Research - (2022) Volume 10, Issue 1
Incidence, Predictability and Causes of Tubal Rupture IN Ectopic Pregnancy in a Pakistani Population: A Descriptive Cross-Sectional Study
Meena Bai1, Ome Kulsoom2*, Azra3, Bushra4, Jabeen Atta5 and Shumaila Javaid6
*Correspondence: Ome Kulsoom, Department of Gynaecology and Obstetrics, Ziauddin University Hospital Karachi, Pakistan, Email:
Abstract
Background: Despite the advances in medical and healthcare sector, ectopic pregnancy remains a prime cause of maternal disability, death, fetal demise and devastating fate of pregnant women especially in the developing world. The usual extra uterine location of ectopic implantation is the fallopian tube, causing 96 percent of all ectopic gestations. The objective of this study is to determine the incidence, predictability and causes of tubal rupture in ectopic pregnancy in patients residing in Pakistan. Material and Methods: A descriptive cross sectional study involving patients of tubal rupture in ectopic pregnancy among all indoor patients visiting Gynaecology and Obstetrics department of Civil Hospital Dow University of Health Sciences Karachi Pakistan from 1 Jan 2020 to 31 Dec 2020. Data was collected pertaining to patients’ age, parity, gestational age, past medical history and duration of symptoms. Microsoft Excel and SPSS 22 were used for data analysis. Results: 73 diagnosed cases of ectopic pregnancy among 6346 pregnant patients reported in the year 2019. The incidence of tubal rupture was 87.67% (64/73). Tubal rupture was more prevalent in patients of age ≤ 24 years and with low parity. In this age group with null parity, the incidence of ruptured ectopic pregnancy was up to 100%. The incidence of tubal rupture was found to be inversely proportional to maternal age and parity, decreasing to 75% with parity of four. In addition, it was found that increase in gestational age from 7 weeks to 11 weeks increased the incidence of tubal rupture from 84.48% to 100% respectively. Seeking earlier medical care was associated with lesser events of tubal rupture in comparison with late report to a hospital after 4 days which elevates the incidence to 100%. Conclusion: The significantly higher incidence of tubal rupture in ectopic pregnancy in Pakistan is a major cause of maternal mortality, morbidity and reduced childbearing potential among women of reproductive age. Prompt identification of high risk groups with predictable signs and precise assessment of variable presentation can prove crucial in decreasing maternal mortality. Mass awareness in women of reproductive age to seek early medical care and precise management in high risk groups is the need of the hour.
Keywords
Ectopic pregnancy, Tubal rupture, Maternal mortality, Parity, Medical care
Introduction
Ectopic pregnancy (EP) is a medical disorder of huge clinical significance, especially in the third world countries, due to the higher disability and deaths related with it. EP is a gestational disorder where the blastocyst gets embedded at a location other than the endometrium of the uterus. The usual extra-uterine area is the fallopian tube, which represents 96 percent of EP [1]. It is a site that commonly isn't prepared structurally and functionally to accommodate the origination or to allow the development of fetal tissue [2]. Patients with tubal gestation are at danger of rupture. In a foreign study, occurrence of tubal rupture was discovered to be 29.5% [3]. “It is the leading cause of maternal mortality in the first trimester and accounts for 10%–15% of all maternal deaths” [4]. Occurrence of ectopic pregnancy rises with female genital infections, period of origination, long term intrauterine contraceptive device, pelvic inflammatory disease, polygamy, history of pelvic surgical procedure and abortions.
Around 1 in each 50 pregnancies in the United States is an ectopic pregnancy, which can't bring about a child [5] while in Pakistan the revealed occurrence of ectopic pregnancy has been referred to as 1:112 to 1:1308 yet the genuine figures could be a lot higher due to under finding and poor measurable records [6]. Ectopic pregnancies could be asymptomatic. The manifestations of a ruptured ectopic pregnancy could be acute or subacute [7]. In intense conditions the patient presents with severe acute abdominal discomfort, shock and have evident indications of hemoperitoneum. In sub-acute cases, female patients reports with pain in abdominal region, amenorrhea and bleed per vagina. Very rarely an ectopic pregnancy persists longer, a chronic presentation is often a mystery and an incidental finding usually on exploratory laparotomy or laparoscopy done for other causes. The scope of clinical signs in ectopic pregnancy ranges from a totally asymptomatic status to peritoneal discomfort because of haemorrhage to the coelomic cavity or even hypovolemic shock. Early detection of ectopic pregnancy before rupture of fallopian tube is essential in forestalling maternal mortality and dismalness.
The diagnosis of ectopic pregnancy is made with a mix approach of clinical assessment, βhCG, Serum progesterone, ultrasonography and laparoscopy. Transvaginal ultrasound imaging is crucial in confirming presumed ectopic pregnancy. Sequential tests with transvaginal imaging, serum HCG levels, or both are important to affirm the analysis [8]. The best symptomatic affirmation of an ectopic pregnancy comes through distinguishing a fetal heartbeat outside the uterine cavity on ultrasonography. The nonappearance of a discernible fetal heartbeat can be deceiving however as a fetal heartbeat does not occur all through every single ectopic pregnancy [8]. Extra indications of ectopic pregnancy include recognizable proof of a gestational sac with or without a yolk sac inside an ectopic area or noticing a complex adnexal mass that strays from the common occurrence of haemorrhagic corpus luteum [8]. When radiologic imaging cannot affirm the presence of an ectopic pregnancy, direct viewing of the dubious mass can happen through laparoscopy or laparotomy.
The advancement in medical field has led to effective medical management of ectopic pregnancy with minimal chances of residual morbidity. Patients presenting at an earlier stages of ectopic gestation can have a maximal benefit of medical management. Most of the patients presenting at a later gestational age necessitates a surgical procedure and risk of residual morbidity increases. Development of medical facilities dedicated for early ectopic pregnancy detection can help in prompt finding of complication diminishing debility and preservation of fertility.
The goal of this research study is determination of the occurrence of rupture of fallopian tube related with ectopic pregnancy in Pakistani population as it might be diverse in our population when contrasted with worldwide information. The subsequent target is to find out any relationship of ruptured pregnancy with order of parity and gestational age.
Material and Methods
This descriptive cross-sectional study was carried out in the Department of Gynaecology and Obstetrics, Civil Hospital Dow University of Health Sciences Karachi Pakistan from 1 Jan 2020 to 31 Dec 2020. Over a year time, 73 patients of ectopic pregnancy were enlisted by consecutive non-probability sampling. With the international prevalence of 29.5% tubal rupture in EP, a confidence interval of 95% and absolute precision of 10% was estimated for the study and the sample size of 73 was calculated.
Patients reported to hospital through A & E and outpatient departments. After getting consent for use of medical data for our study, the patients meeting the inclusion criteria of ectopic pregnancy were enlisted. Pregnant patients with different reasons for intense abdominal discomfort including acute appendicitis, diverticulitis, acute cholecystitis, acute pancreatitis and peritonitis were not included. Clinical diagnosis was made based on symptomatology. Ultrasonography was utilized as the demonstrative methodology in dubious instances of ectopic pregnancy. Ultrasounds of patients were performed and assessed by senior radiologists. The information relating to patients' age, time since onset of symptoms, previous pregnancies, age of present gestation and past clinical history was recorded on a predesigned proforma.
This information was maintained and analyzed in Microsoft Excel and SPSS-22. Rate of occurrence and percentages were determined for categorical factors like tubal break. Mean standard deviation was determined for continuous variables.
Results
This study was undertaken to assess the occurrence of rupture of fallopian tube in ectopic pregnancy, predictability and reasons for fallopian tube rupture in EP. Out of 6346 patients, 73 (1.15%) reported to hospital with signs suspicious of ectopic pregnancy and were to a great extent analyzed clinically, though an ultrasound was performed in dubious instances.
The average age of patients was 24.37 ± 4.68 years with a difference from 17 to 35 years. Average gestational age at reporting time to a healthcare facility was 8.21 ± 2.17 weeks. Least gestational age was 7 weeks while most extreme gestational age was 11 weeks. The average parity of these patients was 1.67 ± 0.82 children with a range of 0–4 previous pregnancies (Table 1).
| Min | Max | Mean | SD | |
|---|---|---|---|---|
| Age (in years) | 18 | 36 | 24.37 | 4.68 |
| Gestational age (in weeks) | 7 | 11 | 8.21 | 1.17 |
| Symptoms duration (in days) | 1 | 6 | 3.5 | 2.5 |
| Number of previous pregnancies | 0 | 4 | 1.67 | 0.82 |
Table 1: Quantitative analysis of collected data (n=73).
Age grouping of patients showed that nearly three fifth of the patients; 60.28% (n=44) were of age between 23–32 years, 21.91% (n=16) patients were in age category of 22 years & below while 17.80% (n=13) patients were in age category of 33 years & above (Table 2).
| Age category | Frequency | Percent |
|---|---|---|
| ≤ 22 Years | 16 | 21.91 |
| 23-32 Years | 44 | 60.28 |
| ≥ 33 Years | 13 | 17.8 |
| Total | 73 | 100 |
Table 2: Age groups of patients n=73.
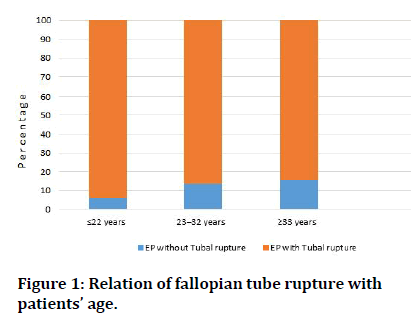
Occurrence of fallopian tube rupture in patients of ectopic implantation was 87.67% (n=64). Age wise classification for assessment of recurrence of tubal rupture revealed that ectopic pregnancy was most prevalent in younger age groups (i.e., 93.75% (n=15) in ≤ 22 years). The frequency diminished with advancing age (i.e., 86.36% (n=38) and 84.64% (n=11) in 23–32 years and ≥ 33 years age group respectively (Figure 1).
Figure 1: Relation of fallopian tube rupture with patients’ age.
Gestational age had a significant effect on recurrence of fallopian tube rupture in EP patients.
Furthermore it was revealed that advancing age of gestation from 7 weeks to 11 weeks was directly proportional to incidence of rupture of fallopian tube, rising from 84.48% to 100%(Table 3).
| Tubal rupture | Total | P-value | ||
|---|---|---|---|---|
| Age of Pregnancy | Yes | No | ||
| Less than 7 weeks | 49 (84.48%) | 9 (15.52) | 58 | 0.086 |
| 7-11 weeks | 15 (100%) | 0 (0%) | 15 | |
| Total | 64 | 9 | 73 | |
Table 3: Proportional increase in tubal rupture with age of pregnancy in ectopic gestations.
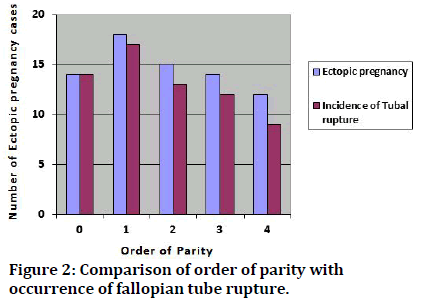
Greater number of previous gestations was found to be a remarkable determinant of increasing occurrence of fallopian tube rupture. Null parity was linked with maximum incidence (100%, n=14) decreasing to 75% with advancing order of pregnancy (Figure 2) (Table 4).
| Number of previous pregnancies | Fallopian tube rupture | Total | p-value | |
|---|---|---|---|---|
| Yes | No | |||
| 0 | 14 (100%) | 0 (0%) | 14 | 0.039 |
| 1 | 17 (94.45%) | 1 (5.55%) | 18 | |
| 2 | 13 (86.7%) | 2 (13.3%) | 15 | |
| 3 | 12 (85.8%) | 2 (14.2%) | 14 | |
| 4 | 9 (75%) | 3 (25%) | 12 | |
| Total | 64 | 7 | 73 | |
Table 4: Relationship of order of pregnancy with occurrence of fallopian tube rupture.
Figure 2: Comparison of order of parity with occurrence of fallopian tube rupture.
In addition, we noticed that earlier the patients reported to hospital, lesser was the chance of rupture of fallopian tube. On average, patients reported in 2.19 ± 1.44 days of appearance of first symptom, ranging from 1 to more than 4 days. Patients presenting within 2 days of appearance of symptoms, the incidence was 83.3% when contrasted with late comers in whom occurrence was 100% (Table 5).
| Tubal rupture | Total | p-value | ||
|---|---|---|---|---|
| Duration of symptoms | Yes | No | ||
| Less than 4 days | 45 (83.3%) | 9 (16.7%) | 54 | 0.398* |
| ≥4 days | 19 (100%) | 0 (0%) | 19 | |
| Total | 64 | 9 | 73 | |
| *p-value not significant | ||||
Table 5: Incidence of tubal rupture in ectopic pregnancy in comparison with duration of presentation to healthcare facility.
Discussion
“Ectopic pregnancy is a high-risk condition with an estimated incidence of 11.1/1000 deliveries” [9]. It is very common and debilitating condition for women of reproductive age, most prevalent in developing countries. A study performed in Pakistan estimated the incidence of ectopic gestations to be 10/1000 deliveries [10]. In our study, the occurrence of ectopic pregnancy was 1.15% (73/6346) which is 11.5/1000 pregnant patients reporting to hospital.
In a hugely populated developing country like Pakistan, the true incidence of ectopic pregnancy might be much higher owing to the lesser medical care seeking attitude of women of reproductive age. This study is undertaken in view of the fact that majority of patient with EP are brought in casualty in critical conditions. Our study offers on rupture of fallopian tube with ectopic gestations. The extent of fallopian tube rupture is still at peak in our populace. We discovered that, in the entirety of these patients, ectopic conceptus was implanted in fallopian tube, comparable with different researches done around the globe in which the majority of ectopic gestations occurred in fallopian tubes [6,11-13]. The frequency of tubal rupture in our study was 87.67%. Our reported incidence is similar to other studies done by Ashfaq, Tabassum and Aziz et al. [14-16]. The significantly high incidence of fallopian tube rupture was secondary to lack of awareness in general population, lack of healthcare seeking attitude in women, unpredictability of gestational outcome, hence the resulting delayed diagnosis caused by unavailability of diagnostic tools such as trans-vaginal ultrasound and β hCG measurements.
Our study shows that most cases of tubal rupture occurs in young age group. Literature review revealed only one study showing increased tubal rupture with increasing age [2]. Most of the cases of fallopian tube rupture were seen in nulliparous and primigravida. Our findings are consistent with other studies [11,13,17]. Some studies show an increase in incidence of ectopic pregnancy with multiparity. In our study, we found more number of cases of rupture of fallopian tube in association with nullipaity. In our study mean gestational age found to be 8.21 ± 1.17 weeks which is in correspondence with study done by Khaleeque and Pinar Cilesiz [12,18]. Advancing age of gestation caused an increment in occurrence of tubal rupture. Majority of patients presenting late in state of shock require resuscitation preoperatively. Late reporting to hospital is a primary cause of death in these patients as identified in other studies as well [13].
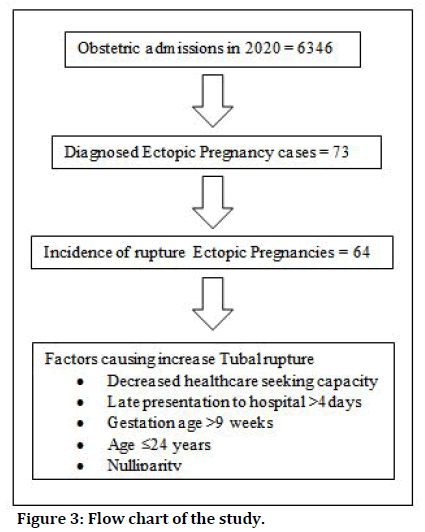
Studies have mentioned variable rates of maternal mortality due to tubal rupture. In our study, we did not have any maternal death associated with tubal rupture in ectopic pregnancy. Late presentation is one of the main reason of complications. It leads to life threatening complications and decreases the chances of tubal conservation. Laparotomy was the primary surgery embraced in intense introduction with internal bleeding. A small portion of the patient received laparoscopic treatment yet the laparoscopic facility isn't generally accessible in most parts of our country. Patients who underwent laparoscopy had a good prognosis. We found that there is increased demand of blood transfusion may be associated with treating cases of fallopian tube ectopic conceptions, though the review information was not accessible, which is the constraint of our research work (Figure 3).
Figure 3: Flow chart of the study.
Conclusion
Tubal rupture in ectopic pregnancy remains a medical emergency of high degree and a gynaecological catastrophe for women of reproductive age in developing countries like Pakistan.
It should be considered a nation wise women health problem. The rising incidence of ectopic pregnancy is likely to continue increasing because of the younger age fertility in women, thus it is necessary to devise means of early predictability and prompt detection. This may also be attributed to the delay in diagnosis due to late presentation and lack of medical care seeking attitude. The ease of access, mass awareness to seek medical care, better healthcare facilities with accurate diagnosis and precise management would result in a considerable reduction in morbidity and mortality related to ectopic pregnancy.
References
- www.uptodate.com/contents/ectopic-pregnancy-epidemiology-risk-factors-and-anatomic-sites.
- Chukus A, Tirada N, Restrepo R, et al. Uncommon implantation sites of ectopic pregnancy: Thinking beyond the complex adnexal mass. Radiographics 2015; 35:946-59.
- Berlingieri P, Bogdanskiene G, Grudzinskas JG. Rupture of tubal pregnancy in the Vilnius population. Eur J Obstet Gynecol Reprod Biol 2007; 131:85-88.
- Sara HG, Uzelac PS. Early pregnancy risks. Current diagnosis and treatment: Obstetrics and gynecology. 10th Edn. Columbus (OH): McGraw-Hill 2007.
- https://www.verywellfamily.com/what-do-statistics-look-like-for-ectopic-pregnancy-2371730
- Ehsan N, Mehmood A. Ectopic pregnancy: An analysis of 62 cases. J Pakistan Med Assoc 1998; 48:26-29.
- Monga A, Dobbs SP. Gynaecology by ten teachers. CRC Press 2011.
- Carusi D. Pregnancy of unknown location: Evaluation and management. Semin Perinatol 2019; 43:95-100.
- Lozean AM, Potter B. Diagnosis and management of ectopic pregnancy. Am Fam Physician 2005; 72:1707-17114.
- Mahboob U, Mazhar SB. Management of ectopic pregnancy: A two-year study. J Ayub Med Coll Abbottabad 2006; 18:34-7.
- Shah N, Khan HN. Ectopic pregnancy: Presentation and risk factors. J Coll Physicians Surg Pal 2005; 15:535-8.
- Khaleeque F, Siddiqui RI, Jafarey SN. Ectopic pregnancies: A three-year study. J Pak Med Assoc 2001; 51:240-243.
- Wasim T. Propotionate morbidity and risk factors of ectopic pregnancy. Ann King Edward Med Univ 2004; 10:298-300.
- Ashfaq S, Sultan S, Aziz S, et al. Ectopic pregnancy with tubal rupture: an analysis of 80 cases. J of Ayub Med Coll Abbottabad 2017; 29:254-7.
- Tabassum RU, A AM, Ahmed MA. Risks factors for tubal ectopic pregnancy. J Surg Pak 2005; 10:22–5.
- Aziz S, Al Wafi B, Swadi H. Frequency of ectopic pregnancy in medical center, Kingdom of Saudia Arabia. J Pak Med Assoc 2001; 61:221-4.
- Hassan N, Zaheen Z, Jatoi N, et al. Risk factors, clinical presentation and management of 62 cases of ectopic pregnancy at tertiary care center. J Liaquat Univ Med Health Sci 2009; 8:238–41.
- Goksedef BP, Kef S, Akca A, et al. Risk factor for rupture in tubal ectopic pregnancy: Definition of the clinical findings. Eur J Obstet Gynecol Reprod Biol 2011; 154:96–99.
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Author Info
Meena Bai1, Ome Kulsoom2*, Azra3, Bushra4, Jabeen Atta5 and Shumaila Javaid6
1Department of Gynaecology and Obstetrics, Civil Hospital Dow University of Health Sciences Karachi, Pakistan2Department of Gynaecology and Obstetrics, Ziauddin University Hospital Karachi, Pakistan
3Department of Gynaecology and Obstetrics Suleman Roshan Medical College Tandoadam, Pakistan
4Department of Gynaecology and Obstetrics Muhammad Medical College Mirpurkhas, Pakistan
5Department of Gynaecology and Obstetrics, Bilawal Medical College LUMHS Jamshoro, Pakistan
6Department of Gynaecology and Obstetrics, Sharif Postgraduate medical institute, sharif medical city hospital Lahore, Pakistan
Citation: Meena Bai, Ome Kulsoom, Azra, Bushra, Jabeen Atta, Shumaila Javaid,Incidence, Predictability and Causes of Tubal Rupture IN Ectopic Pregnancy in a Pakistani Population: A Descriptive Cross-Sectional Study, J Res Med Dent Sci, 2022, 10(1): 110-115.
Received: 21-Dec-2021, Manuscript No. JRMDS-21-48248; , Pre QC No. JRMDS-21-48248 (PQ); Editor assigned: 23-Dec-2021, Pre QC No. JRMDS-21-48248 (PQ); Reviewed: 06-Jan-2022, QC No. JRMDS-21-48248; Revised: 10-Jan-2022, Manuscript No. JRMDS-21-48248 (R); Published: 17-Jan-2022