Research - (2020) Advances in Dental Surgery
Effect of Stress on Periodontal Health: A Clinical Study
Vindhiya Varshini V and Arvina Rajasekar*
*Correspondence: Arvina Rajasekar, Department of Periodontics, Saveetha Dental College, Saveetha Institute of Medical and Technical Sciences, Saveetha University, Chennai, India, Email:
Abstract
Stress has become a part of one's life, which results in development of depression and anxiety. This psychological stress is generally thought to have a negative effect on periodontal health. The aim of this study was to determine the effect of stress on periodontal health among the dental students. A 10- item DAS (Depression, Anxiety and Stress) questionnaire designed to measure the severity of a range of symptoms common to DAS, a validated questionnaire was distributed among 100 undergraduate dental students of a private college. Followed by, periodontal parameters such as presence or absence of pocket depth of more than 3 mm and clinical attachment loss were assessed. The results obtained from the survey were tabulated, analysed and represented graphically using SPSS software (Version 23). Out of 100 students, 64% of them presented with pocket depth of more than 3mm and 63% of them presented with clinical attachment loss. The association between stress and periodontal parameters was found to be statistically significant. The present study suggests that dental students with extremely severe levels of depression, anxiety and stress presented with increased pocket depth and clinical attachment loss. Therefore, psychological factors have an adverse effect on periodontal health.
Keywords
Periodontal health, Stress, Anxiety, Periodontitis, Depression
Introduction
Stress is a reaction of a body to a deleterious nature they are found to distract normal physiological equilibrium. It results in development of depression and anxiety. Stress can be acute or chronic, it depends on the individual, Acute stress is the sudden and temporary response of the human body to a stressor which has a defined beginning and end. Exposure to the stress results in an aura response that is characterized by a “fight or flight” reaction. Chronic stress is the response to intermittent and repeated exposure to a stressor over a continuous period [1]. Repeated exposure to the chronic stress has biological cost and can lead to neurobiol immune dysfunction [2].
Periodontitis is a multifactorial disease [3].
It is usually characterised by the destructive inflammatory process that affects the tooth as well as the supporting hard and soft tissues, resulting in the tissue destruction. Periodontal diseases are due to many local or systemic risk factors, the dental plaque being the main causative factor and genetic polymorphisms, socio economic status, tobacco chewing, smoking habits being the threatening risk factors. Stress has shown stronger association with periodontitis [4]. A relationship was established between gingivitis and psychogenic factors such as stress, anxiety, and depression in the 1970s [5]. DeMarco used the term “periodontal emotional stress syndrome” to insist the impact of the stress suffered by the soldiers involved in the Vietnam War on the progression of periodontal disease in them [6].
Oral hygiene depends on the mental health of the patient [7]. It has been reported that psychological factors can lead patients to neglect their oral hygiene which results in a dental plaque build-up, that has a major effect on periodontal health [8]. Studies have shown that the stress generated by university studies results in a decrease in oral hygiene levels and an increase in crevicular interleukin-1β levels. Therefore, the earlier reports conclude that stress is a risk factor for gingival inflammation [9].
This psychological stress is generally thought to have a net-negative effect on the efficacy of the immune response, subsequently resulting in periodontal health breakdown. On the other hand, depression and anxiety are also the most common psychiatric conditions associated with periodontitis and have shown a biological plausibility in the literature.
Student’s life has many benefits, it also imposes stresses that are inevitable. Due to the various factors such as tight academic schedule, competition among the dental students. Who are designated as health professional students, suffer from the burden of achieving various targets amongst them which can lead to the development of psychological stress? This excessive stress in turn increases the prevalence of psychological factors such as depression, anxiety, and substance abuse and suicidal thoughts. Literature suggests that psychological stress has a detrimental effect on oral health [10]; hence, this study was undertaken to assess the effect of DAS over periodontal health indicators among the dental students. Negative life events manifested as psychological stress and depression are common in day-to-day life, emphasizing the relationship between the person and environment [11].
Previously we have worked on plenty of topics in periodontology [12-26]. Now we are planning to work on the effect of stress on periodontal health among the dental students.
Materials and Methods
A 10- item DAS (Depression, Anxiety and Stress) questionnaire designed based on a previous study [27] to measure the severity of a range of symptoms common to DAS, a validated questionnaire was distributed among 100 undergraduate dental students of a private college. The questionnaire was based on depression, anxiety and stress and all the questions had options 0,1,2 and 3 to be responded, later their scores were summed and assessed in which, score 1: Normal in DAS scale; score 2: Mild in DAS scale; score 3: Moderate in DAS scale; score 4: severe in DAS scale; score 5: extremely severe in DAS scale. Followed by, periodontal parameters such as presence or absence of pocket depth of more than 3 mm and clinical attachment loss were assessed. The results obtained from the survey were tabulated, analysed and represented graphically using SPSS software (Version 23). Then the Chi-square test was done to find out the association between the stress and periodontal parameters.
Results and Discussion
The present study was to assess the effect of stress on periodontal health among undergraduate dental students. Out of 100 students, 46% had a DAS score of 5, 24% had a DAS score of 4, 15% had a DAS score of 3, 10% had a score of 2 and 5% had a DAS score of 1 (Figure 1).
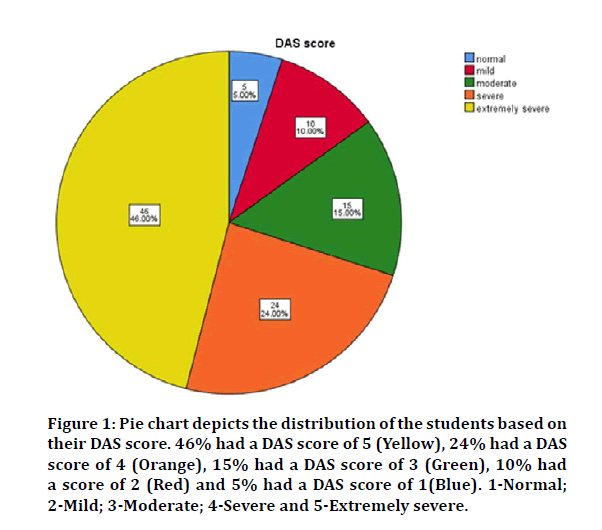
Figure 1: Pie chart depicts the distribution of the students based on their DAS score. 46% had a DAS score of 5 (Yellow), 24% had a DAS score of 4 (Orange), 15% had a DAS score of 3 (Green), 10% had a score of 2 (Red) and 5% had a DAS score of 1(Blue). 1-Normal; 2-Mild; 3-Moderate; 4-Severe and 5-Extremely severe.
Out of 100 students, 64% of them presented with pocket depth of more than 3 mm. 33% of students with DAS score of extremely severe presented with pocket depth of more than 3mm. Also, 17% of students under severe category, 10% of students under moderate category; 3% of students under mild category and 1% of students under normal category presented with pocket depth of more than 3 mm. The association between pocket depth and stress was assessed by Chi-square test and was found to be statistically significant with the p value of 0.027 (Figure 2).
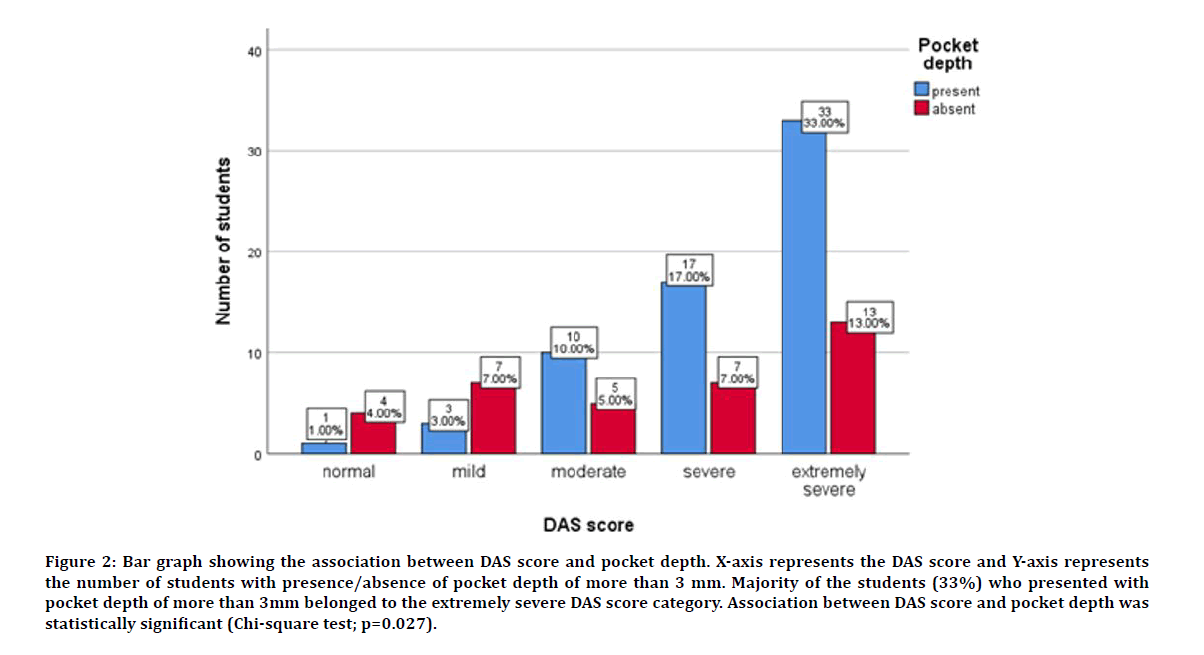
Figure 2: Bar graph showing the association between DAS score and pocket depth. X-axis represents the DAS score and Y-axis represents the number of students with presence/absence of pocket depth of more than 3 mm. Majority of the students (33%) who presented with pocket depth of more than 3mm belonged to the extremely severe DAS score category. Association between DAS score and pocket depth was statistically significant (Chi-square test; p=0.027).
Out of 100 students, 63% of them presented with clinical attachment loss. 39% of students with a DAS score of extremely severe presented with clinical attachment loss. Also, 13% of students under severe category, 10% of students under moderate category; 5% of students under mild category and 1% of students under normal category presented with clinical attachment loss. The association between clinical attachment loss and stress was assessed by Chi-square test and was found to be statistically significant with the p value of 0.00 (Figure 3).
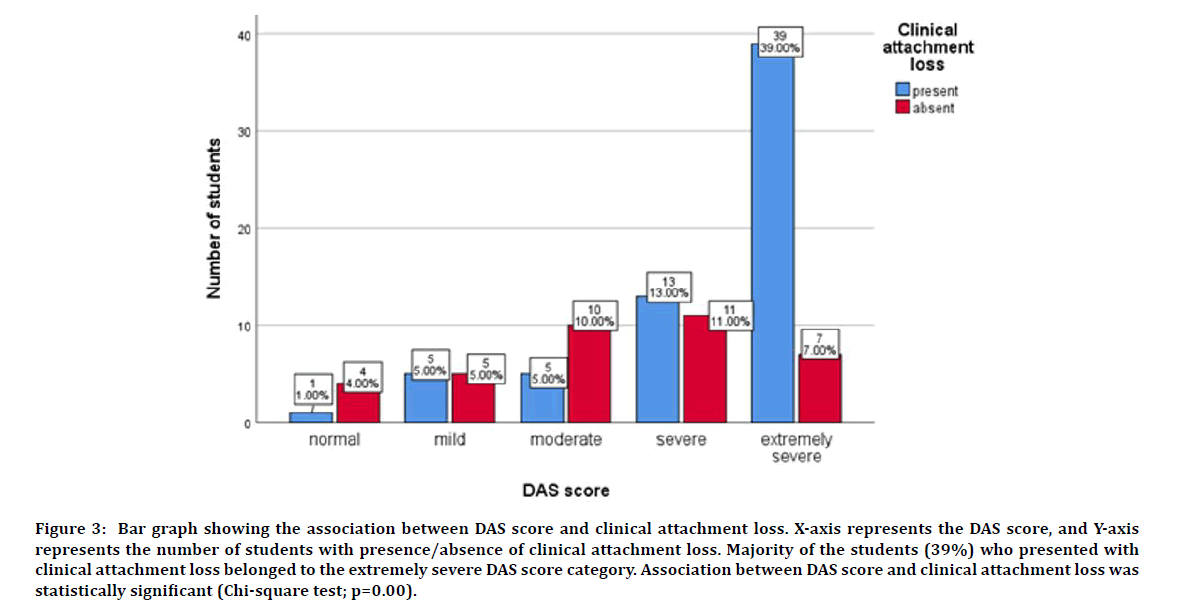
Figure 3: Bar graph showing the association between DAS score and clinical attachment loss. X-axis represents the DAS score, and Y-axis represents the number of students with presence/absence of clinical attachment loss. Majority of the students (39%) who presented with clinical attachment loss belonged to the extremely severe DAS score category. Association between DAS score and clinical attachment loss was statistically significant (Chi-square test; p=0.00).
Oral health can reflect the overall health status of a personnel. Periodontal disease Gingivitis and periodontitis, tooth caries are the most common oral ailments. Periodontitis, which is a multifactorial disease, can have various risk factors such as age, diabetes, genetics, and psychological stress. On the other hand, stress has shown a stronger association to periodontal disease which stands proven in the literature [10].
Stress experienced in day-to-day life depends on an individual's personal life. Similarly, there is a variation in stress between professionals and nonprofessionals, where in professionals have shown higher levels of stress when compared to nonprofessionals [28]. Among the various professionals, health professionals are majorly subjected to stress. Being the forerunners for the health-care system, they are subjected to greater stress-related responsibilities [29]. Hence, this study was taken up to assess the effect of DAS over periodontal health indicators among dental students.
Dental students are exposed to significant stressors. Education in the medical field intends an intensive and competitive preparation of graduates in an attempt to achieve a personally rewarding and socially meaningful career, and hence, various medical programs may have physical and psychological effects on the wellbeing of medical students. Studies has also showed that medical students experience high levels of stress during their undergraduate training [27]. In the current study, dental students have depicted higher stress which in turn increases the periodontal health issues [30].
On the other hand, the academic and professional outcomes are attributed to poor academics and professional dissatisfaction and leads to stress attributed to the stress. On the other hand, dentistry being an art and science in and due to the demanding nature of the training itself evidenced from the research, it was shown that dental students experience considerable amount of stress during training. However, the research confirms that the main effects of stress are attributed to low academic performance and psycho emotional well-being. The fear of poor performance in academics has been the main stressor across the 5-year study period to be the underlying cause of the stress among dental students. Stress experienced by students was the significant workload, and these findings of our study are in coincidence with the study conducted to compare stress levels among medical and paramedical students [31]. However, in contradiction to our findings, there are reports suggesting lower stress levels in dental students than that of medical and Nursing students [32].
Previous studies have shown that academic stress among students can cause gingival inflammation and diminution of the quality of oral hygiene [33]. Apparently, that stress can negatively influence the oral health status [8,34,35]. Participants who are highly susceptible to depression had shown higher values of PD and CAL. This correlation may be due to the negligence of oral hygiene practice under stressful conditions and thereby resulting in increased susceptibility to periodontal disease. These findings are in accordance with the present study.
Conclusion
The present study suggests that dental students with extremely severe levels of depression, anxiety and stress presented with increased pocket depth and clinical attachment loss. Therefore, psychological factors have an adverse effect on periodontal health. Hence, more awareness programs should be conducted among the students to educate about the role of stress on periodontal diseases.
Acknowledgement
The authors of this study would like to express their gratitude towards everyone who facilitated and enabled us to carry out this study successfully.
Conflict of Interests
None declared.
References
- Juster RP, McEwen BS, Lupien SJ. Allostatic load biomarkers of chronic stress and impact on health and cognition. Neurosci Biobehavioral Rev 2010; 35:2–16.
- Gunepin M, Derache F, Trousselard M, et al. Impact of chronic stress on periodontal health. J Oral Med Oral Surg 2018; 24:44–50.
- Genco RJ. Current view of risk factors for periodontal diseases. J Periodont 1996 ;67:1041–1049.
- Elter JR, Beck JD, Slade GD, et al. Etiologic models for incident periodontal attachment loss in older adults. J Clin Periodontol 1999; 26:113–123.
- Formicola AJ, Thompson Witte E, Curran PM. A study of personality traits and acute necrotizing ulcerative gingivitis. J Periodont 1970; 41:36–38.
- Marco TJD, De Marco TJ. Periodontal emotional stress syndrome. J Periodont 1976; 47:67–68.
- Goyal S, Gupta G, Thomas B, et al. Stress and periodontal disease: The link and logic. Industrial Psyc J 2013; 22:4.
- Deinzer R, Granrath N, Spahl M, et al. Stress, oral health behaviour and clinical outcome. Br J Health Psychol 2005; 10:269–283.
- Johannsen A, Bjurshammar N, Gustafsson A. The influence of academic stress on gingival inflammation. Int J Dent Hyg 2010; 8:22–27.
- Biondi M, Zannino LG. Psychological stress, neuroimmunomodulation, and susceptibility to infectious diseases in animals and man: A review. Psych Psychosomatics 1997; 66:3–26.
- Lazarus RS. Toward better research on stress and coping. American Psychologist 2000; 55:665–673.
- Christabel SL, Linda Christabel S. Prevalence of type of frenal attachment and morphology of frenum in children, Chennai, Tamil Nadu. World J Dent 2015; 6:203–207.
- Ramakrishnan M, Bhurki M. Fluoride, Fluoridated toothpaste efficacy and its safety in children-Review. Int J Pharm Res 2018;10:109-114.
- Govindaraju L. Clinical evaluation of quality of obturation and instrumentation time using two modified rotary file systems with manual instrumentation in primary teeth. J Clin Diagnostic Res 2017; 11:ZC55.
- Govindaraju L, Jeevanandan G, Subramanian EMG. Comparison of quality of obturation and instrumentation time using hand files and two rotary file systems in primary molars: A single-blinded randomized controlled trial. Eur J Dent 2017; 11:376–379.
- Govindaraju L, Jeevanandan G, Subramanian EMG. Knowledge and practice of rotary instrumentation in primary teeth among indian dentists: A questionnaire survey. J Int Oral Health 2017; 9:45.
- Govindaraju L, Gurunathan D. Effectiveness of chewable toothbrush in children-A prospective clinical study. J Clin Diagn Res 2017; 11:ZC31–34.
- Gurunathan D, Shanmugaavel AK. Dental neglect among children in Chennai. J Indian Soc Pedod Prev Dent 2016; 34:364–369.
- Jeevanandan G. Kedo S. Paediatric rotary files for root canal preparation in primary teeth-Case report. J Clin Diagn Res 2017; 11:ZR03–ZR05.
- Jeevanandan G, Govindaraju L. Clinical comparison of Kedo-S paediatric rotary files vs manual instrumentation for root canal preparation in primary molars: A double blinded randomised clinical trial. Eur Archives Paediatr Dent 2018; 19:273–278.
- Nair M, Jeevanandan G, Vignesh R, et al. Comparative evaluation of post-operative pain after pulpectomy with k-files, kedo-s files and mtwo files in deciduous molars-A randomized clinical trial. Br Dent Sci 2018; 21:411.
- Packiri S, Gurunathan D, Selvarasu K. Management of paediatric oral ranula: A systematic review. J Clin Diagn Res 2017; 11:ZE06–ZE09.
- Panchal V, Jeevanandan G, Subramanian EMG. Comparison of instrumentation time and obturation quality between hand K-file, H-files, and rotary Kedo-S in root canal treatment of primary teeth: A randomized controlled trial. J Indian Society Pedodont Preventive Dent 2019; 37:75.
- Ravikumar D, Jeevanandan G, Subramanian EMG. Evaluation of knowledge among general dentists in treatment of traumatic injuries in primary teeth: A cross-sectional questionnaire study. Eur J Dent 2017; 11:232–237.
- Somasundaram S. Fluoride content of bottled drinking water in Chennai, Tamilnadu. J Clin Diagnostic Res 2015; 9:ZC32.
- Subramanyam D, Gurunathan D, Gaayathri R, et al. Comparative evaluation of salivary malondialdehyde levels as a marker of lipid peroxidation in early childhood caries. Eur J Dent 2018; 12:67–70.
- Penmetsa G, Seethalakshmi P. Effect of stress, depression, and anxiety over periodontal health indicators among health professional students. J Indian Assoc Public Health Dent 2019; 17:36.
- Prakash J, Singh S, Das RC, et al. A cross-sectional assessment of stress, coping, and burnout in the final-year medical undergraduate students. Industrial Psychiatry J 2016; 25:179.
- Dutta AP, Pyles MA, Miederhoff PA. Stress in health professions students: myth or reality? A review of the existing literature. J Natl Black Nurses Assoc 2005; 16:63–68.
- Borjalilu S, Mohammadi A, Mojtahedzadeh R. Sources and severity of perceived stress among iranian medical students. Iranian Red Crescent Med J 2015; 17.
- Henning K, Ey S, Shaw D. Perfectionism, the imposter phenomenon and psychological adjustment in medical, dental, nursing and pharmacy students. Med Educ 1998; 32:456–464.
- Mane Abhay B, Krishnakumar M, Niranjan Paul C, et al. Differences in perceived stress and its correlates among students in professional courses. J Clin Diagn Res 2011; 5:1228–1233.
- Murphy RJ, Gray SA, Sterling G, et al. A comparative study of professional student stress. J Dent Educ 2009; 73:328–337.
- Deinzer R, Kottmann W, Förster P, et al. After-effects of stress on crevicular interleukin-1beta. J Clin Periodontol 2000; 27:74–77.
- Deinzer R, Rüttermann S, Möbes O, et al. Increase in gingival inflammation under academic stress. J Clin Periodontol 1998; 25:431–433.
Author Info
Vindhiya Varshini V and Arvina Rajasekar*
Department of Periodontics, Saveetha Dental College, Saveetha Institute of Medical and Technical Sciences, Saveetha University, Chennai, IndiaCitation: Vindhiya Varshini V, Arvina Rajasekar, Effect of Stress on Periodontal Health: A Clinical Study, J Res Med Dent Sci, 2020, 8 (7): 259-263.
Received: 16-Sep-2020 Accepted: 02-Nov-2020 Published: 09-Nov-2020
