Review Article - (2022) Volume 10, Issue 7
Speech Appliances in Cleft
Jigna Kachaliya*, Pallavi Daigavane, Priyanka Niranjane, RH Kamble and Tirth Bhutada
*Correspondence: Jigna Kachaliya, Department of Orthodontics, Sharad Pawar Dental College and Hospital, Datta Meghe Institute of Medical Sciences (Deemed to be University) Sawangi (Meghe), Wardha, Maharashtra, India, Email:
Abstract
“Cleft Lip and Palate” (CLP) individuals face a number of aesthetic and functional issues. A cleft lip is inherited deformity
that originates in the womb during fourth and sixth weeks of pregnancy. A cleft palate is a birth abnormality that occurs
between the eighth and the twelfth week of pregnancy. It's a gap in the roof of the mouth caused by the failure of the two
sides of the palate to fuse.
CLP are caused by various factors, the majority of which are unknown. Clefts are assumed to be the result of a mix of genetic
and environmental factors. Parental history, family history, obesity during pregnancy and diabetic female are among the
factors that predispose to development of CLP. Suckling, extreme facial deformities, ear infections, deafness, breathing
difficulties, malocclusion, and poor speech are all concerns that children with CLP face.
Children who have had a cleft palate are more likely to have delays in their speech development and early language
development. These disorders can be developmental or acquired, as well as physical or neurological in nature [1].
The precise character of each articulatory speech order should be recognized as a basis for diagnostic and therapy
planning. When someone's speech sounds nasal, it's usually a sign that they have VPD. However, velopharyngeal structures
must be examined during speech in order to pinpoint the cause of VPD. Doctors can observe the velopharyngeal mechanism
from the side and front using a video x-ray machine (video fluoroscopy). Therapists can build appropriate treatment plans
using extensive information on the nature of the condition and its natural progression.
These people can be treated surgically or non-surgically for their entire condition. This review article mainly focuses on the
non-surgical treatment option for treating speech disorders in patients with CLP. The three main types of appliances
discussed in this article will be “speech bulb obturator”, “palatal lift” and “palatal obturator”.
https://www.mobafire.com/profile/transplanthairistanbul12-1119971?profilepage http://www.effecthub.com/user/3725182 http://hawkee.com/profile/4921038/ https://www.youmagine.com/transplanthairistanbul12/designs https://www.myminifactory.com/users/Transplanthairistanbul12 http://onlineboxing.net/jforum/user/edit/249443.page http://qooh.me/account/home/ https://band.us/band/92227712 https://linktr.ee/transplanthairistanbul12 https://pubhtml5.com/homepage/gmwxs/ https://telegra.ph/Transplanthairistanbul12-08-31 https://www.diggerslist.com/64f060cc50581/about https://www.facer.io/user/1bbecUrwua https://allmyfaves.com/Transplanthairistanbul12 https://www.metal-archives.com/users/Transplanthairistanbul12 https://www.catchafire.org/profiles/2485119/ https://www.fimfiction.net/user/632232/Transplanthairistanbul12 https://www.hebergementweb.org/members/transplanthairistanbul12.546054/ https://www.sqlservercentral.com/forums/user/transplanthairistanbul12 https://www.twitch.tv/transplanthairistanbul12/about https://www.roleplaygateway.com/member/Transplanthairistanbul12/ https://ko-fi.com/transplanthairistanbul12 https://www.provenexpert.com/transplanthairistanbul12/ https://www.intensedebate.com/people/pembikbulut https://www.indiegogo.com/individuals/35105511 https://visual.ly/users/transplanthairistanbul/portfolio https://slides.com/transplanthairistanbul12 https://letterboxd.com/transplanthair/ https://micro.blog/Transplanthair https://fliphtml5.com/dashboard/public-profile/ybcvl https://community.windy.com/user/transplanthairrr https://speakerdeck.com/transplanthairistanbul12 https://trello.com/u/transplanthairistanbul/activity https://www.redbubble.com/people/Transplanthairr/shop?anchor=profile&asc=u https://myanimelist.net/profile/Transplanthairr https://3dwarehouse.sketchup.com/user/851a4681-3d38-4d12-ad90-26805cdbb2bb/Transplanthairistanbul12-T https://www.wattpad.com/user/kerobey https://www.goodreads.com/user/show/169468662-transplanthairistanbul12 https://sourceforge.net/u/transplanthairi/profile https://en.gravatar.com/transplanthairistanbul https://tr.pinterest.com/transplanthairistanbul/ https://www.mapleprimes.com/users/Transplanthairistanbul12 https://medium.com/@transplanthairistanbul https://www.ted.com/profiles/44917766 https://www.infragistics.com/community/members/1997209513d1313c62654fa4b6327bd684ca76a6 https://www.metooo.io/u/64f1b26134cbec3769e08581 https://app.roll20.net/users/12364550/transplanthairistanbul12-t https://list.ly/transplanthairistanbul/ https://giphy.com/channel/Transplanthairistanbul12 https://www.tumblr.com/blog/transplanthairistanbul12 https://dzone.com/users/4988171/transplanthairistanbul12.html https://www.creativelive.com/student/transplanthairistanbul12-transplanthairistanbul12?via=accounts-freeform_2 https://gab.com/Transplanthairistanbul12 https://sketchfab.com/Transplanthairistanbul12 https://www.flickr.com/people/199079408@N06/ https://devpost.com/transplanthairistanbul?ref_content=user-portfolio&ref_feature=portfolio&ref_medium=global-nav https://hub.docker.com/u/transplanthairistanbul12 https://forums.autodesk.com/t5/user/viewprofilepage/user/self https://profiles.wordpress.org/transplanthairistanbul/ https://mastodon.online/@Transplanthairistanbul12 https://wefunder.com/transplanthairistanbul12 https://seedandspark.com/user/transplanthairistanbul12-01h98dvpezt6fg5t3dvys0kdx7 https://calis.delfi.lv/blogs/posts/208553-httpstransplanthairistanbul/lietotajs/312307-transplanthairistanbul12/ https://os.mbed.com/users/transplanthairistanb/ https://notionpress.com/author/920174# https://my.desktopnexus.com/Transplanthairistanbul12/ https://guides.co/a/transplanthairistanbul12-transplanthairistanbul12/ https://www.bahamaslocal.com/userprofile/1/238492/Transplanthairistanbul12.html http://molbiol.ru/forums/index.php?showuser=1296004 https://www.credly.com/users/transplanthairistanbul12-transplanthairistanbul12/badges https://www.mobafire.com/profile/smilemakeovermarmaris12-1124987?profilepage https://www.youmagine.com/smilemakeovermarmaris12/designs https://www.myminifactory.com/users/Smilemakeovermarmaris12 http://qooh.me/Smilemakeov https://linktr.ee/smilemakeovermarmaris12 https://pubhtml5.com/homepage/wrban/ https://telegra.ph/Smilemakeovermarmaris12-10-09 https://www.diggerslist.com/6523fe47abb93/about https://allmyfaves.com/Smilemakeovermarmaris12 https://www.catchafire.org/profiles/2520762/ https://www.fimfiction.net/user/644474/Smilemakeovermarmaris12 https://www.hebergementweb.org/members/smilemakeovermarmaris12.563775/ https://www.sqlservercentral.com/forums/user/smilemakeovermarmaris12 https://www.twitch.tv/smilemakeovermarmaris12/about https://www.roleplaygateway.com/member/Smilemakeovermarmaris12/ https://www.provenexpert.com/smilemakeovermarmaris12/?mode=preview https://www.intensedebate.com/people/Smilemakeo https://www.indiegogo.com/individuals/35476150 https://visual.ly/users/smilemakeovermarmaris/portfolio https://slides.com/smilemakeovermarmaris12 https://letterboxd.com/Smilemakeoverma/ https://fliphtml5.com/dashboard/public-profile/hebyg https://community.windy.com/user/smilemakeoverma https://speakerdeck.com/smilemakeovermarmaris12 https://trello.com/u/smilemakeovermarmaris https://myanimelist.net/profile/Besthairtranss https://3dwarehouse.sketchup.com/user/1657a34a-1af7-408c-a8b3-ebc63c8919b6/Smilemakeovermarmaris12-S https://www.wattpad.com/user/Smilemakeovermar https://www.goodreads.com/user/show/170572298-smilemakeovermarmaris12 https://gravatar.com/smilemakeovermarmaris https://www.mapleprimes.com/users/Smilemakeovermarmaris12 https://medium.com/@smilemakeovermarmaris https://www.ted.com/profiles/45255175 https://www.infragistics.com/community/members/31e1c358ac5743839282499b0cb0fc832c1265d3?_ga=2.92918682.603980954.1696860449-527408912.1696860449 https://www.metooo.io/u/652409a079c47c11a2f0e8a1 https://app.roll20.net/users/12515860/smilemakeovermarmaris12-s https://list.ly/smilemakeovermarmaris/activity https://giphy.com/channel/Smilemakeovermarmaris12 https://www.tumblr.com/smilemakeovermarmaris12 https://www.creativelive.com/student/smilemakeovermarmaris12?via=accounts-freeform_2 https://gab.com/Smilemakeovermarmaris12 https://www.flickr.com/people/199363203@N08/ https://seedandspark.com/user/smilemakeovermarmaris12-01hcadmczr2vwnp8v5achgahq7 https://os.mbed.com/users/smilemakeovermarmari/ https://calis.delfi.lv/blogs/lietotajs/318437-smilemakeovermarmaris12/ https://notionpress.com/author/934579 https://my.desktopnexus.com/Smilemakeovermarmaris12/ https://guides.co/a/smilemakeovermarmaris12-smilemakeovermarmaris12/ https://www.bahamaslocal.com/userprofile/1/250951/Smilemakeovermarmaris12.html http://molbiol.ru/forums/index.php?showuser=1302761 https://www.credly.com/users/smilemakeovermarmaris12-smilemakeovermarmaris12/badges https://devpost.com/smilemakeovermarmaris?ref_content=user-portfolio&ref_feature=portfolio&ref_medium=global-nav https://hub.docker.com/u/smilemakeovermarmaris12 http://onlineboxing.net/jforum/user/editDone/254669.page https://micro.blog/Smilemakeov http://www.effecthub.com/user/3729781 http://hawkee.com/profile/5155278/ https://wefunder.com/smilemakeovermarmaris12 https://www.facer.io/user/X1BgQ0Qhgl https://mastodon.online/@Smilemakeovermarmaris12 https://sketchfab.com/Smilemakeovermarmaris12 https://profiles.wordpress.org/dentalclinicmarmaris12/ https://dzone.com/users/5004739/smilemakeovermarmaris12.html https://www.metal-archives.com/users/Smilemakeovermarmaris12 https://ko-fi.com/smilemakeovermarmaris12#paypalModal https://www.redbubble.com/people/Smilemakk/shop?asc=u https://www.mobafire.com/profile/tekneturumarmaris12-1120904?profilepage http://www.effecthub.com/user/3726311 http://hawkee.com/profile/4970246/ https://www.youmagine.com/tekneturumarmaris12/designs https://www.myminifactory.com/users/Tekneturumarmaris12 http://qooh.me/Tekneturu https://linktr.ee/tekneturumarmaris12 https://pubhtml5.com/homepage/xeosr/ https://telegra.ph/Tekneturumarmaris12-09-09 https://www.diggerslist.com/64fc41ac64c68/about https://allmyfaves.com/Tekneturumarmaris12 https://www.metal-archives.com/users/Tekneturumarmaris12 https://www.catchafire.org/profiles/2493597/ https://www.fimfiction.net/user/635020/Tekneturumarmaris12 https://www.hebergementweb.org/members/tekneturumarmaris12.551211/ https://www.sqlservercentral.com/forums/user/tekneturumarmaris12 https://www.twitch.tv/tekneturumarmaris12/about https://www.roleplaygateway.com/member/Tekneturumarmaris12/ https://www.provenexpert.com/tekneturumarmaris12/ https://www.intensedebate.com/people/kerobey https://www.indiegogo.com/individuals/35186423 https://visual.ly/users/tekneturumarmaris/portfolio https://slides.com/tekneturumarmaris12 https://letterboxd.com/Tekneturumarmar/ https://micro.blog/Tekneturumarmaris12 https://fliphtml5.com/dashboard/public-profile/fonnn https://community.windy.com/user/tekneturu https://speakerdeck.com/tekneturumarmaris12 https://trello.com/u/tekneturumarmaris https://www.redbubble.com/people/Tekneturu/shop?asc=u https://myanimelist.net/profile/Tekneturu https://3dwarehouse.sketchup.com/user/dfd5ab04-60b8-41e5-8fb9-a6ac0f4e2233/Tekneturumarmaris12-T https://www.wattpad.com/user/Tekneturumarmaris12 https://www.goodreads.com/user/show/169744220-tekneturumarmaris12 https://tr.gravatar.com/tekneturumarmaris https://tr.pinterest.com/tekneturumarmaris/ https://www.mapleprimes.com/users/Tekneturumarmaris12 https://medium.com/@tekneturumarmaris https://www.ted.com/profiles/44988590 https://www.infragistics.com/community/members/37de8784fb5b47702f1171b82d8563806f0b3891?_ga=2.109262277.1993449671.1694271709-2097672956.1694271709 https://www.metooo.io/u/64fc8a6734cbec3769ea8344 https://app.roll20.net/users/12395607/tekneturumarmaris12-t https://list.ly/tekneturumarmaris/activity https://giphy.com/channel/Tekneturumarmaris12 https://www.tumblr.com/tekneturumarmaris12 https://dzone.com/users/4990662/tekneturumarmaris12.html https://www.creativelive.com/student/tekneturumarmaris12-tekneturumarmaris12?via=accounts-freeform_2 https://gab.com/Tekneturumarmaris12 https://sketchfab.com/Tekneturumarmaris12 https://www.flickr.com/people/199112151@N03/ https://hub.docker.com/u/tekneturumarmaris12 https://profiles.wordpress.org/tekneturumarmaris12/ https://wefunder.com/tekneturumarmaris12 https://seedandspark.com/user/tekneturumarmaris12-01h9xbgjv994n03gg3f5vd32qf https://calis.delfi.lv/blogs/posts/209969-httpstekneturumarmariscomtr/lietotajs/313497-tekneturumarmaris12/ https://os.mbed.com/users/tekneturumarmaris12/ https://notionpress.com/author/923133# https://my.desktopnexus.com/Tekneturumarmaris12/ https://guides.co/a/tekneturumarmaris12-tekneturumarmaris12/ https://www.bahamaslocal.com/userprofile/1/241117/Tekneturumarmaris12.html http://molbiol.ru/forums/index.php?showuser=1297475 https://www.credly.com/users/tekneturumarmaris12-tekneturumarmaris12/badges https://www.facer.io/user/aeyPVCPR5z https://ko-fi.com/tekneturumarmaris12#paypalModal https://mastodon.online/@Tekneturumarmaris12 https://devpost.com/tekneturumarmaris?ref_content=user-portfolio&ref_feature=portfolio&ref_medium=global-nav http://onlineboxing.net/jforum/user/editDone/250832.page
Keywords
Speech appliances, Cleft lip and palate, Speech bulb obturator, Palatal lift and palatal obturatorIntroduction
CLP are birth defects affecting the face and mouth. A cleft lip is a tiny opening caused by a physical separation or split. A split or opening in the mouth’s roof is known as a cleft palate. It can be unilateral/bilateral/isolated with variations. There are around 250 different types of face clefting disorders, which are among the many congenital birth deformities. Genetic clefts are thought to account for less than 40% of all clefts. Clefting is a multifactorial event with varying etiology. The majority of the time, the reason for CLP is unknown. These situations are unavoidable. Pregnant women who smoke, consume alcohol, or take certain drugs are more likely to give birth to infants with CLP. Parental/family history, obese and diabetic female also contribute to the cause. On the basis of severity of the cleft, children encounter a number of issues including suckling, extreme facial deformities, ear infections, deafness, breathing difficulties, malocclusion, and poor speech [2].
New-borns have the ability to learn the production of sounds on themselves. Tactile-auditory-kinaesthetic feedback loop plays a major role in it. It does so by connecting the acoustic results with sound production's physical repositioning. Infants with a cleft palate, on the other hand, have a hearing loss that affects their auditory system. All of this leads to delays in the formation of speech sounds [3].
Literature Review
Disorders of speech and language
Speech impediment refers to issues with communication and associated areas including articulatory function. Those children who have been affected by cleft palate and have not been treated have a different way of producing sounds, with nasal phenomes (/m/,/n/) being used more frequently for most oral sounds [4].
Because of the mouth-nasal cavity coupling, the utilization of oral noises is required resulting in usage of glottal pauses instead of oral plosives (/p/,/b/,/t/,/d/,/k/,/g/) in cases of patients with open cleft [5].
Dysfluency, articulatory, and phonation abnormalities are some of the terms used to describe these conditions. In cleft palate speaking, velopharyngeal competence is a key factor of articulatory performance. Following primary cleft palate surgery, 75 percent of individuals attain velopharyngeal competence, which increases to 90-95 percent with focused additional surgeries [6]. VPI is a neuro motor or physiological illness in which the velopharyngeal structures move inadequately.
Although perceptual assessments provide essential information in the diagnosis of speech disorders, it has been discovered that therapists can extend their senses and objectify their perceptual findings by incorporating instrumental methods into the diagnosis process [7].
Differential diagnosis is critical in determining whether surgery or non-surgical treatment is the best option. When someone's speech sounds nasal, it's usually a sign that they have VPD. However, velopharyngeal structures must be examined during speech in order to pinpoint the cause of VPD. Doctors can observe the velopharyngeal mechanism from the side and front using a video x-ray machine (video fluoroscopy). On the basis of the disorder's nature, therapists can devise the best treatment strategies. These patients can be treated comprehensively either surgically or non-surgically. Surgical treatment can alter the size and form of the velopharyngeal space, allowing air and sound to exit the mouth rather than enter the nose when the kid speaks.
Operation may not be the finest treatment for persons with VPD in rare instances, either because they are too sick to undergo anaesthesia or surgery. In certain circumstances, a detachable appliance that aids velopharyngeal closure during speaking may be used to treat VPD. The non-surgical procedure has been addressed in this article. The speech bulb obturator, palatal lift, and palatal obturator are the three primary appliances mentioned.
Historical background
Dentists have been creating devices to fix abnormalities in the hard palate since the early 16th century. Prosthodontists today, like their predecessors, are dedicated about assisting people who have an oral cleft. Many people with cleft palate are prescribed prosthetic speech appliances as a preliminary or secondary treatment. In the dissertation, the phrases "obturator" and "speech appliance" are both employed.
Hyper nasality caused by velopharyngeal insufficiency can be corrected with speech equipment like palatal lift prosthesis or a pharyngeal bulb (VPI).
A number of writers have confirmed through a study that velopharyngeal structures show greater mobility in response to speech devices [8]. However, those claims were predicated on analytical views of either nasal emission or reduced hyper nasality, or both rather than physiological evidence of the changes in velopharyngeal function linked with the appliance's implantation and removal. This type of movement improvement has been attributed to the speech appliance's resistance to the muscles and toughness is built by exercising the muscles against defiance [9].
Necessities of the prosthesis
- The appliance must be according to the sufferer specific oral and facial balance.
- Most other restorations should have less retention and support than appliances.
- The appliance's weight and size should be maintained to a minimum.
- The prosthesis should not cause soft tissue displacement.
- The materials chosen should be affordable to repair, extend, and reduce.
Indications for prosthesis
A prosthetic appliance is indicated in cases where the patient shows:
- A broad cleft.
- Soft palate and pharyngeal neuromuscular deficit.
- Surgery that is postponed or fails.
- Incompetent palate-pharyngeal mechanisms.
Prosthetic management
Prosthetic devices: Appliance prosthetic gadget prosthesis is a prefabricated replacement for missing or deformed bodily component. These aids help the patient with key functions including feeding and velopharyngeal closure while also improving their appearances [10].
Speech tools: When surgical management of Velopharyngeal Incompetence/insufficiency (VPI) or symptomatic fistula is not an alternative, prosthetic therapy might be a useful approach [11]. A “speech bulb obturator”, “palatal lift”, and “palatal obturator'' are all language appliances that can help in speech production. The palatal obturator closes defects in the hard palate/velum, whereas the speech bulb obturator and palatal lift address velopharyngeal insufficiency and incompetence, respectively.
Palatal lift: Palatal lift is advised in circumstances of velopharyngeal incompetence, where the velum’s length is normal but shows insufficient or/and inconsistent velar elevation for valve closure. In an ideal condition, there must be enough thickness and velar length, as well as good lateral pharyngeal wall movements.
The palatal lift device is designed in such a way that the anterior base kept in place by a finger like tailpiece that extends to the velum and by the teeth. The tailpiece grows to the velum as therapy begins.
When the velum is very flaccid, this form of prosthesis functions best, allowing the lift to occur without resistance. In addition, normal velum elevation can cause the prosthesis to become loose [12].
The palatal lift can benefit dysarthria individuals when hyper nasality is the root cause of language intelligibility and articulation, phonation, and breathing are mildly compromised [13].
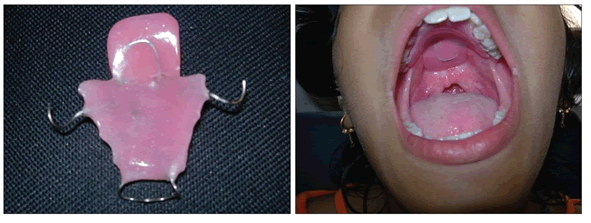
Palatal lift can significantly ameliorate air support and lessen hyper nasality support by restricting air gaps past the nasal route. It can even enhance magnitude by diverting sound towards the oral cavity and preventing it from being absorbed by the rhinal and pharyngeal cavity tissues. Individuals with severe apraxia that disrupts velopharyngeal coordination may benefit from a palatal lift (Figure 1) [14].
Figure 1: Palatal lift.
Characteristics of a palatal lift prosthesis
- It developed as a result of speech issues caused by a lack of palatopharyngeal closure [15].
- During regular speech and deglutition, it is utilized to raise the soft palate to its most optimal position, allowing the pharyngeal wall to close the gap.
- Retention is the most important factor in a successful palatal lift.
- The ideal teeth for palatal lift development are the posterior teeth.
There are two prosthodontic procedures available:
- The palatal lift prosthesis.
- Pharyngeal section prosthesis/combination palatal lift.
Palatal obturator: A “palatal obturator” is a detachable prosthetic tool used to sheath an open palatal defect that causes nasal regurgitation in the course of feeding or is symptomatic through speech [16]. Palatal obturators are most commonly used to close a palatal fistula.
Although palatal fistulas are not as common as they once were, they continue to be a concern for certain people. The surgical closure of a fistula is routinely postponed so that it can be done as part of another surgery. If the patient makes any decision which will lead to delay in surgical therapy or in the case when patient is not ready to correct the fistula surgically, obstruction may be explored for correction [17]. The palatal obturator is composed of acrylic and looks like a dental retainer. Extra acrylic on the top of the appliance, on the other hand, fits snuggly into the deficit zone.
This stops liquids or air pressure from entering the nasal cavity. If a big obturator is required to fill gap, it needs to be flattened so that its weight does not impede with retention (Figures 2 and 3) [18, 19].
Figure 2: Palatal obturator.
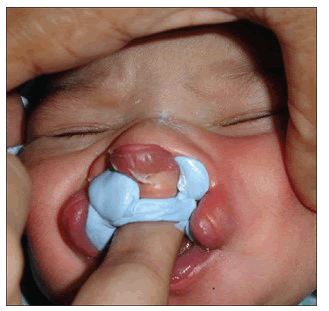
Figure 3: Impression of cleft palate being made.
Obturators for congenital palatal defect
- A simple base plate type helps to correct swallowing and digesting by closing the entrance of the hard palate.
- Obturator with a tail is a speech appliance that corrects speech by restoring soft and hard palate deformities as well as velopharyngeal extension.
Surgical obturator: The surgical obturator is a base plate appliance that is made from the patient's preoperative case and implanted during surgery.
This prosthesis will need to be adjusted on a regular basis to account for rapid soft tissue changes that occur within the defect during wound organization and healing.
Soft palate obturators
- Immediate surgical obturator-To keep the operative packing in place. The rung of hard palate determines superior inferior plane of obturator, while the soft palate determines the width.
- Delayed surgical obturator-Delayed surgical obturator is suitable for patients with modest deformities of the soft palate's posterior or lateral borders.
- Definitive prosthesis-With a final prosthesis, patients with extensive mobility of the residual palate pharyngeal complex during function have a strong chance of achieving normal speech.
Pharyngeal obturator/speech aid prosthesis
It creates a barrier between the nasopharynx and the oropharynx by extending beyond the remnant soft palate. It fills in the gaps in the soft palate without displacing it. It provides a stable framework.
Meatus obturators: To obturate the posterior nasal conchae, meatus obturators protrude vertically from the posterior part of the prosthesis. It is utilized in patients who have significant soft palate abnormalities and a powerful gag reflex. The nasality improves once the prosthesis is placed.
The palatal obturator appliance closes off the nasal passage from the oral orifice by filling an oronasal hole. This enables the patient to exert intraoral pressure in order to produce speech sounds. When used correctly and at a young age, an obturator can assist a kid in developing proper articulation placement rather than compensatory output [20].
Discussion
Speech bulb obturator
A velopharyngeal insufficiency is treated with a speech bulb obturator, which is a detachable device. It's even been used to treat velopharyngeal insufficiency [21].
A speech bulb obturator, like other types of appliances, can be used with partial or complete dentures [22].
These are a viable treatment option for adults who have had oropharyngeal cancer or other maxillary malignancies treated with ablative surgery or radiation [23-25]. They can also be used by those who have had major damage to their palate and are unable to have surgery.
A space bulb obturator is used for speaking. It does so by sealing off the nasal antrum from oral fissure. It is also used to fill the nasopharyngeal breach. This, like a palatal obturator, allows the patient to create speech sounds by impounding intraoral pressure. Hyper nasality can be controlled or eradicated as well.
Prosthetic contraindications
- Surgical repair is only possible when the defect is closed surgically.
- Individuals who are mentally ill.
- In circumstances where there is a lot of caries.
- For patients who refuse to cooperate.
Conclusion
The therapy of certain cleft palate patients with prosthetics is a crucial aspect of a multidisciplinary approach to tackling the various difficulties associated with complete health.
Despite the fact that correcting the palate improves the prognosis for normal speech development, the child is still at risk for articulation issues, abnormal resonance as a result of malocclusion and VPI. Throughout preschool and early childhood, speech and resonance, as well as language, should be regularly monitored.
Finally, our data shows that when used with expertise and professional judgement, the modified prosthetic speech appliance is a considerable improvement and a helpful addition to the orthodontist's cleft arsenal.
References
- Kamble RH, Shrivastav SS, Sangtani J, et al. Assessment of Change in SOC of Parents Participating in the Treatment of Their Children Having Cleft Lip and Palate Anomalies. J Evo Med Dent Sci 2020; 9:2447-2452.
- Gosavi S, Shrivastav S, Kamble R, et al. Multidisciplinary Approach for the Management of a Case of Bilateral Cleft Lip and Palate Baru's Score 5 Using Modified Dentoalveolar Distractor. J Evo Med Dent Sci2020; 9:3276-3280.
- Chapman KL, Hardin-Jones M, Halter KA. The relationship between early speech and later speech and language performance for children with cleft lip and palate. Clin linguist phon 2003; 17:173-197.
- Kalambe S, Jain S, Disawal A, et al. Supra-Threshold Hearing Sensitivity Disorders and Mild Permanent Hearing Loss: Neglected Cause of Hidden Hearing Loss and Speech Defects. Ind J Otolaryngol Head Neck Surg 2020; 1-9.
- Smith BE, Kuehn DP. Speech evaluation of velopharyngeal dysfunction. J Craniofac Surg 2007; 18:251-261.
- Marrinan EM, Labrie RA, Mulliken JB. Velopharyngeal function in nonsyndromic cleft palate: relevance of surgical technique, age at repair, and cleft type. Cleft palate craniofac j 1998; 35:95-100.
- Peterson HA, Marquardt TP. Appraisal and diagnosis of speech and language disorders. Prentice Hall. 1990.
- Beery QC, Rood SR. Pharyngeal wall motion in prosthetically managed cleft palate adults. Cleft palate j 1983; 20:7-17.
- Rosen MS, Bzoch KR. The prosthetic speech appliance in rehabilitation of patients with cleft palate. J Am Dent Assoc 1958; 57:203-210.
- Bhola RD, Pisulkar SG, Godbole SA, et al. Maxillofacial Prosthesis for Combined Intra and Extra-Oral Defect-A Case Report. J Evo Med Dent Sci 2021; 10:550-555.
- Gallagher B. Prosthesis in velopharyngeal insufficiency: effect on nasal resonance. J commun disord 1982; 15:469-473.
- Reisberg DJ. Dental and prosthodontic care for patients with cleft or craniofacial conditions. Cleft palate craniofaci j 2000; 37:534-537.
- Shifman A, Finkelstein Y, Nachmani A, et al. Speech-aid prostheses for neurogenic velopharyngeal incompetence. J prosthet dent 2000; 83:99-106.
- Hall PK, Hardy JC, Lavelle WE. A child with signs of developmental apraxia of speech with who palatal lift prosthesis was used to manage palatal dysfunction. J Speech Hear Disord 1990; 55:454-460.
- Premkumar S. Clinical application of palatal lift appliance in velopharyngeal incompetence. J Indian Soc Pedod Prev Dent 2011; 29:70.
- Walter JD. Obturators for cleft palate and other speech appliances. Dent update 2005; 32:217-222.
- Pinborough-Zimmerman J, Canady C, Yamashiro DK, et al. Articulation and nasality changes resulting from sustained palatal fistula obturation. Cleft palate craniofac j 1998; 35:81-87.
- Abu-Hussein M, Watted N, Hussien E, et al. A Feeding Appliance for a New-born Baby with Cleft Palate. In J Dent Med Sci Res 2017; 1:6.
- Chandna P, Adlakha VK, Singh N. Feeding obturator appliance for an infant with cleft lip and palate. J Indian Soc Pedod Prev Dent 2011; 29:71.
- Raju H, Padmanabhan TV, Narayan A. Effect of palatal lift prosthesis in individuals with velopharyngeal incompetence. In J Prosthod 2009; 22.
- Sun J, Li N, Sun G. Application of obturator to treat velopharyngeal incompetence. Chinese Med J 2002; 115:842-845.
- Abreu A, Levy D, Rodriguez E, et al. Oral rehabilitation of a patient with complete unilateral cleft lip and palate using implant-retained speech-aid prosthesis: clinical report. Cleft palate craniofacJ 2007; 44:673-677.
- Yenisey M, Cengiz S, Sankaya S. Prosthetic treatment of congenital hard and soft palate defects. Cleft palate craniofac J 2012; 49:618-621.
- Dhakshaini MR, Pushpavathi M, Garhnayak M, et al. Prosthodontic management in conjunction with speech therapy in cleft lip and palate: A review and case report. J Int Oral Health JIOH 2015; 7:106.
- Jaiswal S, Kheur M, Lakha T. Management of a velopharyngeal defect with hollow speech bulb prosthesis. J Interdisciplinary Dent 2020; 10:117.
Author Info
Jigna Kachaliya*, Pallavi Daigavane, Priyanka Niranjane, RH Kamble and Tirth Bhutada
Department of Orthodontics, Sharad Pawar Dental College and Hospital, Datta Meghe Institute of Medical Sciences (Deemed to be University) Sawangi (Meghe), Wardha, Maharashtra, IndiaReceived: 23-Apr-2022, Manuscript No. JRMDS-22-49460; , Pre QC No. JRMDS-22-49460; Editor assigned: 02-May-2022, Pre QC No. JRMDS-22-49460; Reviewed: 16-May-2022, QC No. JRMDS-22-49460; Revised: 30-Jun-2022, Manuscript No. JRMDS-22-49460; Published: 07-Jul-2022