Research - (2020) Volume 8, Issue 1
Translucency of Recently Introduced Extra High Translucency Zirconia
Mohammad S Alkatheeri1, AbdulAziz Altahtam2, Abdullah Abukhalaf2, Turki Almaslokhi2, Abdulrahman Almusalam2 and Thamer S Almohareb1*
*Correspondence: Thamer S Almohareb, Department of Restorative Dental Science, Dental College, Saudi Arabia, Email:
Abstract
Aim: To compare the translucency of three recently introduced esthetic zirconia, Argen Z Anterior (Argen Corporation), Ceramill Zolid FX (Amann Girrbach AG), and Prettau Anterior (Zirkonzahn), with that of a commonly used esthetic ceramic material (lithium disilicate), IPS e.max CAD LT (Ivoclar Vivadent).
Materials and methods: The three partially sintered zirconia materials were sectioned using a low-speed water-cooled diamond saw into a square shape, and the final dimensions of [10.0 × 10.0 × 1.5 mm] (n=10/group) were acquired after sintering. As a reference group, the partially sintered lithium disilicate (IPS e.max CAD LT) blocks were sectioned and sintered into similar shapes and dimensions. Then, all samples were finished and polished. The CIE L*a*b* values for each sample were measured on a black and a white background using a spectrophotometer (LabScan XE, Hunter Lab). Then, the values of the translucency parameter (TP) were calculated. Furthermore, all samples were reduced to 1.0 mm in thickness, and the TP was obtained for a second reading. Finally, the data were statistically analyzed.
Results: The control group [IPS e.max CAD LT] was significantly more translucent than the other tested groups (P<0.05). The (Ceramill Zolid FX) zirconia material was significantly less translucent than the other two zirconia materials (ArgenZ Anterior and Prettau Anterior Zirkonzahn). There was no significant difference between the TP value of ArgenZ Anterior at the thickness of 1.0 mm and that of the control group at the thickness of 1.5 mm. Conclusion: By decreasing the thickness of the specimens, the TP will be increased. The (ArgenZ Anterior) and (Zirkonzahn) groups were more translucent than the (Ceramill Zolid FX) group. There was no significant difference between the translucency of (ArgenZ Anterior) reduced to 1.0 mm and that of the IPS e.max group at a 1.5 mm thickness (P< 0.05).
Keywords
Translucency, Spectrophotometer, Monolithic, Translucent zirconia, Zirconia, Lithium disilicate
Introduction
With the increased demand for esthetic materials in dentistry, all ceramic restorations have gained more popularity, and their chemical, physical and mechanical properties have been investigated and extensively evaluated [1-7]. Computer-aided design/computer-aided manufacturing CAD/ CAM ceramic restorations have shown in time as a reliable and time-saving treatment method [8-10]. The ceramic block materials available promote the production of different type of dental prosthesis and restorations. However, none of these ceramic materials possess ideal properties for all types of applications [11].
Zirconia (ZrO2), in particular, tetragonal zirconia polycrystals (TZPs), is a ceramic material that has high crystallinity and is characterized by excellent mechanical properties compared to those of other ceramic materials, such as feldspathic porcelain or glass ceramics [12]. Furthermore, with continuing advancement in CAD/CAM technology, machining highstrength zirconia (TZPs) to make ceramic restorations became more feasible, increasing zirconia’s popularity and versatility in clinical applications such as fixed partial dentures, fullcoverage crowns, and implant abutments [13-17]. However, the esthetic properties of zirconia (TZPs), specifically its translucency, remain a major problem [18]. Therefore, layering zirconia (TZPs) with a more esthetic ceramic material as a veneering is often performed Nonetheless, chipping and fracturing of this veneering ceramic material have been reported as a drawback [4,19-21]. To overcome the chipping problem of layered ceramic, tooth-colored fully contoured monolithic zirconia has been made commercially available [22]. However, because of its lack of translucency, the tooth-colored fully contoured monolithic zirconia is limited in clinical application in esthetically demanding areas [23]. To solve this problem, extensive research and development have focused on the production of translucent zirconia [23-28]. Translucency is one of the main characteristics of natural teeth and is considered an important esthetic factor for any material used for dental restoration [6,7]. The translucency parameter (TP) is a measurement that is usually utilized to assess the translucency of dental materials, which is the difference between the color of a material placed over a white backing and that over a black backing as measured by a colorimeter [29]. Recently, new compositions of zirconia, referred to as “extraor super-high translucency zirconia”, have been introduced to the market with a claim of very high translucency and have been promoted for clinical use in anterior teeth. However, since no studies have investigated the material translucency of extra-/super-high-translucency zirconia, the objective of this research is to assess the translucent properties of three recently introduced esthetic zirconia, ArgenZ Anterior (Argen Corporation), Ceramill Zolid FX (Amann Girrbach AG), and Prettau Anterior (Zirkonzahn), and compare them with those of a commonly used esthetic ceramic material, lithium disilicate (IPS e.max CAD LT, Ivoclar Vivadent).
Materials and Methods
The CAD/CAM presintered disks of zirconia (ArgenZ Anterior 98 × 14, Ceramill Zolid FX Amann Girrbach AG 98 × 87.5 × 14, Prettau Anterior Zirkonzahn 98 × 14 and IPS CAD LT BL1/C 14 compositions) were selected for the study, and their compositions were characterized (Table 1). These zirconia disks were cut using a slow-speed water-cooled diamond saw (IsoMet Low Speed Saw, Buehler, Lake Bluff, IL, USA). Taking into account the shrinkage that will occur during sintering, the cutting dimensions of all specimens were determined. All the specimens were sintered in a furnace (VITA Zyrcomat 6000 MS, VITA Zahnfabrik, Germany) following the manufacturer’s instructions.
| Ceramil Zolid fx white | Prettau Anterior | ||
| Component | Percent by weight | Component | Percent by weight |
| ZrO2+ HfO2+Y2O3 | ≥ 99.0 | ZrO2 | Main component |
| Y2O3 | 9.1-9.55 | Y2O3 | <12% |
| HfO2 | ≤ 5.0 | Al2O3 | <1% |
| Al2O3 | ≤ 0.5 | SiO2 | max 0.02% |
| Other oxidees | ≤ 1.0 | Fe2O3 | max 0.02% |
| ArgenZ Anterior | IPS e.max CAD LT | ||
| Component | Percent by weight | Component | Percent by weight |
| ZrO2+HfO2+Y2O3 | >99 % | SiO2 | 57-80% |
| Y2O3 | 8.5-10% | Li2O | 11-19% |
| HfO2 | <5% | K2O | 0-13% |
| Al2O3 | <0.1% | P2O5 | 0-11% |
| Fe2O3 | <0.1% | ZrO2 | 0-8% |
| - | - | ZnO | 0-8% |
| - | - | Al2O3 | 0-5% |
| - | - | MgO | 0-5% |
| - | - | Coloring oxides | 0-8 |
Table 1: Materials composition according to the manufacturer.
To evaluate translucency, square specimens (n=10 per group) were prepared by cutting the tested materials in partially sintered form by a low-speed water-cooled diamond saw (IsoMet Low Speed Saw, Buehler, Lake Bluff, IL, USA) into final dimensions of 10 ± 0.5 mm long, 10 ± 0.5 mm wide, and 1.5 ± 0.1 mm thick. The shrinkage that occurred during the sintering process was considered and accounted for in the cutting dimensions of the specimens. All the specimens were sintered in a furnace (VITA Zyrcomat 6000 MS, VITA Zahnfabrik, Germany) following the manufacturer’s instructions.
To grind and polish both sides of the specimens, 600 and 1200 grit paper was used in a polishing machine. Before each measurement, the specimens were cleaned with distilled water in an ultrasonic machine (Dri-Clave Ultrasonic cleaner, Columbus Dental) for ten minutes and dried with compressed air. The CIE L*a*b* values were measured on a black and a white background with a colorimeter calibrated with a calibration plate positioned at a constant distance from the surface of the specimen using LabScan XE (Hunter Lab). The illumination of the light source corresponded to average daylight (D65). The material translucency was assessed by the TP value, which was measured by calculating the difference in color between the specimens placed against a white background and those placed against a black background with the following equation:
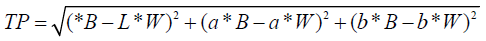
Where L* is brightness, a* is redness to greenness, and b* is yellowness to blueness.
B is the color value of the material measured on the black background, and W refers to the color value of the material measured on the white background. For a second reading, the same samples were reduced to 1.0 mm in thickness, and the TP was obtained again. High translucency and low opacity are indicated as a result of high TP values. For each specimen, the average value of three readings made with its respective background was taken at 1.5 mm and 1.0 mm thicknesses. The TP values for the measured ceramic materials were subjected to statistical analysis using one-way analysis of variance (ANOVA) repeated measurements, followed by paired t-test and independent t-test by using SPSS 12.0 (SAS, Chicago) statistical software with a 5% significance level.
Results
The mean and standard deviation (SD) of the TP [ΔE] for all tested materials measured at 2 different thicknesses are presented in Table 2. The TP of the three zirconia specimens was significantly lower than that of the control group (IPS e.max CAD LT).
| Material | N | Mean | Std. Deviation | P-value | 95% Confidence Interval for Mean | ||
|---|---|---|---|---|---|---|---|
| Lower Bound | Upper Bound | ||||||
| IPS e.max CAD LT | 1.5 mm | 10 | 10.225 | 1.523 | 0 | 9.135 | 11.315 |
| 1.0 mm | 10 | 17.221 | 0.98 | 16.52 | 17.922 | ||
| ArgenZ Anterior | 1.5 mm | 10 | 5.225 | 0.281 | 0 | 5.024 | 5.426 |
| 1.0 mm | 10 | 9.481 | 2.063 | 8.005 | 10.957 | ||
| Ceramil zolid fx | 1.5 mm | 10 | 1.984 | 0.479 | 0.001 | 1.641 | 2.327 |
| 1.0 mm | 10 | 3.217 | 0.674 | 2.735 | 3.699 | ||
| Prettau Anterior | 1.5 mm | 10 | 5.65 | 1.057 | 0 | 4.894 | 6.406 |
| 1.0 mm | 10 | 7.882 | 1.382 | 6.894 | 8.87 | ||
Table 2: Mean ± SD of translucency parameter [ΔE] within all materials tested.
The translucency of the IPS e.max CAD LT group was significantly higher than that of the other tested materials. The difference in the TP was found to be statistically significant between the same materials at 2 different thicknesses. All samples were more translucent at 1.0 mm thickness than at 1.5 mm thickness. Table 3 shows the difference in translucency between the groups within the selected thickness. Zirconia translucency is ordered from the most translucent (highest mean TP value) to the least translucent (lowest mean TP value) [IPS e.max CAD LT, ArgenZ Anterior, Prettau Anterior (Zirkonzahn), Ceramill Zolid FX]. A multiplecomparison test between the materials at a 1.5 mm thickness and those at a 1.0 mm thickness is presented in Table 4. There was no significant difference between the TP of ArgenZ Anterior at the thickness of 1.0 mm and that of the control group at the thickness of 1.5 mm.
| Material | N | Mean | S.D | ANOVA P-Value | Interval for mean | Multiple compression test | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Lower Bound | Upper Bound | IPS e-max | ArgenZ | Ceramil | Zrikonzahn | ||||||
| 1.5 mm | IPS e-max | 10 | 10.225 | 1.523 | 0 | 9.135 | 11.315 | 1 | - | - | - |
| ArgenZ | 10 | 5.225 | 0.281 | 5.024 | 5.426 | 0 | 1 | - | - | ||
| Ceramil | 10 | 1.984 | 0.479 | 1.641 | 2.327 | 0 | 0 | 1 | - | ||
| Zirkonzahn | 10 | 5.65 | 1.057 | 4.894 | 6.406 | 0 | 0.761 | 0 | 1 | ||
| 1.0 mm | IPS e-max | 10 | 17.221 | 0.98 | 0 | 16.52 | 17.922 | 1 | - | - | - |
| ArgenZ | 10 | 9.481 | 2.063 | 8.005 | 10.957 | 0 | 1 | - | - | ||
| Ceramil | 10 | 3.217 | 0.674 | 2.735 | 3.699 | 0 | 0 | - | - | ||
| Zirkonzahn | 10 | 7.882 | 1.382 | 6.5 | 9.264 | 0 | 0.062 | 0 | 1 | ||
Table 3: Comparison between each group within thickness of sample.
| Material | N | Mean | Std. Deviation | Std. Error | Interval of mean | Multiple compression test | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Lower Bound | Upper Bound | IPS e-max | ArgenZ | Ceramil | Zirkonzahn | IPS e-max | ArgenZ | Ceramil | Zirkonzahn | ||||||
| 1.5 mm | 1.5 mm | 1.5 mm | 1.5 mm | 1.00 mm | 1.00 mm | 1.00 mm | 1.00 mm | ||||||||
| 1.5 mm | IPS e-max | 10 | 10.225 | 1.523 | 0 | 9.135 | 11.315 | 1 | - | - | - | - | - | - | |
| ArgenZ | 10 | 5.225 | 0.281 | 5.024 | 5.426 | 0 | 1 | - | - | - | - | - | - | ||
| Ceramil | 10 | 1.984 | 0.479 | 1.641 | 2.327 | 0 | 0 | 1 | - | - | - | - | - | ||
| Zirkonzahn | 10 | 5.65 | 1.057 | 4.894 | 6.406 | 0 | 0.993 | 0 | 1 | - | - | - | - | ||
| 1.00 mm | IPS e-max | 10 | 17.221 | 0.98 | 16.52 | 17.922 | 0 | 0 | 0 | 0 | 1 | - | - | - | |
| ArgenZ | 10 | 9.481 | 2.063 | 8.005 | 10.957 | 0.855 | 0 | 0 | 0 | 0 | 1 | - | - | ||
| Ceramil | 10 | 3.217 | 0.674 | 2.735 | 3.699 | 0 | 0.008 | 0.299 | 0 | 0 | 0 | 1 | |||
| zirkonzahn | 10 | 7.882 | 1.382 | 6.5 | 9.264 | 0.001 | 0 | 0 | 0.002 | 0 | 0.068 | 0 | 1 | ||
Table 4: Multiple comparison test between the materials at two different thicknesses.
Discussion
The translucency of zirconia has been reported to be mainly related to grain size [30,31] and density [31]. In a study performed in 2002, [25] tested different materials and found a significant difference in translucency, which they believed was attributable to differences in the crystal volume and refractive index. Although monolithic zirconia has limited use in esthetic applications due to low translucency and high opacity, cubicphase- containing zirconia showed predictably high translucency and has promising potential for use in esthetic areas.
Tetragonal zirconia has a relatively high refractive index. The addition of alumina, with a different refractive index than zirconia, causes light passing through the alumina-doped zirconia to be sufficiently scattered or absorbed at the grain boundaries so that the zirconia appears relatively opaque. In an initial attempt to produce a more translucent version of zirconia, developers reduced the alumina content from 0.25% to less than 0.05% and improved the processing techniques to control zirconia grain size and processing density to minimize light refraction and increase translucency [32]. In the present study, ArgenZ Anterior and Prettau Anterior (Zirkonzahn) showed significantly higher translucency than Ceramill Zolid FX. This increase in translucency can be related to their composition, which contains cubic phase zirconia. The most recent strategy to increase the translucency of zirconia is to stabilize it with a significant amount of cubic crystalline phase interspersed with the tetragonal phase. Increasing the yttria content to more than 8 mol% will stabilize the cubic phase [32]. The cubic phase of zirconia is isotropic in different crystallographic directions, which decreases the light scattering that occurs at the grain boundaries. As a result, cubic zirconia appears more translucent [32]. Furthermore, thickness is a key factor of light transmittance through zirconia [33,34]. In the present study, there was an inverse relationship between thickness and translucency; translucency increased by decreasing the thickness of the specimens. Additionally, the commonly used esthetic ceramic lithium disilicate (IPS e.max CAD) showed no significant difference in translucency at a 1.5 mm thickness compared to that of the cubicphase- containing zirconia (ArgenZ Anterior) at a 1 mm thickness, considering that the monolithic zirconia crown thickness can be reduced to 1 mm or 0.5 mm, maintaining sufficient strength and fracture resistance [35]. However, further testing of mechanical properties is needed for these specific zirconia materials.
Conclusion
Considering the limitations of the present study, the following conclusions were drawn based on the results:
→ IPS e.max is the most translucent among the materials tested in the present study, followed by ArgenZ Anterior [Argen Corporation].
→ There was an inverse relationship between thickness and translucency; i.e., by decreasing the thickness of the specimens, the TP will be increased.
→ Among the materials marketed as extra high-translucency zirconia, (ArgenZ Anterior) and (Prettau Anterior, Zirkonzahn) were more translucent than (Ceramill Zolid FX).
→ Additionally, the translucency of (ArgenZ Anterior) with a thickness of 1.0 mm is not different from that of the commonly used esthetic ceramic material, lithium disilicate (IPS e.max CAD), with a thickness of 1.5 mm.
Acknowledgments
We would like to express our gratitude to the internship program at the College of Dentistry, King Saud University. In addition, we would like to thank the College of Dentistry Research Center and the Deanship of Scientific Research at King Saud University for their support.
Disclosure of Interest
Authors declare that they have no conflict of interest.
References
- Beuer F, Stimmelmayr M, Gueth JF, et al. In vitro performance of full-contour zirconia single crowns. Den Materials 2012; 28:449-456.
- Komine F, Blatz MB, Matsumura H. Current status of zirconia-based fixed restorations. J Oral Sci 2010; 52:531-539.
- Raigrodski AJ, Chiche GJ, Potiket N, et al. The efficacy of posterior three-unit zirconium-oxide-based ceramic fixed partial dental prostheses: A prospective clinical pilot study. J Prosthet Dent 2006; 96:237-244.
- Al-Amleh B, Lyons K, Swain M. Clinical trials in zirconia: A systematic review. J Oral Rehab 2010; 37:641-652.
- Spear F, Holloway J. Which all-ceramic system is optimal for anterior esthetics? J Am Dent Assoc 2008; 1939:19-24.
- Miyazaki T, Nakamura T, Matsumura H, et al. Current status of zirconia restoration. J Prosthod Res 2013; 57:236-261.
- Huang CW, Hsueh CH. Piston-on-three-ball versus piston-on-ring in evaluating the biaxial strength of dental ceramics. Dent Materials 2011; 27:117-123.
- Fasbinder DJ. The CEREC system: 25 years of chairside CAD/CAM dentistry. J Am Dent Assoc 2010; 141:3-4.
- Giordano R. Materials for chairside CAD/CAM-produced restorations. J Am Dent Assoc 2006; 137:14-21.
- Li RW, Chow TW, Matinlinna JP. Ceramic dental biomaterials and CAD/CAM technology: State of the art. J Prosthod Res 2014; 58:208-216.
- Lambert H, Durand JC, Jacquot B, et al. Dental biomaterials for chairside CAD/CAM: State of the art. J Adv Prosthod 2017; 9:486-495.
- Piconi C, Maccauro G. Zirconia as a ceramic biomaterial. Biomaterials 1999; 20:1-25.
- Tinschert J, Zwez D, Marx R, et al. Structural reliability of alumina, feldspar, leucite, mica and zirconia-based ceramics. J Dent 2000; 28:529-35.
- Matta RE, Schmitt J, Wichmann M, et al. Circumferential fit assessment of CAD/CAM single crowns: A pilot investigation on a new virtual analytical protocol. Quintessence Int 2012; 43:801-809.
- Kohorst P, Herzog TJ, Borchers L, et al. Load-bearing capacity of all-ceramic posterior four-unit fixed partial dentures with different zirconia frameworks. Eur J Oral Sci 12007; 15:161-166.
- Chen YM, Smales RJ, Yip KH, et al. Translucency and biaxial flexural strength of four ceramic core materials. Dent Materials 2008; 24:1506-1511.
- Adatia ND, Bayne SC, Cooper LF, et al. Fracture resistance of yttria-stabilized zirconia dental implant abutments. J Prosthod 2009; 18:17-22.
- Zhang Y. Making yttria-stabilized tetragonal zirconia translucent. Dent Materials 2014; 30:1195-1203.
- Feher SA, Filser F, Luthy H, et al. Prospective clinical study of zirconia posterior fixed partial dentures: 3-year follow-up. Quintessence Int 2006; 37:685-693.
- Feher SA, Filser F, Gauckler LJ, et al. Five-year clinical results of zirconia frameworks for posterior fixed partial dentures. Int J Prosthod 2007; 20:383-388.
- Roediger M, Gersdorff N, Huels A, et al. Prospective evaluation of zirconia posterior fixed partial dentures: Four-year clinical results. Int J Prosthod 2010; 23:141-148.
- Raigrodski AJ. Contemporary materials and technologies for all-ceramic fixed partial dentures: A review of the literature. J Prost Dent 2004; 92:557-562.
- Baldissara P, Llukacej A, Ciocca L, et al. Translucency of zirconia copings made with different CAD/CAM systems. J Prost Dent 2010; 104:6-12.
- Heffernan MJ, Aquilino SA, Diaz-Arnold AM, et al. Relative translucency of six all-ceramic systems. Part II: Core and veneer materials, J Prost Dent 2002; 88:10-15.
- Heffernan MJ, Aquilino SA, Diaz-Arnold AM, et al. Relative translucency of six all-ceramic systems. Part I: Core materials. J Prost Dent 2002; 88:4-9.
- Ozturk O, Uludag B, Usumez A, et al. The effect of ceramic thickness and number of firings on the color of two all-ceramic systems. J Prost Dent 2008; 100:99-106.
- Spyropoulou PE, Giroux EC, Razzoog ME, Translucency of shaded zirconia core material. J Prost Dent 2011; 105:304-307.
- Sachs C, Groesser J, Stadelmann M, et al. Full-arch prostheses from translucent zirconia: Accuracy of fit. Dent Materials 2014; 30:817-823.
- Silva NR, Bonfante EA, Zavanelli RA, et al. Reliability of metalloceramic and zirconia-based ceramic crowns. J Dent Res 2010; 89:1051-1056.
- Stawarczyk B, Ozcan M, Hallmann L, et al. The effect of zirconia sintering temperature on flexural strength, grain size, and contrast ratio. Clin Oral Investigations 2013; 17:269-274.
- Kim MJ, Ahn JS, Kim JH, et al. Effects of the sintering conditions of dental zirconia ceramics on the grain size and translucency. J Adv Prost 2013; 5:161-166.
- McLaren EA, Lawson N, Choi J, et al. New high-translucent cubic-phase-containing zirconia: Clinical and laboratory considerations and the effect of air abrasion on strength. Compendium Cont Edu Dent 2017; 38:13-16.
- Kelly JR, Nishimura I, Campbell SD. Ceramics in dentistry: Historical roots and current perspectives. J Prost Dent 1996; 75:18-32.
- Watts DC, Cash AJ. Analysis of optical transmission by 400-500 nm visible light into aesthetic dental biomaterials. J Dent 1994; 22:112-117.
- Sorrentino R, Triulzio C, Tricarico MG, et al. In vitro analysis of the fracture resistance of CAD-CAM monolithic zirconia molar crowns with different occlusal thickness. J Mech Behavior Biomed Materials 2016; 61:328-333.
Author Info
Mohammad S Alkatheeri1, AbdulAziz Altahtam2, Abdullah Abukhalaf2, Turki Almaslokhi2, Abdulrahman Almusalam2 and Thamer S Almohareb1*
1Department of Restorative Dental Science, Dental College, Riyadh, Saudi Arabia2Internship Program, Dental College, Riyadh, Saudi Arabia
Citation: Mohammad Alkatheeri, AbdulAziz Altahtam, Abdullah Abukhalaf, Turki Almaslokhi, Abdulrahman Almusalam, Thamer Almohareb, Translucency of Recently Introduced Extra High Translucency Zirconia, J Res Med Dent Sci, 2020, 8(1):175-180.
Received: 01-Oct-2020 Accepted: 02-Jun-2020
