Research - (2021) Volume 9, Issue 7
Study of Serum β-HCG and Lipid Profile in Second Trimester as Predictors of Pre-Eclampsia in a Tertiary Care Teaching Hospital
Meghana Puttaswamy1, Usha Brindhini Mathialagan2*, Ramesh kumar3 and Rathnamala M Desai3
*Correspondence: Usha Brindhini Mathialagan, Department of Obstetrics and Gynaecology, SVIMS-Sri Padmavathi Medical college for women, India, Email:
Abstract
Introduction: Early diagnosis, close antenatal surveillance, and timely intervention are key to the management of Preeclampsia. Our aim was to study the association of serum β-HCG and lipid profile in second trimester in the development of preeclampsia. Methods: 100 pregnant women between 14–20 weeks of gestational age with singleton pregnancy irrespective of parity were selected randomly and serum β-HCG and lipid profile were estimated by chemiluminescent immunometric assay and enzymatic calorimetric test respectively. Regular follow up of cases was done till delivery. Results were analysed statistically. Results: Out of 100 women who enrolled in the study 92 women were completely followed till term. Eight women were lost to follow up. Out of 92 cases that completed the study, 14 cases developed pre-eclampsia and 78 remained normotensive. Total cholesterol, triglycerides and LDL values for those women who developed preeclampsia were significantly higher than those who remained normotensive with p value of <0.05 which is statistically significant. Serum β-HCG in preeclampsia group is significantly elevated with p value < 0.05. Conclusion: The present study indicates an increased risk of pre eclampsia in patients with elevated serum β hCG and altered lipid profile in their second trimester. Currently, no screening tests are predictably reliable, valid, and economical; however the above two mentioned tests appear to be good non-invasive early predictors of preeclampsia.
Keywords
Pregnancy, Antenatal, Blood pressure
Introduction
Hypertensive disorders remain among the most significant and intriguing unsolved problems in obstetrics. Hypertensive disorders complicate 5-10% of all pregnancies. 16% of maternal deaths are attributed to hypertensive disorders. Worldwide about 76,000 pregnant women die due to preeclampsia and related hypertensive disorders. It is responsible for 25% of all fetal growth restriction and 15% of preterm birth in developed countries [1].
The incidence of preeclampsia in India is 8-10% and maternal mortality due to preeclampsia is 8% [2]. Preeclampsia is described as a pregnancy specific syndrome that can affect virtually every organ system; appearance of proteinuria remains important diagnostic criteria.
Early diagnosis, close antenatal surveillance, and timely intervention are key to the management of Preeclampsia. During the last two decades, a variety of biological, biochemical, and biophysical markers implicated in the pathophysiology of preeclampsia have been proposed to predict its development. Currently, there are no reliable, economic, and reproducible screening tests that are available, and moreover, the pathophysiologic mechanism of preeclampsia is still not clearly known. The most current hypothesis regarding the pathophysiologic mechanism of preeclampsia points to early placental abnormalities. In pathogenesis of preeclampsia, endothelial cell activation or dysfunction is believed to be the central theme. Elevated β-hCG levels carry an increased risk of preeclampsia. Altered lipid synthesis is also suggested to be an important pathway of pathogenesis in preeclampsia [3,4].
In view of these findings, this study was undertaken, in which both β-hCG and lipid profiles are studied in the early second trimester as early predictors of Preeclampsia. Early identification of women at risk of Preeclampsia is done which may help in taking timely preventive management to prevent or delay these complications.
Materials and Methods
This prospective study was conducted in the department of obstetrics and gynaecology, SDM college of Medical sciences and hospital, after obtaining institutional ethical committee clearance and informed consent on 100 pregnant normotensive patients who were selected randomly between the gestational ages 14-20 weeks attending the ANC clinic irrespective of parity. Women with multiple pregnancy, chronic hypertension, diabetes mellitus and congenital malformations were excluded from the study.
All women were subjected to a detailed history regarding age, parity, past obstetric history, medical history and family history. Height, weight and blood pressure were measured. Routine antenatal investigation was done. Five ml of venous blood sample was collected and tests were carried out. Estimation of serum β-hCG level was done by chemiluminescent immunometric assay method. Serum lipid profile estimation was done by enzymatic calorimetric test. The cases were followed up in antenatal clinic and were examined 4 weekly till 28 weeks, every 15 days once up to 34 weeks and there after weekly till delivery. At every visit blood pressure was recorded. Urine was examined for albumin, if blood pressure was found to be raised. Pregnancy induced hypertension (PIH) was considered if the blood pressure was ≥ 140/90 mm hg on two occasions at least 6 hours apart after 20 weeks of gestation. Preeclampsia was considered if gestational hypertension was associated with proteinuria of atleast 1+ on dipstick.
Statistical analysis
Results so obtained were evaluated and analyzed statistically. Mean ± standard deviation of all the parameters of interest were calculated for hypertensive and normotensive group and difference of means between the two groups was tested by unpaired ‘t’ test. Chi-square test was applied for categorical data. Diagnostic validity tests like sensitivity, specificity, positive predictive value, negative predictive value and overall accuracy were performed to assess diagnostic values of serum β-hCG and lipid profile in the prediction of preeclampsia. A p–value of <0.05 or less was considered statistically significant.
Results
Out of 100 women who enrolled in the study 92 women were completely followed till term. Eight women were lost to follow up. Out of 92 cases that completed the study 14 cases developed preeclampsia and 78 remained normotensive. Mean age among PIH was 22.93 and mean age among normotensive group was 21.17. Mean BMI in PIH group was 23.94 and that in normal group were 22.70. There was no statistical significance among normal and PIH group with respect to mean age (in yrs.) (p=0.1695) and BMI (Kg/m2) (p=0.0639).
Comparison of systolic and diastolic blood pressure at the time of booking (14-20weeks) between the PIH and the normotensive group did not vary significantly (p=0.6919 for systolic and p=0.5802 for diastolic) whereas both systolic and diastolic blood pressure for PIH cases at the time of delivery were significantly higher when compared to normotensive group (p=0.0001).
Comparison of Normal and PIH group with mean Total Cholesterol, Triglycerides, HDL, LDL, VLDL scores and serum β-hCG by independent t test is shown in Table 1. Out of 41 cases with total cholesterol > 200mg/dl, 12 cases developed PIH. Out of 31 cases with triglycerides more than 156mg/dl, 10 developed PIH. Four cases developed PIH in spite of triglycerides being within normal limits. Out of 25 patients who developed PIH, 10 patients had their LDL cholesterol more than 117mg/dl and 4 cases in spite of LDL being less than 117 mg/dl developed PIH. Out of 45 patients with β-hCG more than 35000 IU/mL, 13 developed PIH. All the above said parameters were statistically significant (p= 0.0001).
Table 1: Comparison with mean Total Cholesterol, Triglycerides, HDL, LDL, VLDL scores and serum β-hCG.
| Variable | Groups | Mean | SD | SE | t-value | P-value |
|---|---|---|---|---|---|---|
| Total Cholesterol | Normal group | 184.13 | 49.11 | 5.67 | -4.8591 | 0.0001 |
| PIH group | 255.57 | 57.77 | 15.44 | |||
| Triglycerides | Normal group | 146.76 | 50.09 | 5.78 | -3.0411 | 0.0031 |
| PIH group | 191.71 | 54.51 | 14.57 | |||
| HDL | Normal group | 47.41 | 13.6 | 1.57 | 0.2757 | 0.7834 |
| PIH group | 46.36 | 10.28 | 2.75 | |||
| LDL | Normal group | 101.07 | 24.07 | 2.78 | -4.6736 | 0.0001 |
| PIH group | 137.36 | 38.24 | 10.22 | |||
| VLDL | Normal group | 23.72 | 9.33 | 1.08 | -1.733 | 0.0866 |
| PIH group | 28.5 | 10.23 | 2.74 | |||
| β-hCG | Normal group | 36834.93 | 23120.45 | 2669.72 | -4.4656 | 0.0001 |
| PIH group | 68396.37 | 30016.75 | 8022.31 |
Logistic regression of prediction of PIH by other parameters shows significant association with total cholesterol, triglycerides, and serum beta hCG (Table 2). Diagnostic values of β-hCG and lipid profiles in the prediction of PIH are shown in Table 3 and ROC curve in Figure 1.
Table 2: Table 2: Logistic regression analysis of parameters for prediction of PIH.
| Variables | Odds Ratio | Std. Err. | Z-value | P-value | 95% CI for OR | |
|---|---|---|---|---|---|---|
| Lower | Upper | |||||
| Total cholesterol | 52.86 | 75.88 | 2.76 | 0.0060* | 3.17 | 881.37 |
| TG | 10.44 | 11.52 | 2.13 | 0.0330* | 1.2 | 90.75 |
| HDL | 0.36 | 0.41 | -0.9 | 0.367 | 0.04 | 3.3 |
| LDL | 7.85 | 8.55 | 1.89 | 0.059 | 0.93 | 66.44 |
| VLDL | 19.53 | 31.1 | 1.87 | 0.062 | 0.86 | 442.66 |
| Beta hcg | 26.36 | 37.75 | 2.28 | 0.0220* | 1.59 | 436.45 |
Table 3: Diagnostic validity test of β-hCG and lipid profiles in the prediction of PIH.
| Variables | Total Cholesterol | Triglycerides | HDL | LDL | VLDL | β-hCG |
|---|---|---|---|---|---|---|
| Sensitivity | 26.67 | 42.22 | 28.89 | 35.56 | 6.67 | 92.86 |
| Specificity | 104.55 | 72.73 | 70.45 | 79.55 | 97.73 | 57.33 |
| Positive predictive value | 29.27 | 61.29 | 50 | 64 | 75 | 28.89 |
| Negative predictive value | 95.83 | 55.17 | 49.21 | 54.69 | 50.59 | 97.73 |
| Overall accuracy | 50.6 | 50.6 | 50.6 | 50.6 | 50.6 | 50.6 |
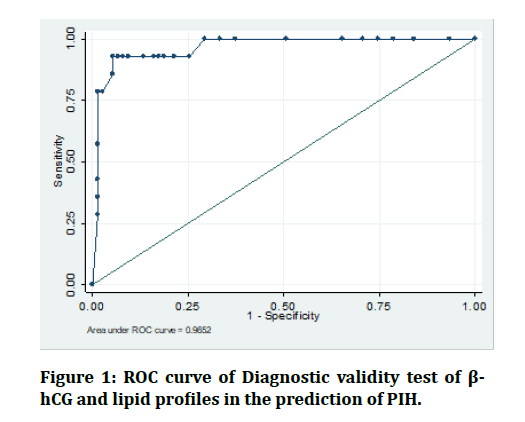
Figure 1: ROC curve of Diagnostic validity test of β- hCG and lipid profiles in the prediction of PIH.
Discussion
Out of 92 cases that completed the study 14 cases developed preeclampsia and 78 remained normotensive. In a study conducted by Kiran et al. [5], 120 patients attending the outpatient department of the Obstetrics and Gynaecology of the Maharaja Agrasen Hospital were selected, out of which 21 cases developed preeclampsia and there was a statistically significant rise of cholesterol levels in pre eclampsia group. In a study conducted by Pradeepa et al [6] in 2016 at Thanjavur, women with high values of β-hCG and lipid profile in the gestational age group 14-20 weeks developed preeclampsia. In a study conducted by Vidyabati et al [1], out of 164 women attending OPD of the Department of OBG at Regional Institute of medical sciences, 29 developed PIH and there was a statistically significant elevations in β-hCG and lipid profile.
In our study majority of women belonged to age group between 20-24 years. Mean age among hypertensive group was 22.93 years and that in normotensive group was 21.17 years. In a study conducted by Kiran Yadav et al [7], 51.7% of cases were in the age group of 25-29 years and maximum number of preeclampsia was found within this group. In a study conducted by Pradeepa et al [6] maximum cases of preeclampsia were distributed in the age group 24.48 ± 2.08 years and in normotensive group it was 23.65 ± 2.47 years. In Vidyabathi et al study [1] means age was 27.17 years. Maximum number of preeclampsia was observed in the age group 31-35 years.
In our study mean systolic blood pressure in normotensive group was 112.99 mm Hg and diastolic was 72.40 mmHg and in the hypertensive group systolic blood pressure was 113.86 and diastolic was 70.71 mmHg. In study conducted by Kiran Yadav et al [7], systolic blood pressure in normotensive group was 112.20 ± 4.60mmHg and diastolic blood pressure was 72.24 ± 5.75mmHg.In preeclampsia group booking blood pressures were 111.43 ± 3.59mmhg and 72.67 ± 4.95mmHg. In a study conducted by Pradeepa et al [6], there was no difference in the blood pressure at booking. Blood pressure at the time of booking between preeclampsia and normotensive group did not vary significantly in all the studies.
In present study elevated β-hCG values was associated with preeclampsia. Out of 45 patients, 13 developed preeclampsia that had their β-hCG values above 35,000IU/ml and was statistically significant. In the study conducted by Vidyabathi et al [1], 29 cases developed preeclampsia out of 164 women. Out of 29 cases, 21 women had elevated β-hCG above 45,000IU/ml. For every 1000mIU/ml increase in serum β-hCG a pregnant women has 10.7% increasing chance of having preeclampsia. However in a study conducted by Kiran Yadav et al [7], there was no correlation between β-hCG and the development of preeclampsia. In a study conducted by Pradeepa et al [6], out of 100 women, 32 women who had high β hCG value of more than 25,000 IU/ml developed preeclampsia with a significant p value of less than 0.01.
In the present study, women with elevated triglycerides, total cholesterol and LDL developed preeclampsia subsequently. In study conducted by Kiran Yadav et al [7] in women who subsequently developed preeclampsia had elevated values of triglycerides, LDL,VLDL, and total cholesterol.
In study conducted by Pradeepa et al [6], elevated triglycerides, LDL, VLDL, total cholesterol and decrease in HDL was associated with preeclampsia. Triglycerides had 96% specificity and 97% PPV. Vidyabati et al [1] showed an association between maternal early pregnancy dyslipidemia especially raised LDL and hypercholesterolemia which was associated with the development of preeclampsia.
Conclusion
Maternal lipid profile and serum β-hCG in the early second trimester is a very good and a effective noninvasive test, which is economical and reliable technique which can be used in the prediction of preeclampsia before the clinical onset of the disease. If prediction is possible, prevention will follow naturally. The present study indicates an increased risk of preeclampsia in patients with elevated β-hCG and dyslipidemia and serves as a promising tool for predicting preeclampsia.
Conflict of Interest
No conflict of interest among the authors.
References
- Vidyabati RK, Hijam Davina, Singh NK, et al. Serum beta HCG and lipid profile in second trimester as predictors of pregnancy induced hypertension. J Obstet Gynecol India 2010; 60:44-50.
- Arun J. Epidemiology of preeclampsia: Impact of obesity. Nutr Rev 2013; 71:S18–S25.
- Vanden Elzen HJ ,Wladimroff JW, Cohen-Overbeek TE, et al.Serum lipids in early pregnancy and risk of early preeclampsia. Br J Obstet Gynaecol 1996; 103:117-22.
- Sattar N, Greer A .Pregnancy complications and maternal cardiovascular risk oppurtunities for intervention and screening. BMJ 2002; 325:157-60.
- Sumitra Y, Namrata S, Sangeeta P, et al. The association of β hcg and lipid profile in predicting pre-eclampsia. J Dent Med Sci 2014; 7:28-31.
- Pradeeba S, Poovathi M, Munira V, et al. Serum beta hcg and lipid profile in early second trimester is a predictor of pregnancy induced hypertension. Int J Reproduction Contraception Obstetr Gynecol 2016; 5:3011-6.
- Yadav K, Aggarwal S, Verma K. Serum bhCG and lipid profile in early second trimesters predictors of pregnancy-induced hypertension. J Obstetr Gynecol India 2014; 64:169–174.
Author Info
Meghana Puttaswamy1, Usha Brindhini Mathialagan2*, Ramesh kumar3 and Rathnamala M Desai3
1Department of Obstetrics and Gynaecology, BGS Global institute of medical sciences, Bangalore, India2Department of Obstetrics and Gynaecology, SVIMS-Sri Padmavathi Medical college for women, Tirupati, India
3Department of Obstetrics and Gynaecology, SDM college of Medical Sciences and hospital, Dharwad, India
Citation: Meghana Puttaswamy, Usha Brindhini Mathialagan, Ramesh kumar3, Rathnamala M Desai, Study of Serum ?-HCG and Lipid Profile in Second Trimester as Predictors of Pre-Eclampsia in a Tertiary Care Teaching Hospital, J Res Med Dent Sci, 2021, 9(7): 432-435
Received: 06-Jul-2021 Accepted: 27-Jul-2021
