Research - (2021) Volume 9, Issue 9
Seroprevalence of COVID-19 in a City in India: A Community-based Cross-Sectional Study
Bapusaheb Nagargoje1, Avesh Palod2, Jagannath Dixit3, Kananbala Yelikar3, Smita Andurkar3 and Shraddha Badgujar3*
*Correspondence: Shraddha Badgujar, Department Community Medicine, Government Medical College, India, Email:
Abstract
Background: Population-based sero-epidemiological studies explain the extent of SARS-CoV-2 infection. This study was conducted in view of studying the seroprevalence in the second phase of pandemic in Nashik City of Maharashtra a state in western India. Maharashtra has the highest case fatality rate of 23.13%, hence it is necessary to study the extent of spread of infection to propose further management protocols until vaccine is made available to public. Objectives: To understand the current spread of infection in the community and thus imply the need for stringent preventive measures to be followed until the vaccine is made available to all. Methods: A Community based cross-sectional study was conducted in the six ‘Prabhags’ of Nashik Municipal Corporation. House to house survey was done from 9th to 11th of January 2021. Google forms were used for data collection and 3-5 ml of venous blood was collected after taking informed consent of the participant. The blood was transported for COVID-19 IgG antibody test by ELISA method at Viral Research and Diagnostics Laboratory, Nashik as per ICMR (Indian Council of Medical Research) guidelines. Results: Total Sero-prevalence of SARS-CoV-2 was 39.53% (CI: 37.55-41.54). A higher seropositivity rate 42.07% (CI: 39.07-46.39) was found in the slum areas (χ2=4.214; p=0.02). The Prabhag with highest seropositivity of 42.66% was New Nashik Cidco. Adding together the people who tested positive for SARS-CoV-2 antigen and those who tested positive for SARS-CoV-2 antibody, 42.29% (996 out of 2355) of population seems to be exposed to COVID-19 infection.
Keywords
COVID-19, SARS-CoV-2, Seroprevalence, Nashik
Introduction
Since December 2019, a novel coronavirus disease had rapidly spread throughout China, leading to a global outbreak and causing considerable public health concern [1]. World Health Organisation (WHO) announced the outbreak of COVID-19 as a global public health emergency on 30 January 2020 [2]. In India, the first case of COVID-19 was reported on January 27, 2020 in Kerala district. Since then, there is a wide variation in the reporting of cases across the country. The case reporting is based on the SARS-CoV-2 antigen testing by Real-Time Reverse Transcription Polymerase Chain Reaction (RT-qPCR) or by Rapid Antigen Test (RAT). Laboratory capacity for testing, health-seeking behaviours and testing strategies in terms of who gets tested, influence the numbers of cases reported. Furthermore, the current testing criteria by Ministry of Health and Welfare (MoHFW) do not recommend a COVID-19 swab test for asymptomatic population, unless they have come in contact with a positive patient; this may have missed many asymptomatic and mild infections [3]. An individual infected with SARS-CoV-2 virus may remain asymptomatic throughout the course of infection or may develop a mildflu- like illness. Data suggests that 80% of infections are mild or asymptomatic and hence, there is a high probability that a number of individuals who were infected with SARS-CoV-2, never got traced as they were never tested [4]. Human body elicits humoral or cellular immune response following any infection. SARS-CoV-2 infection elicits development of IgM and IgG antibodies, which are the most useful for assessing antibody response [5]. In SARS-CoV-2 infections, IgM and IgG antibodies can arise nearly simultaneously in serum within 2 to 3 weeks after the onset of illness. Studies also suggest that some individuals do not develop detectable IgG or IgM antibodies following infection, also how long these antibodies persist in the circulation is yet to be known.
Thus, the absence of detectable IgM or IgG antibodies does not necessarily rule out that they could have previously been infected. However, the presence of these antibodies in blood indicates a past infection as well as development of immunity against the disease [5,6]. Knowledge about the true extent of infection is critical for an effective public health response. World Health Organisation (WHO) states that, the percentage of people that need to be immune in order to achieve herd immunity varies with each disease. The proportion of the population, that must be vaccinated against COVID-19 to begin inducing herd immunity is not yet known. This is an important area of research and varies likely according to the community, the vaccine, the populations prioritized for vaccination, and other factors [7]. Population-based sero-epidemiological studies are therefore a recommended measure to study the extent of spread of infection in an area to aid in this information. The objective of this study was to understand the current spread of infection in the community and thus imply the need for stringent preventive measures to be followed until the vaccine is made available to all.
Methods
A community based cross-sectional study was carried out in the households of Municipal Corporation (NMC) area of Nashik a city in the state of Maharashtra, western region of India. Sample size was calculated taking into consideration the antigen/RTPCR positivity rate of 25% using statistical formula N=Z2pq/e2, where N=Sample size, Z=Standard Normal deviate=1.96, p=25, q=100-p, eabsolute precision. Absolute precision was taken as 1.75. The total sample size of 2355 individuals above 18 years of age, who had been residents of Nashik city for more than 6 months, excluding non-consenting and migrant population, were selected. Study population was taken from six Prabhags of Nashik Municipal Corporation. The samples were taken proportionate to the population and were given appropriate weightage to slum and non-slum areas. Data collection was done from 09th January 2021 to 11th January 2021 by 12 field teams. Each team consisted of 2 doctors, 1 trained phlebotomist, 1 assistant and 1 health worker from the local health post.
After visiting the selected area, main square was identified. Lane was selected randomly by spinning the bottle. After randomly selecting first household, required number of households from that area, were selected by using left hand rule. After the first household every tenth household was selected. In case of refusal, the immediate next household was selected. One adult from each household fulfilling the inclusion criteria was interviewed by using Google form. From the first household oldest male, from second household oldest female, from third household youngest male and from fourth youngest female was interviewed and same sequence was continued further. The study team briefed the selected household about the survey objectives and process involved with the help of participant information sheet. After obtaining consent from the eligible participant, information on basic demographic details, exposure history to laboratory confirmed COVID-19 cases, symptoms suggestive of COVID-19, and clinical history was recorded in the Google form by the survey teams. 3-5 ml of venous blood was collected under all aseptic precautions and transported to Viral Research and Diagnostic Laboratory (VRDL), Nashik as per ICMR guidelines. Antibody testing was done using COVID-19 IgG ELISA technique on the same day. The data collected was entered systematically in Microsoft Excel 2019 and represented in tabular and graphical format. Tests of statistical significance were applied using Open epi online calculator.
Results
A sample size of 2352 was expected to be achieved in Nashik City. Total sample collection achieved was 2355. 30.83% samples were collected from slum and 69.17% samples from non-slum areas Nashik Municipal Corporation. Total Sero-prevalence of SARS-CoV-2 was 39.53%. Seroprevalence was 42.70% in slum areas and 32.12% in non-slum areas. All the findings fall within the range of 95% confidence interval. Chi-square test was applied to study the association between slum areas and sero-positivity which was found to be statistically significant (χ2=4.214; p=0.0201); Odds ratio=1.21 (CI-1.013-1.445) (Table 1).
| Locality | Total samples | Total seropositive | CI 95% |
|---|---|---|---|
| SLUM | 726 (30.83) | 310 (42.70) | 39.07-46.39 |
| NON-SLUM | 1629 (69.17) | 621 (38.12) | 35.76-40.53 |
| TOTAL | 2355 | 931 (39.53) | 37.55-41.54 |
Table 1: Sero-prevalence of SARS-CoV-2.
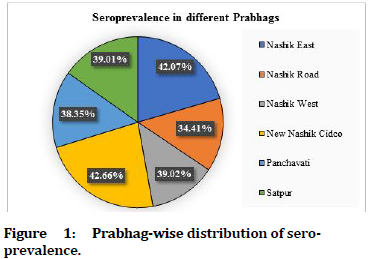
The highest sero-positivity of 42.66% was observed in New Nashik Cidco. followed by 42.07% in Nashik East. The rest of the Prabhags had a seroprevalence ranging from 34.31- 39.01% (Figure 1).
Figure 1. Prabhag-wise distribution of seroprevalence.
Highest sero-prevalence of 75% was seen in the age group of >80 years in slum areas and 46.97% in 18-20 years age group in non-slum areas. Lowest prevalence of 30.77% was seen in 71-80 years age group in slum areas and >80 years age group in non-slum areas. Seroprevalence among males from both slum and non-slum areas was 39.95% and that of females was 39.13%. Whereas, a statistically significant association was found between high seropositivity and females residing in slums (43.26%) than in non-slums (37.13%) (χ2=4.169; p=0.0239) (Table 2).
| Locality | Age | Positive | Negative | Seroprevalence (%) | Total samples | ||
|---|---|---|---|---|---|---|---|
| Males | Females | Males | Females | ||||
| SLUM | 18-20 | 14 | 9 | 10 | 14 | 48.94 | 47 |
| 21-30 | 41 | 43 | 62 | 65 | 39.81 | 211 | |
| 31-40 | 23 | 37 | 25 | 46 | 45.8 | 131 | |
| 41-50 | 26 | 33 | 34 | 42 | 43.7 | 135 | |
| 51-60 | 18 | 24 | 34 | 27 | 40.78 | 103 | |
| 61-70 | 12 | 19 | 21 | 17 | 44.93 | 69 | |
| 71-80 | 3 | 5 | 7 | 11 | 30.77 | 26 | |
| >80 | 3 | 0 | 0 | 1 | 75 | 4 | |
| TOTAL | 140 | 170 | 193 | 223 | 42.7 | 726 | |
| NON-SLUM | 18-20 | 16 | 15 | 17 | 18 | 46.97 | 66 |
| 21-30 | 72 | 82 | 96 | 114 | 42.31 | 364 | |
| 31-40 | 81 | 61 | 132 | 129 | 35.24 | 403 | |
| 41-50 | 47 | 56 | 89 | 101 | 35.15 | 293 | |
| 51-60 | 32 | 46 | 66 | 89 | 33.48 | 233 | |
| 61-70 | 49 | 33 | 61 | 41 | 44.57 | 184 | |
| 71-80 | 21 | 6 | 31 | 15 | 36.99 | 73 | |
| >80 | 3 | 1 | 8 | 1 | 30.77 | 13 | |
| TOTAL | 321 | 300 | 500 | 508 | 38.12 | 1629 | |
Table 2: Age and sex-wise distribution of seroprevalence in slum and non-slum areas.
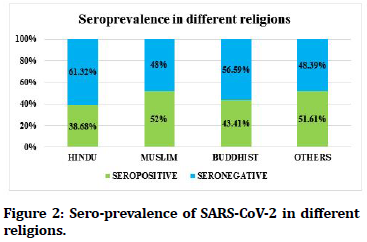
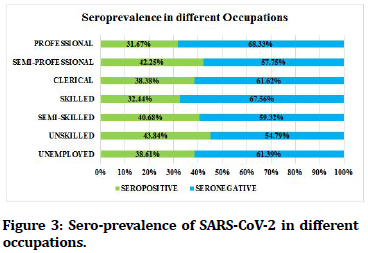
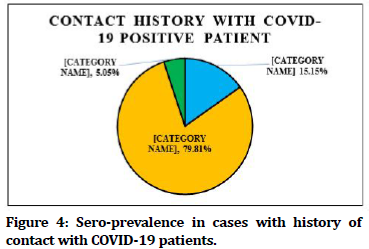
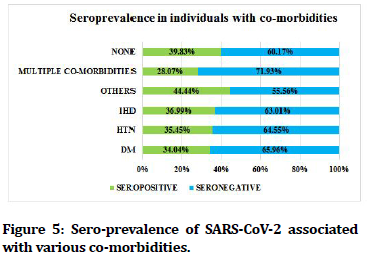
Highest sero-prevalence of 52% was seen in Muslim religion, followed by Others (Sikh, Christian, etc.)- 51.61%, Buddhist- 43.41%, and Hindu-38.68%. Chisquare test was applied to study the association between Muslim religion and sero-positivity which was found to be statistically significant with, χ2=5.037; ‘p’ value=0.0124, Odds ratio=1.685 (CI-1.061-2.683) (Figure 2). Highest sero-prevalence of 45.21% was present in unskilled workers (Job that does not require any formal training). Lowest sero-prevalence of 31.67% was seen in Professional workers like Doctors, lawyers, professors, expert etc (Figure 3). Of the total seropositive cases, 743 (79.80 %) were found to have no history of contact with COVID-19 positive patient, 141 (15.15%) had history of contact with confirmed case of COVID-19 and 47 (5.05%) were unaware of any contact history (Figure 4). Seropprevalence was 36.99% in individuals with Ischaemic Heart Disease, 35.45% in individuals with Hypertension, and 34.04% in cases with Diabetes Mellitus. 39.83% seroprevalence was seen in individuals without any co-morbid conditions. Seroprevalence was 28.07% in individuals with more than one co-morbid conditions like Diabetes, Hypertension, Ischaemic Heart Disease, Hypothyroidism, Bronchial Asthma, etc (Figure 5).
Figure 2.Sero-prevalence of SARS-CoV-2 in different religions.
Figure 3. Sero-prevalence of SARS-CoV-2 in different occupations.
Figure 4. Sero-prevalence in cases with history of contact with COVID-19 patients.
Figure 5. Sero-prevalence of SARS-CoV-2 associated with various co-morbidities.
The time interval between swab test for SARS-CoV-2 antigen to SARS-CoV-2 antibody test signifies the time taken for formation of IgG against SARS-CoV-2 infection. Among 2355 samples tested for sero-positivity, 517 samples were also tested for SARS-CoV-2 antigen, of which 170 (32.88%) were tested antigen positive.
Of which 61.76% (105 out of 170) were seropositive and 38.24% (65 out of 170) were seronegative. 25.92% (134 out of 517) samples were antigen negative but seropositive. Therefore, total number of people who got infected with COVID-19 can be arrived at, by adding together the people who tested positive for SARS-CoV-2 antigen and those who tested positive for SARS-CoV-2 antibody.
Thus, 42.29% (996 out of 2355) of population seems to be exposed to COVID-19 infection. Sero-prevalence was highest in the time interval of more than three weeks. Chi-square test was applied to study the co-relation between SARS-CoV-2 antigen and SARS-CoV-2 antibody detection, which was statistically significant, with (χ2=25.56; p=0.000) (Table 3).
| Time interval | Antigen test positive | Total | |
| Seropositive | Seronegative | ||
| 1 - 2 WEEKS | 15 | 15 | 30 |
| 2 - 3 WEEKS | 12 | 8 | 20 |
| > 3 WEEKS | 78 | 42 | 120 |
| Total | 105 | 65 | 170 |
| Time interval | Antigen test negative | TOTAL | |
| SEROPOSITIVE | Seronegative | ||
| 1 - 2 WEEKS | 64 | 81 | 145 |
| 2 - 3 WEEKS | 20 | 32 | 52 |
| > 3 WEEKS | 50 | 100 | 150 |
| TOTAL | 134 | 213 | 347 |
Table 3: Time interval between SARS-CoV-2 antigen and antibody test.
Discussion
In Geneva, Between April 6 and May 9, 2020, a seroprevalence of 4.8% in first week was found which increased to 10.8% by fifth week [8]. The first national sero-prevalence survey conducted by Indian Council of Medical Research (ICMR) in May and June during initial phase of pandemic, reported a seroprevalence of 0.73% [9]. Estimated sero-prevalence of COVID-19 in Aurangabad Municipal Corporation area in the month of August 2020 was found to be 11.81% [10]. In Delhi, by early July 2020, 23% population of the surveyed areas had developed IgG antibodies [11,12]. In present study, total sero-prevalence of SARS-CoV-2 was 39.53%. Sero prevalence was more in slum areas as compared to nonslum areas in, with 42.70% in slum and 32.12% in nonslum areas (χ2=4.214; p=0.0201). It was found that people residing in slum areas were 1.21 times more likely to develop sero-positivity as compared to non-slum areas. Similar findings were present in Mumbai, 57% in slums and 16% in non-slum areas had developed these antibodies [11]. Higher prevalence in slums could possibly be due to high population density, crowded housing and shared common facilities like water points, toilets etc. The ‘Epidemiological and Serological Surveillance of COVID-19 in Pune’ conducted in 5 highincidence Prabhags also supports the idea, that the seroprevalence was higher in those who live in tenement or hutment dwellings, and among those who share toilets [13]. We also found a statistically significant association between high seropositivity and females residing in slums (43.26%) than in non-slums (37.13%) (χ2=4.169; p=0.0239). In the present study, Odds Ratio was calculated for relationship between religion and seropositivity and it revealed that the Muslims had a 1.685 times higher chance of developing sero-positivity, than all others with a p-value 0.0124, which indicated that this association was statistically significant. Similar findings were seen in sero-surveys conducted in Aurangabad and Malegaon, that the seropositivity was more among Muslims, and the association of religion with seropositivity was statistically significant [10,14]. 80% of the sero positive people had no history of contact with confirmed COVID-19 case. This indicates community transmission. According to CDC, some individuals do not develop detectable IgG or IgM antibodies following infection, also how long these antibodies persist in the circulation is yet to be known.6 In corroboration to which we found that 38.62% people had antibodies with prior SARS-CoV-2 antigen test negative whereas, 38.24% had prior SARS-CoV-2 antigen test positive but no detectable antibodies in circulation. High prevalence of seropositivity in other studies from Aurangabad [10], Mumbai [11], Delhi [12], and Pune [13], and Ahmedabad [15] also suggest that there is community spread of infection, and most of the infections are asymptomatic and go undetected. In accordance to WHO, the achievement of herd immunity depends on, the community, the vaccine that is used, the populations prioritized for vaccination, and other factors [7]. Population-based sero-epidemiological studies are therefore a recommended measure to study the extent of spread of infection in an area to aid in this information.
Conclusion
It is observed that a higher sero-positivity rate is significantly associated with slums as compared to nonslums. Sero-positivity rate is very similar from 38.35% to 42.07% in different Prabhags of Nashik City. Antigen test positivity is associated with sero-positivity. However, there were many individuals who possibly had asymptomatic or mild infection of COVID-19 who showed sero-positivity despite a negative SARS-CoV-2 antigen test. The study is representative of the entire city and hence it can be said that 42.29% (996 out of 2355) of population seems to be exposed to COVID-19 infection. The expected seroprevalence for achieving herd immunity varies from 65% to 95% depending on the disease and the community. Even then, only 42.29% population was found to be exposed to COVID-19 infection in Nashik city. Thus, there should be no false sense of security generated in common public due to present seropositivity rate. It is yet necessary to strictly implement the practice of wearing masks, washing hands with soap and water and physical distancing. This study may be made use of, for deciding the priority of vaccination in near future, as achieving herd immunity with safe and effective vaccines makes diseases rarer and saves lives.
Ethical Considerations
This study with was approved by Institutional Ethics Committee of Manavata Clinical Research Institute on 07th January 2021. Written Informed consent was taken from each eligible participant before enrolling him/her in the study. This study was conducted in accordance with latest version of Declaration of Helsinki.
Acknowledgements
The author acknowledges the support of all the doctors, technical staff and local health workers for their sincire and meticulous field work during the survey.
Source of Support
Nashik Municipal Corporation.
Conflict of Interest
None.
References
- Wang F, Qu M, Zhou X. The timeline and risk factors of clinical progression of COVID-19 in Shenzhen, China. J Transl Med 2020; 18:270.
- https://www.who.int/emergencies/diseases/novel-coronavirus-2019
- https://www.mohfw.gov.in/pdf/AdvisoryonstrategyforCOVID19TestinginIndia.pdf
- Gideon M, Merone L. A systematic review and meta-analysis of published research data on COVID-19 infection fatality rates. Int J Infectious Diseas 2020; 101:138-148.
- Hosseini A, Hashemi V, Shomali N, et al. Innate and adaptive immune responses against coronavirus. Biomed Pharmacother 2020; 132:110859.
- https://www.cdc.gov/coronavirus/2019-ncov/lab/resources/antibody-tests-guidelines
- https://www.who.int/news-room/q-a-detail/coronavirus-disease-covid-19-serology
- Stringhini S, Wisniak A, Piumatti G, et al. Seroprevalence of anti-SARS-CoV-2 IgG antibodies in Geneva, Switzerland (SEROCoV-POP): A population-based study. Lancet 2020; 396:10247.
- Kumar MS, Bhatnagar T, Manickam P, et al. National sero-surveillance to monitor the trend of SARS-CoV-2 infection transmission in India: Protocol for community-based surveillance. Indian J Med Res 2020; 151:419.
- Dixit JV, Iravane J, Andurkar SP, et al. Seroprevalence of COVID-19 in Aurangabad district. IJCRT 2020; 8.
- https://science.thewire.in/health/delhi-mumbai-seroprevalence-survey-results-infection-fatality-rates/
- https://indianexpress.com/article/cities/delhi/delhi-sero-survey-coronavirus-covid-cases-death-toll-6563510
- http://www.iiserpune.ac.in/userfiles/files/Pune_Serosurvey_summary_17_08_2020_ENGLISH.pdf
- Saple P, Gosavi S. Study the prevalence of seroconversion among population exposed to SARS-CoV-2 infection by IgG antibody testing: Community based, cross sectional study from urban area of Malegaon, Maharashtra. 2020.
- https://www.livemint.com/news/india/ahmedabad-sero-survey-suggests-nearly-one-in-four-has-covid-antibodies-11599108738476.html.
Author Info
Bapusaheb Nagargoje1, Avesh Palod2, Jagannath Dixit3, Kananbala Yelikar3, Smita Andurkar3 and Shraddha Badgujar3*
1MOH, Nashik Municipal Corporation, India2COVID-19 testing unit, Nashik Municipal Corporation, India
3Department Community Medicine, Government Medical College, Aurangabad, India
Citation: Bapusaheb Nagargoje, Avesh Palod, Jagannath Dixit, Kananbala Yelikar, Smita Andurkar, Shraddha Badgujar,Seroprevalence of COVID-19 in a City in India: A Community-based Cross-Sectional Study, J Res Med Dent Sci, 2021, 9(9): 48-53
Received: 18-May-2021 Accepted: 06-Sep-2021