Research - (2021) Volume 9, Issue 4
Anemia in Type 2 Diabetes Mellitus as a Risk Factor for the Presence and Severity of Microvascular Complication-Diabetic Retinopathy
Kalagara Srirupa Tejasvi and P Manimekalai*
*Correspondence: P Manimekalai, Department Of General Medicine, Sree Balaji Medical College and Hospital, Bharath Institute of Higher Education and Research, India, Email:
Abstract
Aims and objectives: To estimate the prevalence of anemia in patients with type 2 diabetes mellitus. To assess the role of anemia as a risk factor for the presence and the severity of diabetic retinopathy among the diabetic in-patients and out-patients of Sree Balaji Medical College & Hospital, Chennai.
Methods: Single centre, cross-sectional analytical study was done. 100 patients who met the inclusion, as well as exclusion criteria, were included in the study. The study was conducted among the in-patients as well as out-patients of the Department of General Medicine, Sree Balaji Medical College & Hospital, Chennai.
Results: In our study, we observed that diabetic individuals had a higher prevalence of anemia of 69% when compared to the general population. We observed that anemia was more prevalent among the females, older age group and longer duration of diabetes mellitus.
Conclusion: Diabetic individuals have a higher prevalence of anemia than non-diabetic individuals. Anemia can be considered as an independent risk factor in the presence and severity of diabetic retinopathy. Diabetic Retinopathy, Anemia, Type 2 Diabetes Mellitus.
Keywords
Diabetic retinopathy, Diabetes mellitus, Type 2 diabetes, Anemia, Cerebrovascular disease
Introduction
Aretaeus of Cappadocia coined the term “Diabetes”. He was an eminent Pneumatic School physicist who lived in the 2nd century AD in Alexandria and Rome. Appolinaire Bouchardat (1806-1886), the French ophthalmologist and Professor of Hygiene in Paris, reported the development of visual loss without cataract in diabetics in 1846. This was partially reversible, and the change was associated with better diabetes management in most cases. Similar remarks were made by Francois Tavignot few years later. The theory, however, was not proven until the ophthalmoscope invention. Diabetes mellitus is the term used for a category of metabolic disorders that share the common hyperglycemic phenotype.
There are approximately 40 different types of Diabetes Mellitus. Type 1 DM, Type 2 DM, MODY, GDM to name a few. Type 1 Diabetes Mellitus is the result of autoimmune destruction of pancreatic beta cells, resulting in absolute insulin deficiency. Type 2 Diabetes Mellitus is predominantly due to insulin resistance. Diabetes due to genetic mutations is categorized as MODY. Hyperglycemia has toxic effects on the body. They are broadly classified into acute and chronic complications. Diabetic Ketoacidosis is usually seen in type 1 DM whereas Hyperglycemic Hyperosmolar State predominantly is seen in type 2 DM individuals. Retinopathy, Nephropathy and Neuropathy constitute the microvascular complications of Diabetes Mellitus. Macrovascular complications include Peripheral Arterial Disease, Coronary artery disease, and Cerebrovascular disease. Other complications include Gastroparesis, Cherioarthropathy, Cataracts, Glaucoma, Hearing loss. As of 2014, 422 million people in the world have Diabetes Mellitus [1].
Diabetic Retinopathy is defined as the characteristic group of lesions in the retina that occur in individuals who had diabetes for long. Diabetic Retinopathy is considered as the priority eye diseases by the WHO. It is estimated that in 2002, diabetic retinopathy accounted for about 5% of world blindness, amounting to 5 million people turning blind [2]. Therefore, it is recommended by the ADA for annual or biannual fundus examination and laser therapy if indicated. It is included under the VISION 2020 to reduce the burden of blindness due to diabetic retinopathy. Retinopathy is a leading cause of blindness in the diabetic population. Blindness is 25 times more common in diabetic patients than non-diabetic. Diabetic retinopathy is ranked as the sixth common cause of blindness in India. While a few patients with type 2 diabetes mellitus may have retinopathy at the time of diagnosis, almost 60% of patients with type 2 DM will have retinopathy after two decades. The availability of resources for preventing, diagnosing and treating the devastating effects of retinopathy on vision is a major issue at present [3].
The incidence of diabetic retinopathy increases as age advances. The risk of diabetic retinopathy is greater between the age of 30-60years. Many risk factors are known to play a role in the incidence of diabetic retinopathy. Duration of diabetes is one of the most important risk factors. Other risk factors include uncontrolled diabetes, pregnancy, hypertension, nephropathy, hyperlipidemia, smoking, cataract surgery, obesity, and anemia. Anemia is more common in the diabetic population than the general population. Among diabetic individuals, anemia can develop faster and more severe than in patients with renal impairment from other causes. According to World Health Organization, anemia is defined as Hb < 13g/dl in men and Hb< 12g/dl in women at sea level.
This definition by WHO when applied to the population, it was found that 25% of patients with diabetes have anemia. On average, 1 in 4 individuals with diabetes has anemia. The causes of anemia in diabetic individuals are nutritional deficiency due to diabetes, medications used for diabetes and diabetes related conditions and erythropoietin deficiency due to diabetic nephropathy. It can be considered that diabetic individuals who are anemic are more prone to develop retinopathy, cardiovascular and cerebrovascular events. People who have both anemia and diabetes tend to have a shorter lifespan than those who have diabetes but not anemia [4]. There are many theories regarding the presence of anemia and the role in the development of complications. One of them being that anemia can result in a false low level of HbA1C, leading to under-treatment of hyperglycemia, leading to the progression of micro and macrovascular complications [5]. Gender also has a profound influence on the prevalence of anemia. According to many studies, anemia can be the sole risk factor for the development of retinopathy. There are also observations made which suggest that severity of retinopathy in a diabetic individual depends on the presence of anemia.
Materials and Methods
✓ The study was conducted among the inpatients and out-patients of Sree Balaji Medical College and Hospital, Chennai.
✓ Most of them were in-patients of the General Medicine Ward of Sree Balaji Medical College & Hospital, Chennai.
✓ This study was conducted from November 2017 to July 2019.
✓ A total of 100 patients were taken for the study.
Study design: Cross-sectional, Analytical study.
Sample size: 100.
Inclusion criteria
✓ All the patients had type 2 Diabetes Mellitus.
✓ All the patients selected for the study were attending the out-patient and in-patient departments of General Medicine at Sree Balaji Medical College and Hospital, Chennai.
✓ All the patients selected for the study were more than 40 years of age.
Exclusion criteria
✓ Type 1 Diabetes Mellitus patients were excluded from the study.
✓ Subjects with age below 40 years were excluded from the study.
Among the patients selected for the study, the following variables were taken into consideration.
✓ Age.
✓ Gender.
✓ Duration of diabetes mellitus.
✓ Hemoglobin.
✓ Blood Urea.
✓ Creatinine.
✓ Diabetic Retinopathy and its grades.
Age
Patients were categorized based on age as follows.
✓ 40-49 years
✓ 50-59 years.
✓ 60-69 years.
✓ ≥ 70 years.
Gender
Among the 100 patients chosen for the study, 55 were females, 45 were males.
Duration of diabetes
Duration of diabetes was categorized as
✓ <5 years.
✓ ≥ 5 years.
Results
The study was conducted among 100 inpatients and outpatients of the Department of General Medicine at Sree Balaji Medical College & Hospital, Chennai. The estimation of hemoglobin, blood urea and creatinine were done. Fundus examination was done for all the patients and it was graded based on ETDRS (Early Treatment Diabetic Retinopathy Study). The effect of anemia on the presence and severity of diabetic retinopathy was assessed. The severity of retinopathy was also compared with gender, age, duration of diabetes and blood urea and serum creatinine values.
The collected data were analysed with IBM. SPSS statistics software 23.0 Version. To describe about the data descriptive statistics frequency analysis, percentage analysis was used for categorical variables and the mean & S.D were used for continuous variables. To find the significant difference between the bivariate samples in independent groups the Unpaired sample t -test was used. To find the significance in categorical data Chi-Square test was used. In both the above statistical tools the probability value 0.05 is considered as significant level. In our study of 100 individuals, patients of age more than 40 years were included in the study. Most of the individuals were 40-49years old constituting 36% of the study population. Around 69% of the individuals had anemia in our study, and it was more prevalent in the age group ≥ 70 years. Almost everybody who was more than 70 years of age was found to be anemic. The prevalence of anemia increased with age of the patient and was found to be statistically significant with p-value 0.035 (Table 1 and Figure 1).
| Age group | Frequency | Percent |
|---|---|---|
| 40-49 yrs. | 36 | 36 |
| 50-59 yrs. | 22 | 22 |
| 60-69 yrs. | 28 | 28 |
| >= 70 yrs. | 14 | 14 |
| Total | 100 | 100 |
Table 1: Age distribution.
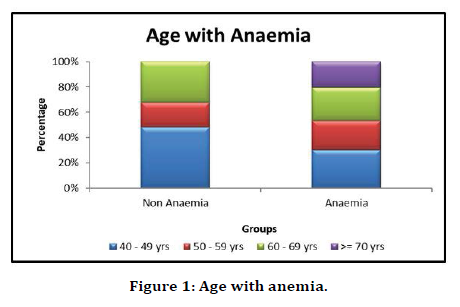
Figure 1. Age with anemia.
Among 100 individuals in the study. 55 of them were females. Out of which, 43 individuals had anemia, amounting to a prevalence of 78.2%. Anemia was more prevalent among females. The gender distribution with anemia was found to be statistically significant at p-value 0.028 (Table 2 and Figure 2).
| Frequency | Percentage | |
|---|---|---|
| Female | 55 | 55 |
| Male | 45 | 45 |
| Total | 100 | 100 |
Table 2: Gender distribution.
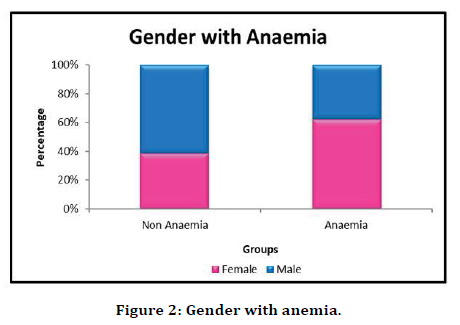
Figure 2. Gender with anemia.
The study population was divided into two groups. Patients who have had Diabetes for less than five years and those who had Diabetes for more than five years. Out of 100 patients, 44 patients had diabetes for less than five years. Among the 44 patients, 24 patients had anemia, amounting to a prevalence of 54.5% among patients who had diabetes for less than 5 years. 80.3% of individuals who had diabetes for more than 5 years duration had anemia. The difference between duration of diabetes and prevalence of anemia was found to be highly statistically significant with p-alue 0.006 (Figure 3 and Figure 4).
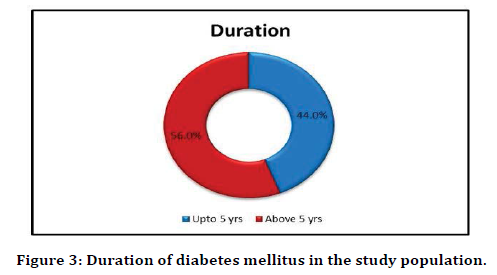
Figure 3. Duration of diabetes mellitus in the study population.
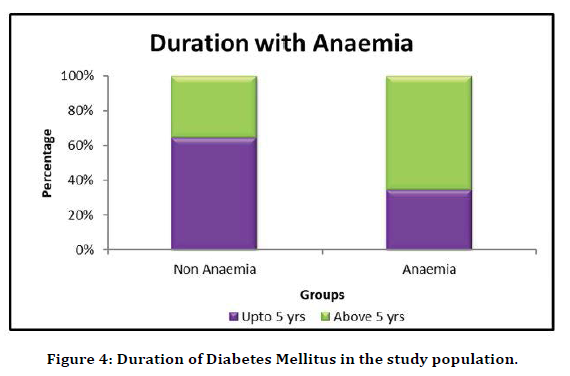
Figure 4. Duration of Diabetes Mellitus in the study population.
In our study, 69% of the individuals were anemic. Fundus changes were broadly classified as the presence and absence of diabetic retinopathy. Among the study population, 43% of the individuals had diabetic retinopathy. On comparing the two variables, it was observed that 55.1% of the individuals had both diabetic retinopathy as well as anemia. The comparison between diabetic retinopathy and anemia was found to be highly statistically significant with p-value 0.0005 (Table 3 and Figure 5).
| Diabetic retinopathy | Frequency | Percentage |
|---|---|---|
| No | 57 | 57 |
| Yes | 43 | 43 |
| Total | 100 | 100 |
Table 3: Distribution of diabetic retinopathy.
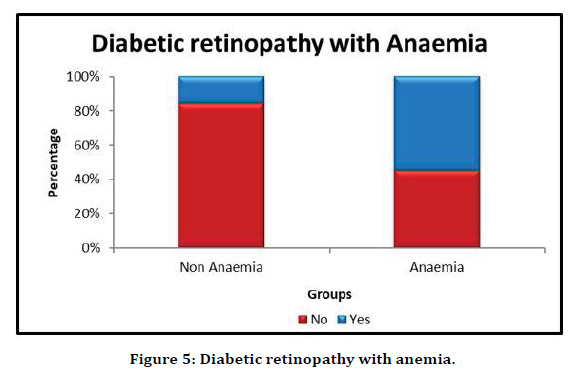
Figure 5. Diabetic retinopathy with anemia.
Fundus examination of all individuals in the study population was done. The findings were reported as diabetic retinopathy absent, mild NPDR, moderate NPDR, severe NPDR, PDR and CSME. Diabetic retinopathy was seen in 43% of the individuals. 12 people had moderate NPDR, amounting to 28% of diabetic retinopathy. It was observed that Diabetic Retinopathy was more prevalent among anemic individuals (Table 4 and Figure 6).
| Grade of Retinopathy | Frequency | Percent |
|---|---|---|
| Absent | 61 | 61 |
| CSME | 8 | 8 |
| PDR | 10 | 10 |
| Mild NPDR | 6 | 6 |
| Moderate NPDR | 12 | 12 |
| Severe NPDR | 3 | 3 |
| Total | 100 | 100 |
Table 4: Grades of retinopathy distribution.
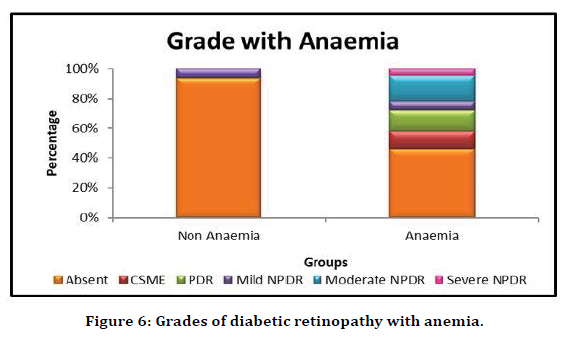
Figure 6. Grades of diabetic retinopathy with anemia.
In our study, it was seen that diabetic retinopathy was slightly more prevalent among males. Out of the 43 individuals who had diabetic retinopathy, 23 were males constituting 53.48%. Males had higher prevalence of CSME as well as PDR. Out of 10 individuals who had PDR, 7 were males, constituting 70%. 5 out of 8 individuals who had CSME were males, amounting to 62.5%. mild NPDR and moderate NPDR were seen in equal numbers among the males and females. But, as the males had higher prevalence of diabetic retinopathy, the prevalence of mild NPDR and moderate NPDR was higher among females. No statistics can be computed for this observation as gender is a constant variable (Table 5 and Table 6).
| Gender | |||||
|---|---|---|---|---|---|
| Female | Male | Total | |||
| Grade | Absent | Count | 35 | 22 | 57 |
| % | 100.00% | 100.00% | 100.00% | ||
| Total | Count | 35 | 22 | 57 | |
| % | 100.00% | 100.00% | 100.00% | ||
Table 5: Absence of diabetic retinopathy among males and females.
| Gender | Total | ||||
|---|---|---|---|---|---|
| Female | Male | ||||
| Grade | Absent | Count | 3 | 1 | 4 |
| % | 15.00% | 4.30% | 9.30% | ||
| CSME | Count | 3 | 5 | 8 | |
| % | 15.00% | 21.70% | 18.60% | ||
| Mild NPDR | Count | 3 | 3 | 6 | |
| % | 15.00% | 13.00% | 14.00% | ||
| Moderate NPDR | Count | 6 | 6 | 12 | |
| % | 30.00% | 26.10% | 27.90% | ||
| PDR | Count | 3 | 7 | 10 | |
| % | 15.00% | 30.40% | 23.30% | ||
| Severe NPDR | Count | 2 | 1 | 3 | |
| % | 10.00% | 4.30% | 7.00% | ||
| Total | Count | 20 | 23 | 43 | |
| % | 100.00% | 100.00% | 100.00% | ||
Table 6: Grades of diabetic retinopathy among males and females.
Diabetic Retinopathy was more prevalent among the individuals who had Diabetes for more than five years of duration. Out of 43 individuals who had diabetic retinopathy, 36 individuals had diabetes for longer than five years. In our study, 56 individuals had diabetes longer than five years. It was seen that 36 out of 56 individuals had diabetic retinopathy, amounting to 64.28%. Mild NPDR, Moderate NPDR, Severe NPDR, PDR and CSME all were seen in higher proportion in individuals who had diabetes for longer duration. No statistics can be computed for this observation as gender is a constant variable (Table 7).
| Duration | Total | ||||
|---|---|---|---|---|---|
| Up to 5 yrs. | Above 5 yrs. | ||||
| Grade | Absent | Count | 37 | 20 | 57 |
| % | 100.00% | 100.00% | 100.00% | ||
| Total | Count | 37 | 20 | 57 | |
| % | 100.00% | 100.00% | 100.00% | ||
Table 7: Absence of diabetic retinopathy vs duration of diabetes.
Discussion
In our study of 100 patients, we studied the significance of anemia as a risk factor for the severity and presence of diabetic retinopathy. We also compared anemia as a potential risk factor with other factors such as age, gender, duration of diabetes mellitus. We also studied the prevalence of anemia in diabetic individuals [6,7]. It was observed in our study that anemia was more prevalent among diabetic individuals than the general population. Our study had an anemia prevalence rate of 69%. Anemia was more prevalent among both males and females when compared to the general population. In our study, anemia was more prevalent among patients of age more than 70 years than any other age group. The prevalence of anemia with difference in age was found statistically significant with age group, p-value 0.035.
In our study, females had a higher prevalence of anemia, with a prevalence rate of 78.18%. The distribution of sex with anemia at p-value 0.028 was found to be statistically significant. In our study, patients with longer duration of Diabetes Mellitus had a higher prevalence of anemia. 80.3% of individuals who had diabetes for more than 5 years of duration had anemia. The difference between duration of diabetes and prevalence of anemia was found to be highly statistically significant with p-value 0.006 [8].
In our study, 69% of the individuals were anemic. 55.1% of the individuals had both diabetic retinopathy as well as anemia. The comparison between diabetic retinopathy and anemia was found to be highly statistically significant with p-value 0.0005. Diabetic retinopathy was seen in 43% of the individuals. 12 people had moderate NPDR, amounting to 28% of diabetic retinopathy. It was observed that Diabetic Retinopathy was more prevalent among anemic individuals. Moderate NPDR, severe NPDR, PDR and CSME were seen only among the anemic individuals. Mild NPDR was seen in non-anemic individuals as well as anemic individuals but, the prevalence was more among the anemic patients with Diabetes. The grades of retinopathy, when compared with anemia, was found to be highly statistically significant with a p-value of 0.0005 [4,9,10].
In our study, it was seen that diabetic retinopathy was slightly more prevalent among males. Out of the 43 individuals who had diabetic retinopathy, 23 were males constituting 53.48%. Males had higher prevalence of CSME as well as PDR. Out of 10 individuals who had PDR, 7 were males, constituting 70%. 5 out of 8 individuals who had CSME were males, amounting to 62.5%. Mild NPDR and moderate NPDR were seen in equal numbers among the males and females. But, as the males had higher prevalence of diabetic retinopathy, the prevalence of mild NPDR and moderate NPDR was higher among females. The purpose of this study is to elucidate the importance of early detection of retinopathy [11]. Retinopathy when treated earlier can prevent permanent blindness, thereby reducing the burden of blindness in the world. Elucidating anemia as a risk factor for diabetic retinopathy improves the prognosis of diabetic retinopathy. Anemia being a modifiable risk factor for diabetic retinopathy, when treated at the right time can delay the progression to severe grades of retinopathy [12-15].
It was reported by Friedman and associates [16] that the treatment of anemia with erythropoietin was correlated with substantial resolution of macular hard exudates among the individuals who had both diabetes mellitus and anemia. On treating the anemia, the hemoglobin levels increase, which improves the tissue oxygenation and may result in reduced VEGF production. VEGF when produced in lower quantities, there is a lower stimulus for neovascularization and thereby reduces the likelihood to develop retinopathy or to progress to severe grades of retinopathy [17,18]. Based on the above observations, it can be concluded that a diabetic individual should be investigated for complete blood count and fundoscopy at least twice a year. Anemia, when detected earlier and treated at the earliest, can prevent the onset of retinopathy and also delay the progression if a patient already has diabetic ret inopathy. Diabetic retinopathy, when detected earlier and treated earlier, can prevent permanent blindness. As mentioned earlier, it is one of the priority eye diseases and should be given due importance for reducing the burden of blindness in the world [19-22].
Conclusion
Anemia is more prevalent among diabetic individuals than the general population in both males and females. Anemia is more prevalent in individuals with diabetes mellitus for a longer duration Anemia is more prevalent in patients of older age group, age more than 70 years. Anemia is an independent risk factor for the development of diabetic retinopathy in diabetic individuals. Diabetic individuals with anemia have a preponderance to develop severe grades of retinopathy. Severe grades of retinopathy are seen in diabetic individuals with anemia. Higher prevalence of retinopathy is seen in anemic individuals with diabetic retinopathy. Diabetic retinopathy is a preventable etiology of blindness. Progression of diabetic retinopathy can be impaired or postponed by the treatment of anemia.
Funding
No funding sources.
Ethical approval: The study was approved by the Institutional Ethics Committee
Conflict of Interest
The authors declare no conflict of interest.
Acknowledgments
The encouragement and support from Bharath University, Chennai, is gratefully acknowledged. For provided the laboratory facilities to carry out the research work.
References
- https://www.who.int/news-room/fact-sheets/detail/diabetes#:~:text=Diabetes%20is%20a%20major%20cause,were%20directly%20caused%20by%20diabetes.
- https://www.who.int/news-room/fact-sheets/detail/blindness-and-visual-impairment
- Adetunji OR, Mani H, Olujohungbe A, et al. Prevalence and characteristics of anaemia in diabetes. Practical Diabetes Int 2008; 25:110-113.
- Singh R, Ramasamy K, Abraham C, et al. Diabetic retinopathy: An update. Indian J Ophthalmol 2008; 56:179.
- https://www.cmcendovellore.org/practical-guide-to-dm/
- Diabetic Retinopathy in Brad Bowling, Kanski’s clinical Ophthalmology: A systematic approach, 8 th ed, Elsevier,2016, PP 520
- Dunst J, Becker A, Lautenschläger C et al, Anemia and elevated systemic levels of vascular endothelial growth factor (VEGF) pubmed.gov, StrahlentherOnkol. 2002 Aug;178(8):436-41.
- M. Rema & R.Pradeepa, Diabetic Retinopathy: An Indian perspective, Indian J Med Res 125, March 2007, pp 297-310
- Sinclair SH, Malamut R, Delvecchio C, et al. Diabetic retinopathy: Treating systemic conditions aggressively can save sight. Cleveland Clin J Med 2005; 72:447-454.
- Rodriguez-Fontal M, Kerrison JB, Alfaro DV, et al. Metabolic control and diabetic retinopathy. Current Diabetes Reviews 2009; 5:3-7.
- Ray D, Mishra M, Ralph S, et al. Association of the VEGF gene with proliferative diabetic retinopathy but not proteinuria in diabetes. US National Library of Medicine, Diabetes 2004; 53:861-864.
- Thomas M, Tsalamandris C, MacIsaac R, et al. Anemia in diabetes: An emerging complication of microvascular disease. Current Diabetes Reviews 2005; 1:107-126.
- Thomas MC, MacIsaac RJ, Tsalamandris C, et al. Unrecognized anemia in patients with diabetes: a cross-sectional survey. Diabetes Care 2003; 26:1164-1169.
- Singh DK, Winocour P, Farrington K. Erythropoietic stress and anemia in diabetes mellitus. Nature Reviews Endocrinol 2009; 5:204.
- Ranil PK, Raman R, Rachepalli SR, et al. Anemia and diabetic retinopathy in Type 2 diabetes mellitus. J Assoc Physicians India 2010; 58:91-94.
- Davis MD, Fisher MR, Gangnon RE, et al. Risk factors for high-risk proliferative diabetic retinopathy and severe visual loss: Early Treatment Diabetic Retinopathy Study Report Investigative Ophthalmology and Visual Science 1998; 39:233-252.
- Shorb SR. Anemia and diabetic retinopathy. Am J Ophthalmol 1985; 100:434-436.
- Friedman E, Brown C, Berman D. Erythropoietin in diabetic macular edema and renal insufficiency. Am J Kidney Dis 1995; 26:202-208.
- Bosman DR, Winkler AS, Marsden JT, et al. Anemia with erythropoietin deficiency occurs early in diabetic nephropathy. Diabetes Care 2001; 24:495-499.
- https://apps.who.int/iris/handle/10665/40707
- Camargo JL, Gross JL. Conditions associated with very low values of glycohaemoglobin measured by an HPLC method. J Clin Pathol 2004; 57:346-349.
- Thankachan P, Muthayya S, Walczyk T, et al. The burden of anemia among women in India. Eur J Clin Nutr 2003; 57:52-60.
Author Info
Kalagara Srirupa Tejasvi and P Manimekalai*
Department Of General Medicine, Sree Balaji Medical College and Hospital, Bharath Institute of Higher Education and Research, Chennai, Tamil Nadu, IndiaCitation: Kalagara Srirupa Tejasvi, P Manimekalai, Anemia in Type 2 Diabetes Mellitus as a Risk Factor for the Presence and Severity of Microvascular Complication-Diabetic Retinopathy, J Res Med Dent Sci, 2021, 9 (4):488-495.
Received: 27-Mar-2021 Accepted: 23-Apr-2021
