Case Report - (2021) Volume 9, Issue 1
Venous Malformation in the Lower Lip Treated with Sclerotherapy and Surgery-A Case Report
Mashail Mahmoud Mahgoub Hamid1,2*, Mohammed Hassan Aljezoli2 and Mohammed A Higzi2
*Correspondence: Mashail Mahmoud Mahgoub Hamid, College of Dentistry, King Khalid university, Saudi Arabia, Email:
Abstract
Vascular malformations in the maxillofacial region present several challenges; Sclerotherapy with ethanolamine oleate (EO) is an effective and recommended treatment modality. A 6-year-old girl presented to our institution with an enlarged lower lip and was diagnosed as a low-flow venous malformation. 5% EO was injected as the sclerosing agent. The patient underwent a total of 4 sessions of sclerotherapy, separated by intervals of 2 weeks and when the lesion had decreased in size surgical recontouring under general anesthesia was performed. Postoperative aesthetic and functional outcomes were excellent without recurrence. The findings of this case suggest that sclerotherapy followed by surgery is a very efficient method of treatment of venous malformation.
Keywords
Venous malformation, Lip, Ethanolamine oleate
Introduction
Vascular anomalies are abnormalities of blood vessels or endothelial cells. The two most common types are hemangiomas and vascular malformations which may appear to be remarkably similar but differ in their pathogenesis and clinical behavior and subsequently the treatment modalities. Vascular malformations are irregular vascular networks defined by their blood vessel type; they are present at birth, slow- growing, infiltrative, and destructive. Intervention is usually required for almost all vascular malformations while may be needed for nearly 40% of hemangiomas [1].
Case Presentation
A 6-year-old girl presented to the Department of Oral and Maxillofacial Surgery at Khartoum Teaching Dental Hospital complaining of a diffuse swelling in the lower lip. The swelling had been noticed by the patient’s mother at birth, it started as a small nodule that increased in size gradually with time, No history of trauma was given by the parents. The lesion was not associated with pain or pus discharge, it bled occasionally due to trauma. The patient did not undergo any treatment as the case was misdiagnosed by another surgeon as being a case of haemangioma that may undergo spontaneous involution and should be conservatively monitored without intervention.
On examination, a diffuse swelling involving the whole lip was present resulting in it prolapse. On palpation, the swelling was ill-defined, soft in consistency and non-tender. Affected mucosa was pinkish in color, with a smooth and thickened surface (Figure 1A).
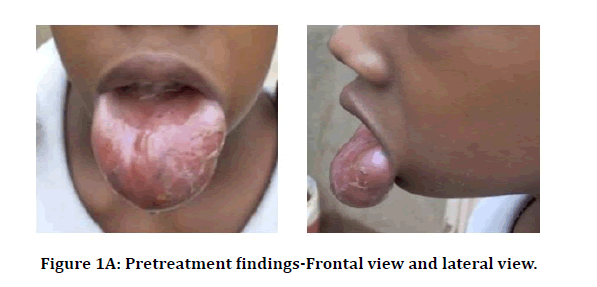
Figure 1A: Pretreatment findings-Frontal view and lateral view.
Differential diagnosis
The differential diagnosis was either: vascular
malformation or hemangioma. However vascular
low-flow malformation was considered due to
the pinkish-purple aspect, consistency, absence
of vascular pulsation. CT Angiography showed
a flow through the lower lip and the feeding
vessel was the inferior labial vein (Figure 1B). 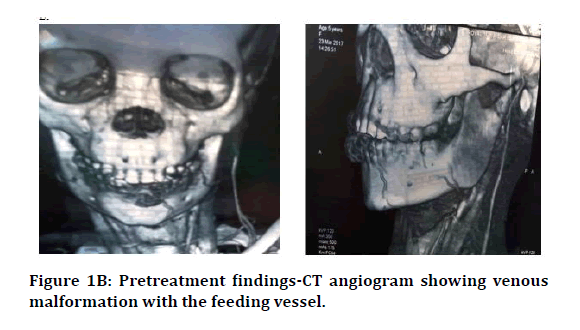
Figure 1B: Pretreatment findings-CT angiogram showing venous malformation with the feeding vessel.
The lesion was diagnosed as a low-flow-type vascular malformation (venous malformation). The treatment plan was to reduce the size of the lesion using a sclerosing agent followed by surgical recontouring of the lip.Management
Sclerotherapy was performed using 5% ethanolamine oleate. An infiltration of local anesthesia 2% Lidocaine) was given with rubbing a cotton swab on the surface of the anomaly to minimize puncture discomfort, then the drug was injected with a Short Needle Insulin Syringe with manual pressure on the lip during injection to interrupt blood flow and prevent leakage of the sclerosing agent. The sclerosing agent was administered 4 times at 2 weeks of interval. Each time, 2 ml of the sclerosing agent was injected. A decrease in the size of the lesion with localized fibrosis was apparent after each session.
Total excision of the residual lesion was performed under general anesthesia. Superficial mucosa and muscular layer were excised along with the lesion by locally ligating the inferior labial vessels, lip plasty was performed, Bleeding was locally controlled with suction and diathermy, the defect was primarily closed. The patient has since been followed, with no signs of recurrence (Figure 2).
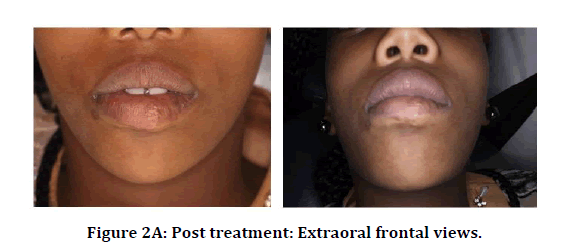
Figure 2A: Post treatment: Extraoral frontal views.
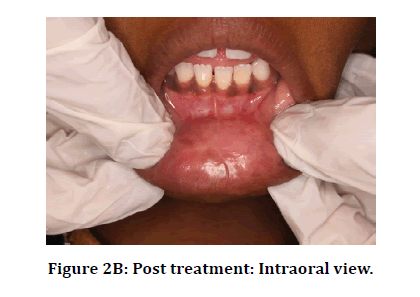
Figure 2B: Post treatment: Intraoral view.
Discussion
Vascular malformations are abnormal development of blood vessels. Clinically lesions present as soft, non-pulsating mass. The lesions fill with dependency and are compressible [2,3]. Patients’ complaints usually include progressive growth, disfigurement, pain, shortness of breath, and dysphagia [4].
Sclerotherapy is an effective and minimally invasive technique, it is the first-line treatment for vascular malformations, providing healing rates of 70% -100%. The low flow rate of venous malformation makes sclerotherapy an effective treatment, allowing effective concentrations of sclerosing agents to remain nearly constant when delivered directly to the lesion [5-8].
Although many sclerosing agents are available, such as sodium morrhuate, sodium psylliate, Ethanolamine oleate is particularly useful because of its low toxicity compared to other sclerosis inducing agents [6,9,10]. Ethanolamine oleate is an anionic detergent when applied intravenously damages the endothelium by its detergent action and induces inflammation and fibrosis by the formation of intravariceal thrombi [11].
Previous studies on the effectiveness of sclerotherapy with ethanolamine oleate confirm that it is a well-tolerated and sufficient method with a high success rate and high patient satisfaction. It has good sclerosing action, as well as its minor adverse effects [5,12-18]. Even when the sclerotherapy with monoethanolamine reduced the lesion only partially, it provided good preparation for further surgery either for excision of residual lesion or esthetic improvement by excision of scar tissues [19,20].
Although benign lesions, venous malformation can present a diagnostic and management challenge. A multidisciplinary approach is strongly recommended as there is no single superior treatment modality. Surgery remains one of the most superior treatment options and may offer a cure for localized venous malformation. However, excision of complex lesions remains difficult secondary to intraoperative bleeding and undesirable functional and cosmetic outcomes. On the other hand, although sclerotherapy is one of the most effective treatment methods, patients with large lesions, sclerotherapy alone is usually inadequate to keep the lesion under control, and surgery is then considered to remove the residual lesion. Therefore, the best treatment protocol is to perform sclerotherapy initially to control the lesion progression then should be followed by surgery [1,3,4,21].
Conclusion
This case demonstrates that sclerotherapy of venous malformation by injection of 5% ethanolamine oleate into the lesion was an effective treatment. It provided rapid and safe involution of the lesion with satisfactory outcomes. Misdiagnosis of vascular lesions can lead to mismanagement and delays treatment.
Ethical Approval
Treatment consent: The patient’s parents formally consented with the procedures and were informed about the possible complications of the procedures.
Consent for Publication
The authors used non identifiable photographs and no identifying details were mentioned in the report.
Conflict of Interest
The authors have disclosed no potential conflicts of interest, financial, commercial or otherwise.
References
- Richter GT, Friedman AB. Hemangiomas, and vascular malformations: Current theory and management. Int J Pediatr 2012; 2012:645678.
- Aboelatta YA, Nagy E, Shaker M, et al., Venous malformations of the head and neck: A diagnostic approach and a proposed management approach based on clinical, radiological, and histopathology findings. Head Neck 2014; 36:1052-1057.
- Buckmiller LM, Richter GT, Suen JY. Diagnosis and management of hemangiomas and vascular malformations of the head and neck. Oral Dis 2010; 16:405-418.
- Glade RS, Richter GT, James CA, et al. Diagnosis and management of pediatric cervicofacial venous malformations: Retrospective review from a vascular anomalies center. Laryngoscope 2010; 120:229-35.
- Bonan PR, Miranda LD, Mendes DC, et al. Effectiveness of low flow vascular lesions sclerosis with monoethanolamine: Report of six cases. Med Oral Patol Oral Cir Bucal 2007; 12:E524-527.
- Costa JR, Torriani MA, Hosni ES, et al. Sclerotherapy for vascular malformations in the oral and maxillofacial region: Treatment and follow-up of 66 lesions. J Oral Maxillofac Surg 2011; 69:88-92.
- Da Silva WB, Ribeiro AL, de Menezes SA, et al. Oral capillary hemangioma: A clinical protocol of diagnosis and treatment in adults. Oral Maxillofac Surg 2014; 18:431-437.
- Fernandes DT, Rogério-de Andrade Elias RS, Silva PA, et al. Benign oral vascular lesions treated by sclerotherapy with ethanolamine oleate: A retrospective study of 43 patients. Med Oral Patol Oral Cir Bucal 2018; 23:e180-e187.
- Johann AC, Aguiar MC, do Carmo MA, et al. Sclerotherapy of benign oral vascular lesion with ethanolamine oleate: An open clinical trial with 30 lesions. Oral Surg Oral Med Oral Pathol Oral Radiol Endod, 2005; 100:579-584.
- Dilsiz A, Aydin T, Gursan N. Capillary hemangioma as a rare benign tumor of the oral cavity: A case report. Cases J 2009; 2:8622.
- Nishida R, Inoue R, Takimoto Y, et al. A sclerosant with astringent properties developed in China for oesophageal varices: Comparison with ethanolamine oleate and polidocanol. J Gastroenterol Hepatol 1999; 14:481-488.
- de Oliveira CD, Ribeiro MC, do Amaral MB, et al. Experience with 5% ethanolamine oleate for sclerotherapy of oral vascular anomalies: A cohort of 15 consecutive patients. J Craniomaxillofac Surg 2019; 47:106-111.
- Ribeiro MC, Grossmann SD, do Amaral MB, et al. Effectiveness and safety of foam sclerotherapy with 5% ethanolamine oleate in the treatment of low-flow venous malformations in the head and neck region: A case series. Int J Oral Maxillofac Surg, 2018; 47:900-907.
- Qiu Y, Chen H, Lin X, et al. Outcomes and complications of sclerotherapy for venous malformations. Vasc Endovascular Surg 2013; 47:454-461.
- Gomes CC, Gomez RS, Do Carmo MA, et al. Mucosal varicosities: Case report treated with monoethanolamine oleate. Med Oral Patol Oral Cir Bucal 2006; 11:44-46.
- Das BK, Hoque S. Treatment of venous malformations with ethanolamine oleate. Asian J Surg 2008; 31:220-224.
- Horbach SE, Lokhorst MM, Saeed P, et al. Sclerotherapy for low-flow vascular malformations of the head and neck: A systematic review of sclerosing agents. J Plast Reconstr Aesthet Surg 2016; 69:295-304.
- Masaki M, Obara K, Suzuki S, et al. The destructive effects of sclerosant ethanolamine oleate on mammalian vessel endothelium. Gastroenterol Jpn 1990; 25:230-235.
- Tabe S, Habu M, Kawano M, et al. Venous malformation at the upper lip treated with sclerotherapy–A case report. J Oral Maxillofac Surg Med Pathol 2019; 31:204-207.
- Matsumoto K, Nakanishi H, Koizumi Y, et al. Sclerotherapy of hemangioma with late involution. Dermatol Surg 2003; 29:668-671.
- Sohail M, Bashir MM, Ansari HH, et al. Outcome of management of vascular malformations of lip. J Craniofac Surg, 2016; 27:e520-e524.
Author Info
Mashail Mahmoud Mahgoub Hamid1,2*, Mohammed Hassan Aljezoli2 and Mohammed A Higzi2
1College of Dentistry, King Khalid university, Saudi Arabia2University of Khartoum, Sudan
Citation: Mashail Mahmoud Mahgoub Hamid, Mohammed Hassan Aljezoli, Mohammed A Higzi, Venous Malformation in the Lower Lip Treated with Sclerotherapy and Surgery–A Case Report, J Res Med Dent Sci, 2021, 9 (1): 105-108.
Received: 12-Sep-2020 Accepted: 11-Dec-2020
