Case Report - (2022) Volume 10, Issue 3
Pathognomonic Oral Profile of Lubinsky-MacGibbon Syndrome for Lowering the Risk of Progressive Renal Failure: Rare Case Report
Almoataz Bellah Abdullah Tawfiq Abdel-Bari*, Ahmed Abd El-Latif Mosleh and Khaled Abd El-Hamid Saad
*Correspondence: Almoataz Bellah Abdullah Tawfiq Abdel-Bari, Department of Oral and Maxillofacial Surgery, Tanta University, Egypt, Email:
Abstract
Lubinsky-MacGibbon syndrome is an extremely rare condition characterized by defective amelogenesis and bilateral medullary nephrocalcinosis. Because nephrocalcinosis is symptomless even though renal complications may not emerge until late childhood or early adulthood, the pathognomonic orodental findings and panoramic radiographic features present in early childhood play an exclusive role in the early detection of this rare syndrome for better renal prognosis.
Keywords
Lubinsky-macgibbon syndrome, Enamel renal syndrome, Amelogenesis imperfecta, Multiple impacted teeth, Consanguineous parents, Bilateral medullary nephrocalcinosis
Introduction
Lubinsky-MacGibbon syndrome is recognized by several synonyms including, but not limited to, enamel renal syndrome (ERS), amelogenesis imperfecta nephrocalcinosis syndrome, MacGibbon syndrome, Lubinsky syndrome [1].
It is an extremely rare inherited disorder caused by recessive FAM20A gene mutations, which also responsible for “Amelogenesis Imperfecta and Gingival Fibromatosis Syndrome “(AIGFS). A detailed clinical comparative aspect of both syndromes concludes that the recessive FAM20A mutations cause a single illness with a specific oral phenotype often linked to renal calcification, but in the former the oral phenotype has been extensively investigated while in latter one the kidney phenotype has not been fully investigated [2]. The office of rare diseases of the National Institutes of Health lists it as a "rare illness".
Amelogenesis imperfecta (AI) is a broad term for a collection of inherited diseases that affect the structure and look of the enamel of all or nearly all teeth in an equal way, causing structural and clinical alterations to the enamel. It is inherited in an autosomal dominant, autosomal recessive or X-linked manner and may be related to morphologic or biochemical alterations in other body regions [3]. There are various multi-organ disorders that have this trait; however, it is only a pathognomonic of a handful [4,5].
The first time that AI and nephrocalcinosis (NC) were documented in a young lady after her 26-year-old brother, who had both, died. Until the age of 16, renal function was steady in the documented instances, but renal failure and death soon followed [6]. More and more instances of NC and enamel abnormalities have been documented in recent years under "Amelogenesis imperfecta and nephrocalcinosis" or "Enamel Renal Syndrome" terms [7]. The typical oral features even if, inexistence of accompanying developmental health issues is pathognomonic, with significant enamel hypoplasia, delayed or absent tooth eruption, ectopic eruption route, and pulp and gingival calcification in both the temporary as well as permanent dentition. Also, coexistence of gingival hyperplasia, which may range from subtle to severe from one patient to another [2].
The goal of this case report is to emphasize the dentist's critical role in the early detection of this rare syndrome through description of the characteristics orodental features of Lubinsky- MacGibbon syndrome in two infants born to consanguineous parents.
Case Report
The first instance was a 16-year-old male patient who arrived to our department complaining from delayed eruption of upper and lower permanent teeth and yellowish staining of erupted teeth after seeking other dental specialties help. When family history was obtained, it was discovered that the parents were consanguineous (first degree cousins), and no health concerns were noticed throughout the prenatal period or childhood. Physical examinations in general were inconclusive. No history of drug use or systemic illness was present. Extra-oral examination was unremarkable.
Intraoral examination (Figures 1A to Figure 1F) revealed permanent mandibular and maxillary first molars have erupted devoid of any cuspal features, lower left first and second molars, unerupted canines , upper first premolars, while erupted teeth showing yellowish discoloration with smooth surface , widely spaced (relative microdontia), nearly flat cusps on erupted posterior teeth suggesting wear of hypoplastic enamel after eruption which result in reduced vertical dimensions during occlusion, decreased anterior overbite , semi-lunar notch in upper right central incisor’s edge. Despite significant attrition, no dental discomfort or sensitivity was obtained during jaw function. On careful soft tissue examination, it revealed generalized Fibrous gingival hyperplasia affecting both arches in a mild degree.
Orthopantomography (OPG) (Figure 1g) revealed enamel hypoplasia of all the teeth. The canines were impacted. Multiple intrapulpal calcification visible in certain permanent teeth's pulp chambers, impacted posterior teeth with dilacerated roots. The predicted radiodensity difference between dentine and enamel is minimized, indicating either a low mineral concentration in enamel or the lack of enamel, respectively. Significant pericoronal radiolucencies were detected around lower impacted molars, characterized by sclerotic borders. For the second permanent molars, an aberrant eruption route is identified that is particularly obvious, with an inverted trajectory toward the mandibular canal and maxillary sinus. Dental follicle hyperplasia appears to be connected with an aberrant eruption route and a lack of eruption. On certain teeth, substantial localized root partial replacement of resorbed dentin by bone has occurred.
Serum electrolytes, calcium, phosphate, urea, creatinine, and alkaline phosphatase levels were all within normal limits, as were renal function tests. No metabolic hard tissue disease involvement confirmed by normal endocrine profile. Although the patient had no history of major illnesses or disorders, these orodental and radiographic findings were strongly suggestive of Lubinsky-MacGibbon syndrome, so he was referred to be evaluated by a nephrology specialist for bilateral medullary nephrocalcinosis to confirm our suspicion. Within a week after our recommendations, patient return to us with abdomen and pelvis’s computed tomography reporting existence of small bilateral medullary nephrocalcinosis with no urinary tract abnormalities (Figure 1H and Figure I) as well as a marvelous nephrological referral’s thanks. Thus, Lubinsky-MacGibbon syndrome was definitively diagnosed based on orodental features mainly and after radiological renal evaluation confirmed the diagnosis, the patient was referred to a nephrologist and clinical geneticist, with the risk of progressive renal failure being considered if it’s ignored and referred to fixed prosthodontics department for dental rehabilitation.
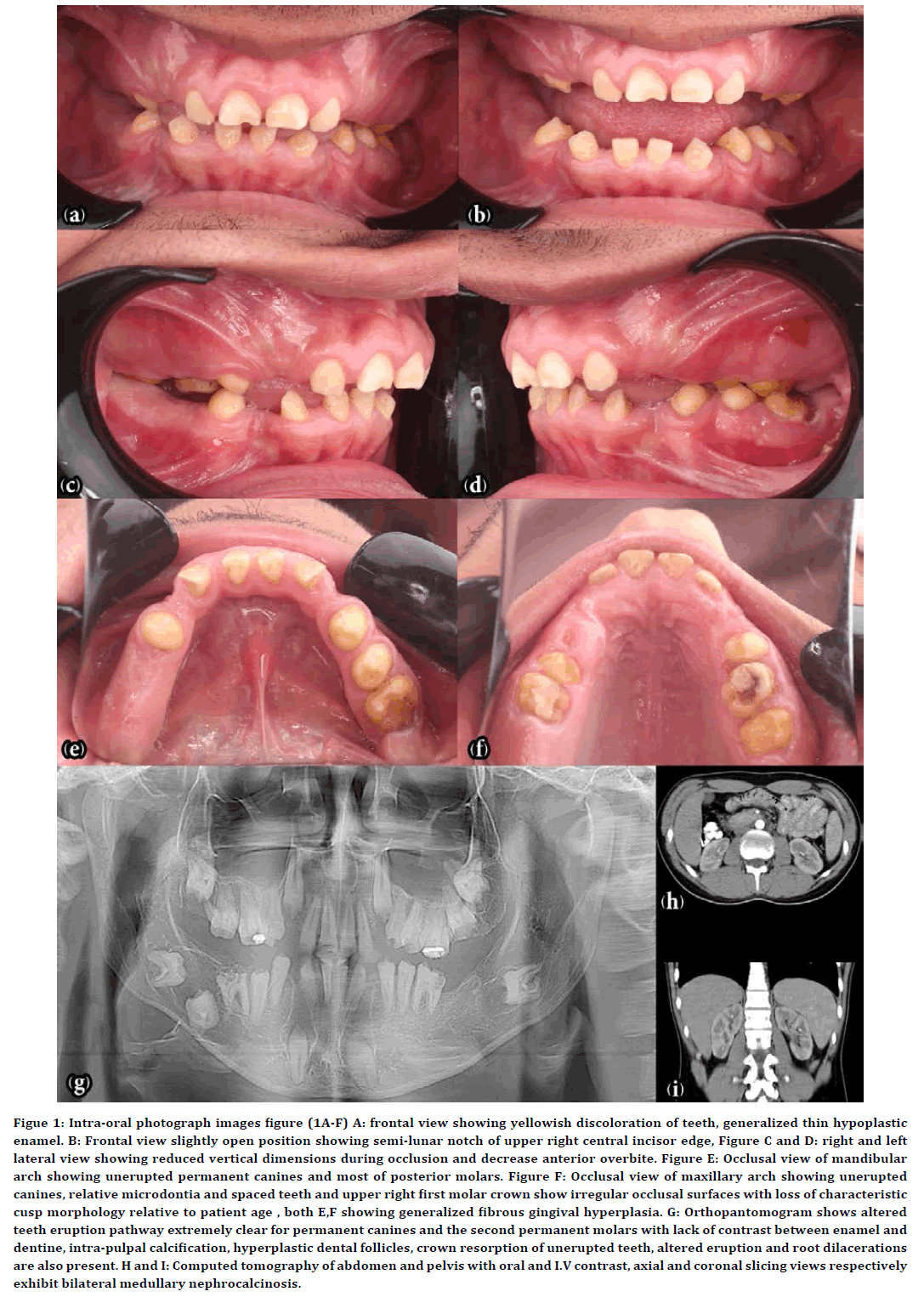
Figure 1. Intra-oral photograph images figure (1A-F) A: frontal view showing yellowish discoloration of teeth, generalized thin hypoplastic enamel. B: Frontal view slightly open position showing semi-lunar notch of upper right central incisor edge, Figure C and D: right and left lateral view showing reduced vertical dimensions during occlusion and decrease anterior overbite. Figure E: Occlusal view of mandibular arch showing unerupted permanent canines and most of posterior molars. Figure F: Occlusal view of maxillary arch showing unerupted canines, relative microdontia and spaced teeth and upper right first molar crown show irregular occlusal surfaces with loss of characteristic cusp morphology relative to patient age , both E,F showing generalized fibrous gingival hyperplasia. G: Orthopantomogram shows altered teeth eruption pathway extremely clear for permanent canines and the second permanent molars with lack of contrast between enamel and dentine, intra-pulpal calcification, hyperplastic dental follicles, crown resorption of unerupted teeth, altered eruption and root dilacerations are also present. H and I: Computed tomography of abdomen and pelvis with oral and I.V contrast, axial and coronal slicing views respectively exhibit bilateral medullary nephrocalcinosis.
Discussion
This case was prepared for our departmental discussion by doing an online search on AI and multiple impacted teeth keywords. One of the most unusual associations of AI and NC has been discovered, with pathological orodental findings analogical to those in this case report as a precautionary measure, she was advised to seek nephrologist help for renal examination which confirm the incidence of this unusual association.
Lubinsky-MacGibbon syndrome is uncommon ailment and few people are aware of its existence, Even among dentists [8].Consanguineous and nonconsanguineous families have previously been shown to have this condition. Thin or missing enamel was seen in all instances, as well as bilateral NC [1,4-7,9-13].While progressive renal failure occurs in a subset of individuals [6,7,10,11]. Some affected individuals developed renal tubular diseases [1,5,9-11].
Some cases reported coexistence of this syndrome with different renal diseases including, but not limited to polycystic kidney disease and inability of the kidneys to get rid of acids from the blood into the urine as usual [9]. In certain circumstances 2 patients died before they reached the age of thirty, one had coronary occlusion while the other developed persistent pyelonephritis [13].
Furthermore, the “common oral presentation” of this syndrome, many uncommon characteristics have been identified in the literature. According to certain researches, hypertrichosis was associated with hearing loss in two patients diagnosed as lubinsky-MacGibbon syndrome. The fact behind loss of hearing is Rain syndrome caused by FAM20C mutation. This may explain the presence of such a feature in lubinsky- MacGibbon syndrome [14].All of these indicating how much is unknown and poorly understood about this syndrome.
The consanguineous marriage of the parents in the present case report suggests an autosomal recessive inheritance.
Even in late childhood or early adulthood, patients with this syndrome may not develop kidney problems until they have had repeated infections of the urinary tract, kidney colic, or have passed a kidney stone [12].
ERS/AIGFS has been recorded in the literature, however it has been referred to as AI, AI with interradicular dentine dysplasia, AI with gingival fibromatosis, AI with odontogenic fibroma-like hamartomas surrounding non-erupted teeth, AI with crown resorption, and AI with unerupted teeth. As of this writing, there have been around 100 reports of ERS-like instances recorded throughout the globe to far. The dental/oral and renal characteristics were only examined in 16 of the patients. ERS has been underestimated in these situations because renal status was not carefully assessed [2].
Conversely, AI is a relatively common disorder that dentists confront and occurs as an isolated trait, or part of a syndrome [15]. The hypoplastic kind of AI is the most often linked to this syndrome out of all the others [16]. As the initial point of contact for these patients, dentists must be able to recognize individuals with ERS and distinguish it from AI so that they are referred for proper renal assessments and genetic counselling [16].
An oral clinical diagnosis of ERS is deemed suitable for inclusion because of the pathognomonic aspects of the disease [2]. In the present case, ERS was suspected based on pathognomonic dental finding.
Nephrocalcinosis (NC), highlighted by radiographs, CT scans, or ultrasound’s increased echogenicity, which is a serious condition that can occur in conjunction with worsening of glomerular function or nephrolithiasis [17]
It is recognized that untreated NC is connected with a high morbidity, despite the fact that the disease is typically asymptomatic. In Lubinsky- MacGibbon syndrome, no predisposing factors such as hypercalcemia and hypercalciuria have been found. On the contrary, Hypocalciuria, low phosphate levels, and proteinuria have all been documented in urine samples [18]. In the present case, Laboratory results, kidney tests, and the patient's endocrine profile are all normal in this instance. So silent NC can lead to the renal functions’ impairment. generalized hypoplastic AI in children acts as a red flag to the dentist to attain complete family history and previous medical records pertaining to the urinary tract and refer them for further testing, such as renal function tests and ultrasonography, to look for the presence of NC. Also, An awareness campaign among nephrologists is needed to promote oral examinations for children with unexplained NC. [19]. Oral and dental conditions are complex to treat except for gingival hyperplasia, for which gingivectomy has been shown to be effective and without recurrence [20,21]. AI has a high morbidity, and people who suffer from it lack confidence and have a worse quality of life, not to mention teeth that don't function or look as they should [22]. The most challenging condition to treat is a lack of eruption, even if dental function and aesthetics are key reasons for seeking professional dental help, Conventional procedures like dental ceramic crowns, for example, can only restore teeth that have already emerged [9]. In the most severe instances, in which several teeth have not erupted, necessitating the need of overdentures, follicle hyperplasia does not permit teeth to erupt, and the removal of primary teeth does not promote their emergence. They've been tried for occlusion with orthodontic traction, but the results were sluggish and variable. Non-erupted teeth challenge dental surgery because of the lack of a universal agreement on their treatment [2].
Conclusion
The orodental features are the first to emerge and the key reasons for which the patient seek professional help, the dentists are usually the first to see affected patients early due to amelogenesis imperfecta and delayed eruption of primary and permanent teeth while oral and maxillofacial surgeons are the second ones after referral for multiple impacted teeth as a result of lack of knowledge regarding this syndrome, the early diagnosis provided by the oral symptoms leads to a better renal prognosis , such patients should be referred to a nephrologist and clinical geneticist to prevent the morbidity and mortality associated with this underestimated entity.
Declaration of Patient Consent
According to the authors' certification, all required patient consent documents have been obtained. These photographs and other clinical data will be published in the journal with the patient's agreement. Those who are being treated are aware that their names and initials will not be made public and that every effort will be taken to keep them private. However, even though their identity is safeguarded, and anonymity is not 100% assured.
Source of Funding
None.
Conflicts of Interest
All authors declare to have no conflict of interest related to this work.
Acknowledgement
I would especially like to thank my family and colleagues for their encouragement as well as top art’s printing service center.
References
- de la Tranchade IN, Bonarek H, Marteau JM, et al. Amelogenesis imperfecta and nephrocalcinosis: A new case of this rare syndrome. J Clin Pediatr Dent 2004; 27:171-175.
- de la Dure-Molla M, Quentric M, Yamaguti PM, et al. Pathognomonic oral profile of enamel renal syndrome (ERS) caused by recessive FAM20A mutations. Orphanet J Rare Dis 2014; 9:84.
- Aldred MJ, Savarirayan R, Crawford PJ. Amelogenesis imperfecta: A classification and catalogue for the 21st century. Oral Dis 2003;9:19-23.
- Hall RK, Phakey P, Palamara J, et al. Amelogenesis imperfecta and nephrocalcinosis syndrome. Case studies of clinical features and ultrastructure of tooth enamel in two siblings. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1995; 79:583-92.
- Hunter L, Addy LD, Knox J, et al. Is amelogenesis imperfecta an indication for renal examination? Int J Paediatr Dent 2007; 17:62-5.
- Mac Gibbon D. Generalized enamel hypoplasia and renal dysfunction. Australian Dent J 1972; 17:61-63.
- Dellow EL, Harley KE, Unwin RJ, et al. Amelogenesis imperfecta, nephrocalcinosis, and hypocalciuria syndrome in two siblings from a large family with consanguineous parents. Nephrol Dial Transplant 1998; 13:3193-6.
- Reddy P, Aravelli S, Goud S, et al. Amelogenesis Imperfecta with Nephrocalcinosis: A rare association in siblings. Cureus 2019; 11:e5060.
- Elizabeth J, Lakshmi Priya E, Umadevi KM, et al. Amelogenesis imperfecta with renal disease: A report of two cases. J Oral Pathol Med 2007; 36:625-628.
- Lubinsky M, Angle C, Marsh PW, et al. Syndrome of amelogenesis imperfecta, nephrocalcinosis, impaired renal concentration, and possible abnormality of calcium metabolism. Am J Med Gen 1985; 20:233-43.
- Fu XJ, Nozu K, Goji K, et al. Enamel-renal syndrome associated with hypokalaemic metabolic alkalosis and impaired renal concentration: a novel syndrome? Nephrol Dial Transplan 2006; 21:2959-2562.
- Martelli-Júnior H, dos Santos Neto PE, de Aquino SN, et al. Amelogenesis imperfecta and nephrocalcinosis syndrome: A case report and review of the literature. Nephron Physiol 2011; 118:62-65.
- Paula LM, Melo NS, Silva Guerra EN, et al. Case report of a rare syndrome associating amelogenesis imperfecta and nephrocalcinosis in a consanguineous family. Arch Oral Biol 2005; 50:237-42.
- Pêgo SPB, Coletta RD, Dumitriu S, et al. Enamel-renal syndrome in 2 patients with a mutation in FAM20 A and atypical hypertrichosis and hearing loss phenotypes. Oral Surg Oral Med Oral Pathol Oral Radiol 2017; 123:229-34.
- Dourado MR, Dos Santos CRR, Dumitriu S, et al. Enamel renal syndrome: A novel homozygous FAM20A founder mutation in 5 new Brazilian families. Eur J Med Gen 2019; 62:103561.
- Kirzioglu Z, Ulu KG, Sezer MT, et al. The relationship of amelogenesis imperfecta and nephrocalcinosis syndrome. Med Oral Patol Oral Cirugia Bucal 2009; 14:e579-82.
- Evan AP, Unwin RJ, Williams JC. Renal stone disease: A commentary on the nature and significance of Randall's plaque. Nephron Physiol 2011; 119:p49-53.
- Kala Vani SV, Varsha M, Sankar YU. Enamel renal syndrome: A rare case report. J Indian Soc Pedod Prev Dent 2012; 30:169-72.
- Kantaputra PN, Kaewgahya M, Khemaleelakul U, et al. Enamel-renal-gingival syndrome and FAM20A mutations. Am J Med Gen Part A 2014; 164a:1-9.
- Martelli-Júnior H, Bonan PR, Dos Santos LA, et al. Case reports of a new syndrome associating gingival fibromatosis and dental abnormalities in a consanguineous family. J Periodont 2008; 79:1287-96.
- Roquebert D, Champsaur A, Gil del Real P, et al. Amelogenesis imperfecta, rough hypoplastic type, dental follicular hamartomas and gingival hyperplasia: Report of a case from central America and review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2008; 106:92-98.
- Hashem A, Kelly A, O'Connell B, et al. Impact of moderate and severe hypodontia and amelogenesis imperfecta on quality of life and self-esteem of adult patients. J Dent 2013; 41:689-94.
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Author Info
Almoataz Bellah Abdullah Tawfiq Abdel-Bari*, Ahmed Abd El-Latif Mosleh and Khaled Abd El-Hamid Saad
Department of Oral and Maxillofacial Surgery, Tanta University, EgyptReceived: 26-Feb-2022, Manuscript No. JRMDS-22-55639; , Pre QC No. JRMDS-22-55639 (PQ); Editor assigned: 01-Mar-2022, Pre QC No. JRMDS-22-55639 (PQ); Reviewed: 14-Mar-2022, QC No. JRMDS-22-55639; Revised: 21-Mar-2022, Manuscript No. JRMDS-22-55639 (R); Published: 28-Mar-2022
