Review Article - (2022) Volume 10, Issue 8
Role of Herd Immunity in COVID-19
Swarupa Chakole, Himabindu Reddy* and Ashok Mehendale
*Correspondence: Himabindu Reddy, Department of Community Medicine, Jawaharlal Nehru Medical College, Datta Meghe Institute of Medical Sciences, Wardha, Maharashtra, India, Email:
Abstract
Background: With the rise in cases of COVID-19, the concept of herd immunity came into play which is expected to play a very important role in the control of this pandemic. For herd immunity to work we require only a part of the entire population to be immune which can be either by vaccination or natural infection. Although we are exactly not sure about the lasting impact that these antibodies will have on us or about the re activation of virus, as of now this remains the best option with us to combat the disease process. The effectively of vaccine, virus transmission, and the level of pre-existing immunity along with other factors play a very important role in determining the time required to reach herd immunity. With this we can prevent the immune compromised or individuals with other co morbid conditions predisposed to this disease as in them the disease process would be fast and response to treatment slow or undetermined. The main element of vaccine production depends on the population behaviours along with the pathogen. It is on the basis of these criteria that we analyse the study between herd immunity and COVID-19. As we know now that this disease spreads as the healthy individuals come in contact with infected individuals therefore the most effective way to prevent it is by maintaining social distancing. So with the herd immunity coming into play the transmission of the disease is stopped and we can achieve our aim of preventing the spread of the disease by making just a part of the population immune.
Objective: The purpose is to review the article related to attainment of herd immunity in COVID-19
Methodology: For the review article we gathered the data from various data bases like PubMed, Google scholar, and science direct and other websites involving searches such as herd immunity, vaccines, natural immunity, COVID-19.
Result: After reviewing the article we can say that herd immunity plays a very important role in controlling the transmission of COVID-19
Conclusion: After looking at all the perspectives although we conclude that herd immunity will play the leading role in the control of transmission but it is a very challenging task that would take a lot of time to become effective, till then measures such as social distancing, hygiene practices and sanitation should be considered to stop disease transmission.
Keywords: Vaccine, COVID-19, Herd immunity, Infection, Immuno compromised
https://marmarisinvestments.com
https://realestateinmarmaris.com
https://balloonsdocia.com
https://cappadociahotairballoon.org
Introduction
Herd Immunity and COVID-19
The history has always seen the occurrence of pandemics creating havocs on the lives of people affected, along with the devastating impacts that last forever. Whether it is plague (1720), cholera outbreak (1820), Spanish flu (1920) or the emergence of SARS-CoV-2 (COVID-19) at the end of 2019 reported for the first time in wuhan, china [1]. We know six species of human coronavirus till date in which each species is further divided into two different strains. The genera comprises of alpha, beta, gamma and delta [2]. Out of these the beta gene belonging to the family of positive sense single stranded RNA also known as SARS-COV-2 is responsible for the 2019 pandemic and causes severe acute respiratory syndrome. It transmits through direct contact with the infected individuals, droplet infection and via faeco oral route [3,4]. Other factors which play an important role in disease transmission are social distancing, hygiene maintenance, climatic changes and the pre-existing immunity in the individuals [5]. As per the suggestive evidences the virus spread from the seafood market in wuhan, china where animals like bats, birds, frogs, snakes are sold, there has been a possibility since very beginning that bats have been the source of transmission as they are considered to be the reservoir host [6,7].
Luterature Review
Pathophysiology
Like every other disease viruses enter the host cells and use the host machinery for their reproduction and metabolism. They generate a specific cellular protein which interferes with the host immune system to carry out a normal physiological response or give a hyper response in return to these proteins. In the same process the binding of the various proteins produced by the virus to the host cells cause an increase in blood pressure, inflammatory reactions along with fibrosis [8,9]. A protein produced by the virus binds to ACE-II and predisposes to hypertension and diabetes [10,11]. The disease has a more debilitating impact on elderly, immune compromised states and people with other co-morbid conditions [12]. Depending on the age, immune status and patient care, the time duration between the onset of symptoms and death lies in a range of 5-42 days approximately with a median of 14 days [13]. Herd immunity attained via vaccines is pathogen specific and for SARS CoV-2, a value of nearly 65-68% is estimated to be required for the establishment of herd immunity [14]. (If the value of R0 is 3). The transmission of the infection in a population can be effectively evaluated with the concept of herd immunity. As already discussed earlier, even if a limited number of people in a population are immune against the pathogen, the outbreak won’t occur as even if an individual harbours the pathogen, the contact between the diseased and the susceptible individual is broken which would confer herd immunity to the population [15]. With herd immunity the transmission rate reduces, in other words the number of secondary cases in a population that would have occurred by a primary case stands at a low level now, forming the baseline of this concept [16]. It is a form of indirect protection to immune compromised, people with chronic debilitating condition, children, infants and pregnant women [12]. In simple words the threshold of the herd immunity is a critical proportion of a population that have to be immunized so that the epidemic can be eliminated. This concept has been successfully used for the eradication of small pox in 1970’s by reducing the transmission rates. Other immunization programs such as control of measles, mumps, rubella and pertussis also work on the same principle [17]. More emphasis needs to be laid on vaccines that work on the reduction in transmission rather than those which are work only to reduce the disease progress so as the outcome is increased. Vaccines should be cost effective, with minimum side effects, should be applicable and accessible to a wide range of population and cover wider age groups. Social motivations need to be provided to people especially in rural areas, so that they take part in the mass vaccinations programs and our aim of establishment of herd immunity is achieved [16]. They should be informed about the vaccine benefits and their myths should be resolved about the side effects which the vaccine has and the vaccine safety should be addressed. As in India the rural population acquires a major part whose behavioural response to the epidemic determines the outcome. The feasibility of herd immunity: it depends upon the availability and distribution of the vaccine, number of people, who get vaccinated, effectively of the vaccine. Pandemic has resulted into a large proportion of the population affected the disease nearly 3.5 million clinically confirmed cases of COVID-19 and has caused about 2,50,000 deaths worldwide as of 4th may, 2020 [18]. The disease process continues and would be infecting so many people around as I write down this article further changing the lives of people for once and forever. Presently, we are not certain about the effectiveness and the duration of these of these trials and exact safety and efficacy levels that these studies would confer. So, we go with the estimate of the clinical trials of vaccine which take around 12-20 months approximately. While these trials are on-going meanwhile the establishment of herd immunity through natural infection should be taken into consideration and worked upon as it is equally important and can significantly reduce the disease transmission. The transmission can be suppressed by introducing the control measures (mainly social distancing, self-isolation, usage of masks and sanitizers, hygiene practices) that reduces the chances of endogenous transmission and further preventing re infection. From here on we will understand the concept of herd immunity with the calculation of R0 (the basic reproduction number) which tells us about the virus infectivity. With the spread of the SARS-CoV-2, many studies were carried out on different levels according to which the basic reproduction number of the virus ranges in between 2 to 6 [19]. If we take the example of a cohort study conducted in Wuhan, China with 426 confirmed cases, R0 was approximately around 2.3 which imply that each infected individual gives rise to 2.3 other infections on an average [20]. With the recent estimates the value of R0 stands at 5.7 which clearly depict the difficulty in determining the exact value of R0 in the on-going pandemic [21]. With this base we understand that if R0 is higher the transmission is high and with a low R0 the transmission rate is less. As per one study Out of the various studies done on COVID-19 says that the virus would remain in the surrounding with us forever only the difference would be that the devastating impact of it on the surrounding would be reduced or that people would become accustomed to it, and the response of the various individuals would differ.
Objective
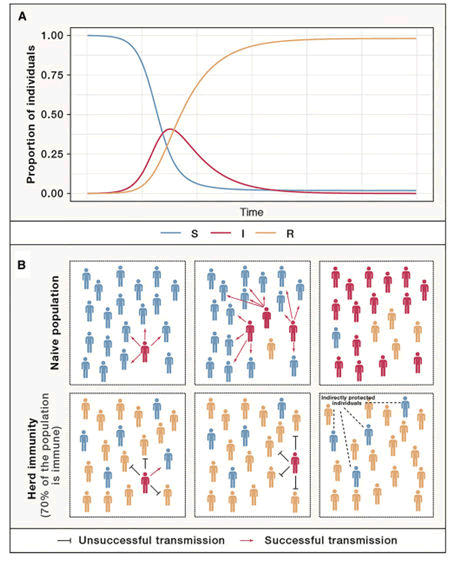
The purpose of this article is to make people aware about the benefits and the concept of herd immunity in disease transmission and control. The resources required and the implementations to be carried out in order to achieve the herd immunity in less duration and protect the community from the devastating impacts of the disease. The most important factors required to understand herd immunity include infectivity of the pathogen, the route of transmission, along with the immune status of the individual [22]. Herd immunity is the resistance of a group or population to attack by a disease to which a large proportion of the group is immune, thus reducing the chances of an infectious individual to make effective contact with a susceptible host. It can be achieved by either vaccination or by natural infection with the pathogen [23]. When an infected individual is introduced into the community various possibilities can occur, the most predicted one is that the pathogen will continue to multiply and spread to the susceptible host in the community in an unchecked manner, infecting them, if the host does not have any immunity against the pathogen. But if the same pathogen is introduced in a community where a proportion of people have immunity against the pathogen the spread or the transmission of the pathogen reduces and therefore less people are infected. So, if the predisposed individual in a population is reduced, if the hosts are immune to the pathogen, the pathogen cannot be transmitted and hence there is a decline in prevalence. Herd immunity threshold refers to a point at which the proportion of the susceptible individuals falls below the threshold needed for transmission [12]. Herd immunity becomes effective above this level of immunity and the individuals, who were earlier predisposed to get infected with the pathogen, are now at a much lower risk (Figure 1) [19].
Figure 1: Herd immunity.
Discussion
As discussed earlier the parameter determining the herd immunity threshold is R0 (the basic reproduction number). When an individual infected with the pathogen is introduced into a susceptible community spread of the disease occurs to the susceptible hosts, these are known as secondary infections and the average number of these secondary infections is taken as the R0 values. Suppose if the given value of R0 is 5, this implies that during an infectious period one infected host will result into spread of the infection to 5 other people, (the assumption is that there is no immunity in the population under study). The herd immunity threshold determination is done by a mathematical formula 1-1/R0. (So if we take the value of R0 as 5, the herd immunity threshold comes out to be 0.8) [12]. With the above study we come to know that as the value of R0 increases the spread of the pathogen is larger and to stop this transmission a greater number of people need to be immune. Reproduction number is another important parameter to determine the level of immunity in a population denoted by Re or Rt. The average number of secondary cases which occurred from a single index case over a specific infectious period in a partly immune population determines the value of Re [9]. As R0 takes into consideration a completely susceptible population with no immunity while the Re calculation is based on a population which is partly immune, the values of these two vary depending on the present immune status of the population, which changes when an outbreak occurs or when there is administration of mass vaccinations. The main goal of vaccination programs is to bring the value of Re below 1 [19].
This value can be achieved only when the herd immunity threshold is exceeded by the population under study. With these levels the spread of the pathogen in the community is not maintained and there is decline in the number of individuals infected with the disease in the population.
Establishment of herd immunity
The establishment of herd immunity depends on natural infection and vaccination. The main purpose of these should be to prevent the transmission of the disease along with the disease progress. After the attainment of herd immunity threshold, the strength and duration of the acquired immunity should be used to determine the efficacy. Clinical manifestations cannot be considered as an indicator of transmissibility as even asymptomatic hosts can be highly infectious and can be a contributing factor in disease progress and the epidemic spread. In certain diseases such as measles lifelong immunity is acquired, in such cases the effectiveness of herd immunity is high which can avert the spread of the pathogen. While in some other diseases such as rotavirus and pertussis, the immunity decreases with time. This leads to the decrease in effectiveness of the herd immunity and a possibility of outbreaks in future. The other factor that plays an important role is the evenly distribution of immunity in a population [19]. Suppose if the immunity is not evenly distributed and there is a cluster of population which is not immunized and they come in contact with other people, in that case these individuals can cause local outbreaks even if the immunized individuals in a population exceed the herd immunity threshold. The disease spread needs to be controlled at the local level which can be achieved by awareness among the public, health measures and the actions taken by community as a whole. Considering the above factors our next aim remains to undertake 1) Mass vaccination programs effectively and enrolling a large number of people 2) Natural immunity of the population over time with the virus. Hence, although we aim at achieving herd immunity that would decline the disease progress we know that this is something which would take a lot of time with all the factors working together positively in a particular direction and would require the participation of health workers, government, the organisations working at both national and international levels, the administration, and most importantly the population under risk, the inputs by all these people will determine the output. For now the most that we can do is to follow all the norms such as social distancing, maintaining hygiene, usage of mask and hand sanitizers to combat the spread of the disease progress [18,24]. And special arrangements should be made to provide support to public health and medical systems (so as to reduce the burden on healthcare system).
Conclusion
The development of vaccine remains to be the most important factor to control COVID-19 spread. But with the changing strains of the virus and the variations in the climatic conditions of various areas the task of attainment of herd immunity appears to be a difficult one/tedious and time consuming process. Once we reach a point at which a proportion of the population becomes immune which prevents the transmission of infection, there will be a decline in the number of affected cases, henceforth a decline in the outbreak. Therefore the most important factors which need to be taken care of include the population, the climatic variations and the level of the pre-existing immunity in the community. However such process takes time and a large number of people would be infected during this, a part of which will succumb to disease. The vulnerable group in the society should be given special attention. Along with providing the hospitals with more funds, making the availability of medications, oxygen cylinders easily available to the people along with cost effectively so that we don’t lose any life due to unavailability of resources. Although we do not know the exact outcome that we will get after doing this entire procedure as there would be different constraints present at different levels that would hamper our outcome but for now as we do not have any other option that is strongly suggestive to limit the disease we go forward with the approach of herd immunity as it has benefited us in past and is expected to play a key role now as well. With all the resources put together and with people working together in a particular direction by following all the norms and guidelines, this difficult task can be attained. And for now this is the only hope left with us, in spite of the fact that we do not know the exact time that it would take or the exact level of effectiveness that would be present in an individual or a community as a whole. So with working on this together, meanwhile we need to follow all the safety guidelines so that the chain can be broken and we come back to our normal lives which for now appears to be far away but will definitely be possible in near future.
References
- Sisay T, Tolessa T. COVID-19 Pandemic: A Compressive Review on Gender, Herd Immunity, and Physiological Mechanisms. Risk Manag Health Policy 2020; 13:2963-2974.
- Zhang H, Kang Z, Gong H, et al. The digestive system is a potential route of 2019-nCov infection: a bioinformatics analysis based on single-cell transcriptomes. BioRxiv 2020.
- He X, Lau EHY, Wu P, et al. Temporal dynamics in viral shedding and transmissibility of COVID-19. Nat Med 2020; 26:672-675.
- Van Damme W, Dahake R, Delamou A, et al. The COVID-19 pandemic: diverse contexts; different epidemics-how and why?. BMJ Glob Health 2020; 5:003098.
- Zhu N, Zhang D, Wang W, et al. A novel coronavirus from patients with pneumonia in China. N Engl J Med 2019z
- World Health Organization. Coronavirus disease (COVID-19) Weekly Epidemiological Update and Weekly Operational Update. Coronavirus disease 2019 (COVID-19) situation report. 2022.
- Zhou P, Yang X-L, Wang X-G, et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 2020;1–4.
- Jia HP, Look DC, Shi L, et al. ACE2 receptor expression and severe acute respiratory syndrome coronavirus infection depend on differentiation of human airway epithelia. J Virol 2005; 79:14614–14621.
- Monteil V, Kwon H, Prado P, et al. Inhibition of SARS-CoV-2 infections in engineered human tissues using clinical-grade soluble human ACE2. Cell 2020; 181:905–913.
- Turner AJ, Hiscox JA, Hooper NM. ACE2: from vasopeptidase to SARS virus receptor. Trends Pharmacol Sci 2004; 25:291–294.
- Anderson RM, May RM. Vaccination and herd immunity to infectious diseases. Nature 1985; 318:323–329.
- Wang W, Tang J, Wei F. Updated understanding of the outbreak of 2019 novel coronavirus (2019-nCoV) in Wuhan, China. J Med Virol 2020; 92:441–447.
- Kadkhoda K. Herd Immunity to COVID-19. Am J Clin Pathol. 2021; 155:471-472.
- Fontanet A, Cauchemez S. COVID-19 herd immunity: where are we?. Nat Rev Immunol 2020; 20:583-584.
- Sisay T, Tolessa T. COVID-19 Pandemic: A Compressive Review on Gender, Herd Immunity, and Physiological Mechanisms. Risk Manag Healthc Policy 2020; 13:2963-2974.
- Centers for Disease Control and prevention (CDC). Prevention of acquired immune deficiency syndrome (AIDS): report of inter-agency recommendations. MMWR Morb Mortal Wkly Rep 1983; 32:1–125.
- Brett TS, Rohani P. COVID-19 herd immunity strategies: walking an elusive and dangerous tightrope. medRxiv2020; 117:25897-25903.
- Randolph HE, Barreiro LB. Herd Immunity: Understanding COVID-19. Immunity 2020; 52:737-741.
- Li Q, Guan X, Wu P, et al. Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia. N Engl J Med 2020; 382:1199–1207.
- Sanche S, Lin YT, Xu C, et al. High contagiousness and rapid spread of severe acute respiratory syndrome coronavirus 2. Emerg Infect Dis 2020;26:1470-1477.
- Dong M, He F, Deng Y. How to Understand Herd Immunity in the Context of COVID-19. Viral Immunol 2021; 34:174-181.
- Kien VD, Van Minh H, Giang KB, et al. Trends in childhood measles vaccination highlight socioeconomic inequalities in Vietnam. Int J Public Health 2017; 62:41-49.
- Kadkhoda K. Herd Immunity to COVID-19. Am J Clin Pathol 2021; 155:471-472.
- D Souza G, Dowdy D. Whatâ??s Herd Immunity and How Can We Achieve It with COVID-19. Johns Hopkins School of Public Health Expert Insights. 2020.
Author Info
Swarupa Chakole, Himabindu Reddy* and Ashok Mehendale
Department of Community Medicine, Jawaharlal Nehru Medical College, Datta Meghe Institute of Medical Sciences, Wardha, Maharashtra, IndiaCitation: Swarupa Chakole, Himabindu Reddy, Ashok Mehendale, Role of Herd Immunity in Covid-19, J Res Med Dent Sci, 2022, 10 (8): 000-000.
Received: 30-May-2022, Manuscript No. JRMDS-22-49721; , Pre QC No. JRMDS-22-49721; Editor assigned: 01-Jun-2022, Pre QC No. JRMDS-22-49721; Reviewed: 14-Jun-2022, QC No. JRMDS-22-49721; Revised: 03-Aug-2022, Manuscript No. JRMDS-22-49721; Published: 12-Aug-2022