Research - (2022) Volume 10, Issue 1
The Association of Distal Caries in Mandibular Second Molars with the Position of Mandibular Third Molars: A Cone Beam Computed Tomography Study
Danya Hashem1* and Ebtihal Zainalabdeen2
*Correspondence: Danya Hashem, Department of Restorative Dental Science, College of Dentistry, Taibah University, Madinah, Saudi Arabia, Email:
Abstract
Introduction: There is a high prevalence of impacted mandibular third molars (M3Ms) worldwide and surgical removal of M3Ms is a common procedure in oral and maxillofacial surgery. Few studies have explored the effect of eruption status of M3Ms on the presence of distal caries lesions of mandibular second molar (M2M) by using cone beam computed tomography (CBCT). Aim: Analyze the prevalence of caries and the degree of its severity on the distal surface of M2Ms in a Saudi population and correlate this with the eruption and position of the M3Ms in three dimensions using CBCT. Materials and Methods: CBCT scans of 160 patients were included and the patient age and gender, impaction depth and angulation of the M3M, contact point localization and horizontal position of the M3M, the presence of distal caries and its severity on the M2M were assessed. Association between distal caries and demographic/radiographic variables were analyzed using Pearson’s chi-square and Fisher exact test and multivariate regression was used to identify risk factors. Results: The prevalence of distal caries in M2Ms adjacent to the M3Ms was 15%. Contact point localization was the only variable associated with the presence of distal caries in M2Ms where impacted M3Ms with a contact point at or above the CEJ of the M2M are associated with distal caries. Conclusions: Clinical risk should influence the decision for prophylactic removal of the M3M. Careful evaluation of the distal caries on the M2M and cautious consideration of the extraction of the M3Ms should be undertaken.
Keywords
Cone beam computed tomography, Distal caries, Mandibular third molar, Mandibular second molar
Introduction
Dental caries is one of the most prevalent chronic infectious diseases that affect people worldwide [1,2]. Dental caries is a multifactorial disease that depends on many factors such as the tooth, time, diet, and bacteria in the biofilm which contribute to caries development [3]. The position of the tooth and its inclination is one important factor. A partially erupted tooth does not participate in mastication and is in a lesser self-cleansing area offering a condition more favorable for food and bacterial accumulation that cannot be cleaned through normal brushing and flossing compared to a fully erupted tooth causing caries development [4,5]. The prevalence of caries on the distal surface of mandibular second molars associated with a semi-erupted mandibular third molar can range from 7 to 32% [6]. Previous studies have been conducted to evaluate the association of caries on distal surface of mandibular second molars with mandibular third molars using various modalities like clinical examination [7], periapical [8], bitewings [9], and panoramic radiographs [10]. To date, very few studies have explored the effect of eruption status of mandibular third molars on the presence of distal carious lesions of mandibular second molars by using cone beam computed tomography (CBCT). Compared with two-dimensional radiographs, CBCT images offer distinct advantages of three-dimension visualization free from overlaps and have been shown to improve the detection of proximal carious lesions for mandibular second molars [11]. It has been found that the buccolingual position of mandibular third molars cannot be visualized using panoramic and periapical techniques [11,12]. CBCT can supply the detailed information of the proximity relationship between mandibular second and third molars in three dimensions, making analysis of risk factors of distal caries of mandibular second molars more accurate [13]. This retrospective study aims to analyze the prevalence of caries and the degree of its severity on the the distal surface of mandibular second molars in a Saudi population and correlate this with the eruption and position of the mandibular third molars in three dimensions using cone beam computed tomography images taken at Taibah University Dental College (TUDC) in Madinah. Clinical significance of the study is to evaluate high-risk patients and formulate a protocol for early diagnosis of this pathology along with proposal of prophylactic removal of mandibular third molar in the former condition. The null hypothesis is that there is no correlation between the prevalence and severity of distal caries on the mandibular second molar and the degree of eruption and position of the mandibular third molar in three dimensions using cone beam computed tomography.
Materials and Methods
Study design, ethical considerations, and sample selection
This is a retrospective cross sectional radiographic study reviewed and approved by the Taibah University College of Dentistry Research Ethics Committee (TUCDREC/ 13102020/DHashem) in Madinah, Saudi Arabia. The radiographs used in this study were anonymous, and the confidentiality of the patients maintained. A total of 561 CBCT scans were taken of patients referred between April 2019 and April 2021 with different fields of view from several different departments, including oral surgery, endodontics, prosthetics, and orthodontics at Taibah Dental Hospital. However only large and medium field of view CBCT scans showing the entire maxillary and mandibular dentition were included in this study. Furthermore, CBCT images were excluded from this study if they 1) had artifacts owing to the presence of high-density materials or other reasons that obscured the areas of interest, 2) patients younger than 21 years old with impacted M3Ms favorable to erupt with less than two thirds of the roots [14], and 3) impacted M3M with missing adjacent M2M. Therefore, only 257 out of a total of 561 CBCT scans were eligible for inclusion in the study.
Radiographic assessment
CBCT scans were reclaimed from the records of the Carestream R4 Clinical and Practice Management Software database (CareStream Health, Rochester, NY, USA) of Taibah University Dental college and were acquired with a CS 9300 PREMIUM 3D CBCT device (CareStream, Rochester, NY, USA) set at 73 kV and 12 mA. Two observers with >7 years of experience measured and evaluated the impacted lower molars variables and the presence of distal caries in the second mandibular molars independently. The CBCT volumes were manipulated by InVivoDental software version 6.0.1 from Anatomage, Inc. A random sample of 30 CBCT images were evaluated to assess inter-observer agreement and repeated after 2 weeks to assess intra-observer reliability.
The impaction depths of the M3Ms were categorized according to the classification of Pell and Gregory [15]. A line was extended from the highest point of the impacted M3M to the adjacent M2M.
If the line was above the occlusal plane of the M2M then this was considered “level A”. If the line contacted the adjacent M2M in the middle of the crown then this was considered “level B”.
If the line contacted the M2M in the cervical area, then this was considered “level C”.
The angulation of the M3M was calculated by measuring the angle of the intersection made by the occlusal plane of the M2M and the occlusal plane of the M3M [16]. The occlusal plane was drawn along the tips of the cusps of the M2M and the M3M.
The resulting angle between to the two line was considered as <−15° (distally angulated), -15° to +15° (vertically angulated), 16°–75°(mesially angulated), >75° (horizontally angulated). If no angle was formed between the two, then this was considered as “others” (Figure 1).
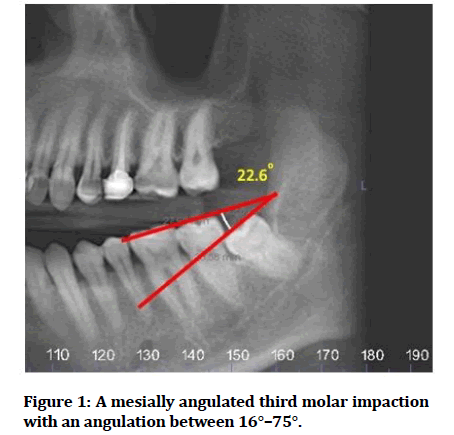
Figure 1: A mesially angulated third molar impaction with an angulation between 16°–75°.
The contact point localization between M3Ms and M2Ms was classified according to where the two teeth contact in relation to the CEJ into: above, at, or below the CEJ.
The horizontal position of the impacted M3M was determined using axial and cross-sectional slices to visualize the buccolingual position of the M3M in the alveolar crest. The tooth was considered located in the buccal, central, or lingual depending on how near it is to either side (buccal or lingual) [17].
If the distance from both sides of the M3M are equal then this was considered to be located in the central of the alveolar bone (Figure 2).
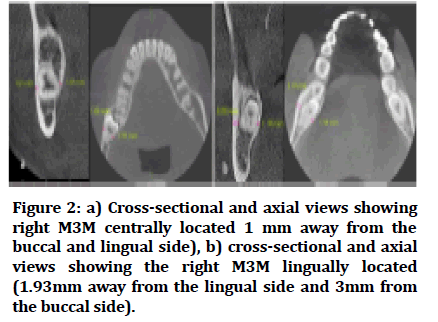
Figure 2: a) Cross-sectional and axial views showing right M3M centrally located 1 mm away from the buccal and lingual side), b) cross-sectional and axial views showing the right M3M lingually located (1.93mm away from the lingual side and 3mm from the buccal side).
Caries analysis carried out in this study has been adopted according to the study by Chen et al. which adapted and modified the radiographic classification in the International Caries Detection and Assessment System (ICDAS) and the International Caries Classification and Management System (ICCMS™). Therefore, according to the radiographic appearance, the severity of carious lesions was classified as (1) slight caries, involving less than half the dentin thickness; (2) moderate caries, involving at least half the dentin thickness and with the pulp cavity remaining unbroken; and (3) severe caries, involving the pulp cavity [13].
Statistical analysis
Data were processed using SPSS 25.0 for Windows (SPSS Inc., Chicago, IL, USA). The inter-observer and intraobserver agreement on the measurement of the radiographic characteristics was analyzed using Cohen’s κ test (poor agreement, less than 0.40; moderate agreement, 0.40 to 0.59; good agreement, 0.60 to 0.74; excellent agreement, 0.75 to 1.00). The association between distal caries in the M2M and demographic/ radiographic variables was analyzed using Pearson’s chisquare and fisher exact test.
Multivariate logistic regression model was built to further evaluate predictive values of the factors for the prevalence of distal caries in M2Ms.
The severity of distal caries among different groups classified according to the radiographic characteristics was compared by the Kruskal-Wallis test or Mann-Whitney U test. The level of significance was set at a p value <0.05.
Results
From the 257 impacted lower molars, only one M3M from each patient was included in this study to avoid the potential for selection bias. Thus, when both right and left M3Ms of the same patient met the inclusion criteria, only one M3M was randomly included.
Accordingly, a total of 160 impacted molars from 160 CBCT scans were included in the study. There were 98 (61%) males and 62 (39%) females, with a mean age of 33 years (21-70 years).
The level of agreement between the two observers was excellent (κ=0.771–1; p<0.001). The intra-observer reliability of both observers ranged from good to excellent (κ of observer A=0.722–1; κ of observer B=0.766–1; p < 0.001) (Table 1).
| Intra-observer reliability “A” (P<0.001) | Intra-observer reliability “B” (P<0.001) | Inter-observer Agreement (P<0.001) | |
|---|---|---|---|
| M3M angulation | 0.76 | 0.89 | 1 |
| Impacted M3M depth | 0.9 | 0.87 | 0.77 |
| Contact point with CEJ | 0.75 | 0.83 | 0.8 |
| Horizontal location of M3M | 0.79 | 0.76 | 0.8 |
| Caries of M3M | 1 | 1 | 1 |
| Caries of M2M | 0.72 | 0.97 | 0.97 |
| Depth of distal caries M2M | 0.79 | 1 | 1 |
Table 1: Intra-observer reliability and inter-observer agreement for each variable.
The overall prevalence of distal caries in M2Ms adjacent to the M3Ms was 15% (15/160). Most M3Ms were mesially inclined 57.5% (92/160) and class A impacted 51.9% (83/160) in the sagittal plane, and lingually positioned 58% (93/160) in the horizontal plane. The presence of distal caries in M2Ms and its association with various demographic and radiographic characteristics are shown in Table 2. Pearson’s chi-square independence tests indicated that age, gender, depth of impaction, mesial angulation and horizontal position of M3M, are not associated with presence of distal caries. However, only contact point localization were associated with the presence of distal caries in M2Ms (p<0.05; Table 2). Distal caries in M2Ms were more observed in the cases in which the contact points were above the distal CEJ of M2Ms or at CEJ, 25.6% (10/39) and 18.8% (9/48) respectively, compared to those cases in which the contact point was below the distal CEJ of M2Ms 8.3%(5/60) (Table 2).
| Variable | Total (N=160) | Presence of distal caries of M2M | P value | |
|---|---|---|---|---|
| Yes (%) | No (%) | |||
| Age (years) | ||||
| 21-27 | 48 | 5(10.4) | 43(89.6) | 0.1 |
| 28-37 | 80 | 17(21.3) | 63(78.8) | |
| >37 | 32 | 2(6.3) | 30(93.8) | |
| Gender | ||||
| Male | 98 | 15(15.3) | 83(84.7) | 1 |
| Female | 60 | 9(14.5) | 53(85.5) | |
| M3M angulation | ||||
| Vertical | 25 | 5(20) | 20(80) | 0.624 |
| Mesioangular | 92 | 15(16.3) | 77(83.7) | |
| Horizontal | 36 | 3(8.3) | 33(91.7) | |
| Distoangular | 5 | 1(20) | 4(80) | |
| Others | 2 | 0 | 2(100) | |
| Impaction depth according to Pell and Gregory | ||||
| Level A | 83 | 17(20.5) | 66(79.5) | 0.143 |
| Level B | 56 | 6(10.7) | 50(89.3) | |
| Level C | 21 | 1(4.8) | 20(95.2) | |
| Contact point localization | ||||
| No contact | 13 | 0 | 13(100) | 0.04* |
| Above CEJ | 39 | 10(25.6) | 29(74.4) | |
| At CEJ | 48 | 9(18.8) | 39(81.3) | |
| Below CEJ | 60 | 5(8.3) | 55(91.7) | |
| Horizontal position | ||||
| Buccal | 1 | 0 | 1(100) | 0.327 |
| central | 66 | 7(10.6) | 59(89.4) | |
| Lingual | 93 | 17(18.3) | 76(81.7) | |
| *Statistically significant (p < 0.05 by Pearson’s chi-square independence test (fisher exact test) between categorical variables) | ||||
Table 2: The prevalence of distal caries in mandibular second molars and its associations with the demographic/radiographic characteristics.
Multivariate logistical regression analysis revealed that contact point at or above the CEJ of M2M was identified as a risk factor for distal caries in M2Ms (contact point above the CEJ; OR:3.95, contact point below the CEJ; OR : 2.23),(Table 3) however, the odd ratio was statistically significant with contact point “above CEJ” p value <0.05 and non-significant with “at CEJ”. Lingual horizontal position of M3Ms had (OR: 1.33) more likely to cause distal caries in M2Ms when compared with M3M in the central position (p>0.05). Mesioangular and distoangular M3M impaction showed increased risk of M2M distal caries (OR: 1.11 and 1.1 respectively) although not statistically significant. Horizontal position showed reduced risk or protective effect to caries OR:0.451, all p value >0.05 (Table 3).
| Variable | OR | 95% CI of OR | p value | |
|---|---|---|---|---|
| Upper | Lower | |||
| Contact point localization | ||||
| Below | 1 | |||
| Above | 3.948 | 1.097 | 14.21 | 0.036 |
| At | 2.225 | 0.678 | 7.3 | 0.187 |
| Horizontal position of M3M | ||||
| Median | 1 | |||
| Lingual | 1.331 | 0.484 | 3.661 | 0.58 |
| M3M angulation | ||||
| Vertical | 1 | |||
| Mesioangular | 1.105 | 0.318 | 3.835 | 0.875 |
| Horizontal | 0.451 | 0.09 | 2.259 | 0.333 |
| Distoangular | 1.077 | 0.083 | 13.981 | 0.955 |
Table 3:Logistical regression analysis for identified risk factors for distal caries in M2Ms.
Comparison of the severity of carious lesions on M2M among groups classified according to the radiographic characteristics showed no significant difference in studied groups, P value >0.05 (Table 4).
| Variable | n | Frequency at each severity score | Mean rank | P value | ||
|---|---|---|---|---|---|---|
| Class I | Class II | Class III | ||||
| Age (years) | ||||||
| 21-27 | 5 | 1 | 2 | 2 | 11.3 | 0.89 |
| 28-37 | 16 | 1 | 9 | 6 | 12 | |
| >37 | 2 | 0 | 1 | 1 | 13.75 | |
| M3M angulation | ||||||
| Vertical | 5 | 2 | 1 | 2 | 9.9 | 0.726 |
| Mesioangular | 14 | 0 | 8 | 6 | 13 | |
| Horizontal | 3 | 0 | 2 | 1 | 12 | |
| Distoangular | 1 | 0 | 1 | 0 | 8.5 | |
| *Other | ||||||
| Contact point localization | ||||||
| Above CEJ | 10 | 1 | 5 | 4 | 12 | 0.07 |
| At CEJ | 8 | 1 | 6 | 1 | 8.94 | |
| Below CEJ | 5 | 0 | 1 | 4 | 16.9 | |
| Horizontal position | ||||||
| Median | 6 | 0 | 2 | 4 | 15.5 | 0.1 |
| Lingual | 17 | 2 | 10 | 5 | 10.76 | |
| *Buccal | ||||||
| *Other group and buccal group were omitted due to insufficient data | ||||||
Table 4: Comparison of the severity of carious lesions on M2M among groups classified according to the radiographic characteristics by the Kruskal-Wallis test or Mann-Whitney U test.
Discussion
This study was conducted on a Saudi population in Madinah using CBCT radiography to assess the prevalence of distal caries and the degree of its severity on the the distal surface of the M2M and correlate this with the eruption and position of the mandibular third molars. In this study, the prevalence of distal caries in M2Ms adjacent to the M3Ms was 15% which was lower compared to other studies using CBCT. This may be due to the fact that the CBCT radiographs had been taken for different diagnostic purposes by several departments such as oral surgery, prosthodontics, endodontics, and orthodontics. Therefore, the third and second molars involved may be asymptomatic with fewer chances for distal caries involvement. In a CBCT study by Jajashree et al., a total of 45% of M2Ms had distal caries associated with impacted M3Ms [18]. However, the sample size involved was 35 patients which is too small for the results to be reliable. Another study conducted in a Chinese population using 500 CBCT images found the prevalence of distal caries in the M2M to be 52% [19]. The authors reported this high percentage to be caused by patients not seeking dental services until their teeth exhibit symptoms and therefore the majority of third molars were symptomatic displaying swelling of the gingiva and sensitivity or pain related to the third or second molars. This may cause M2Ms with distal caries to be more likely included in the study [19]. Another CBCT study conducted by Chen et al. on 421 Chinese patients found the prevalence of distal caries in M2Ms associated with M3Ms to be 31%. The authors claim that this lower percentage is more representative of the Chinese population compared to the previous study as the CBCT images were randomly selected from an archive referred from all departments in the hospital [13].
The most common type of impaction in this study was recorded to be mesio-angular which is supported by other studies on the Saudi population [20-23] and other studies elsewhere [18,24,25]. Contact point localization was found to be associated with the presence of distal caries in M2Ms more than other variables. Contact point above the distal CEJ of M2Ms or at CEJ was associated with distal caries. This is in agreement with the study by Jajashree et al. where they reported that contact point at the CEJ was associated with a higher risk of distal caries [18]. Another study found that distal caries was more likely to be present when the contact point was at or below the CEJ identified using panoramic radiographs [26] which is in agreement with another study using CBCT radiographs [13]. This condition seems to favor food impaction and plaque accumulation facilitating caries development in the area.
Age, gender, depth of impaction, mesial angulation and horizontal position of M3M were associated to some degree with distal caries on the M2M although not statistically significant. Although previous studies indicated that the prevalence and severity of distal caries in M2Ms increases with age where older patients have a higher incidence of distal caries, this study found no association between age and distal caries probably due to the low mean age of the sample which is in agreement with the study by Chen et al. and Marques et al. [13, 26]. Similarly, gender was not found to have an association with distal caries in line with previous studies [13, 19] although Falci et al. found male patients have a greater chance of developing distal caries on the M2M [8]. They suggest the reason for this may be that women cared more about their oral health and actively seek dental services more frequently than men. It is crucial to point out that neither this study, or previous studies correlated the effect of oral hygiene, income level, or education level on the prevalence of distal caries. In this study, Pell and Gregory classification level A depth of impaction was more associated with distal caries compared to levels B and C although not statistically significant. This is comparable with the study by Falci et al. where more carious M2M were associated with Level A depth of impaction although not statistically significant [8]. This is logical as Level C depth of impaction would indicate complete enclosure of the crown of the M3M because the crown’s position is below the cervical line of the second molar and hence a lesser degree of association with distal caries on the M2M.
Risk factors for the development of distal caries according to the angle of impaction were mesial or distal while horizontal impaction showed the lowest risk. Mesial or distal angular impaction may expose the distal surface of the M2M to the oral environment. Because the area is difficult to clean, food impaction and plaque accumulation occurs resulting in caries formation on the distal surface of the M2M [24]. If the carious lesion is too large to be restored, extraction of the M3M becomes necessary to enable restoration of the M2M. Therefore, early detection and evaluation of the caries risk of the M2Ms associated with M3Ms is essential for the prevention of distal caries in the M2Ms.
The severity of distal caries on the M2M and its correlation with the eruption and position of the M3Ms was evaluated in this study as the prognosis and treatment of the distal caries on the M2M is dependent on the extent of the lesion [13], however no significant association was found. No other study evaluated the effect of the three-dimensional position of M3Ms on the severity degree of distal caries in M2Ms except for the study by Chen et al. where they found that M3M mesial angulation of 15°–75° increased the severity of distal caries in the M2M [13].
This study was conducted on a Saudi population in the city of Madinah using CBCT radiographs. Including other regions in Saudi Arabia would have the potential benefit of comparison for regional differences. Another limitation of this study was that it did not include clinical verification of caries. Further studies evaluating oral hygiene and socioeconomic status should be conducted to analyze their effects on distal caries on the M2M.
Conclusion
The null hypothesis stating that there is no correlation between the prevalence and severity of distal caries on the M2M and the degree of eruption and position of the M3M using cone beam computed tomography is partially rejected. Based on the results of this study, impacted M3Ms with a contact point at or above the CEJ of the M2M are associated with distal caries. Clinical risk should influence the decision for prophylactic removal of the M3M. Careful evaluation of the distal caries on the M2M and cautious consideration of the extraction of the M3Ms should be undertaken.
Author Contributions
“Conceptualization:D.H. and E.Z./
Methodology: D.H. and E.Z.
Validation: D.H. and E.Z.
Data curation: D.H. and E.Z.
Writing—Original draft preparation: D.H. and E.Z.
Writing—Review and editing: D.H. and E.Z.
All authors have read and agreed to the published
version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
The study was conducted according to the guidelines of the Declaration of Helsinki, and approved by the Taibah University College of Dentistry Research Ethics Committee (TUCDREC/13102020/DHashem).
Conflicts of Interest
The authors declare no conflict of interest.
References
- Petersen PE. Global policy for improvement of oral health in the 21st century–implications to oral health research of World Health Assembly 2007, World Health Organization. Community Dent Oral Epidemiol 2009; 37:1-8.
- Hashem D, Mannocci F, Patel S, et al. Evaluation of the efficacy of calcium silicate vs. glass ionomer cement indirect pulp capping and restoration assessment criteria: A randomised controlled clinical trial—2-year results. Clin Oral Investig 2019; 23:1931-9.
- Selwitz RH, Ismail AI, Pitts NB. Dental caries. Lancet 2007; 369:51-9.
- Prajapati VK, Mitra R, Vinayak KM. Pattern of mandibular third molar impaction and its association to caries in mandibular second molar: A clinical variant. Dent Res J 2017; 14:137.
- Hashem D, Hammad OAA, Farran J, et al. Oral health practice of primary school children in the region of Madinah, Saudi Arabia: A cross-sectional study. J Int oral Health 2021; 13:449.
- Glória JCR, Martins CC, Armond ACV, et al. Third molar and their relationship with caries on the distal surface of second molar: A meta-analysis. J Oral Maxillofac Surg 2018; 17:129-41.
- Chang SW, Shin SY, Kum KY, Hong J. Correlation study between distal caries in the mandibular second molar and the eruption status of the mandibular third molar in the Korean population. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2009; 108:838-43.
- Falci SGM, De Castro CR, Santos RC, et al. Association between the presence of a partially erupted mandibular third molar and the existence of caries in the distal of the second molars. Int J Oral Maxillofac Surg 2012; 41:1270-4.
- Pepper T, Grimshaw P, Konarzewski T, et al. Retrospective analysis of the prevalence and incidence of caries in the distal surface of mandibular second molars in British military personnel. Br J Oral Maxillofac Surg 2017; 55:160-3.
- Srivastava N, Shetty A, Goswami RD, et al. Incidence of distal caries in mandibular second molars due to impacted third molars: Nonintervention strategy of asymptomatic third molars causes harm? A retrospective study. Int J Appl Basic Med 2017; 7:15.
- Tyndall DA, Rathore S. Cone-beam CT diagnostic applications: Caries, periodontal bone assessment, and endodontic applications. Dent Clin North Am 2008; 52:825-41.
- Hashem D, Brown JE, Patel S, et al. An in vitro comparison of the accuracy of measurements obtained from high-and low-resolution cone-beam computed tomography scans. J Endod 2013; 39:394-7.
- Chen Y, Zheng J, Li D, et al. Three-dimensional position of mandibular third molars and its association with distal caries in mandibular second molars: A cone beam computed tomographic study. Clin Oral Investig 2020; 1-9.
- Friedrich RE, Ulbricht C, von Maydell LAB. The influence of wisdom tooth impaction on root formation. Ann Anat 2003; 185:481-92.
- Pell GJ. Impacted mandibular third molars: classification and modified techniques for removal. Dent Digest 1933; 39:330-8.
- Shiller WR. Positional changes in mesio-angular impacted mandibular third molars during a year. J Am Dent Assoc 1979; 99:460-4.
- Ge J, Zheng JW, Yang C, et al. Variations in the buccal-lingual alveolar bone thickness of impacted mandibular third molar: Our classification and treatment perspectives. Sci rep. 2016; 6:1-9.
- Jajashree KA, Senthilnathan KP, Kumar MP. Association between impacted mandibular third molars and distal caries in second molars-A radiographic study. Res J Pharm Technol 2018; 11:2309-12.
- Kang F, Huang C, Sah MK, et al. Effect of eruption status of the mandibular third molar on distal caries in the adjacent second molar. J Oral Maxillofac Surg 2016; 74:684-92.
- Hassan AH. Pattern of third molar impaction in a Saudi population. Clin Cosmet Investig Dent 2010; 2:109.
- Syed KB, Zaheer KB, Ibrahim M, et al. Prevalence of impacted molar teeth among Saudi population in Asir region, Saudi Arabia–a retrospective study of 3 years. J Int Oral Health 2013; 5:43.
- Alfadil L, Almajed E. Prevalence of impacted third molars and the reason for extraction in Saudi Arabia. Saudi Dent J 2020; 32:262-8.
- Bayoumi AM, Baabdullah R, Bokhari A, et al. The prevalence rate of third molar impaction among Jeddah population. Int J Dent Oral Health 2016; 2:4.
- McArdle LW, McDonald F, Jones J. Distal cervical caries in the mandibular second molar: an indication for the prophylactic removal of third molar teeth? Update. Br J Oral Maxillofac Surg 2014; 52:185-9.
- Alhadi Y, Al-Shamahy HA, Aldilami A, et al. Prevalence and pattern of third molar impaction in sample of Yemeni adults. On J Dent Oral Health 2019; 1:1-4.
- Marques J, Montserrat-Bosch M, Figueiredo R, et al. Impacted lower third molars and distal caries in the mandibular second molar. Is prophylactic removal of lower third molars justified? J Clin Exp Dent 2017; 9:e794.
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Author Info
Danya Hashem1* and Ebtihal Zainalabdeen2
1Department of Restorative Dental Science, College of Dentistry, Taibah University, Madinah, Saudi Arabia2Department of Oral Radiology, College of Dentistry, Taibah University, Madinah, Saudi Arabia
Citation: Danya Hashem, Ebtihal Zainalabdeen, The Association of Distal Caries in Mandibular Second Molars with the Position of Mandibular Third Molars: A Cone Beam Computed Tomography Study, J Res Med Dent Sci, 2022, 10(1): 375-381
Received: 22-Dec-2021, Manuscript No. Jrmds-21-50316; , Pre QC No. Jrmds-21-50316 (PQ); Editor assigned: 24-Dec-2021, Pre QC No. Jrmds-21-50316 (PQ); Reviewed: 07-Jan-2022, QC No. Jrmds-21-50316; Revised: 12-Jan-2022, Manuscript No. Jrmds-21-50316 (R); Published: 19-Jan-2022
