Research - (2021) Volume 9, Issue 2
Microbial Contamination of Toothbrush Bristles among Gingivitis and Periodontitis: An in vitro study
Saravanan and Sankari Malaiapan*
*Correspondence: Sankari Malaiapan, Department of Periodontics, Saveetha Dental College and Hospital, Saveetha Institute of Medical and Technical Sciences (SIMATS), Saveetha University Tamilnadu, Chennai, India, Email:
Abstract
Microbes survive in a wide variety of environments, including toothbrush bristles regardless where they are kept. Microbial contamination of toothbrush bristles occurs after the initial use and increases with repeated usage. The aim of the study was to quantify the microbial contamination of toothbrush bristles among gingivitis and periodontitis subjects. A total 10 subjects’ toothbrush bristles were collected and cultured. The total number of colony forming units after 24 hours ,Gingivitis group sample1 shows(1.02%),sample 2(0.75%),sample 3(0.95%), sample 4(1.49%) and sample 5(14.27%) and Periodontitis group sample 1(11.5%),sample 2(8.83%),sample 3(19.02%), sample 4(17.66%) and sample 5(24.46%). From the study it can be inferred that microbial contamination was higher in periodontitis patients' bristles than the gingivitis.
Keywords
Toothbrush bristles, Microorganism, Brain infusion agar, Sabouraud agar
Introduction
Bacterial plaque in the vicinity of gingival margin has been emphasized to play a potential role in the pathogenesis of periodontal disease; Regular removal of supragingival plaque has been shown to reduce counts of pathogenic species [1]. Mechanical plaque control is done by toothbrush and interdental aids. Our study was done with mechanical plaque control such as toothbrush. Plaque control is important for maintaining oral hygiene. Mechanical plaque control can be done at home. Tooth brush is an efficient tool for removing the oral biofilm and therefore the soft debris out of the mouth, especially from the tooth and tongue surfaces, is that of the toothbrush. Choice of tooth brush isn't important but the care and maintaining of the toothbrush are important for the good oral hygiene and health also, toothbrush isn't the perfect environment for microorganisms’ growth, it's capable to get microbes from plaque and calculus in mouth .Oral hygiene is an important practice for healthy living. The first devices utilized in cleaning the teeth include the twig brush, tooth stick, also referred to as the toothpick, and plantain stalk with charcoal [2]. Microbial contamination of toothbrush bristles occurs after use and increase of microbial load [3,4]. The microbes that contaminate toothbrush bristles originate from oral cavities and moist environment [5]. The biofilms that develop within the toothbrushes contain different bacterial species [6], viruses [7] and fungi [8,9] that are present within the mouth, also as some from the environment. The maintenance of toothbrushes are of enormous importance for bacterial survival: toothbrushes which are kept in rooms with open air have less bacteria than those which are kept closed, and therefore the bacterial growth is 70% higher in a wet and guarded environment. The wet environment within the bathroom, where toothbrushes are usually kept, may facilitate the bacterial growth and therefore the crossed contamination. The aerosols produced during flushing in lavatories, carries E.coli and Pseudomonas [10]. Plaque control is important for maintaining oral hygiene. Mechanical plaque control can be done at home. Tooth brush is an important factor which has been used daily to reduce plaque accumulation. As tooth brushes were used regularly more number of microorganism harbour in toothbrush bristles. Proper maintenance of tooth brush helps in reduction of plaque and prevent from periodontal disease. Previously we worked on plenty of topics in periodontics [11-26]. And now the current study was done to identify the differences in microbial contamination in toothbrush bristles between gingivitis and periodontitis subjects.
Materials and Methods
Patients visited the Department of Periodontics in Saveetha dental college were included in this study in which ten patients' tooth brushes were collected, were from both sexes male and female. Toothbrushes were collected from Gingivitis and periodontitis subjects. In which 5 toothbrushes were collected from gingivitis and 5 toothbrushes were collected from patients with periodontitis. Inclusion criteria gingivitis patients, periodontitis patients who were under 1st dental visit before phase 1 therapy and exclusion criteria patients who have undergone periodontal therapy, patients under periodontal treatment. The study was approved by the institutional review board and ethical committee. Informed consent was obtained from all participants before commencement of the study. The study was done in BRULAC department of Saveetha University. The samples (Toothbrush bristles) were collected in a sterile container with 10 ml brain heart infusion agar is a growth media for microorganisms which is used in culture. The plates were stored in a bacteriological incubator at 37° C for a period of 24 hours for microbial growth analysis. After 24h growth the colony-forming units (CFU) were counted and subsequent microorganisms identification. Total numbers of microorganisms were determined in each plate. Each plate containing microorganism was counted and estimated in Total viable count (TVC) gives quantitative estimation of bacteria, number of colony forming units (CFU/ml).
Results and Discussion
A total of 10 toothbrushes were collected from patients visiting Department of Periodontics, which 5 toothbrushes were collected from gingivitis patients and 5 toothbrushes were collected from periodontitis patients. Patient with Gingivitis group sample1 shows (1.02%), sample 2(0.75%), sample 3(0.95%), sample 4(1.49%) and sample 5(14.27%) and Periodontitis group sample 1(11.5%), sample 2(8.83%), sample 3(19.02%), sample 4(17.66%) and sample 5(24.46%) (Figures 1 and 2).

Figure 1. This figure shows the number of bacterial colonies formed from toothbrush samples obtained from gingivitis and periodontitis patients.
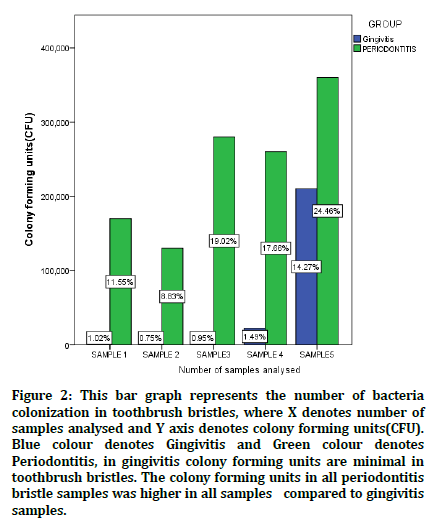
Figure 2. This bar graph represents the number of bacteria colonization in toothbrush bristles, where X denotes number of samples analysed and Y axis denotes colony forming units(CFU). Blue colour denotes Gingivitis and Green colour denotes Periodontitis, in gingivitis colony forming units are minimal in toothbrush bristles. The colony forming units in all periodontitis bristle samples was higher in all samples compared to gingivitis samples.
After 24 hours colony forming units were assessed in gingivitis patients and periodontitis patients which shows patients with periodontitis patients has higher amount of colony formation units in toothbrush bristles compared with gingivitis patients has lesser number of colony forming units. In our study patients with gingivitis and periodontitis were selected who visited first time for dental treatment. Gingivitis and Periodontitis occurs due to accumulation of plaque and calculus study. The result was colony forming units in gingivitis was in concurrence without values but no direct comparison is possible since they have compared healthy against gingivitis. The toothbrush contamination among healthy individuals occurs earlier after the primary use, and increases with its further usage [27,28]. Oral cavity harbors highest concentrations of various microbial populations (more than bacterial 700 species’, from which 400 are found within the periodontal pockets [29]. The alpha haemolytic streptococci have periodontal pathogen potential; can prevent the colonization of the more pathogenic species’, also as viridans streptococci which may have a role due to the expansion inhibition of the periodontal pathogens [30]. The microorganisms get locked across E.coli [29]. The contaminated toothbrushes harbour pathogenic bacteria that cause local and systemic infections. Thus can serve as potential sources of various systemic conditions, like heart diseases, arthritis, bacteremia and brain stroke. Immuno compromised patients organisms are more prone to super infections, like multiple drugs resistant Enterococcus faecalis and enteric gram negative species’, Pseudomonas and Candida albicans, in gediadrtic patients excessive antibiotic overload [3]. Evidence shows that toothbrushes from both healthy patients and patients with oral disease had both potentially pathogenic bacteria and viruses such as Staphylococcus aureus, E. coli, Pseudomonas, and herpes simplex virus. The inflammatory bowel disease patients responded well to treatment after replacement of the contaminated toothbrushes once they replaced the used toothbrushes with new ones [4]. The different microorganisms could grow on toothbrushes after its usage [27]. The bacteria that adhere accumulate and survive on the toothbrushes, could also be transferred across to the individuals, thus spreading the disease [5,31]. The fluids and food debris accumulate in the spaces between tufts by capillary action; and serve as nidus for bacterial growth [32]. The toothbrushes when kept in closed containers are safer than exposed surfaces which have higher bacterial counts [33]. Retention of moisture and oral debris within the bristles enhanced bacterial survival [7]. Bacteria get entrapped within the bristles and enhance bacterial survival (aerobic versus anaerobic), toothbrush design also plays a significant role [9]. The toothbrush can act as a reservoir for microbial colonization. Advances in therapeutic strategy for treatment of periodontal disease should not underestimate the value of mechanical plaque control. The study limitations are smaller sample size and periodontal pathogens harboring the bristles also should be assessed with a larger sample. As per the saying prevention is better than cure, simple maintenance of not only oral but also the tooth brushes plays a significant role in local and systemic wellbeing.
Conclusion
In Periodontitis patients show a higher amount of colony forming units compared to gingivitis patients shows lower amount of colony forming units.
Acknowledgement
Saravanan carried out the study, participated in the sequence alignment, statistical analysis and drafted the manuscript. Dr.Sankari Malaippan conceived the study, participated in its design and coordinated and provided guidance to draft the manuscript. All authors read and approved the manuscript.
Conflict of Interest
There were no conflicts of interest as defined by the authors.
References
- Haffajee AD, Thompson M, Torresyap G, et al. Efficacy of manual and powered toothbrushes (I). Effect on clinical parameters. J Clin Periodontol 2001; 28:937-946.
- Hyson JM. History of the toothbrush. J History Dent 2003; 51:73–80.
- Saravia ME, Nelson-Filho P, da Silva RA, et al. Viability of Streptococcus mutans toothbrush bristles. J Dent Children 2008; 75:29-32.
- Warren DP, Goldschmidt MC, Thompson MB, et al. The effects of toothpastes on the residual microbial contamination of toothbrushes. J Am Dent Assoc 2001; 132:1241-1245.
- Caudry SD, Klitorinos A, Chan EC. Contaminated toothbrushes and their disinfection. J Canadian Dent Assoc 1995; 61:511-516.
- Moore G, Smyth D, Singleton J, et al. Does targeted and quantified control of the microbiological environment within the intensive care unit reduce colonisation and healthcare-acquired infection?: P1643. Clin Microbiol Infection 2009; 15.
- Mehta A, Sequeira PS, Bhat G. Bacterial contamination and decontamination of toothbrushes after use. New York State Dent J 2007; 73:20.
- Lock G, Dirscherl M, Obermeier F, et al. Hepatitis C–contamination of toothbrushes: Myth or reality?. J Viral hepatitis 2006; 13:571-573.
- Bunetel L, Tricot‐Doleux S, Agnani G, et al. In vitro evaluation of the retention of three species of pathogenic microorganisms by three different types of toothbrush. Oral Microbiol Immunol 2000; 15:313-316.
- Muhammed SQ, Alhumdany AA, Al-Waily ML. Effects of nano-zinc oxide on tensile properties of natural rubber composite. Kufa J Eng 2018; 9:77-90.
- Kaarthikeyan G, Jayakumar ND, Sivakumar D. Comparative evaluation of bone formation between PRF and blood clot alone as the sole sinus-filling material in maxillary sinus augmentation with the implant as a tent pole: A randomized split-mouth study. J Long Term Effects Med Implants 2019; 29.
- Ravi S, Malaiappan S, Varghese S, et al. Additive effect of plasma rich in growth factors with guided tissue regeneration in treatment of intrabony defects in patients with chronic periodontitis: a split‐mouth randomized controlled clinical trial. J Periodontol 2017; 88:839-845.
- Murthykumar K, Arjunkumar R, Jayaseelan VP. Association of vitamin D receptor gene polymorphism (rs10735810) and chronic periodontitis. J Investigative Clin Dent 2019; 10:e12440.
- Ramesh A, Vellayappan R, Ravi S, et al. Esthetic lip repositioning: A cosmetic approach for correction of gummy smile–A case series. J Indian Society Periodont 2019; 23:290.
- Ramesh A, Varghese S, Jayakumar ND, et al. Comparative estimation of sulfiredoxin levels between chronic periodontitis and healthy patients–A case‐control study. J Periodont 2018; 89:1241-1248.
- Vijayashree Priyadharsini J. In silico validation of the non‐antibiotic drugs acetaminophen and ibuprofen as antibacterial agents against red complex pathogens. J Periodont 2019; 90:1441-1448.
- Ramesh A, Ravi S, Kaarthikeyan G. Comprehensive rehabilitation using dental implants in generalized aggressive periodontitis. J Indian Society Periodont 2017; 21:160.
- Arjunkumar R. Nanomaterials for the management of periodontal diseases. Dent App Nanotechnol 2018; 203-215.
- Kavarthapu A, Thamaraiselvan M. Assessing the variation in course and position of inferior alveolar nerve among south Indian population: A cone beam computed tomographic study. Indian J Dent Res 2018; 29:405.
- Khalid W, Vargheese SS, Lakshmanan R, et al. Role of endothelin-1 in periodontal diseases: A structured review. Indian J Dent Res 2016; 27:323.
- Khalid W, Varghese SS, Sankari M, et al. Comparison of serum levels of endothelin-1 in chronic periodontitis patients before and after treatment. J Clin Diagnos Res 2017; 11:ZC78.
- Priyanka S, Kaarthikeyan G, Nadathur JD, et al. Detection of cytomegalovirus, epstein–barr virus, and torque teno virus in subgingival and atheromatous plaques of cardiac patients with chronic periodontitis. J Indian Society of Periodont 2017; 21:456-460.
- Ramamurthy JA, Mg V. Comparison of effect of hiora mouthwash versus chlorhexidine mouthwash in gingivitis patients: A clinical trial. Asian J Pharm Clin Res 2018; 11:84.
- Ramesh A, Varghese SS, Doraiswamy JN, et al. Herbs as an antioxidant arsenal for periodontal diseases. J Intercultural Ethnopharmacol 2016; 5:92.
- Thamaraiselvan M, Elavarasu S, Thangakumaran S, et al. Comparative clinical evaluation of coronally advanced flap with or without platelet rich fibrin membrane in the treatment of isolated gingival recession. J Indian Society Periodontol 2015; 19:66.
- Varghese SS, Thomas H, Jayakumar ND, et al. Estimation of salivary tumor necrosis factor-alpha in chronic and aggressive periodontitis patients. Contemporary Clin Dent 2015; 6:S152.
- Beneduce C, Baxter KA, Bowman J, et al. Germicidal activity of antimicrobials and VIOlight® personal travel toothbrush sanitizer: An in vitro study. J Dent 2010; 38:621-625.
- Downes J, Hooper SJ, Wilson MJ, et al. Prevotella histicola sp. nov., isolated from the human oral cavity. Int J Systematic Evolutionary Microbiol 2008; 58:1788-1791.
- Slots J, Jorgensen MG. Effective, safe, practical and affordable periodontal antimicrobial therapy: Where are we going, and are we there yet?. Periodontol 2000; 28:298-312.
- Naik R, Mujib BA, Telagi N, et al. Contaminated tooth brushes–potential threat to oral and general health. J Family Med Primary Care 2015; 4:444.
- ADA Division of Communications. For the dental patient. Toothbrush care, cleaning and replacement. J Am Dent Assoc 2006; 137:415.
- Glass RT, Lare MM. Toothbrush contamination: a potential health risk? Quintessence Int 1986; 7:39–42.
- Dayoub MB, Rusilko D, Gross A. Microbial contamination of toothbrushes. J Dent Res 1977; 56:706–706.
Author Info
Saravanan and Sankari Malaiapan*
Department of Periodontics, Saveetha Dental College and Hospital, Saveetha Institute of Medical and Technical Sciences (SIMATS), Saveetha University Tamilnadu, Chennai, IndiaCitation: Shebi S, Karthik Ganesh Mohanraj, Morphometric Localization of Mandibular Foramen with Reference to Various Anatomical Landmarks in Dry Human Mandibles and its Clinical Implications, J Res Med Dent Sci, 2021, 9 (2): 239-242.
Received: 23-Sep-2020 Accepted: 11-Feb-2021
