Research - (2020) Advances in Dental Surgery
Financial Status of People who Undergo Dental Treatment
Bipin, Dhanraj Ganapathy* and Keerthi Sasanka L
*Correspondence: Dhanraj Ganapathy, Department of Prosthodontics, Saveetha Dental College, Saveetha Institute of Medical and Technical Sciences, Saveetha University, Chennai, India, Email:
Abstract
Dental caries is one of the major oral health issues in most of the developing countries. If these caries aren’t diagnosed and treated in early stages, it will lead to potential threats where some of the population were not able to afford the treatment. So early dental treatment would prevent severe destruction of oral health and also avoids expenses to proceed the dental treatment. This study was a questionnaire-based study done on the adult population with ethical permissions from the institutional research board. The questionnaire had 15 questions related to the attitude and knowledge about affordable financial status by every patient undergoing dental treatment. The questionnaire was put up in the Survey Planet - An online based Survey platform and responses were collected. 94.6% of the people in rural areas lag awareness about dental treatment and this seems to be a shocking result as we are in the most advanced world. 53.8% of the study population still feel that they are not satisfied with the treatment given for what they pay. The purpose of the study was to know about the awareness and attitude about financial status of people undergoing dental treatment and check whether they were able to spend the required cost for the treatments. Nowadays even the technology is getting advanced, the people are still unable to afford dental treatment. Better awareness should be created among the people so that even the economically weaker section can also afford dental treatment.
Keywords
Dental awareness, Dental attitude, Dental procedures, Socioeconomic status, Income, Education level, oral health, Inequalities
Introduction
Dental caries is one of the major oral health issues in most of the developing countries. If these caries are not diagnosed and treated in early stages, it will lead to potential threats where some of the population is not able to afford the treatment. So early dental treatment would prevent severe destruction of oral health and avoids expenses to proceed the dental treatment. Many studies show that even developed countries are deficient in giving treatments to people visiting clinics [1– 3]. Inequalities in Socioeconomic status underlie many health disparities in the world, including oral health. Even children in today’s world face the same issue. As the Parents income plays an important role in affording dental treatment for their children. Many Parents are not aware of the dental caries and its effects [4,5]. Public health is now recognized as being a core component of the undergraduate medical and dental curriculum. We should expand the focus and understanding of the dental profession. As people assume that the cost of treatment is very high, they are scared to even afford basic treatment like Scaling. There should be proper planning and management of health services so, that people get clarity for what they pay [1,6]. These socioeconomic inequalities in Oral health is a major challenge today for health policy it includes not only inequalities which is considered to be unfair but also reducing the burden of oral health problems in groups which offer great potential for improving the average oral health status of the population [7,8]. The socioeconomic status refers to differences in the prevalence or incidence of oral health problems between individuals of lower- and higher-class people [9]. Some studies also prove that financial status of the people is decreasing gradually, and this seems to be the major drawback in affording even general treatments [10]. The most important factors of Socioeconomic status include income, occupational status, and level of education [11]. Even Some of the recent surveys show that non fluoridated urban areas communities experience tooth decay in higher level [12–14]. Even in the Schools, Students should be taught of oral health. High level of education on oral health is very much essential to understand the oral health behaviour Some treatments like implants, periodontal surgery, Cosmetic dental procedures require high financial background Affluent person receive more treatment as they are financially well settled [10]. Oral health care often involves patients making direct payments for their care and treatment. Some of the studies showed many parameters that includes Human Development Index (HDI), the Urban Population Growth (UPG), Infant Mortality Rate (IMR), Mean Years of Schooling (MYS), Under-Five Mortality Rate (UMR), Gross National Product per Capita (GNP) and the GINI Index (GI). Based on these parameters Socio economic status was calculated to check whether the dental treatment and medical treatment is affordable by all categories of people undergoing treatment [12]. Early detection of the diseases and diagnosing it with proper treatment would reduce the cost of treatment and the risk of dental problems. Previously our department has published extensive research on various aspects of prosthetic dentistry [15–24], this vast research experience has inspired us to research about the awareness on use of steroid drugs among football players. The aim of the study is to evaluate the financial status of patients undergoing dental treatment.
Materials and Methods
The study was done on the random population. The study population included people with different age groups. As this study mainly focuses on the Socio-economic status, the questionnaire was prepared based on the topic. 15 questions were created under the questionnaire and it was circulated through Survey planet. The subjects were requested to respond to each item in the specific format given at the end of each item. All the participants could choose one of the given three to four choices for each item in the questionnaire. the descriptive statistics was obtained. Finally, the responses were collected, and it was estimated to be 100.
Questionnaire
Do you think people in rural areas lag awareness on dental health? Yes/No
Do you think patients are satisfied with the dental treatments given for what they pay? Yes/ No
If a patient undergoes dental treatment, do you think a patient must be prepared mentally and physically? Yes/No
Have you ever come across the word ‘dental insurance’? Yes/ No
Have you ever noticed the people of NRI bear the pain, wait for a period to undergo dental treatment in India? Yes/No
Is India one of the Cheapest places for undergoing dental treatment? Yes/ No
Should we need to trust a dentist who charges less than who charges more for general dental treatment? Yes/No
Dentistry overseas is more expensive’ Do you think many dentists abroad still pay student loans even after qualifying? Yes/No
Do you think dental insurance has more beneficial effects? Yes/No
Do you think schemes for dental insurance are made available everywhere throughout the country? Yes/No
Observation
Do you think people in rural areas lag awareness on dental health?
Yes-91.9%
No-8.1%
Do you think patients are satisfied with the dental treatments given for what they pay?
Yes-48%
No-12%
If a patient undergoes dental treatment, Do you think a patient must be prepared mentally and physically?
Yes-69.3%
No-30.7%
Have you ever come across the word ‘dental insurance’?
Yes-50.5%
No-49.5%
Have you ever noticed the people of NRI bear the pain, wait for a period of time to undergo dental treatment in India?
Yes-58.6%
No-41.4%
Is India one of the Cheapest places for undergoing dental treatment?
Yes-58%
No-42%
Should we need to trust a dentist who charges less than who charges more for general dental treatment?
Yes-63.9%
No-36.1%
Dentistry overseas is more expensive’ Do you think many dentists abroad still pay student loans even after qualifying?
Yes-70.4%
No-29.6%
Do you think dental insurance has more beneficial effects?
Yes-56.6%
No-43.4%
Do you think schemes for dental insurance are made available everywhere throughout the country?
Yes-59.6%
No-40.4%
Results and Discussion
As the Survey results show that most of the population lag awareness on dental health. Survey results clearly showed that 91.9% of the people residing in rural areas lag awareness on dental health. 52% of the patients were not satisfied with the dental treatments given for what they pay. 69.37% of the study population feel that a person should be mentally and physically prepared before undergoing treatment. More than half of the study population were not sure about dental insurance. Some of the developed countries like the United States and United Kingdom have the Special scheme for dental insurance. Many Non-Resident Indians afford dental treatment only during the visit to the native place. As, even they feel that the cost of dental treatment is very much affordable in developing countries like India. 58.6% of the study population felt that most of the nonresident Indians wait for a period to undergo dental treatment in India. 58% of them felt India is one of the cheapest places for affording dental treatment. 63.9% felt that they trust a dentist who charges less than who charges more for general and dental treatment. 70.4% of the study felt that dentistry overseas is more expensive. Even many dentists residing abroad still pays student longs even after qualifying. 56.4% of the study population thought dental insurance was more beneficial for them. 59.6% of the study population even felt that schemes like dental insurance are made available everywhere throughout the country. Some patients have poor attitudes on the part of the physician, during the treatment or during interactions with patients. Some studies even show that low economic status would really affect the dental treatment taken by the patients. Patients would have negative attitude on the undergoing dental treatment due to their personal socio-economic issues (Figures 1-10).
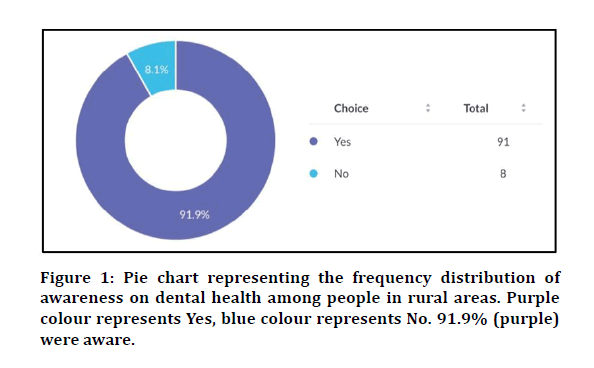
Figure 1: Pie chart representing the frequency distribution of awareness on dental health among people in rural areas. Purple colour represents Yes, blue colour represents No. 91.9% (purple) were aware.
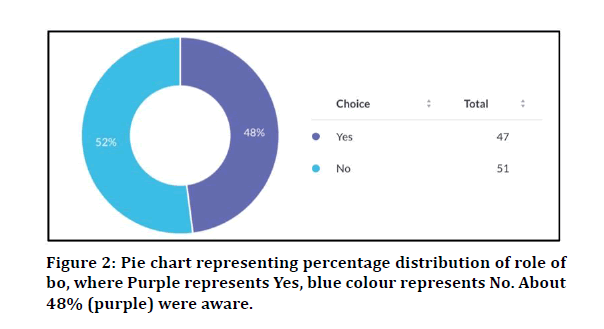
Figure 2: Pie chart representing percentage distribution of role of bo, where Purple represents Yes, blue colour represents No. About 48% (purple) were aware.
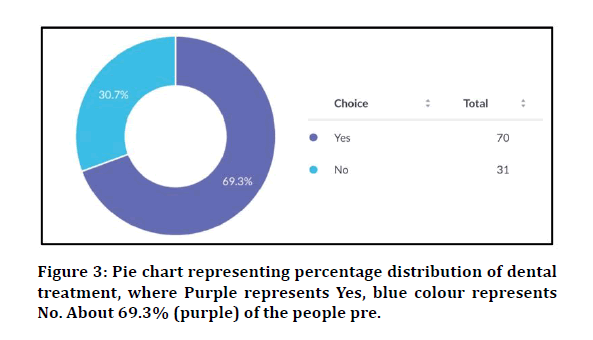
Figure 3: Pie chart representing percentage distribution of dental treatment, where Purple represents Yes, blue colour represents No. About 69.3% (purple) of the people pre.
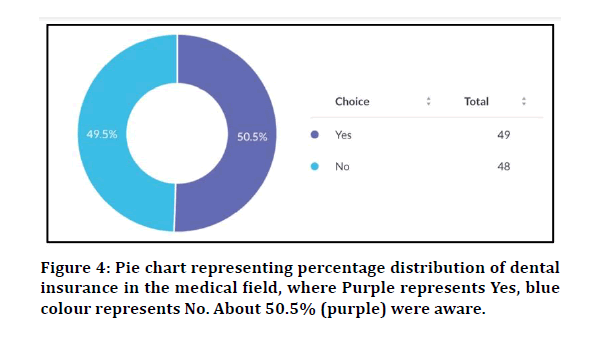
Figure 4: Pie chart representing percentage distribution of dental insurance in the medical field, where Purple represents Yes, blue colour represents No. About 50.5% (purple) were aware.
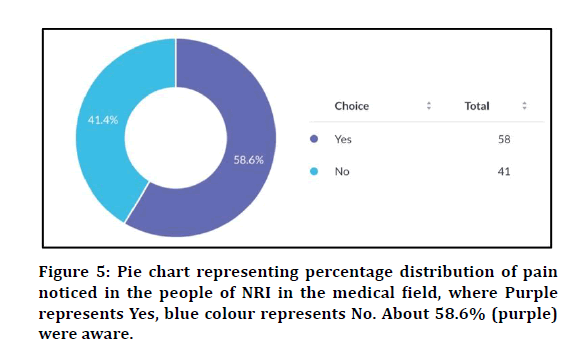
Figure 5: Pie chart representing percentage distribution of pain noticed in the people of NRI in the medical field, where Purple represents Yes, blue colour represents No. About 58.6% (purple) were aware.
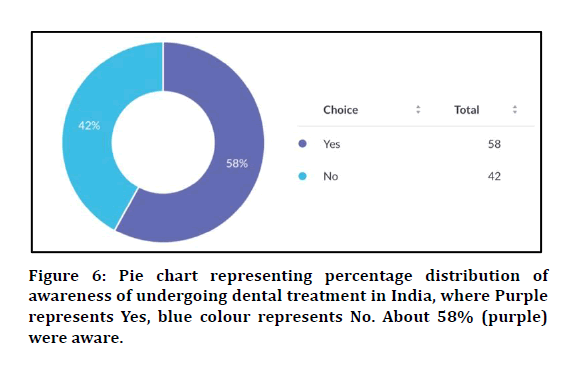
Figure 6: Pie chart representing percentage distribution of awareness of undergoing dental treatment in India, where Purple represents Yes, blue colour represents No. About 58% (purple) were aware.
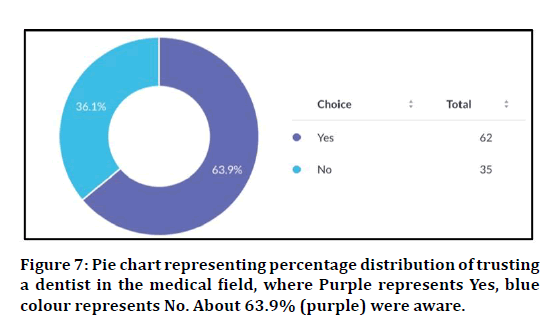
Figure 7: Pie chart representing percentage distribution of trusting a dentist in the medical field, where Purple represents Yes, blue colour represents No. About 63.9% (purple) were aware.
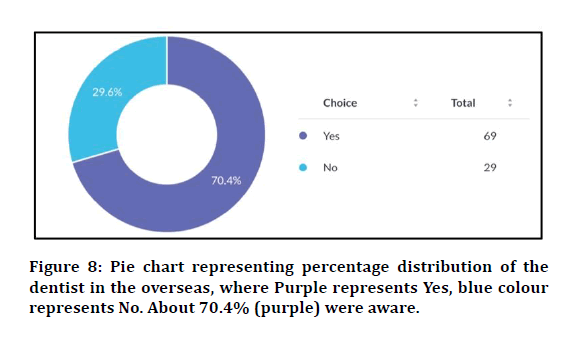
Figure 8: Pie chart representing percentage distribution of the dentist in the overseas, where Purple represents Yes, blue colour represents No. About 70.4% (purple) were aware.
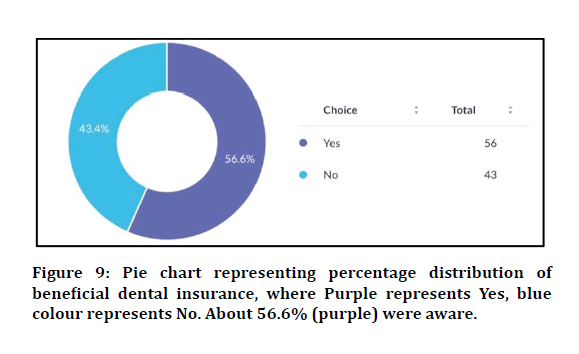
Figure 9: Pie chart representing percentage distribution of beneficial dental insurance, where Purple represents Yes, blue colour represents No. About 56.6% (purple) were aware.
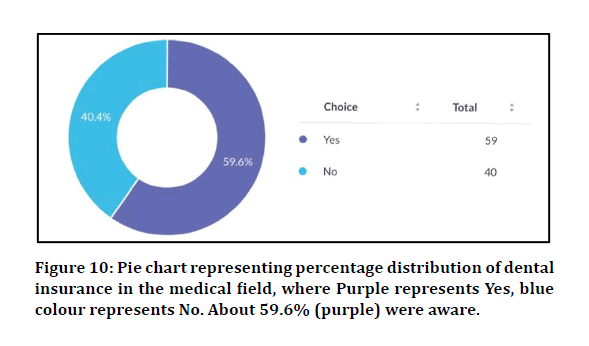
Figure 10: Pie chart representing percentage distribution of dental insurance in the medical field, where Purple represents Yes, blue colour represents No. About 59.6% (purple) were aware.
Conclusion
This study concludes, most of the people these days are aware of the basic oral hygiene techniques, they show a responsible attitude towards these procedures. But certain people do not have basic knowledge about dental hygiene and itstechniques, and they have a lethargic attitude to maintain oral health.
Acknowledgement
With Sincere gratitude, we acknowledge the staff members of the department of conservative dentistry and Endodontics and Saveetha dental college and study participants for their extended support towards the completion of research.
Conflict of Interest
Conflict of interest declared as none.
References
- Grinin VM, Kabak DS, Vagner VD, et al. Assessment of dental status of patients undergoing treatment in a multidisciplinary hospital. Clin Dent 2019; 3:83–85.
- http://www.isrctn.com/
- Aluckal E. P3.57 Knowledge and attitude of dental students towards the dental treatment of patients with hiv/aids in mangalore city. Epidemiology, Monitoring Evaluation 2017; 93:A113.
- Mendoza-Mendoza A, Perea MB, Yañez-Vico RM, et al. Dental fear in children: The role of previous negative dental experiences. Clin Oral Investigations 2015; 19:745–751.
- Gallagher PJ, Gallagher J. Summary of factors influencing patients’ continuing attendance at a given dentist. Br Dent J 2018; 218:348–349.
- Neves ÉTB, Lima LCM de, Dutra L da C, et al. Oral health literacy, sociodemographic, family, and clinical predictors of dental visits among Brazilian early adolescents. Int J Paediatr Dent 2020; 15.
- Kennedy BP, Kawachi I, Glass R, et al. Income distribution, socioeconomic status, and self-rated health in the United States: Multilevel analysis. BMJ 1998; 317:917–921.
- Milyo J, Kennedy BP, Kawachi I, et al. Income distribution, socioeconomic status, and self-rated health in US. BMJ 1999; 318:1417–1417.
- Shin BM, Jung SH, Kim MH, et al. Did the extended coverage policy contribute to alleviating socioeconomic inequality in untreated dental caries of both children and adolescents in South Korea? BMC Oral Health 2020; 20:1-10.
- Kim JA, Choi HM, Seo Y, et al. Relations among obesity, family socioeconomic status, oral health behaviors, and dental caries in adolescents: the 2010–2012 Korea National Health and nutrition examination survey. BMC Oral Health 2018; 18:114.
- Skeie MS, Klock KS. Dental caries prevention strategies among children and adolescents with immigrant-or low socioeconomic backgrounds- do they work? A systematic review. BMC Oral Health. 2018; 18:20.
- Hobdell MH, Oliveira ER, Bautista R, et al. Oral diseases and socio-economic status (SES). Br Dent J 2003; 194:91–96.
- Lalloo R, Myburgh NG, Hobdell MH. Dental caries, socio-economic development, and national oral health policies. Int Dent J 1999; 49:196–202.
- Hobdell MH. Economic globalization and oral health. Oral Diseases. 2001; 7:137–143.
- Ariga P, Nallaswamy D, Jain AR, et al. Determination of correlation of width of maxillary anterior teeth using extraoral and intraoral factors in Indian population: A systematic review. J Dent 2018; 9:68–75.
- Jyothi S, Robin PK, Ganapathy D, et al. Periodontal health status of three different groups wearing temporary partial denture. Res J Pahram Technol 2017; 10:4339.
- Duraisamy R, Krishnan CS, Ramasubramanian H, et al. Compatibility of nonoriginal abutments with implants: Evaluation of microgap at the implant-abutment interface, with original and nonoriginal abutments. Implant Dent 2019; 28:289–295.
- Selvan SR, Ganapathy D. Efficacy of fifth generation cephalosporins against methicillin-resistant Staphylococcus aureus-A review. RES J Pharma Technol 2016; 9:1815.
- Ganapathy D, Sathyamoorthy A, Ranganathan H, et al. Effect of resin bonded luting agents influencing marginal discrepancy in all ceramic complete veneer crowns. J Clin Diagn Res 2016; 10:ZC67–ZC70.
- Subasree S, Murthykumar K, Dhanraj G. Effect of aloe vera in oral health-A review. Res J Pharma Technol 2016; 9:609.
- Jain A, Ranganathan H, Ganapathy D. Cervical and incisal marginal discrepancy in ceramic laminate veneering materials: A SEM analysis. Contemporary Clin Dent 2017; 8:272.
- Vijayalakshmi B, Ganapathy D. Medical management of cellulitis. Res J Pharma Technol 2016; 9:2067.
- Ganapathy DM, Kannan A, Venugopalan S. Effect of coated surfaces influencing screw loosening in implants: A systematic review and meta-analysis. World J Dent 2017; 8:496–502.
- Ashok V, Suvitha S. Awareness of all ceramic restoration in rural population. Res J Pharma Technol 2016; 9:1691.
Author Info
Bipin, Dhanraj Ganapathy* and Keerthi Sasanka L
Department of Prosthodontics, Saveetha Dental College, Saveetha Institute of Medical and Technical Sciences, Saveetha University, Chennai, IndiaCitation: Bipin, Dhanraj Ganapathy, Keerthi Sasanka L,Financial Status of People who Undergo Dental Treatment, J Res Med Dent Sci, 2020, 8 (7): 117-121.
Received: 15-Sep-2020 Accepted: 16-Oct-2020 Published: 23-Oct-2020
