Research - (2021) Volume 9, Issue 4
The effects of Menaquinone 7 on Bone Remodeling Using Biochemical and Histological Analysis (An in vivo Study)
Saba H Alzubaidi1*, Manar M Alnema2, Ghada A Taqa3 and Banan K Al Obaidy4
*Correspondence: Saba H Alzubaidi, Department of Pedodontics Orthodontics Preventive dentistry, College of Dentistry, University of Mosul, Iraq, Email:
Abstract
Objective: To observe the effect of Menaquinone 7 on bone remodeling using biochemical and histological analysis in rabbits as a model.
Materials and methods: Healthy adult male rabbits were selected to use in our study. The animals were split into 2 main groups of six animals for each group (control and vitamin K2 groups).
Results: demonstrated that the Menaquinone 7 administration significant increase in BALP at day 28 ( 1.0 ± 0.19) in comparison with control (0.5 ± 0.1) while no significant difference at 14 and 42 days . whereas NTX level showed no significant increase in at day 14 in control and Menaquinone 7(K2) (4.2 ± 0.1 ) (4.4 ± 1.0) respectively but at day 30 showed significant increase in NTX in control group (10.3 ± 0.1) in comparison with Menaquinone 7(K2) group (0.65 ± 0.1) also at day 42 showed significant difference in NTX level in control group (4.1 ± 0.1) in comparison with Menaquinone 7(K2) group(0.67 ± 0.1). Also a significant increase in osteoid tissue at the three experimental periods than control group.
Conclusions: This study concluded that Menaquinone 7(K2) increase in bone alkaline concentration level and decrease in bone resorption marker NTX, in addition to increase in osteoid tissue compare to control group .
Keywords
Menaquinone7, Bone remodeling, NTX, BALP, Osteoid tissue
Introduction
The mini-screw is a small device that is fixed temporarily into bone tissue for improving an orthodontic anchorage [1]. Although the orthodontic mini-screw gives absolute and compliance free anchorage, but it is quite right about its stability that there is till now a few apprehension [2] because nearly 40% of the treated orthodontic cases may undergo a miniscrew complication and failure [1], as the host (bone quality) consider the main factor that affect stability of mini-screw [3]. The fat-soluble compound which is important for clotting of the blood exist in 2 typs those are: Phylloquinone (vitamin K1) and menaquinone (vitamin K2) [4] .
Menaquinone with 7 isoprene residues (MK-7) ,which can be found in natto and many natural products, consider as an important subtype and more bioactive than the other vitamin K vitamins regarding bone formation [5] and the prevention of cardiovascular disease [6].
So, the purpose of our study was to observe the effect of MK-7 on bone tissue using Bone-specific alkaline phosphatase BALP and N-terminal telopeptide NTX bone markers ELIZA kits in serum of treated rabbits in different periods.
Materials and Methods
Twelve healthy mature male white rabbits were used, distributed equally into two main groups (control and experimental group). Each group was further divided into three groups (two rabbits in each) according to the period of the vitamin K2 administration (2, 4 and 6 weeks). The weights and age of rabbits were 1.8-2.3 Kg, 8-12 months respectively.
Thirty-six mini-screws made of Ti-6Al-4V alloy (GSSEM/South Korea) with 1.4 mm diameter, and 6mm long were used. Each rabbit implanted with three mini-screws in the right femur.
The dose of the vitamin which was given to the animals in units of mg/kg can be measured according to the following equation : Animal dose (mg/kg) = human equivalent dose (mg/kg) X Conversion factor (Human km/Animal km)The required dose of MK-7 which is safe for the rabbit was (900 μg/day), which was between the normal range of 555-1110 μg/day and high enough to be an effective dose that was derived from the HED of MK-7 of the dose of 180-360 μg/ day [7].
Every rabbit administrated MK-7 at morning via loading way. Each animal at the end of 14, 28 and 42 days was sacrificed with an over dose of ketamine hydrochloride [8]. During animal sacrifices, blood samples were collected from the jugular vein. Plain tubes were used to collect a 5 ml of blood and kept at room temperature for thirty minutes, then centrifuged for a period of twenty minutes at speed rate of 3000 rpm to separate the serum from the blood. A micropipte was used to transfer the collected serum into eppendr off tube and kept in deep freeze at -20 C to be thawed for analysis using ELISA microplate reader. The response of bone to the intake of vitamin K2 was evaluated by using bone formation ; Rabbit Bone Alkaline Phosphatase, (BALP) and bone resoption ; Rabbits cross linked N-telopeptide of type I collagen (NTX) bone markers ELISA kits. The bone block was sectioned longitudinally; each implant was carefully removed from its position. Serial cuts of 6mm thick were made parallel to the implant site, and then stained with Carazzi haematoxylin and Eosin Lison, so it can be visualized under common optical microscope. After the slides were prepared, and using an optical microscope of 40X magnification, images were taken. The grading of the osteoid tissue [9] within the periimplant sulcus was evaluated (Table 1).
| Grade | Histological response observed |
|---|---|
| 0-Nile | Sign of bone formation could not be detected in the field of operation (X10) |
| 1-Mild | Osteoid tissue present in minimal amount , less than half of the field (X10) |
| 2-Moderate | Small amount of mature bone be distinguished in the field (X10) |
| 3-Sever | The formation of huge amount of mature bone ( more than 3/4 of the field regions) could be detected (X10) |
Table 1: Grading of osteoid tissue formation.
Statistical analysis
The data were expressed as mean and standard deviation. One way analysis of variance (ANOVA) were used to analyze the difference between three Follow-up period. Independent t-test was used to analyzed the difference between two groups. The level of significance was at p ≤ 0.05 .
The histological data were tested and compare by Kruskal-wallis one way analysis of variance on Ranks, then use Dunn's test to determine difference within each group.
Results
ANOVA and Duncan multiple Statistical analysis showed significant increase in Bone-specific alkaline phosphatase at p≤0.05 between control group and Menaquinone 7 (K2) group at different follow-up times (Table 1).
Independent t-test Statistical analysis test demonstrated a significant increase in BALP at day 28 after in Menaquinone7(K2) group ( 1.0 ± 0.19) in comparison with control (0.5 ± 0.1). At day 14 no significant difference between Menaquinone7(K2) group (0.74 ± 0.16 ) in comparison with control group (0.44 ± 0.15). Also at day 42 ANOVA and Duncan multiple Statistical analysis showed there no significantly increased in Bone-specific alkaline phosphatase in Menaquinone7(K2) group (0.6 ± 0.1) when compared with control group (0.43 ± 0.1)(Figure 1).
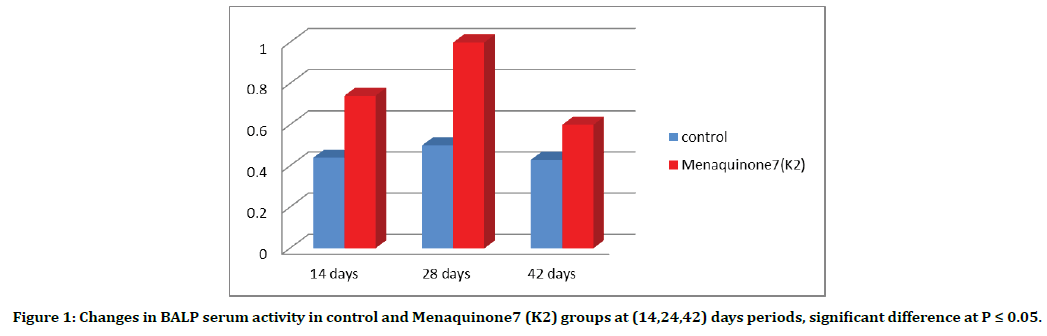
Figure 1. Changes in BALP serum activity in control and Menaquinone7 (K2) groups at (14,24,42) days periods, significant difference at P ≤ 0.05.
In control group, ANOVA and Duncan multiple tests showed no significant difference in all treated period at 14, 28, 42 days (0.44 ± 0.1) ( 0.5 ± 0.1) ( 0.43 ± 0.1) respectively, while in Menaquinone7(K2) group we found significantly increased in Bone-specific alkaline phosphatase at day 28 (1.0 ± 0.19) when compared to day 14 and 42 (0.74 ± 0.16) (0.6 ± 0.1) respectively (Figure 1).
ANOVA and Duncan multiple statistical analysis at P ≤ 0.05 showed significant increase in N-terminal telopeptide NTX bone marker in control groups compare with Menaquinone 7(K2) groups which is showed decrease NTX bone marker at different follow-up times (Table 2).
| BALP | NTX | |||
|---|---|---|---|---|
| Follow-up period | Control Mean ± SD | Menaquinone7) Mean ± SD | Control Mean ± SD | Menaquinone7Mean ± SD |
| Day 14 | 0.44 ± 0.15a | 0.74 ± 0.16a | 4.2 ± 0.1a | 4.4 ± 1.0a |
| Day 28 | 0.5 ± 0.1a A | 1.0 ± 0.19b B | 10.3 ± 0.1b A | 0.65 ± 0.1b B |
| Day 42 | 0.43 ± 0.1a | 0.6 ± 0.1a | 4.1 ± 0.1a A | 0.67 ± 0.1b B |
| Different capital letters mean there are significant different in the same raw at p≤0.05 | ||||
| Different small letters mean there are significant different in the same Colum at p≤0.05 | ||||
Table 2: Comparison of BALP, NTX activity in serum rabbits (ng/ml) at three times in two groups of the study.
Independent sample t-test showed no significant increase in NTX level at day 14 in control and Menaquinone 7(K2) (4.2 ± 0.1 ) (4.4 ± 1.0 ) respectively . At day 28 showed significant increase in NTX in control group (10.3 ± 0.1) in comparison with Menaquinone 7(K2) group (0.65 ± 0.1) . At day 42 showed significant difference in NTX between control (4.1 ± 0.1) in comparison with Menaquinone 7(K2) group (0.67 ± 0.1) as shown in (Figure 2).
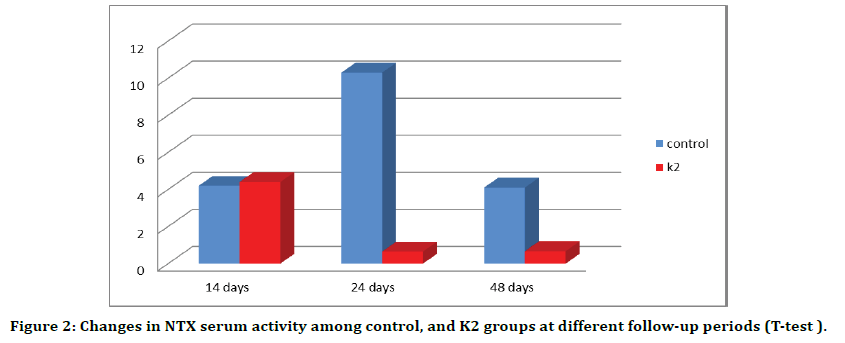
Figure 2. Changes in NTX serum activity among control, and K2 groups at different follow-up periods (T-test ).
In control group, statistical ANOVA and Duncan multiple test presented a significant increase in NTX at day 14 (10.3 ± 0.1) when compared with 28 and 42 (4.2 ± 0.1) (4.1 ± 0.1) groups respectively, while in Menaquinone7 (K2) group we found significantly decrease in NTX at 28 and 42 day (0.65 ± 0.1)( 0.67 ± 0.1) respectively in comparison to day 14 (4.4 ± 1.0) (Figure 2).
In Table 3, there is a significant increase in osteoid tissue formation among the vitamin K2 group when compare to control group at the three experimental periods. Also, a significant increase in osteoid tissue formation in control and vitamin K2 groups at the third experimental period (day 42) when compare to 14 and 28 days groups respectively.
| Groups | Chi-Square | Chi-Square | Chi-Square |
|---|---|---|---|
| Group I (Day14) | Group II (Day 28) | Group III (Day 42) | |
| Control | A† | A | B |
| 5.000 (0.025)* | 5.000 (0.025)* | 5.000 (0.025)* | |
| Vitamin K2 | A | A | B |
| *=Significant at p≤0.05 | |||
| † -Different capital letters mean there are significant different in the same raw at p ≤ 0.05 | |||
Table 3: Histological finding of osteoid tissue formation in control and vitamin K2 groups at the three experimental periods.
Discussion
White rabbite was used in this study, as its suitable model for the researches correlated to the healing of bone [10] and widly in use in implantology's researches [11]. Also, rabbit's femur bone used as a site of implantation because the quality of its tissue resemble the human bone tissues [12] . In this study, the period which the experiment took place in was that of three healing periods; 14, 28 and 42 days starting from the day of the screw insertion. Alsandook et al. [13] study three healing periods (2,4, and 6 weeks) of bone around the miniscrews in a rabbit model and they concluded that the appearance of osteoclasts at 4 weeks and at 6 weeks osteoblasts appear.
Vitamin K2 has an effect on osteoblasts's proliferation and differentiation [14]. It inhibits the induction of apoptosis in osteoblasts and inhibits Fass-mediated apoptosis in a dosedependent manner [15], and subsequently could increase the activity of alkaline phosphatase [14,16], and the level of bone anabolic markers such as osteocalcin in the cell medium [17,18]. As the alkaline phosphatase activity increase, it will lead to an increase in the formation of the organic matrix and mineral part of the bone, as will the deposition of osteocalcin and hydroxyapatite in the bone. In the conducted study, showed increase in BALP in all Menaquinone 7(K2) groups in comparison with control groups, with statistically significant increase in 28 day group. Osteoblasts produce bone alkaline phosphatase which is directly proportion with the formation of bone. Osteoblasts produce uncarboxylated osteocalcin, , which require MK-7 to convert it to carboxylated osteocalcin. So that, carboxylated osteocalcin can pick-up the calicum molecules from the blood and convert it to bone matrix [19,20]. Our result came in accordance with the result of Julia et al. [21], they concluded that Vitamin K2 has shown to prompt the formation of bone via stimulating osteoblast differentiation and carboxylation of osteocalcin, and increasing alkaline phosphatase, also, Akbari et al. [22], state that Vitamin K has an anabolic effect on the bone in many ways like promoting osteoblast differentiation.
Kameda et al. [23] had reported that vitamin K2 cause inhibition of bone resorption by osteoclastic in rabbit model. The N terminal telopeptide (NTX) used as bone resorption markers, which is released during collagen degradation [24]. In this study, showed significant increase in N-terminal telopeptide NTX bone marker which mean increased bone resorption rates in control groups in comparison with Menaquinone 7(K2) groups which showed decrease in bone resorption rates at different follow-up times. The result of this study come in agreement with the result of Kawata et al [25] , they displayed that the capability of vitamin K2 to induce apoptosis of osteoclast Also, Vamsee et al. [26], concluded that his vitamin organize bone turnover which involves removal of old or damaged bone by osteoclasts and a new bone formed by osteoblasts will replace the damaged one. Wu et al. [27] state that Vitamin K2 found to greatly restrain RANKL-medicated osteoclast cell formation of bone marrow macrophages. Furthermore, a significant increase in osteoid tissue formation in vitamin K2 group in comparison to control group in all experimental periods was shown in this study, which is a good indicator of osteoblast formation and subsequent bone formation as stated by Setiawati et al. [28] in that, osteoid tissue are produced by Osteoblasts, by means of differentiating osteoblasts from the ectomesenchyme condensation center and producing bone fibrous matrix (osteoid). Later, osteoid is mineralized .
Conclusion
Vitamin K is a multifunctional vitamin; It has an positive effect on bone. There is elevation in BALP in all Menaquinone 7(K2) groups. Osteoblast produce bone alkaline phosphatase which is positively correlated with the formation of bone. Also, there is significant decrease in NTX in Menaquinone 7(K2) groups which indicate decrease in bone resorption rates at different follow-up times. In addition to significant increase in osteoid tissue formation in Menaquinone 7(K2) groups at the three experimental groups in comparison to control group.
References
- Lam R, Allan B, Goonewardene MS, et al. Success rates of a skeletal anchorage system in orthodontics: A retrospective analysis. Angle Orthod 2017; 88:1-8.
- Kharbanda OP, Samrit V. Mini-screw Implants: AIIMS protocol and contemporary clinical and research studies. J C O 2016; 1:1-4.
- Chugh T, Jain AK, Jaiswal RK, et al. Bone density and its importance in orthodontics. J Oral Biol Craniofac Res 2013; 3:92–97.
- Beulens JW, Booth SL, van den Heuvel EG, et al. The role of menaquinones (vitamin K2) in human health. Br J Nutr 2013; 110:1357–1368.
- Harshman SG, Shea MK. The role of vitamin K in chronic aging diseases: Inflammation, cardiovascular disease, and osteoarthritis. Curr Nutr Rep 2016; 5:90–98.
- Sardana M, Vasim I, Varakantam S, et al. Inactive matrix gla-protein and arterial stiffness in type 2 diabetes mellitus. Am J Hypertens 2017; 30:196–201.
- Buchanan GS, Melvin T, Merritt B, et al. Vitamin K2 (Menaquinone) supplementation and its benefits in cardiovascular disease, osteoporosis, and cancer. Marshall J Med 2016; 2:53-66.
- Jimbo R, Anchieta R, Baldassarri M, et al. Histomorphometry and bone mechanical property evolution around different implant systems at early healing stages: An experimental study in dogs. Implant Den 2013; 22:596-603.
- Suleiman MS. Preservation of surgically extracted tooth socket using β-calcium sulphate hemihydrate prepared from Iraqi gypsum rocks (an experimental study on dogs): PhD Thesis 2015.
- Dhaliwal JS, Murshed M, Feine JS. Osseointegration of standard and mini-dental implants: A histomorphometric comparison. Int J Implant Dent 2017; 3:1-9.
- Borie E, Calzzani R, Dias FJ, et al. Morphometry of rabbit anatomical regions used as experimental models in implantology and oral surgery. Biomed Res 2017; 28:5468-5472.
- Lukiantchuki MA, Filho LI, Iwaki LCV, et al. Histologic and histomorphometric study of bone repair around short dental implants inserted in rabbit tibia, associated with tricalcium phosphate graft bone. Acta Scientiarum Health Sci 2014; 36:257-263.
- Alsandook TA, Alsultan MM, Alzubaidi SH . Histological evaluation of tissues using a bone inducing substance in cases of micro-screw implant "an experimental in Vivo study". Al-Rafidain Dent J 2014; 14:1-8.
- Min Z, Jinxing M, Sheng L, et al. Vitamin K2 analog menaquinone-7 shows osteoblastic bone formation activity in vitro. Biomed Res 2017; 28:1364-1369.
- Koshihara Y, Hoshi K, Okawara R, et al. Vitamin K stimulates osteoblastogenesis and inhibits osteoclastogenesis in human bone marrow cell culture. J Endocrinol 2003; 176:339–348.
- Asawa Y, Amizuka N, Hara K . Histochemical evaluation for the bio logical effect of menatetrenone on metaphyseal trabeculae of ovariectomized rats. Bone 2004; 35:870–880.
- Kim M, Na W, and Sohn C. Vitamin K1 (phylloquinone) and K2 (menaquinone-4) supplementation improves bone formation in a high-fat diet-induced obese mice. Clin Biochem Nutrition 2013; 53:108–113.
- Poon C C, Li RW, Seto SW. In vitro vitamin K(2) and 1alpha,25-dihydroxyvitamin D(3) combination enhances osteoblasts anabolism of diabetic mice. Eur J Pharmacol 2015; 767:30–40.
- Patti A, Gennari L, Merlotti D, et al. Endocrine Actions of osteocalcin. Int J Endocrinol 2013; 2013:846480.
- Theuwissen E, Magdeleyns EJ, Braam LA, et al. Vitamin K-status in healthy volunteers. Food Funct 2014; 5:229-234.
- Julia KDV, Marisa AND ,Virgínia RP, et al. Effect of vitamin K in bone metabolism and vascular calcification: A review of mechanisms of action and evidences. J Critical Reviews Food Sci Nutrition 2017; 57:3959-3970.
- Akbari S, Rasouli-Ghahroudi AA . Vitamin K and bone metabolism: A review of the latest evidence in preclinical studies. Biomed Res Int 2018; :1-8.
- Kameda T, Miyazawa K, Mori Y. Vitamin K2 inhibits osteoclastic bone resorption by inducing osteoclast apoptosis. Biochem Biophy Res Communications 1996; 220:515–519.
- Garnero P, Cloos P, Sornay-Rendu E. Type I collagen racemization and isomerization and the risk of fracture in postmenopausal women: The OFELY prospective study. J Bone Miner Res 2002; 17:826–833.
- Kawata T, Zernik JH, Fujita T, et al. Mechanism in inhibitory effects of vitamin K2 on osteoclastic bone resorption: In vivo study in osteopetrotic (op/op) mice. J Nutritional Sci Vitaminol 1999; 45:501–507.
- Vamsee DM, Eva M. Regulation of bone remodeling by vitamin k2. Oral Dis 2017; 23:1021–1028.
- Wu WJ, Kim MS, Ahn BY. The inhibitory effect of vitamin K on RANKL-induced osteoclast differentiation and bone resorption. Food Funct 2015; 6:3351-3358.
- Setiawati R, Rahardjo P. Bone development and growth, in book, osteogenesis and bone regeneration. Intech Open 2019; 82452.
Author Info
Saba H Alzubaidi1*, Manar M Alnema2, Ghada A Taqa3 and Banan K Al Obaidy4
1Department of Pedodontics Orthodontics Preventive dentistry, College of Dentistry, University of Mosul, Iraq2Department of Oral and Maxillofacial Surgery, College of Dentistry, University of Mosul, Iraq
3Department of Dental Basic Sciences, College of Dentistry, University of Mosul, Iraq
4Left bank Specialized Dental Centre, Mosul, Iraq
Citation: Saba H Alzubaidi, Manar M Alnema, Ghada A Taqa, Banan K Al Obaidy, The effects of Menaquinone 7 on Bone Remodeling Using Biochemical and Histological Analysis (An in vivo Study), J Res Med Dent Sci, 2021, 9 (4):75-79.
Received: 10-Feb-2021 Accepted: 31-Mar-2021
