 that has been reported to be associated with second premolars and maxillary first premolars [15]. In the current case, all third molars were detected except for the mandibular left third molar, which may suggest an association between the agenesis of the third molar and the delayed development of the second premolar. This finding contradicts to the results presented by past case reports [22,26,37]. Therefore, these findings show that the predicted cause of the unilateral delayed development of the mandibular left second premolar might be attributed to the MSX1 gene mutation.
Finally, to minimize the risk of misdiagnosis, radiographic evaluation (panoramic radiograph) and periodic periapical x-rays every 6 months for the area with tooth agenesis should be interpreted carefully in growing patients in which unusual circumstances may take place.
Conclusion
Pediatric dentists and orthodontists should consider the late tooth odontogenesis in growing patients. To provide the proper case management a final treatment plan should not be formulated before a careful radiographic evaluation including series of radiographs to confirm the agenesis of the mandibular second premolar in a growing patient.
References
- Kanellis M. Orthodontic treatment in the primary den-tition. In: Bishara SE, Edn. Textbook of Orthodontics. Philadelphia, WB Saunders Co 2001; 248-56.
- Woodside D. The significance of late developmental crowding to early treatment planning for incisor crowding. Am J Orthod Dentofacial Orthop 2000; 117:559-61.
- Kurol J. Early treatment of tooth-eruption disturbances. Am J Orthod Dentofacial Orthop 2002; 121:588-91.
- Sankey W, Buschang P, English J, et al. Early treatment of vertical skeletal dysplasia: The hyper-divergent phenotype. Am J Orthod Dentofacial Orthop 2000; 118:317-27.
- Friedman M. Dentists and other oral health care providers. WebMD Med Ref 2019.
- Byrd E. Incidence of supernumerary and congenitally missing teeth. J Dent Child 1943; 10:84-6.
- Brook A. Dental anomalies of number, form, and size: Their prevalence in British school children. J Int Assoc Dent Child 1974; 5:37-53.
- Rose J. A survey of congenitally missing teeth, excluding third molars, in 6,000 orthodontic patients. Dent Pract Dent Rec 1966; 17:107-14.
- Bergström K. An orthopantomographic study of hypodontia, supernumeraries and other anomalies in school children between the ages of 8â??9 years. An epidemiological study. Swed Dent J 1977; 1: 145â??57.
- Locht S. Panoramic radiographic examination of 704 Danish children aged 9-10 years. Community Dent Oral Epidemiol 1980; 8:375â??80.
- Polder B, Van’t Hof M, Van der Linden F, et al. A meta-analysis of the prevalence of dental agenesis of permanent teeth. Community Dent Oral Epidemiol 2004; 32:217â??26.
- Rølling S, Poulsen S. Agenesis of permanent teeth in 8138 Danish schoolchildren: Prevalence and intra-oral distribution according to gender. Int J Paediatr Dent 2009; 19:172-75.
- Rakhshan V. Meta-analysis of observational studies on the most commonly missing permanent dentition (excluding the third molars) in non-syndromic dental patients or randomly selected subjects, and the factors affecting the observed rates. J Clin Pediatr Dent 2015; 39:199â??207.
- Shafi S, Alshehri E, Mir S. Prevalence of congenitally missing premolars in college of dentistry, King Khalid University, Abha, Kingdom of Saudi Arabia: Can early treatment make a difference?. Int J Sci Stud 2018; 6:4-7.
- Nieminen P. Genetic basis of tooth agenesis. J Exp Zool B Mol Dev Evol 2009; 312B:320â??342.
- Kist R, Watson M, Wang X, et al. Reduction of Pax9 gene dosage in an allelic series of mouse mutants causes hypodontia and oligodontia. Hum Mol Genet 2005; 14:3605â??17.
- Ranta R. Hypodontia and delayed development of the second premolars in cleft palate children. Eur J Orthod 1983; 5:145â??8.
- Massler M, Schour I, Fongheh H. Developmental pattern of the child as reflected in the calcification pattern of the teeth. Am J Dis Child 1941; 62:33-67.
- https://www.zvab.com/buch-suchen/titel/normale-histologie-entwicklungsgeschichte-z%E4hne-menschen/
- Ravn J, Nielsen H. A longitudinal radiographic study of the mineralization of 2nd premolars. Scand J Dent Res 1977; 85:232-6.
- Memmott J, Kuster C, Sullivan R. A very delayed developing premolar: Clinical report. AAPD 1985; 7:137-9.
- Bicakci A, Doruk C, Babacan H. Late development of a mandibular second premolar. Korean J Orthod 2012; 42:94-8.
- Ying C, Zhe Y, Bin X. Delayed development of maxillary second premolar: Case report and literature review. J Clin Pediatr Dent 2021; 45:63-5.
- Cunat J, Collord J. Late developing premolars: A report of two cases. JADA 1973; 87:18-85.
- Ranta R, Ylipaavalniemi P. Developmental course of supernumerary premolars in childhood: Report of two cases. J Dent Child 1981; 48:385-8.
- Coupland M. Apparent hypodontia. Br Dent J 1982; 152:388.
- Nolla C. The development of the permanent teeth. J Dent Child 1960; 27:254-66.
- Rølling S. Hypodontia of permanent teeth in Danish schoolchildren. Scand J Dent Res 1980; 88:365Â9.
- Moyers R. Handbook of orthodontics. 3rd Edn. Chicago: Year Book Medical Publishers 1972; 166Â476.
- Nielsen H, Ravn J. A radiographic study of mineralization of permanent teeth in a group of children aged 3Â7 years. Scand J Dent Res 1976; 84:109Â18.
- Fines C, Rebellato J, Saiar M. Congenitally missing mandibular second premolar: treatment outcome with orthodontic space closure. Am J Orth Dent Ortho 2003; 23:676â??82.
- Svedmyr B. Genealogy and consequences of congenitally missing second premolars. J Int Assoc Dent Child 1983; 14:77-82.
- Bergstrom K. An orthopantomographic study of hypodontia, supernumeraries and other anomalies in school children between the ages of 8-9 years. An epidemiological study. Swed Dent J 1977; 1:145-57.
- Lindqvist B. Extraction of deciduous second molar in hypodontia. Eur J Orthod 1980; 2:173-81.
- Vastardis H. The genetics of human tooth agenesis: New discoveries for understanding dental anomalies. Am J Orthod Dentofacial Orthop 2000; 117:650â??6.
- Nasman M, Forsberg CM, Dahllof G. Long-term dental development in children after treatment for malignant disease. Eur J Orthod 1997; 19:151â??9.
- Alexander-Abt J. Apparent hypodontia: A case of misdiagnosis. Am J Orthod Dentofacial Orthop 1999;116: 321-3.
- Vastardis H, Karimbux N, Guthua S, et al. A human MSX1 homeodomain missense mutation causes selective tooth agenesis. Nat Genet 1996; 13:417Â21.
- Stockton D, Das P, Goldenberg M, et al. Mutation of PAX9 is associated with oligodontia. Nat Genet 2000; 24:18Â9.
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Author Info
Department of Pediatric Dentistry and Orthodontics, College of Dentistry, King Saud University, Riyadh, Saudi ArabiaCitation: Zain Hafiz, Delayed Development of Mandibular Second Premolar: Review and 7 Years follow up Case Report, J Res Med Dent Sci, 2022, 10(1): 587-592
Received: 06-Dec-2021, Manuscript No. JRMDS-21-49193; , Pre QC No. JRMDS-21-49193 (PQ); Editor assigned: 08-Dec-2021, Pre QC No. JRMDS-21-49193 (PQ); Reviewed: 22-Dec-2021, QC No. JRMDS-21-49193; Revised: 27-Dec-2021, Manuscript No. JRMDS-21-49193 (R); Published: 03-Jan-2022
