Case Report - (2022) Volume 10, Issue 5
Nerve Sheath Myxoma-A Rare Case Report
Satyam Singh1*, Samarth Shukla1, Sourya Acharya2 and Preeti Mishra1
*Correspondence: Satyam Singh, Department of Pathology, Jawaharlal Nehru Medical College, Sawangi, Wardha,maharastra, India, Email:
Abstract
Nerve Sheath Myxoma, an infrequent benign soft tissue neoplasm of peripheral nerves emerges from nerve sheath was first illustrated by Harkin and Reed in 1969.Nerve Sheath Myxoma strike people of all peer category and same predisposition for both with most frequent area of occurrence being the fingers and knee. Here, we introduce a case report of nerve sheath myxoma of the Axilla, diagnosed and confirmed with histopathology.Keywords
Ne rve sheath, Myxoma, Neoplasm, Soft tissue, AxillaIntroduction
Nerve Sheath Myxoma is an infrequent benign soft tissue neoplasm. It emerges from nerve sheath. It was first illustrated by Harkin and Reed in 1969 [1]. And formulated title “Nerve Sheath Myxoma”. Earlier, it was contemplated to be analogous to neurothekeoma. However, recent studies revealed that both neoplasms have different origins [2,3]. In this article we report a case of Nerve Sheath Myxoma occurring in Right axilla (Figure1).
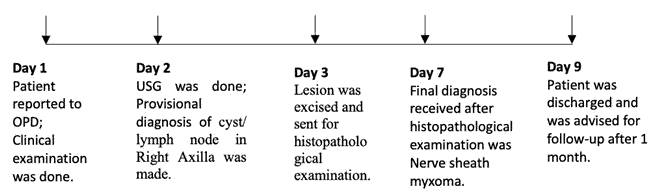
Figure 1: Timeline
Case Presentation
A 51 years old male patient presented to Surgical OPD with complaints of swelling in Right Axilla for 2 months.
Clinical findings
On examination, two swellings were present in Right Axilla with measurement of size 2 × 1 cm and 1 × 1 cm respectively which were soft, painless, firm and mobile.
Diagnostic assessment
Ultrasound suggested multiple lobulated hypoechoic lesions in the subcutaneous plane with loss of fatty hilum likely to be lymph nodes suggestive of infective etiology. Based on clinical examination and USG findings, a clinical diagnosis of cyst/lymph node in Right Axilla was made. Lesion was excised and sent for histopathological examination. Specimen received on gross examination single, irregular, whitish brown tissue piece with skin and fat attached. Specimen measuring 3.2 × 1 × 0.6 cm. Skin measuring 3.5 × 0.5 cm. On cut section, whitish cystic area identified.
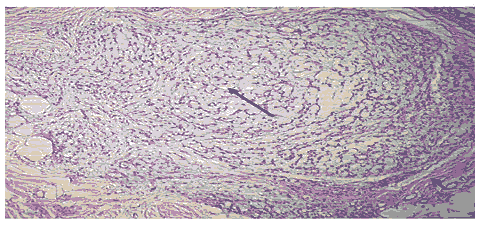
Figure 2: Photomicrograph 1(10x view) HE-stained slide shows cellular tumour tissue arising from peripheral nerve sheath (short arrow) tissue predominantly shows stellate to spindle shaped cell (long arrow) with mild atypia, scant eosinophilic cytoplasm, cells are scattered around fibro myxoid stroma interconnected through bipolar processes.
Peripheral areas of photomicrograph show unremarkable nerve sheath, multiple myxoid lobules, cells are small stellate to spindle shaped with mild nuclear atypia, scant eosinophilic cytoplasm with thin processes scattered in myxoid fibro myxoid stroma. At places shows occasional mitotic figure. Based on these features, histopathological diagnosis of nerve sheath myxoma was reported. Patient was advised for follow up after 1 month, but patient lost to follow up. The informed consent was obtained from the patient.
Discussion
Nerve sheath myxoma is an uncommon benign soft tissue tumour of peripheral nerves. It was firstly explained by Harkin and Reed [1]. As a myxoid neoplasm of benign nature with emergence from Schwann cells. It manifests as sluggish growth asymptomatic nodular lesion in dermis and subcutaneous tissues, most frequent area of occurrence are fingers and knees [2]. Nerve sheath myxoma was earlier regarded as Neurothekeoma. Recent researches have evidently distinguished these neoplasms as two different existence based on histomorphology, immunohistochemistry, and genetic evaluations [3-4]. On histopathological investigation, nerve sheath myxoma displays a well-defined multiple nodular neoplasm consisting myxoid nodules splitted by thread-like partition (septae). These nodules have scattered clumping of benign spindle-stellate and epithelioid cells encompassing by myxoid stroma. The neoplastic cells are conclusive for S-100, Glial Fibrillary Acidic Protein (GFAP), vimentin, and collagen type IV [5]. In their genomic study, have advocated that nerve sheath myxoma has emergence from peripheral nerve sheath cells, while neurothekeoma mimic cellular fibrous histiocytomas and they derived from fibroblastic cells. [3,4] Immunohistochemically study showed, neurothekeomas are favourable for EMA and are unfavourable for S-100 and GFAP and their most frequent area of occurrence comprising head and neck, where it exhibits as an individual mass [6].
Other histopathological distinctive interpretation of nerve sheath myxoma includes myxoid tumors, consisting of plexiform neurofibroma, myxoid neurofibroma, myxoid schwannoma, extraneural perineuroma, and cutaneous, juxta-articular, and intramuscular myxomas [2]. Myxoid neurofibroma is imperfectly confined tumour which is not capsulated, devoid of lobular structure and revealing patchy S-100 positivity [7]. Myxoid schwannoma displays centre of Antoni A with Verocay bodies. They do not manifest multinodularity but demonstrate S-100 [2]. Extraneural perineuromas demonstrates a helical design arranged in clusters of myxoid or collagenous stroma. They can be distinguished from nerve sheath myxoma on immunohistochemistry as perineuromas demonstrate conclusive for EMA and are negative for S-100, GFAP, and CD34 [8].Cutaneous myxomas in the dermis and subcutis show numerous myxoid masses, with neoplastic cells, being spindle to stellate configuration. Cutaneous myxomas show CD34 positivity but are negative for S-100 [9]. Intramuscular and juxta-articular myxomas might depict same histopathological features but are clinically eliminated [2]. Plexiform neurofibroma, linked to neurofibromatosis, includes nerve trunks which are large and is multinodular, myxoid lesions, which depicts S-100 immunostaining [2].
Conclusion
We introduce an uncommon case report of nerve sheath myxoma, at a rare site in Right Axilla. It signifies to differentiate nerve sheath myxoma with other additional myxoid tumours, principally neurothekeoma. Immunohistochemical studies have a central character in confirmation as histomorphological characters solely are not adequate for the conclusion. The demarcation from neurothekeoma is of paramount importance as nerve sheath myxomas have a powerful tendency to give rise to regional reoccurrences.
References
- Reed RJ, Harkin JC. Tumors of the peripheral nervous system. Armed Forces Institute of Pathology. 1983.
- Bhat A, Narasimha A, Vijaya C, et al. Nerve sheath myxoma: report of a rare case. Jcdr 2015; 9:07.
- Fetsch JF, Laskin WB, Hallman JR, et al. Neurothekeoma: an analysis of 178 tumors with detailed immunohistochemical data and long-term patient follow-up information. Am J Surg Pathol 2007; 31:1103-1114.
- Sheth S, Li X, Binder S, et al. Differential gene expression profiles of neurothekeomas and nerve sheath myxomas by microarray analysis. Modrn Pathol 2011; 24:343-354.
- Fetsch JF, Laskin WB, Miettinen M, et al. Nerve sheath myxoma: a clinicopathologic and immunohistochemical analysis of 57 morphologically distinctive, S-100 protein-and GFAP-positive, myxoid peripheral nerve sheath tumors with a predilection for the extremities and a high local recurrence rate. Am j surg pathol 2005; 29:1615-1624.
- Bartake A, Palaskar SJ, Narang B, et al. Nerve sheath myxoma of the oral cavity: a distinct entity. Br J Neurosurg 2019; 33(2):213-214.
- Ponce-Olivera R, Tirado-Sanchez A, Peniche-Castellanos A, et al. Myxoid neurofibroma: an unusual presentation. Ind j dermatol 2008; 53:35.
- Housini I, Dabbs DJ. Fine needle aspiration cytology of perineurioma. Report of a case with histologic, immunohistochemical and ultrastructural studies. Acta cytol 1990; 34:420-424.
- Carney JA, Headington JT, Su WD, et al. Cutaneous myxomas: a major component of the complex of myxomas, spotty pigmentation, and endocrine overactivity. Arch dermatol 1986; 122:790-800.
Author Info
Satyam Singh1*, Samarth Shukla1, Sourya Acharya2 and Preeti Mishra1
1Department of Pathology, Jawaharlal Nehru Medical College, Sawangi, Wardha,maharastra, India2Department of Medicine, Jawaharlal Nehru Medical College, Sawangi, Wardha, maharastra, India
Citation: Satyam Singh, Nerve Sheath Myxoma-A Rare Case Report, J Res Med Dent Sci, 2022, 10(5): 51-52.
Received: 23-Feb-2022, Manuscript No. 44288; , Pre QC No. 44288; Editor assigned: 25-Feb-2022, Pre QC No. 44288; Reviewed: 11-Mar-2022, QC No. 44288; Revised: 25-Apr-2022, Manuscript No. 44288; Published: 03-May-2022
