Research - (2021) Volume 9, Issue 4
Role of Trans Vaginal Sonography and Magnetic Resonance Imaging in Perimenopausal Bleeding
*Correspondence: Prabakaran M, Department of Radio Diagnosis, Sree Balaji Medical College & Hospital, Bharath Institute of Higher Education and Research, India, Email:
Abstract
To differentiate and characterize uterine and ovarian lesions based on MRI and TVS findings. To identify organ of origin of uterine and ovarian lesions based on MRI and TVS findings. To diagnose abnormalities which have a difficulty in detection with TVS? MRI is found to be more precise and many a times gold standard in comparison to TVS to characterize, localize and evaluate the number of lesions in benign as well as malignant pelvic pathologies.
Keywords
Gynecology, Ovarian lesions, Hyperplasia
Introduction
Menstruation is a process of cyclical vaginal bleeding in response to ovarian hormones. Abnormal uterine bleeding is any variation in the normal menstrual cycle and includes changes in frequency, duration and amount of blood loss during or in between the cycles. Menstrualdisorders are the main cause affecting 50% of perimenopausal age group patients. There complaints may significantly affect the quality of life and lead to surgical intervention. A detailed history and physical examination can often detect the cause of abnormal uterine bleeding and direct the need for further investigation and treatment [1-3].
The international Federation of Gynecology and Obstetrics worked up on menstrual disorders and has proposed a classification system (PALM-COEIN) for the causes of abnormal uterine bleeding in women. The PALM includes conditionsthat are referred to as the structural causes that could be evaluated and diagnosed on imaging and/or biopsy. The COEIN refers tothe underlying medical disturbances that could result in abnormal uterine bleeding. PALMCOEIN includes polyp, adenomyosis, leiomyoma, malignancy and hyperplasia, coagulopathy, ovulatory dysfunction, endometrial, iatrogenic and not yet classified [4].
Among the imaging modalities used today including transvaginal ultrasound, colour Doppler, hysterosonosalphingography, computed tomography, magnetic resonance imaging to determine the mass lesion, trans abdominal ultrasound is the imaging modality of choice [5,6]. For appropriate treatment, definitive characterization of lesion is important. Thus, a preoperative diagnosis is always important to determine the treatment of choice. If the endometrial surface circumference is more than 50 % in case of sub mucosal fibroid it can be resected hysteroscopically rather than laparoscopic ally. Depending upon the number and site of lesion in case of intramural fibroids, choice is made between laparoscopy and hysterectomy. It helps in identifying the extent of the lesion by various measurements like size and circumference and also the need for exact location[7].
Upto a specific degree, Transvaginal Ultrasonography aids in portraying the lesion. But it is highly dependent on the skill of the operator and a couple of lesions may get away from the field of view occasionally. A standout among the most common disorders in Gynaecology is adnexal masses. Adnexal components include ovary, fallopian tubes broad ligament and associated blood vessels and nerve structures. Two- third of the cases include ovarian tumours which introduce and present itself as a challenge to most of the practitioners. Imaging of adnexal masses is required and is essential in diagnosing amongst malignant and benign lesions so as to choose the appropriate treatment[8].
In this study, detailed evaluation of uterine mass lesions like location, size, number, measurements, degenerative changes within the lesions, extent of the lesion is performed using Transvaginal ultrasound and correlated with MRI. Final diagnosis by imaging is compared with histopathological reports wherever it was available. Comparisons were made between the three modalities for 1) Detection and sensitivity of the lesions and 2) Characterization & differentiation between different lesions.
Materials and Methods
A prospective study was done 40 patients with suspected uterine and adnexal masses. All patients were subjected to TVS and MRI examination. Final correlation with histopathology was done wherever it was acquired.
Method of Collection of Data
• Detailed clinical history and consent were taken from the patients or their attenders. TVS was performed on Siemens Acuson 2000 transvaginal transducer. The TVS images were evaluated.
• Magnetic resonance imaging of pelvis was performed with HITACHI APERTO machine. A pelvic phased array coil was used in most cases; in cases where lesions were large, a body coil was used for better coverage. The following sequences were obtained:
1. Axial TI-weighted spin echo images from the renal hilum to the symphysis pubis (TR/TE 400-640 ms/10-14 s, slice thickness 5-8 mm, gap 1-2 mm, field of view 24-38 cm, NEX 1-2, matrix 256x192-256.
2. Axial T2- weighted fast spin echo images of the pelvis (TR/ TE 4000-6000 ms/90-110 ms effective, echo train length 8, slice thickness 5-7 mm, gap 1-2 mm, field of view 24-38 cm, NEX 2, 512x256 matrix).
3. Sagittal T2-weighted fast spin echo images from one femoral head to the other (TR/TE 4000-6000 ms/90-110 ms, echo train length 8, slice thickness 5-7 mm, gap 1-2 mm, field of view 24-32 cm, NEX 2, 512x256 matrix).
Materials
• The main source of data for the study is patients from Sree Balaji Medical College, Chrompet.
• All patients referred to the department of Radiology with clinically suspected uterine and adnexal lesions will be subjected for the study.
Study tools
• Socio-demographic details.
• MRI evaluation of the patient correlated with TVS and compared with histopathology whenever possible.
Inclusion Criteria
• All patients with clinically suspected uterine and adnexal lesions of all age groups
• All patients referred to the department of radiology with clinically suspected uterine and adnexal lesions was subjected for the study.
• The patients were evaluated for pelvic lesions focusing on uterine, ovarian and cervical lesions in which TVS and MRI was done and correlated with HPE/surgerywherever necessary.
Exclusion criteria
• Patients of low socioeconomic status who didn’t agree to be a part of study.
• Patients who were afraid of closed spaces.
• Patients inculcated with metallic bioimplants and grafts.
• Unmarried women were not considered for TVS.
Results
Table 1 shows that among 40 females majority of them were in pre menopause period 25 (62.5%) and the rest in the post menopause period 15 (37.5%). It is represented in Bar chart (Figure 1).
| Frequency | Percent | |
|---|---|---|
| Pre menopause | 25 | 62.5 |
| Post menopause | 15 | 37.5 |
| Total | 40 | 100 |
Table 1: Distribution of Pre and Post menopause study participants.
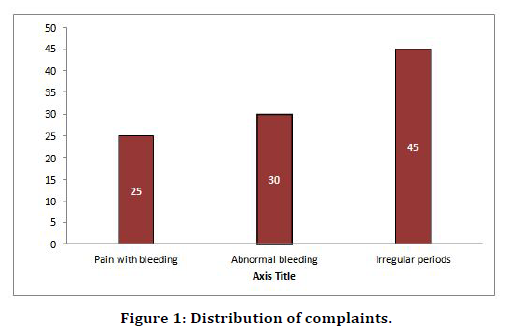
Figure 1. Distribution of complaints.
Table 2 explains that among 40, majority were diagnose fibroids 15 (35.0%), adnexal lesions 11 (27.5%), carcinoma of cervix 5 (12.5%), endometrial lesions 5 (12.5%) and adenomyosis 4 (10.0%).
| Number of Cases | Frequency | Percent |
|---|---|---|
| Fibroids | 14 | 35 |
| Adenomyosis | 4 | 10 |
| Carcinoma of cervix | 5 | 12.5 |
| Adnexal lesions | 11 | 27.5 |
| Endometrial lesions | 6 | 15 |
| Total | 40 | 100 |
Table 2: Distribution of cases.
Table 3 shows that out of 8 samples MRI and HPE picked all 5 cases of ca cervix. The true positives were 5 and true negatives were 3. There is significant association detected.
| Ca Cervix HPE | |||
| MRI | Present | Absent | Total |
| Present | 5 | 0 | 5 |
| Absent | 0 | 3 | 3 |
| Total | 5 | 3 | 8 |
Table 3: Comparison of Ca Cervix of MRI with HPE.
T2 sagittal section of MRI pelvis shows hyper intense areas within the thickened functional zone representing cystic changes of adenomyosis (Figure 2). T1 sagittal section of MRI pelvis shows heterogeneous lesion in cervix (Figure 3). Figure 4 shows T2 sagittal section of MRI pelvis shows heterogeneous intensity within the Endometrium invading the myometrium in the anterior wall. Figure 5 shows that among 11 patients TVS diagnosed 4 as Complex Adnexal Cysts, 3 as Dermoid, 2 as Simple ovarian Cyst, 1 as hemorrhagic Cyst and 1 as Possibly hydrosalpinx and MRI diagnosed 3 as Complex Adnexal Cysts, 3 as Dermoid, 2 as Simple ovarian cysts, 2 as hemorrhagic cyst and 1 as hydrosalpinx. T2 axial section of MRI shows well defined hypo intense lesion on anterior wall of myometrium (Figure 6).
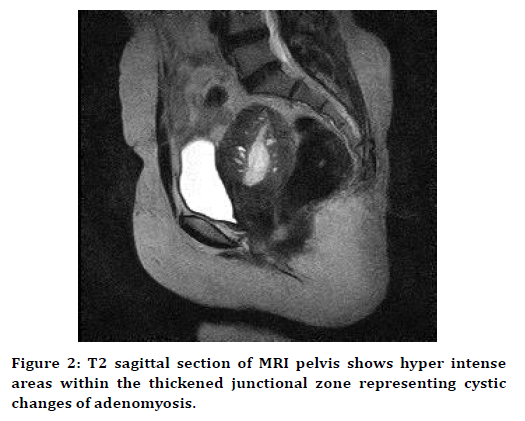
Figure 2. T2 sagittal section of MRI pelvis shows hyper intense areas within the thickened junctional zone representing cystic changes of adenomyosis.
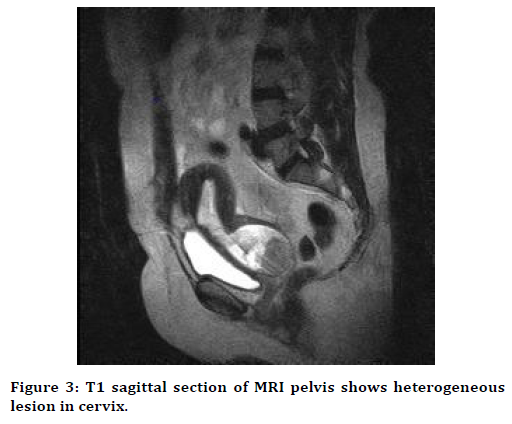
Figure 3. T1 sagittal section of MRI pelvis shows heterogeneous lesion in cervix.
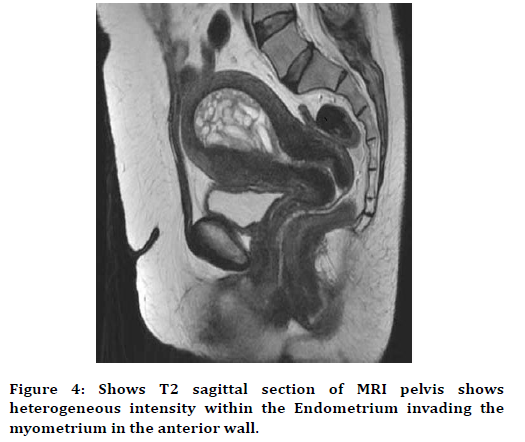
Figure 4. Shows T2 sagittal section of MRI pelvis shows heterogeneous intensity within the Endometrium invading the myometrium in the anterior wall.
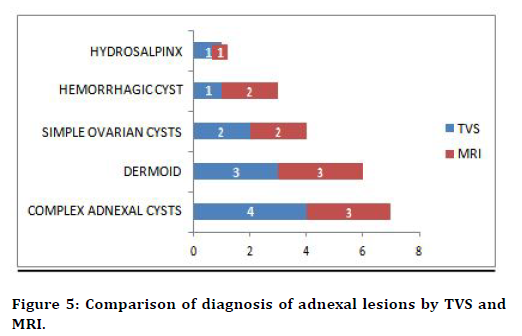
Figure 5. Comparison of diagnosis of adnexal lesions by TVS and MRI.
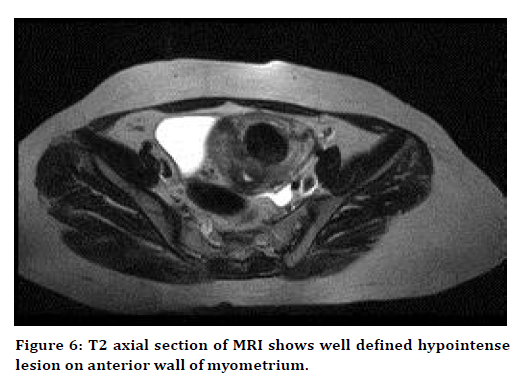
Figure 6. T2 axial section of MRI shows well defined hypointense lesion on anterior wall of myometrium.
Discussion
TVS and MRI was performed in 40 patients who were referred to the department of radiology with clinically suspected uterine and adnexal lesions. These patients were later evaluated for uterine, ovarian and cervical lesions, and the findings were correlated. Both premenopausal and post-menopausal women were subjected to the study. In our study it was noted that among 40 participants majority of them were in the age group of 35-45 years : 27 patients (67.5%) followed by 45-55 years : 5 patients(12.5%) and 55-65 years : 8 patients(20%) [9].
About 62.5% of the patients were in the premenopausal group and 37.5% of the patients in the postmenopausal age group. Most of these patients belonged to reproductive age group since majority of these benign lesions are more commonly seen in this age group. This is highlighted by VG Padubidri, Shirish N Daftary, et al in their study[10].
Out of 40 patients in our study 10 patients complained of pain with bleeding (25%), 12 patients complained of abnormal uterine bleeding (30%) and 18 patients complained of irregular periods (45%), few had combination of these symptoms but the above mentioned were the most common complaints[11].
All the patients in our study were sub-grouped into 5 categories ; based on the underlying pathologies: 1) Fibroids–14 patients (35%) 2) Adenomyosis–4 patients (10.0%) 3) Carcinomacervix -5 patients (12.5%) 4) Adnexal lesions–11 patients (27.5%) 5) Endometriallesions–6 patients (7.6%)[12].
On MRI T1 weighted sequences, 5 lesions out of 6 lesions showed isointense signal (83.3%) and 1 lesion showed hyperintense signals (16.7%). On T2 weighted sequences 1 out of 6 lesions showed heterogenous intensity and 1 lesion showed hypointense signal intensity (16.7%) and 4 patients showed hyperintense signal intensity (66.6%).
In our study only one case of hydrosalpinx was diagnosed by MRI but TVS diagnosed it as complex adnexal lesion. It was difficult to confirm the diagnosis due to presence of multiseptated anechoic lesions which had both complete and incomplete compartments variedly. In MRI, the cases were easily identified with the lesions appearing hyperintense in T2 weighted images and hypointense in T1 weighted images[13]
Sugimura et al. did a study among 35 women with endometriosis and concluded that diagnostic accuracy was improved with addition of fat saturated images. So usage of conventional images along with fat saturated images is suggested in assessment of endometriosis for better accuracy [14].
Patel et al did a study to quantify the likelihood ratio of the sonographic features and experienced radiologist assessment to diagnose hemorrhagic cysts and come to a certain conclusion in coming to a diagnosis via ultrasound. Two experienced radiologists were selectedwho were unaware of the patient’s clinical history. Using a standardized checklist for each mass, each sonologist observed certain features which included the presence of fibrin strands, a retracting clot, septations, and wall irregularity on 30 hemorrhagic cysts. The first sonologist diagnosed 25 cases correctly with 1 false positive, 2 false negatives and 3 indeterminate cases[15-19].
The second sonologist diagnosed 24 cases correctly with 1 false positive, zero false negatives and 6 indeterminate cases and came to a conclusion that fibrin strands and retracting clots are basic features visualized in majority of the cases to come to a certain diagnosis of hemorrhagic cysts and at least 90% of the cases would have either of the features[20-23].
Conclusion
MRI is found to be more precise and many a times gold standard in comparison to TVS to characterize, localize and evaluate the number of lesions in benign as well as malignant pelvic pathologies.In cases of adenomyosis, MRI turned out to be more accurate in its diagnosis where ultrasound was found indeterminate in visualizing the junctional zone. MRI turned out to be more superior than transvaginal ultrasound in cases of fibroids in aiding their number and location. In endometrial lesions, TVS can be used as a great screening tool. MRI was found to be crucial in determining myometrial invasion. In instances of endometrial carcinoma, MRI conclusion cannot forestall the requirement for endometrial biopsy.Extent of carcinoma cervix and its invasion to adjacent viscera was found to be superior in MRI compared to ultrasound. In the adnexal lesions, characterization and differentiation of various types of lesions, TVS was less specific in contrast to MRI. Finally, we conclude the TVS lacks specificity and sensitivity in relation to MRI but acts as a great screening tool in evaluation and further management as it is cost effective and less time consuming. MRI is accordingly a more precise preoperative imaging modality for portraying and distinguishing the distinct features of varied lesions.
Funding
No funding sources.
Ethical Approval
The study was approved by the Institutional Ethics Committee
Conflict of Interest
The authors declare no conflict of interest.
Acknowledgments
The encouragement and support from Bharath University, Chennai is gratefully acknowledged. For provided the laboratory facilities to carry out the research work.
References
- Saini A, Dina R, McIndoe G, et al. Characterization of adnexal masses with MRI. Am J Roentgenol 2005; 3:1004-1009.
- ACR practice guideline for the performance of pelvic ultrasound in females. Reston, VA: American College of Radiology 2006.
- ACR practice guideline for the performance of magnetic resonance imaging (MRI) of the soft tissue components of the pelvis. Reston, VA: American College of Radiology Amended 2006
- Schwartz LB, Panageas E, Lange R, et al. Female pelvis: Impact of MR imaging on treatment decisions and net cost analysis. Radiology 1994; 192:55-60.
- Padubidri VG, Shirish ND. Shaw’s text book of gynaecology, 16th Edn.
- Murase E, Siegelman ES, Outwater EK, et al. Uterine leimyomas histopathologic features, MR imaging findings, differential diagnosis and treatment. Radiographics 1999; 19:1179-97.
- Bailey CL, Ueland FR, Land GL, et al. The malignant potential of cystic ovarian tumors in women over 50 years of age. Gynecol Oncol 1998; 69:3-7.
- Smorgick N, Maymon R. Assessment of adnexal masses using ultrasound: a practical review. Int J Womens Health 2014; 6:857–863.
- Bazot M, Cortez A, Darai E, et al. Ultrasonography compared with magnetic resonance imaging for the diagnosis of adenomysis: Correlation with histopathology. Hum Reprod 2001; 16:2427-33.
- Devimeenal J, Arun DS. Comparison of the diagnostic accuracy of magnetic resonance imaging (MRI), transabdominal ultrasound (TAS), transvaginal ultrasound (TVS) in characterizing the uterine mass lesions. J Dent Med Sci 2017; 16:65-74.
- Kochiyil J, Jeevan V. Utility of MRI in uterine and adnexal lesions. Int J Med Res Review 2016; 4:655-663.
- Levens ED, Wesley R, Premkumar A, et al. Magnetic resonance imaging and transvaginal ultrasound for determining fibroid burden: Implications for research and clinical care. Am J Obstetr Gynecol 2009; 200:537-e1.
- Adusumilli S, Hussain HK, Caoili EM, et al. MRI of sonographically indeterminate adnexal masses. Am J Roentgenol 2006; 187:732–740.
- Haggerty AF, Hagemann AR, Chu C, et al. Correlation of pelvic magnetic resonance imaging diagnosis with pathology for indeterminate adnexal masses. Int J Gynecol Cancer 2014; 24:1215-21.
- Scoutt LM, McCarthy SM, Lange R, et al. MR evaluation of clinically suspected adnexal masses. J Comput Assist Tomogr 1994; 18:609-18.
- Archana B, Michelle F. Evaluation and histopathological correlation of abnormal uterine bleeding in perimenopausal women. J Bombay Hosp 2010; 52:69-72.
- Bindushree K, Gurushankar G, Geetha S, et al. Ultrasonographic evaluation of abnormal uterine bleeding in postmenopausal women. Int J Reprod Contracept Obstet Gynecol 2015; 4:229-234.
- Rajul R. Role of imaging in female infertility. Indian J Radiol Imaging 2010; 20:168-73.
- Medl M, Kulenkampff KJ, Stiskal M, et al. Magnetic resonance imaging in the preoperative evaluation of suspected ovarian masses. Anticancer Res 1995; 15:1123-5.
- Aubel S, Wozney P, Edwards RP. MRI of female uterine and juxta-uterine masses: clinical application in 25 patients. Magnetic Resonance Imaging 1991; 9:485-91.
- Sohaib SA, Mills TD, Sahdev A, et al. The role of magnetic resonance imaging and ultrasound in patients with adnexal masses. Clin Radiol 2005; 60:340–348.
- Ahmed LA, Ahmed SN, Ashraff SS, et al. Ultrasound versus magnetic resonance imaging in diagnosis of malignant and surgically difficult adnexal cases. Med. J Cairo Univ 2016; 84:141-143.
- Baltarowich OH, Kurtz AB, Pasto ME, et al. The spectrum of sonographic findings in hemorrhagic ovarian cysts. Am J Roentgenol 1987; 148:901-905.
Author Info
Department of Radio Diagnosis, Sree Balaji Medical College & Hospital, Bharath Institute of Higher Education and Research, Chennai, Tamil Nadu, IndiaCitation: Pujitha DS, Prabakaran M, Role of Trans Vaginal Sonography and Magnetic Resonance Imaging in Perimenopausal Bleeding, J Res Med Dent Sci, 2021, 9 (4): 331-336.
Received: 20-Mar-2021 Accepted: 08-Apr-2021
