Research - (2019) Volume 7, Issue 1
Study of CT Scan Findings in Children with Seizures in Tabriz Children's Hospital, Iran
Parisa Hajali Oghli* and Mehdi Hafezi Nasab Jolgeh
*Correspondence: Parisa Hajali Oghli, Tabriz University of Medical Sciences, Tabriz, Iran, Email:
Abstract
Introduction: Seizures occur in 3 to 4 percent of children under the age of 6 years. Although it’s clinical manifestation can be very worrying for families, its prognosis is generally good and in some cases it may lead to epilepsy.
Aim: The aim of this study was to determine the CT scan findings of children with seizure in Tabriz Children's Hospital.
Materials and Methods: In this study patients who were sent to children's CT scan for seizure and epilepsy were enrolled. Before performing, questions included age, sex, clinical symptoms, type of seizure, history of seizure, EEG findings, family history of seizure, duration of seizure were asked. Then, patients who have a CT scan indication were sent to do so. After performing the CT scan, all of the information, including the CT scan report, entered the statistical analysis program.
Results: According to CT scan findings, 28 patients (28%) had abnormal findings and 72 (72%) had normal findings. Mean ± SD of patients’ age with normal CT scan findings was 3.76 ± 3.02 years and in patients with abnormal CT scan findings was 3.17 ± 2.85 years. There was significant relationship between CT scan findings and the age of the patients (p=0.001). Mean ± SD of duration of seizure history with normal CT scan finding was 23.79 ± 3.52 months and in patients with abnormal CT scan findings was 21.93 ± 1.87 months. There was statistically significant relationship between CT scan findings and duration of seizure history in the studied patients (p=0.001). In boys, the findings of CT scan were normal in 39 patients (67.9%) and abnormal in 18 patients (32.1%). In girls’ population 34 patients (77.3%) had normal CT scan findings and in 10 patients (22.7%) CT scan findings were abnormal. There was no statistically significant relationship between gender and CT scan findings (p=0.372). Patients with normal CT scan findings also had normal EEGs. In contrast to 28 patients with abnormal CT scan findings, 17 patients (60.7%) had normal EEG and 11 patients (39.3%) had abnormal EEG findings. There was a significant correlation between CT scan and EEG findings in seizure detection (p=0.001). The most common cause of abnormal CT scan findings was cerebral edema, with the frequency of 7 patients (25%).
Conclusion: CT scan findings are more abnormal in children with lower age seizures and longer seizure history. Also, in the present study, the increased frequency of localized seizures indicates that in our study, the majority of hospitalized patients had.
Keywords
CT scan, Focal epilepsy, Febrile, Children
Introduction
Convulsion caused by fever is a type of convulsion associated with fever above 39°C. Fever is also due to the presence of an infectious center in a part other than the brain. This convulsion usually begins with a sudden increase in body temperature, and is often seen as a febrile disease initially and is usually associated with upper respiratory system infections such as colds. Children are highly prone to convulsion because their brain and nervous systems have not yet been matched. The febrile convulsion is a tonic-clonic and generalized one. The first stage of convulsion usually lasts about half a minute and includes symptoms such as reduced consciousness, firmness of the body and limbs, respiratory depression for about 30 seconds (after this time, when breathing starts again, it may be very superficial) and involuntary urination or defecation. The second phase of convulsion often takes less than five minutes. At this stage, the child is still unconscious and the symptoms include face or limb leaping (tonic-clonic movements) and the return of the eyes upward. After completing the second phase, the child becomes conscious and then may sleep for one to two hours. Waking up, he may be confusing, sleepy and irritable. About a third of children, who have a febrile convulsion attack, will be exposed to another attack during six months. The majority of children with febrile convulsions have no problems in the long run, and few may have epilepsy in the future.
The febrile convulsion occurs in children between one month and six years of age at temperature above 38°C. Patients with this type of convulsion have no symptoms of central nervous system (CNS) infection or electrolyte imbalance and previous history of febrile convulsion. Although it’s clinical manifestation can be very worrying for families, its prognosis is generally good and in some cases it may lead to epilepsy [1-4]. Fever and convulsion are divided into two groups based on clinical symptoms:
1. Simple fever and convulsion: Convulsions lasting less than 10-15 minutes, as generalized tonic-clonic and they do not take place in 24 hours more than one time [5].
2. Complex fever and convulsion: Focal convulsions, lasting over 15 minutes with neurological symptoms at the post-convulsion stage [5,6].
Some studies have reported that CT scan may be disabled to detect about 40% of the cerebral structural lesions with convulsions, including small tumors and vascular malformations. Therefore, it is believed that a CT scan is a suitable diagnostic modality when a MRI is not available. Therefore, so far, the determination of indications for CT scan in children with primary convulsion without fever has been discussed [7,8].
Frequent convulsion attack, called epilepsy, in every 200 children occurs for one person. During an epilepsy attack, the brain waves become disordered and irregular. Consequently, disturbances of consciousness and sometimes uncontrolled movements occur. Apart from epilepsy, there are many other causes for convulsion, one of which is fever. It should also be noted that the occurrence of a single convulsion is not an indication of epilepsy. Sometimes the cause of epilepsy is a build-up disorder in the brain, but in most cases, there is no specific cause. In some afflicted children, the convulsion attacks occur after a sensory stimulus, such as bright and intense light, and in others there is no starting factor. Different types of epileptic convulsions have already been identified and defined. In children, the tonic-clonic convulsions are more common, more than three-quarters of children with epilepsy suffer from these convulsions, small epilepsy or absence is the second most common epilepsy in children.
A study was done by Adams et al. to investigate the results of children's cerebral CT scan and its association with the cause of CT scan requests. This study concluded that CT scan in meningitis without a disturbance in consciousness and the first generalized convulsion with normal neural examination, headache without risk symptoms was not very helpful and MRI is more useful in detecting the developmental delay and structural disorder of the brain [9].
In a study done by Shahabi et al. to investigate the rate of ischemic brain lesions and brain imaging findings in neonates with convulsion, it was concluded that the stroke is the second most common cause of convulsion attacks in the newborn infants after asphyxia. Brain CT was also a very important diagnostic tool in this study. Brain imaging (CT Scan/MRI) was recommended for all neonates with convulsions that have no asphyxia and are seemingly healthy in the clinical examination, also, have no other causes for convulsion [10]. A study was conducted by Abbasi et al. to investigate the findings of brain CT scans in children with convulsion referring to Kashan's treatment centers; the findings from medical history, neurological exam and CT scan were registered in questionnaires, then these findings were extracted and analyzed. The study concluded that the most common abnormal finding in CT scan of children was the epilepsy of brain atrophy. Also, in the epileptic children with mental, motor disorder, and the cases with an onset of convulsion at lower ages, the chance of abnormal CT scan is higher [11]. In the study of Maytal et al., conducted on the morbidity and mortality in children with state convulsion, 193 children with state convulsion were evaluated for 13.2 months out of which, 97 patients were participated in the study, with an age range between 1 month and 18 years with an average of 5 years. The cause of state convulsion was idiopathic in 46 patients, remote symptomatic in 45 cases, febrile in 46 cases, acute symptomatic in 45 cases and progressive neurology in 11 cases. In this study of mortality and morbidity, the sate convulsion was estimated low [12].
The aim of this study was to evaluate the CT scan of children with convulsion in Tabriz Children's Hospital during 2016.
Materials and Methods
The study was descriptive-analytic; all patients who had been diagnosed with convulsion and epilepsy in the CT scan ward in 2012-2016 were participated in the study during one year. Before performing CT scan, the questions were proposed about the checklist included age, sex, clinical symptoms, type of convulsion, history of convulsion, EEG findings, and family history of convulsion and duration of convulsion. They were entered in the study done as census and one by one. Then, the patients who have a CT scan indication were sent to do so. After performing the CT scan, all of the information, including the CT scan report, was entered in the statistical analysis program. According to previous studies, considering the alpha value of 0.05 and the power of 80% and maximum acceptable error of 0.1 by G. Power software, 100 patients as Sample size were required to enter the study. Considering the possibility of quitting the study by patients or insufficient data on this subject, 120 patients participated in the study (Figure 1).
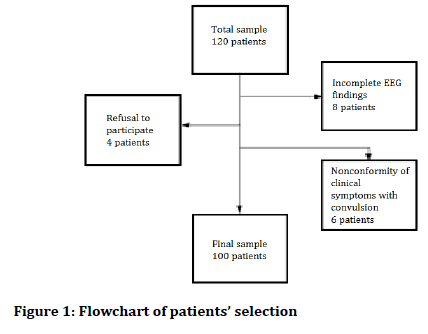
Figure 1. Flowchart of patients’ selection.
The criteria inclusion for entering the study included the parents' permission to participate in the study, the presence of CT indication, and the presence of family history of convulsion and the exclusion criteria are follows as: the parents' refusal to participate in the study, the incompleteness of the EEG findings, and the nonconformity of clinical symptoms with convulsion. By the inclusion/exclusion criteria, 20 patients were excluded because of the nonconformity of clinical symptoms with convulsion.
The patients were asked questions in the form of a checklist prepared before the study began. Questions included age, sex, clinical symptoms, type of convulsion, history of convulsion, EEG findings, and family history of convulsion and duration of convulsion. The table of variables has been given in Table 1.
| Variables | Scale | Type of variable | Method of control/evaluation | Scientific definition of variable (if necessary) | |||||
|---|---|---|---|---|---|---|---|---|---|
| Quantitative | Qualitative | ||||||||
| Distance-based | Relational | Nominal | Rank-based | Independent | Dependent | Disturbing | |||
| Age | ■ | □ | □ | □ | ■ | □ | □ | Checklist | Year |
| Gender | □ | □ | ■ | □ | ■ | □ | □ | Checklist | Male-female |
| Type of convulsion | □ | □ | ■ | □ | ■ | □ | □ | Checklist | Simple-complicated |
| History of convulsion | □ | □ | ■ | □ | ■ | □ | □ | Checklist | Year |
| EEG findings | □ | □ | ■ | □ | □ | ■ | □ | EEG system | Normal-abnormal |
| Familial history of convulsion | □ | □ | ■ | □ | ■ | □ | □ | Checklist | Yes-No |
| Time of convulsion | ■ | □ | □ | □ | ■ | □ | □ | Checklist | Second-minute |
| CT findings | □ | □ | ■ | □ | □ | ■ | □ | Checklist | Normal-abnormal |
Table 1: Variables
In this study, the information of patients has been confidential and no names of patients have been mentioned. The present study was carried out after being approved at the moral Committee of Tabriz University of Medical Sciences. For all patients, CT scan was requested by Clinicians who did not know about the study. All data were entered into the statistical analysis by SPSS software version 20 and the results were analyzed using Chi square and Fisher tests, and the significance level of p-Value was less than 0.05.
Results
In this descriptive-analytic study, 100 patients were studied. The mean ± standard deviation of the patients' age was 3.60 ± 2.97 years, with a minimum age of 41 days and a maximum age of 13 years. The patients’ age histogram has been shown in Figure 2.
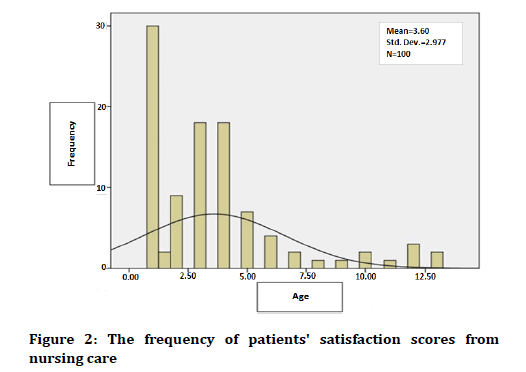
Figure 2. The frequency of patients' satisfaction scores from nursing care.
For the sex distribution, 56 patients were male (56%) and 44 patients were female (44%). Figure 3 shows the sex distribution of the patients under study.
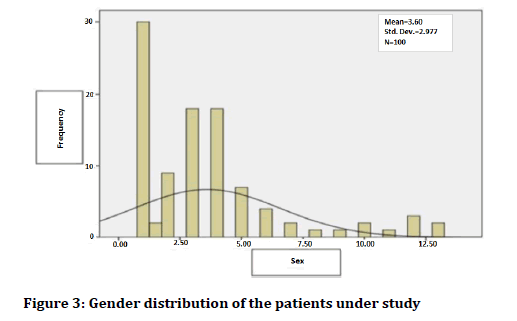
Figure 3. Gender distribution of the patients under study
For convulsion type, 60 patients (60%) had local convulsions and 40 patients (40%) had generalized convulsions. Figure 4 shows the frequency of convulsion types in patients under study by gender.
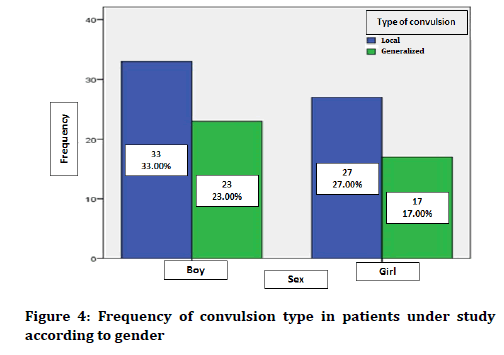
Figure 4. Frequency of convulsion type in patients under study according to gender
In terms of previous convulsion history, 40 patients (40%) had a history of convulsion in the past, and 60 (60%) had no previous convulsion history. Figure 5 shows the status of previous convulsion history in patients, considering convulsion type. The duration of the history of convulsion was 23.51 ± 2.94 months in the patients under study. The minimum duration of According to the obtained data, 11 patients (11%) had abnormal EEG findings, and 89 patients (89%) had normal EEG results. Figure 6 shows the status of EEG findings based on the type of convulsion.
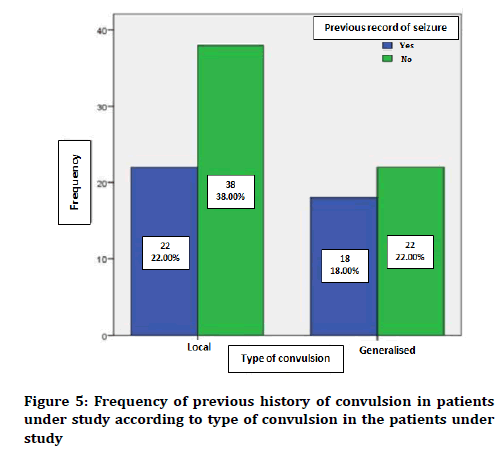
Figure 5. Frequency of previous history of convulsion in patients under study according to type of convulsion in the patients under study
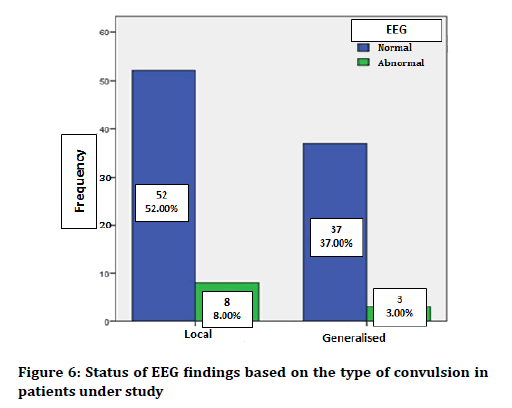
Figure 6. Status of EEG findings based on the type of convulsion in patients under study
In terms of the family history of convulsion, none of the patients had family history of convulsion. Mean ± standard deviation of the duration of convulsion was equal to 2.70 ± 2.14 minutes in the patients under study, with a minimum duration of convulsion of less than 1 minute and maximum convulsion duration of 11 minutes. The mean ± standard deviation of the age of patients with local convulsion was equal to 3.43 ± 3.14 years and in the type of generalized convulsion was 3.85 ± 2.73 years. Block diagram of age distribution in the convulsion types in patients under study has been shown in Figure 7.
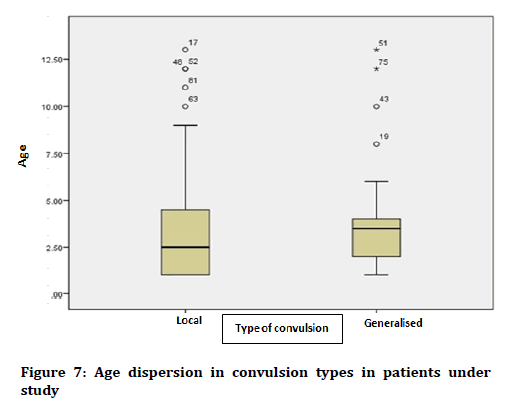
Figure 7. Status of the presence or absence of fever in the types of convulsion in the patients under study
In terms of the presence of fever, 28 patients (28%) had fever and convulsion, but 72 (72%) had no symptoms of febrile convulsion. Figure 8 shows the presence or absence of fever in convulsion types in the patients under study.
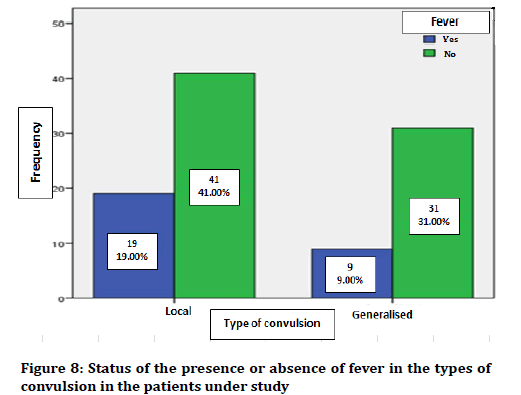
Figure 8. Surgical training questionnaire
In terms of CT scan findings, 28 patients (28%) had abnormal findings, and 72 patients (72%) had normal findings. Figure 9 shows the frequency of CT scan findings in patients under study.
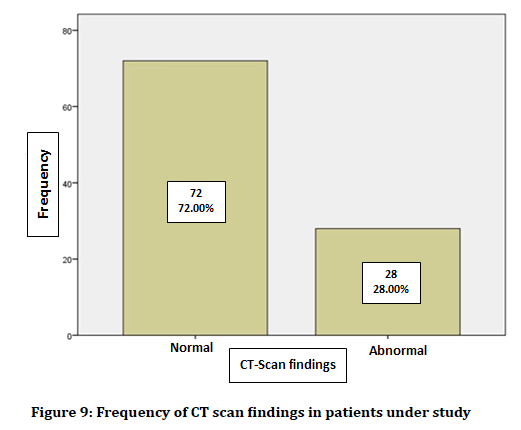
Figure 9. Frequency of CT scan findings in patients under study
The mean ± standard deviation of patients’ age with normal CT scan finding was 3.76 ± 3.02 years and in the patients with abnormal CT scan findings, it was equal to 3.17 ± 2.85 years. There was a significant correlation between CT scan findings and the age of the patients (p=0.001), so that the abnormal findings of CT scan increase as the patients’ age decreases. Mean ± SD of the duration of convulsion history with the normal CT scan finding was equal to 23.79 ± 3.52 months and in the patients with abnormal CT scan findings was 21.93 ± 1.87 months. There was no statistically significant relationship between CT scan findings and duration of convulsion history in the patients under study (p=0.001). The findings of CT scan of male patients were normal in 39 patients (67.9%) and abnormal in 18 patients (32.1%). In female patients, 34 patients (77.3%) had normal CT scan findings and 10 patients (22.7%) were abnormal ones. There was no statistically significant relationship between gender and CT scan findings (p=0.372). Figure 10 shows the frequency of distribution of CT scan findings according to the gender of patients.
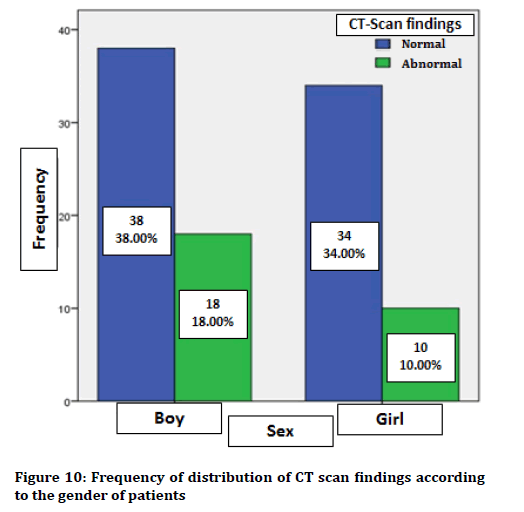
Figure 10. Frequency of distribution of CT scan findings according to the gender of patients
Patients with normal CT scan findings also had normal EEGs. In contrast, of 28 patients with abnormal CT scan findings, 17 patients (60.7%) had normal EEG and 11 patients (39.3%) had abnormal EEG. There was a significant correlation between CT scan finding and EEG in convulsion detection (p=0.001). Figure 11 shows the distribution frequency of CT scan findings in relation to EEG findings in the patients under study.
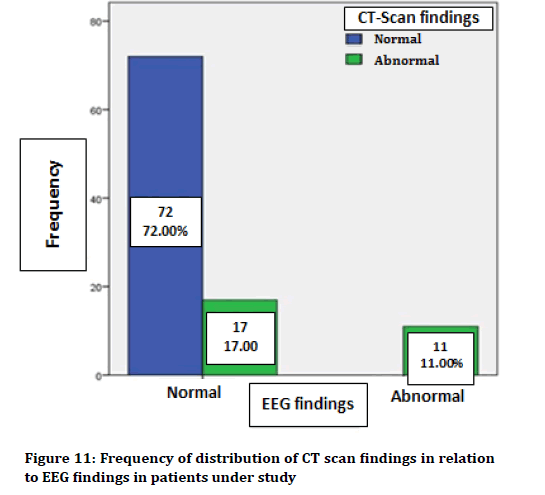
Figure 11. Frequency of distribution of CT scan findings in relation to EEG findings in patients under study
The findings obtained for patients with abnormal CT scans have been presented in Table 2, according to age, sex, type of convulsion, history of convulsion and EEG disorder.
| Row | Age (years) | Gender | Type of convulsion | History of convulsion | EEG |
|---|---|---|---|---|---|
| 1 | 31 days alt | Male | Local | No | Normal |
| 2 | 7 years | Female | Local | Yes (6 months) | Normal |
| 3 | 3 years | Male | Local | No | Normal |
| 4 | 3 years | Female | Generalized | No | Normal |
| 5 | 6 years | Male | Local | Yes (68 months) | Normal |
| 6 | 1.5 years | Female | Generalized | Yes (8 months) | Normal |
| 7 | 7 years | Male | Local | Yes (15 months) | Normal |
| 8 | 4 years | Male | Generalized | Yes (beginning of birth) | Abnormal |
| 9 | 1 years | Male | Local | Yes (beginning of birth) | Abnormal |
| 10 | 3 years | Female | Local | Yes (beginning of birth) | Abnormal |
| 11 | 6 months | Male | Local | No | Abnormal |
| 12 | 4 months | Female | Local | Yes (4 months) | Normal |
| 13 | 6 months | Male | Local | No | Normal |
| 14 | 3 years | Male | Local | No | Normal |
| 15 | 1 year | Female | Local | Yes (8 months) | Normal |
| 16 | 3 years | Male | Local | Yes (15 months) | Normal |
| 17 | 4 years | Male | Generalized | Yes (48 months) | Abnormal |
| 18 | 1 year | Male | Local | Yes (15 months) | Abnormal |
| 19 | 3 years | Female | Generalized | Yes (29 months) | Abnormal |
| 20 | 13 years | Male | Local | No | Abnormal |
| 21 | 1 year | Male | Local | No | Normal |
| 22 | 8 years | Male | Generalized | No | Normal |
| 23 | 7 years | Female | Local | Yes (6 months) | Abnormal |
| 24 | 3 years | Male | Local | No | Normal |
| 25 | 1 year | Female | Local | Yes (18 months) | Abnormal |
| 26 | 1 year | Male | Generalized | No | Normal |
| 27 | 1 year | Male | Local | No | Normal |
| 28 | 7 years | Female | Local | Yes (7 months) | Abnormal |
Table 2: Study of patients with abnormal CT scan results according to age, gender, type of convulsion, history of convulsion and EEG disorder
The normal findings of CT scan with convulsion symptoms including normal brain CT scan and paranasal sinus opacity were observed in 9 cases. According to Table 2, the abnormal CT scan findings have been discussed below.
1. The brain mass of Frontal and Hydrocephalic lobe-Diagnosis: Frontal lobe cerebral mass (1 case).
2. Reduced cerebellar density, loss of differentiation of white and gray moon, cerebellar ventricles-Diagnosis: Cerebral edema (9 cases).
3. Reduction of parenchyma and brain volume along with calcification-Diagnosis: Sturge- Weber (2 cases).
4. Gluosis in the parasagittal areas of the two sides-Diagnosis: Sagittal sinus thrombosis (1 case).
5. Spacing of cerebrospinal fluid and ventricular system, reducing brain parenchyma volume- Diagnosis: Parenchymal atrophy (6 cases).
6. Severe reduction of parenchymal volume of the brain, porencephalic cysts in both hemispheres, severe periventricular calcification-Diagnosis: Prenatal injury and TORCH syndrome (4 cases).
7. Gallon venous aneurysm with venous thrombosis (1 case).
8. One case of lenticular density loss in the shape of the right and the posterior part of the right frontal lobe; one case of loss of density of the parotid occipital area-Diagnosis: Arterial infarction (2 cases).
9. Corpus callosum agenesis, subdural effusion with a slightly higher density than CSFDiagnosis: Meningitis (2 cases).
Discussion
Convulsion is a sudden disorder in the brain function, which can be manifested as an abnormal, sensory, behavioral movement, or a disorder of consciousness; it is a sign of an underlying disease of the central nervous system [13]. Convulsion is one of the most common neurological manifestations in children, with an incidence of 4-6 per thousand children [14]. Although the occurrence of convulsion without a stimulus such as high fever, is often considered to be a chronic convulsion disorder or epilepsy, less than half of these children will be exposed to secondary convulsions [15]. The presence of two non-stimulated convulsions over a period of more than 24 hours suggests an epileptic disorder in the brain that may lead to convulsions in the future [16,17]. Studies conducted in Iran indicate a high prevalence of convulsion in Iranian society; in a study conducted by Nasehi et al. in 2009 in children under the age of 12 years in Tehran, the prevalence of convulsion in the whole lifetime was 32 people per 1000 population; this was reported in boys more than girls [16]. Consistent with this study, in the current study, the convulsion prevalence was higher in boys than in girls, while the prevalence of convulsions in all life (not counting febrile convulsion) was reported to be 2 to 5 percent [18].
The febrile convulsion also has an incidence of 1 child per 15,000 children. The probability of frequent convulsions in cases such as convulsion at the age under 15 months, the frequent fever, so that if convulsions occur in the early stages of a fever in which the body temperature still is low, the risk of recurrence of convulsion and the continuation of further attacks will be high [19]. To investigate the cause of convulsion, some various diagnostic measures are needed, including CT scan to monitor the structure of the brain [14]. Several studies have been carried out on CT scan changes in children with convulsion; 30 to 60% of children with convulsions have had abnormal findings in CT scan [20,21]. In most of these studies, the most common finding in CT scan was brain atrophy. In the current study, 28 patients (28%) had abnormal CT scans; the most common abnormal finding was related to cerebral edema with the frequency of 9 patients (32.15%) and the second finding was the parenchymal atrophy with a frequency of 6 cases (21/5%). In a study conducted by Trainor et al. to investigate the findings of brain CT scans in children with convulsion, the findings of this research showed that 46 patients (43%) had abnormal CT scans. The most common abnormal finding was the cerebral atrophy with the frequency of 33 people (71.7% of abnormal cases and 30.8% of all patients). Children under one year old had 72%, 1-5 years 46.4% and 5-15 years 27.8% of abnormal CT scan. In children with mental disorder had 88.8% and those with motor impairment 77.75% of abnormal CT scan. In this study, the most common abnormal finding was CT scan of children with epilepsy of cerebral atrophy [22]. It seems that in the epileptic children with mental and motor disorder and the cases with an onset of convulsions at lower ages, the chance of abnormal CT scan is higher and the present study is consistent with the above study. In the study of Razieh et al., the most common abnormalities were brain atrophy with a frequency of 21% and then intracranial hemorrhage with a frequency of 5% [23]. The results show that convulsions are higher in lesions involving cerebral parenchyma. In the present study, the patients admitted to the departments, ICU patients and emergency patients who were admitted to hospital were examined. Therefore, the reason for the difference in the current study was the prevalence of convulsion induced by the cerebral atrophy; in other studies, the parenchymal atrophy has been identified as the most common cause.
In a study conducted by Razieh et al., to examine the results of CT scan of children's brain and its association with the cause of CT scan request, the brain scan images of 40 girls and 60 boys with a mean age of 17.42 years were studied which was normal in 61% of cases. In the current study, the brain CT scan findings were normal in 66.7% of patients. In our study, 57 girls and 63 boys with an average age of 3.38 years were studied. In the above study, the abnormal CT scan findings in infants under one year were significantly higher (p=0.001) [23]. Consistent with the above study, in the current study, there was a significant correlation between age of patients and abnormal CT scan findings (p=0.001), as the age decreases, the abnormal CT scan findings increase. According to the results, it can be concluded that in children with less age-related convulsions, the abnormal CT scan findings are higher.
In a study by Shahabi et al., that was conducted to investigate the rate of ischemic brain lesions and the brain imaging findings in neonates with convulsion, 31 newborn infants who had been hospitalized due to convulsion in the first three days of birth in the neonate and care unit were followed up for a year and examined [10]. The neonates who did not have encephalopathy and seemed healthy at the neurological examination were monitored for 18 months. According to the results of this study, out of 31 neonates who had a convulsion during one year, five people (16%) had convulsions due to ischemic brain lesions. Focal convulsion occurred in three cases and generalized one in two people; it was controlled only by phenobarbital in four patients, but in one case, in addition to phenobarbital, the phenytoin was added. Nervous examination was normal in most neonates other than one who had mild spasticity in the right limbs. Brain ultrasound was unnatural in only one person, while the brain CT scan showed a focal lesion of the brain in every five patients. These focal lesions were more on the left side. The brain bar was abnormal in three cases. In the follow-up of patients, one of them experienced severe mental and motor disorder while the other one had a slight delay in neuronal development. The study concluded that the stroke is the second most common cause of convulsion attacks in the newborns after asphyxia. Brain CT was also a very important diagnostic tool in this study. Brain imaging (CT scan/ MRI) was recommended for all neonates with convulsions that had no asphyxia and were seemingly healthy in the clinical examination as well as they had no other causes for convulsion [10]. In the current study, the convulsion occurred in two patients with brain edema in the context of metabolic disease and two cases of arterial infarction. In the current study, in patients with abnormal CT scan findings, 21 cases had local convulsions and 7 patients had generalized convulsions. The results of the present study indicate that the increased frequency of local convulsions shows that in the present study, the hospitalized patients were more exposed to local convulsion. The patients with normal CT scan findings also had normal EEGs. In contrast, of 28 patients with abnormal CT scan findings, 17 patients (60.7%) had normal EEG and 11 patients (39.3%) had abnormal EEG. There was a significant statistical correlation between CT scan finding and EEG finding in detecting convulsion (p=0.001).
Conclusion
According to the results obtained in this study, it can be concluded that in the lower age children with convulsion and history of longer convulsion, the abnormal CT scan findings are more frequent. Also, in the present study, the increased frequency of local convulsion indicates that the hospitalized patients were more frequently exposed to local convulsion.
In our study we don’t considered congenital malformations such as metabolic diseases or fetal noxious during pregnancy and delivery; that can affect the results of study. Lastly, it’s good to matching drug profiles of patents with seizure types and CT scan results that can be an arguable topic.
Conflict of Interest
The authors declare that there is no conflict of interest regarding the publication of this manuscript.
References
- King MA, Newton MR, Jackson GD, et al. Epileptology of the first seizure presentation: A clinical, electroencephalographic, and magnetic resonance imaging study of 300 consecutive patients. Lancet 1998; 352:1007-11.
- Engel J. A proposed diagnostic scheme for people with epileptic seizures and with epilepsy: Report of the ILAE task force on classification and terminology. Epilepsia 2001; 42:796-803.
- Fisher RS, Boas WV, Blume W, et al. Epileptic seizures and epilepsy: Definitions proposed by the international league against epilepsy (ILAE) and the international bureau for epilepsy (IBE). Epilepsia 2005; 46:470-2.
- Maytal J, Shinnar S. Febrile status epilepticus. Pediatrics 1990; 86:611-6.
- de Flagge Moreno N. Simple febrile seizure, complex seizure, generalized epilepsy with febrile seizure plus, FIRES and new syndromes. Medicina 2013; 73:63-70.
- Yang Y, Mahaffey CL, Bérubé N, et al. Complex seizure disorder caused by Brunol4 deficiency in mice. PLoS Gen 2007; 3:e124.
- Russo A, Scarpini G, Boni A, et al. Relationship between 18F-FDG PET hypometabolism and EEG findings in pediatric focal epilepsy: Visual assessment versus statistical parametric mapping (SPM) and surgical implication. Eur J Paediatr Neurol 2017; 21:e100.
- Yang PJ, Berger PE, Cohen ME, et al. Computed tomography and childhood seizure disorders. Neurology 1979; 29:1084.
- Adams KF, Schatzkin A, Harris TB, et al. Overweight, obesity, and mortality in a large prospective cohort of persons 50 to 71 years old. N Engl J Med 2006; 355:763-78.
- Shahabi D, Fakhraei D, Kazemyan D. Ischemic brain lesions and brain imaging findings in neonates with convulsion. J Pajouhandeh 2008; 13:347-53.
- Abbasi M. A comparative study on the concept of convulsion in traditional Iranian medicine and classic medicine. Avicenna J Phytomed 2015; 5.
- Maytal J, Shinnar S, Moshé SL, et al. Low morbidity and mortality of status epilepticus in children. Pediatrics 1989; 83:323-31.
- Warden CR, Zibulewsky J, Mace S, et al. Evaluation and management of febrile seizures in the out-of-hospital and emergency department settings. Ann Emerg Med 2003; 41:215-22.
- Coté CJ, Karl HW, Notterman DA, et al. Adverse sedation events in pediatrics: Analysis of medications used for sedation. Pediatrics 2000; 106:633-44.
- Baumann RJ. Technical report: Treatment of the child with simple febrile seizures. Pediatrics 1999; 103:e86.
- Nasehi MM, Shamsabadi F, Ghofrani M. Paraclinical findings and treatment response of children with refractory epilepsy in Mofid Children's Hospital in 2007-2008. JMUMS 2010; 20:24-9.
- Freitas A, Casella EB, Valente M, et al. Neonatal seizures: The overlap between diagnosis of metabolic disorders and structural abnormalities. Case report. Arq Neuropsiquiatr 2003; 61:478-81.
- Angus-Leppan H, Parsons LM. Epilepsy: Epidemiology, classification and natural history. Medicine 2008; 36:571-8.
- Raoof R, Esmaeili-Mahani S, Abbasnejad M, et al. Changes in hippocampal orexin 1 receptor expression involved in tooth pain-induced learning and memory impairment in rats. Neuropeptides 2015; 50:9-16.
- Rathor MY, Shahar MA, Omar AM, et al. Assessment of knowledge, attitude and practices of epilepsy patients towards their illness and treatment in a tertiary care hospital in Kuantan Pahang Malaysia. Bangladesh J Med Sci 2017; 16:545-53.
- Baumann RJ, Duffner PK. Treatment of children with simple febrile seizures: The AAP practice parameter. Pediatr Neurol 2000; 23:11-7.
- Trainor JL, Hampers LC, Krug SE, et al. Children with first‐time simple febrile seizures are at low risk of serious bacterial illness. Acad Emerg Med 2001; 8:781-7.
- Razieh F, Mehdi A. The study of the results of children cerebral CT scan and its relation with the cause of CT scan. Horizon of Knowledge 2008; 14:27-36.
Author Info
Parisa Hajali Oghli* and Mehdi Hafezi Nasab Jolgeh
Tabriz University of Medical Sciences, Tabriz, IranCitation: Parisa Hajali Oghli, Mehdi Hafezi Nasab Jolgeh, Study of CT scan findings in children with seizures in Tabriz children's hospital, J Res Med Dent Sci, 2019, 7(1): 170-177.
Received: 02-Jan-2019 Accepted: 08-Feb-2019
