Research - (2021) Volume 9, Issue 6
Expression of Immunohistochemical Markers in Papillary Carcinoma Thyroid and Non-Neoplastic Lesions of Thyroid
Gayathri Priyadarshini RS and Ponnuswamy Karkuzhali*
*Correspondence: Ponnuswamy Karkuzhali, Sree Balaji Medical College & Hospital Affiliated to Bharath Institute of Higher Education and Research, India, Email:
Abstract
Thyroid gland nodules and carcinoma is extremely common worldwide and are discovered during routine medical care. The most common carcinoma are well- differentiated papillary carcinoma (80% of all thyroid cancers) and follicular carcinoma (15%). The final diagnosis to distinguish cytologically undetermined tumors is made on surgically removed specimen by histopathological examination in routine Hematoxylin-Eosin (H&E) stained sections. Though in many cases diagnosis is obvious by Cytology alone in a sizeable number the diagnosis is only presumptive. PTC has a papillary architecture and distinctive set of nuclear features, such as ground glass nuclei, nuclear grooves and nuclear pseudoinclusions. None of these findings are individually specific totally for Papillary carcinoma. The present study was designed to study the expression of Immunohistochemical markers like ck19, and galectin- 3 in Papillary carcinoma and Non Neoplastic lesions of thyroid and to see whether the expression pattern may provide a link to the development of papillary carcinoma at a later date. Out of the 122 cases, 30 cases of PTCs and 92 Non Neoplastic lesions were observed. In the present study, we conclude that Galectin-3 maybe a useful specific marker in confirming the diagnosis of PTC.
Keywords
CK19, Galectin-3, Papillary carcinoma, NonNeoplastic lesions, Thyroid, Hematoxylin-eosin
Introduction
Thyroid gland nodules and carcinoma is extremely common worldwide and are discovered during routine medical care. It is estimated that up to 7% of the general population develops clinically palpable thyroid nodules [1,2] and in that 50% are benign like multinodular goitre or thyroiditis. Primary thyroid cancers constitute 1% of all malignant tumors are from all organs. The most common carcinoma is well- differentiated papillary carcinoma (80% of all thyroid cancers) and follicular carcinoma (15%). Rest are only differentiated carcinoma (< 1%) and anaplastic carcinoma (<2%) [3,4]. The diagnosis of thyroid lesions is made preoperatively by cytological criteria using samples obtained by fine-needle aspiration biopsy (FNAB) and FNAB guided by ultrasonography, which has led to the discovery of an infra-clinical reservoir of thyroid nodules in 20 to 76 % of the general population [5-7]. The final diagnosis to distinguish cytologically undetermined tumors is made on surgically removed specimen by histopathological examination in routine Hematoxylin- Eosin (H&E) stained sections. Though in many cases diagnosis is obvious by Cytology alone in a sizeable number the diagnosis is only presumptive.
PTC has a papillary architecture and distinctive set of nuclear features, such as ground glass nuclei, nuclear grooves and nuclear pseudo inclusions. None of these findings are individually specific totally for papillary carcinoma. Moreover in follicular variant of PTC, papillae may not be seen even in histology and the diagnosis is based on the typical nuclear images of PTC. However, it is often difficult to differentiate PTC from follicular variant and other benign papillary hyperplasia of the thyroid gland based on their morphology, causing many intra and inter - observer variability and disagreement among pathologists. Consequently, some tumors are categorized as thyroid tumors of uncertain malignant potential (TTs- UMP) 47. TT UMP is a controversial, newly described entity, referring to a borderline lesion which shows questionable, incomplete PTC-nuclear features and/or capsular and vascular invasion. Thus, there is a need for ancillary studies in arriving at an accurate diagnosis.
Immunohistochemistry plays a complementary role in clarifying this dilemma and for the management and prognosis of the patient. Many studies have shown that immunohistochemistry techniques may provide additional data of markers involved in the genesis and specific characteristics of thyroid lesions. [5,8]. Immunohistochemical markers most supporting the diagnosis of thyroid cancer are CK19, TG, Ki67, Calcitonin, TTF-1, BRAF, RET, HBME- 1, SERPINA I ,TfRl/CD71, FHL 1 which are reported to have a prognostic value for papillary carcinoma. In this study, we have used CK-19 and Galectin-3 in various non-neoplastic thyroid lesions and papillary thyroid carcinoma [8].
Cytokeratin-19 is a low molecular weight cytokeratin m a group of intermediate filaments and is responsible for the structural integrity of epithelial cells [3,5]. It is expressed on neoplastic epithelium and primarily directed for papillary carcinomas. However in some studies focal reactivity has been reported in benign follicular lesions and also areas of degeneration. In papillary carcmoma it has shown diffuse and strong cytoplasmic staining [9]. Galectin-3 (Gal-3) is - galactosidase binding lectin consisting of amino acids and is involved in the process of cell migration, cell growth, neoplastic transformation, adherence and apoptosis [10,11]. Many studies have found that galectin-3 expression is of value in discriminating benign and malignant thyroid nodules, with relatively high sensitivity and specificity, especially in papillary carcinoma. Although it is more prominently expressed in the cytoplasm is also found in the nucleus. The present study was designed to study the expression of Immunohistochemical markers like ck19, and galectin-3 in papillary carcinoma and Non Neoplastic lesions of thyroid and to see whether the expression pattern may provide a link to the development of papillary carcinoma at a later date.
Materials and Methods
Source of data
A total of 122 cases were taken from the Department of Pathology, Sree Balaji Medical College and Hospital, Chennai, between June 2014 and November 2015. We received total thyroidectomy, sub-total thyroidectomy, and right/left hemithroidectomy specimens from the Department of Surgery, Sree Balaji Medical College and Hospital, Chennai. The specimens were received 10% formal saline. Representative sections were taken after gross examinations. The tissue sections were processed by the standard Proponal-Xylol Paraffin Wax schedule. The sections were embedded in Paraffin wax. 4-μm thick sections were taken and primarily stained with H&E in all cases. Additional 3-μm sections were taken in Poly LLysine smeared slides for IHC. These cases consisted of 30 cases of PTCs and 92 Non Neoplastic lesions, including 32 hashimoto's Thyroiditis, 32 nodular hyperplasia, 16 simple follicular hyperplasia and 12 nodular goitre with papillary hyperplasia.
Section cutting and staining technique
The specimens were examined grossly and representative sections were taken and then the routine processing of dehydration, clearing and embedding was done. These sections were cut to 4-μm thickness and all were stained with H&E. and further 3-μm sections were taken in Poly L Lysine smeared slides for IHC.
Staining method
Haematoxylin and eosin (H&E)
• Deparaffinised slides were immersed m first xylene bath for 3 minutes.
• Then transferred to second xylene bath for 2-3 minutes.
• Then immersed in the bath of graded alcohol of 100%, 90%, 70%, and 50% each for 3 minutes.
• Rinsed in running water for 1 minute and then briefly in distilled water.
• Stained with Harris' haematoxylin for 5-10 minutes and rinsed in tap water.
• Differentiated in 1% acid alcohol by dipping 3-4 times and washed in tap water briefly.
• Blueing was done with running tap water. For 10-20 mm.
• Stained with acidified 1% aqueous eosin for 30 seconds.
• Washed in running tap water for 1 minute.
• Dehyrated by passing through 3 baths of absolute alcohol.
• Passed through Xylene for 15-20 seconds.
• Mounted in DPX. (Diestrene dibutyl Pthalate Xylene)
Results: Nuclei-Blue; Cytoplasm - shades of Pink.
Immunohistochemical materials
The immunohistochemical technique was performed on 3-μm thick sections of the paraffin embedded blocks using the Non Biotin Micropolymer based detection system of PathnSitu using Primary antibody galetin 3 from BioSB & CK 19 from PathnSitu . Antigen retrieval was carried out using microwave oven.
IHC staining procedure
• 3μ sections were taken on Poly L Lysine coated slides.
• Slides were incubated at 60°C overnight.
• Deparaffinisation of sections were done using two changes of xylene 15 minutes each.
• Hydrated through graded alcohols, 100% two changes 3 minutes each, 96% two changes 3minutes each.
• Distilled water for 3 minutes.
• Antigen retrieval was done in microwave Oven - Power 1 (100°C) 60 min.
• Primary blockage done using 3% H2O2 in Methanol for 20 minutes
• Washed in distilled water for 3 minutes.
• Washed in two changes of TBST buffer for 5 minutes each.
• Secondary blocking done using 3% BSA for 20 minutes.
• Incubated with primary antibody for 30min at room temperature.
• Washed in two changes of TBST buffer for 5 minutes each.
• Tissue sections covered with Poly Excel Target Binder and incubated for 10min at RT.
• Washed in TBST buffer 3 changes each for 2 minutes.
• Sections covered with Poly Excel Poly HRP and incubated for 10 minutes at RT.
• Washed in TBST buffer 3 changes each for 2 minutes.
• Sections covered with Stunn DAB chromogen solution and incubated for 5 minutes at RT. (Solution preparation- Stunn DAB buffer 1 ml + Stunn DAB chromogen 1 drop-mixed well and stored in the dark. Stable for a week at 2-8°C).
• Washed in two changes of TBST buffer for 5 minutes each.
• Counter stained with Harris’ Haematoxylin for 10 minutes at RT.
• Sections were dehydrated using graded alcohols.
• Clearing was done with 2 changes of Xylene each for 5 minutes.
• Mounted with DPX.
Result: CK-19: Cytoplasm - Brown colour; Galectin 3: Cytoplasm and/or nucleus-Brown colour.
Immunohistochemical evaluation
The following staining patterns were considered positive: Cytoplasmic and/or membrane expression of CKl 9 and Gal-3. A positive immunoreactivity was considered when at least 10% of the tumor cells stained positively for these antibodies.
The intensity of staining for CK-19 and galectin-3 were scored as follows [12]
• 0-No staining in the area of the lesion.
• 1+ Poor (5-29%) staining in the area of the lesion.
• 2+ Moderate (30-69%) lining in the area of the lesion.
• 3+ Strong (70-100%) staining in the area of the lesion.
Results
The present study includes 122 cases of thyroid masses removed surgically and received in our department over a period of 1 ½ years from June 2014 to November 2015. The specimens were received from the Department of Surgery SBMCH. These 122 cases include 30 (24.6%) cases of Papillary Carcinoma, as we have not included other neoplastic lesions of thyroid, and other nonneoplastic lesions are, 32 (26.2%) cases of Hashimoto's Thyroiditis, 32 (26.2%) cases of Nodular Hyperplasia, 16 (13.1%) cases of Simple follicular hyperplasia & 12 (9.8%) cases Nodular Goitre showing focus of Papillary Hyperplasia of Thyroid.
The diagnosis of PTC is based on True papillae, Psammoma bodies, Dark red colloid, Crowded nuclei, Optically clear ("Orphan Annie") chromatin, Irregular nuclear contours, Nuclear grooves and Intranuclear cytoplasmic inclusions. The diagnosis of HT is based on Sheets of lymphocytes and plasma cells, abundant germinal centres, florid inflammation, Atrophied follicles and Htirthle cell changes. The diagnostic features of nonneoplastic lesions (NH, SFH & NGPH) are Nodules composed of varying sizes of follicles, Cellular nodules epithelium, tightly packed cellular epithelium, Fibrosis around cystic areas, dystrophic calcification and haemorrhage with hemosiderin-laden macrophages and Pseudo papillary & true papillary structures (Sanderson polsters) are seen projecting into the cystic spaces.
We have split the non-neoplastic lesions into 3 categories, simple follicular hyperplasia, nodular hyperplasia and nodular goiter with papillary hyperplasia.
Though this is not a scientific classification, we have framed this classification as Nodular hyperplasia may mimic follicular neoplasia to the unwary and papillary hyperplasia may be erroneously categorized as papillary carcinoma. As our present study is primarily to differentiate Papillary carcinoma thyroid from other lesions of thyroid, separating out papillary hyperplasia into a separate category will give more useful insight rather than clubbing them together with other nontumorous conditions (Table 1).
| Cases | Number | Percentage |
|---|---|---|
| Papillary thyroid carcinoma | 30 | 24.60% |
| Hashimotos thyroiditis | 32 | 26.20% |
| Nodular hyperplasia | 32 | 26.20% |
| Simple follicular hyperplasia | 16 | 13.10% |
| Nodular goiter with papillary hyperplasia | 12 | 9.80% |
| Total | 22 | 100% |
Table 1: Case distribution.
As per literature, PTC is common between the age group of 25-50 years of age.
We had peak incidence at 20- 40 years of age. HT is commonly seen in 45-60 years of age as per literature and in our study the peak incidence is between 20-60 years of age. Other non-neoplastic lesions are known to occur commonly at puberty and young adult life, and our study showed a peak incidence at 20-40 years of age (Table 2). In our study, 23 patients (18.85%) were males and 99 patients (81.14%) were females. Our study showed a female preponderance, with a Male: Female ratio being 1:4 (Table 3).
| Age group | PTC | HT | NH | SFH | NGPH |
|---|---|---|---|---|---|
| Up to 20 | 4 | 4 | 0 | 0 | 0 |
| 21-40 | 26 | 12 | 16 | 12 | 6 |
| 41-60 | 0 | 14 | 14 | 4 | 4 |
| >60 | 0 | 2 | 2 | 0 | 2 |
Table 2: Age distribution.
| Sex | PTC | HT | NH | SFH | NGPH |
|---|---|---|---|---|---|
| Male | 5 | 6 | 5 | 4 | 3 |
| Female | 25 | 26 | 27 | 12 | 9 |
Table 3: Sex distribution.
Immunohistochemistry results
Cytokeratin-19
CK-19 was found to show strong 3+ positivity m all 30 PTC cases, in Hashimoto's Thyroiditis it shows variable degree of expression with 16 cases showing 3+ positivity, 10 cases showing 2+ positivity and 6 cases showing 1+ positivity. But in nodular hyperplasia, this marker shows weak 1+ positivity in 14 cases, 2+ positivity in 10 cases and 3+ positivity in 6 cases, also 2 cases showing negative result. In simple follicular hyperplasia , 10 cases show 2+ positivity, 4 cases show 3+ positivity and 2 cases were found to be negative. Nodular goitre with papillary hyperplasia shows equal distribution of cases, with 4 cases showing in 2+ positivity and 4 cases showing 3+ positivity scores and 4 cases were also found to be negative (Table 4). Thus, Cytokeratin-19 showed hundred percent strong positivity in papillary carcinoma of thyroid, but it also showed varying intensity of scoring in non-neoplastic lesions.
| Ck-19 score | 0 | 1+ | 2+ | 3+ | Total |
|---|---|---|---|---|---|
| PTC | 0 | 0 | 0 | 30 | 30 |
| HT | 0 | 6 | 10 | 16 | 32 |
| NH | 2 | 14 | 10 | 6 | 32 |
| SFH | 2 | 0 | 10 | 4 | 16 |
| NGPH | 4 | 0 | 4 | 4 | 12 |
Table 4: CK-19 score in thyroid lesions.
Galectin-3
Galectin-3 showed strong 2+ positivity in 14 cases and 3+ positivity in 16 cases of papillary carcinoma of thyroid and it was weakly positive with 1+ scored in 2 cases of nodular hyperplasia. All other 30 cases of nodular hyperplasia, 32 cases of Hashimoto' s Thyroiditis, 16 cases of SFH and 12 cases of NGPH were found to be negative (Table 5).
| Galectin- 3 score | 0 | 1+ | 2+ | 3+ | Total |
|---|---|---|---|---|---|
| PTC | 0 | 0 | 14 | 16 | 30 |
| HT | 32 | 0 | 0 | 0 | 32 |
| NH | 30 | 2 | 0 | 0 | 32 |
| SFH | 16 | 0 | 0 | 0 | 16 |
| NGPH | 12 | 0 | 0 | 0 | 12 |
Table 5: Galectin-3 score in thyroid lesions.
Galectin-3 showed hundred percent positive m papillary carcinoma of thyroid, other lesions of hashimoto's thyroiditis showed negativity. Nodular hyperplasia showed mild 1+ positive intensity of staining in 2 cases. Other nonneoplastic cases like simple follicular hyperplasia and nodular goitre with papillary hyperplasia showed negativity.
Overall result
CK-19 was positive in 93.44% cases of total cases found in our study.
Galectin-3 was positive in 26.22% of total number of cases. The comparison of positivity in CK-19 and Gal-3 is done.
Co-Expression of CK-19 & Gal-3 in thyroid lesions
Papillary carcinoma of thyroid
In PTC, CK-19 was uniformly positive in all cases with 3+ score. Galectin-3 was found positive in 100% of PTC with varying degree of expression (2+ and 3+ score) (Table 6).
| Negative | 1+ | 2+ | 3+ | |
|---|---|---|---|---|
| CK-19 | 0 | 0 | 0 | 30 |
| Galectin-3 | 0 | 0 | 14 | 16 |
Table 6: Ck-19 vs. Galectin-3 in PTC.
Hashimotos thyroiditis
HT is known to progress to papillary carcinoma, HT was included in the study to see whether there is any early expression of Galectin-3 pointing towards the possibility of future development of PTC. In HT, CK-19 was positive 1n all cases with varying degree of expression, whereas Galectin-3 was uniformly negative in all cases (Table 7).
| Negative | 1+ | 2+ | 3+ | |
|---|---|---|---|---|
| CK-19 | 0 | 6 | 10 | 16 |
| Galectin-3 | 32 | 0 | 0 | 0 |
Table 7: Ck-19 Vs Galectin-3 in HT.
Nodular hyperplasia
In NH, all cases were negative for Galectin-3 except for two. And CK-19 was positive in varying intensity except two cases, which were found to be negative (Table 8).
| Negative | 1+ | 2+ | 3+ | |
|---|---|---|---|---|
| CK-19 | 2 | 14 | 10 | 6 |
| Galectin-3 | 30 | 2 | 0 | 0 |
Table 8: Ck-19 vs. Galectin-3 in NH.
Simple follicular hyperplasia
In SFH, Galectin-3 was negative in all cases, and CK- 19 showed strong 2+ and 3+ positivity, except in two cases, which were negative (Table 9).
| Negative | 1+ | 2+ | 3+ | |
|---|---|---|---|---|
| CK-19 | 2 | 0 | 10 | 4 |
| Galectin-3 | 16 | 0 | 0 | 0 |
Table 9: Ck-19 vs Galectin-3 in SFH.
Nodular hyperplasia goiter with papillary
Papillary hyperplasia in hyperplastic thyroid lesions may mimic PTC in histopathological sections and so it was included in the study to see whether these markers will help in getting a clear diagnosis in grey area lesions. Papillary hyperplasia also showed complete Galectin-3 negativity and 66.66 % of cases of NGPH showed CK-19 positivity of varying degree (2+ &3+) (Table 10).
| Negative | 1+ | 2+ | 3+ | |
|---|---|---|---|---|
| CK-19 | 4 | 0 | 4 | 4 |
| Galectin-3 | 12 | 0 | 0 | 0 |
Table 10: Ck-19 vs. Galectin-3 in NGPH.
Histopathology is explained in Figures 1 to Figure 31.
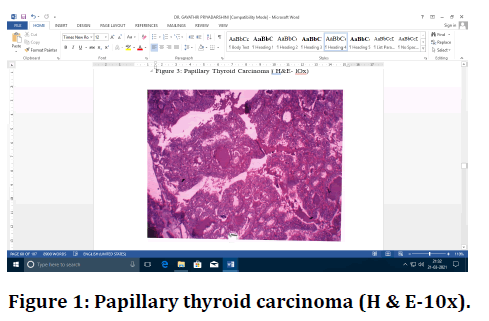
Figure 1. Papillary thyroid carcinoma (H & E-10x).

Figure 2. Papillary carcinoma thyroid (H&E- 10x).
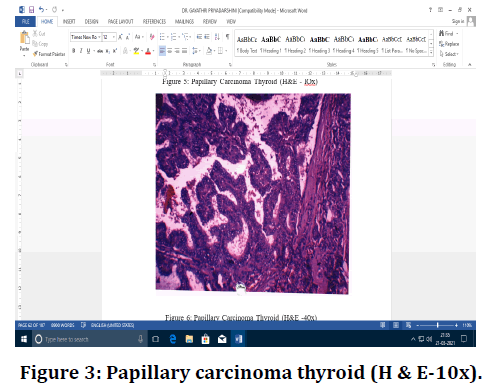
Figure 3. Papillary carcinoma thyroid (H & E-10x).
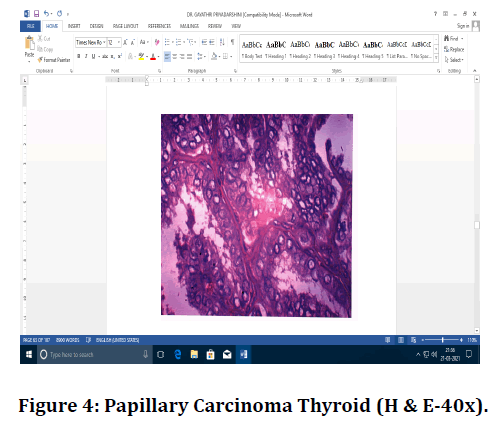
Figure 4. Papillary Carcinoma Thyroid (H & E-40x).
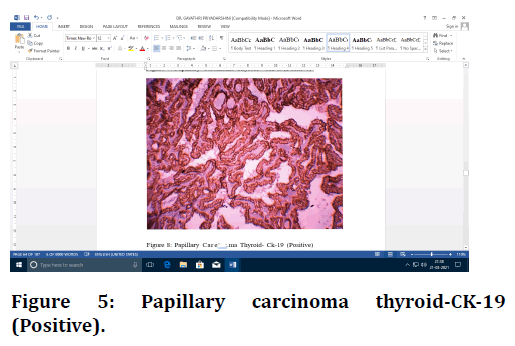
Figure 5. Papillary carcinoma thyroid-CK-19 (Positive).
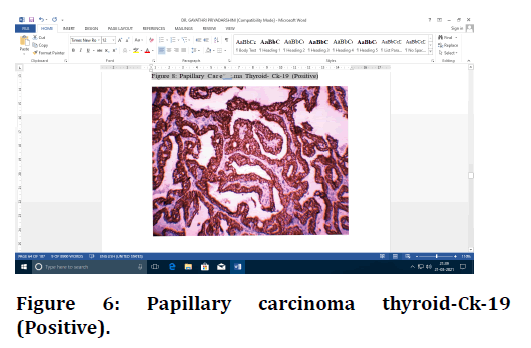
Figure 6. Papillary carcinoma thyroid-Ck-19 (Positive).

Figure 7. Papillary carcinoma thyroid-galectin-3 (Positive).
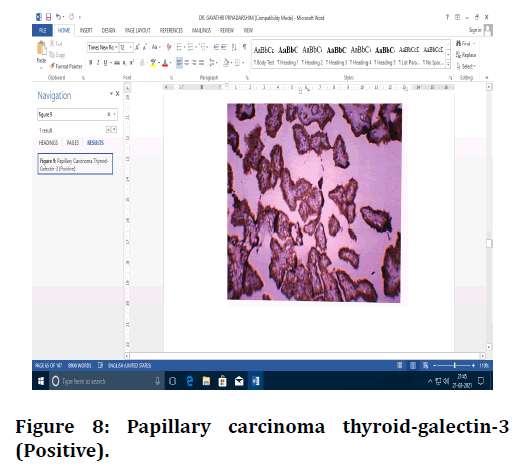
Figure 8. Papillary carcinoma thyroid-galectin-3 (Positive).

Figure 9. Hashimoto's thyroiditis (H & E-10x).
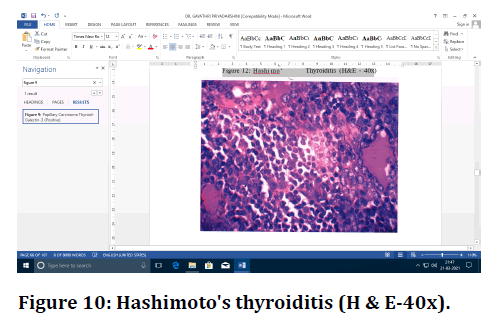
Figure 10. Hashimoto's thyroiditis (H & E-40x).
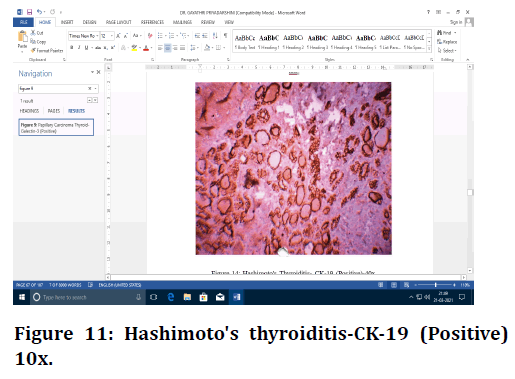
Figure 11. Hashimoto's thyroiditis-CK-19 (Positive) 10x.
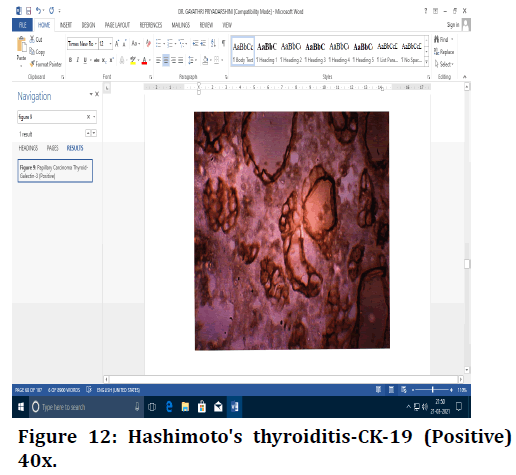
Figure 12. Hashimoto's thyroiditis-CK-19 (Positive) 40x.
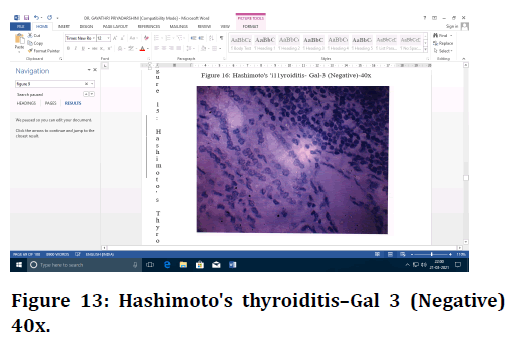
Figure 13. Hashimoto's thyroiditis–Gal 3 (Negative) 40x.
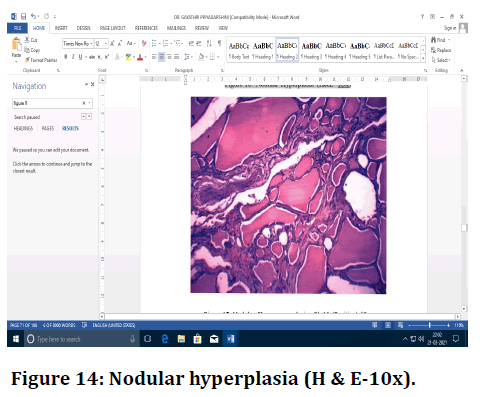
Figure 14. Nodular hyperplasia (H & E-10x).
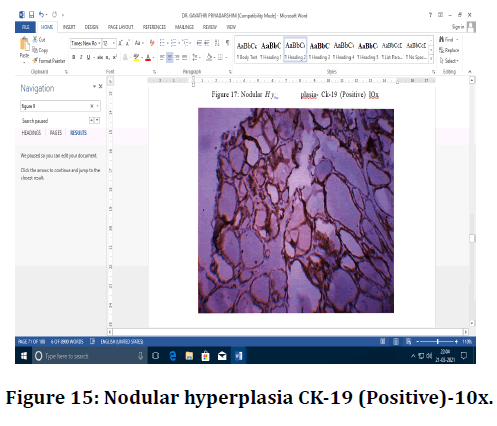
Figure 15. Nodular hyperplasia CK-19 (Positive)-10x.
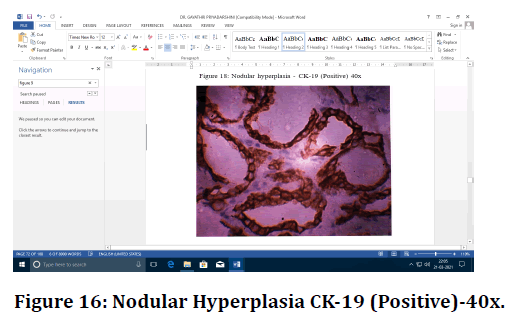
Figure 16. Nodular Hyperplasia CK-19 (Positive)-40x.
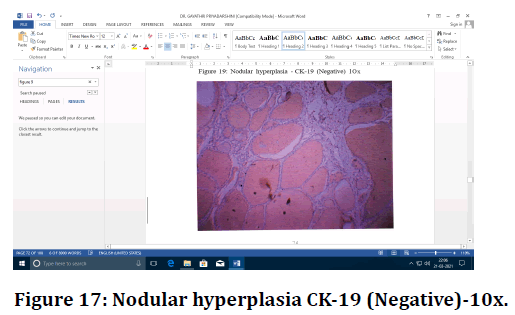
Figure 17. Nodular hyperplasia CK-19 (Negative)-10x.
Figure 18. Nodular hyperplasia CK-19 (Negative)-40x.
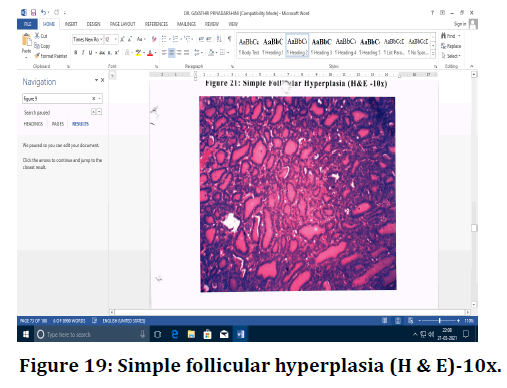
Figure 19. Simple follicular hyperplasia (H & E)-10x.
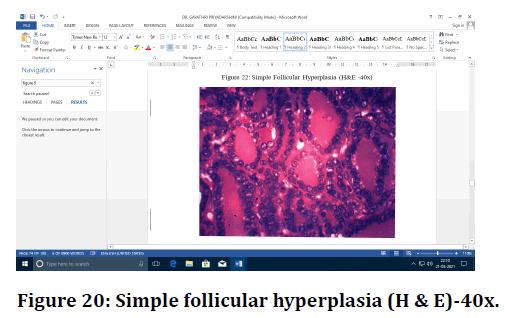
Figure 20. Simple follicular hyperplasia (H & E)-40x.
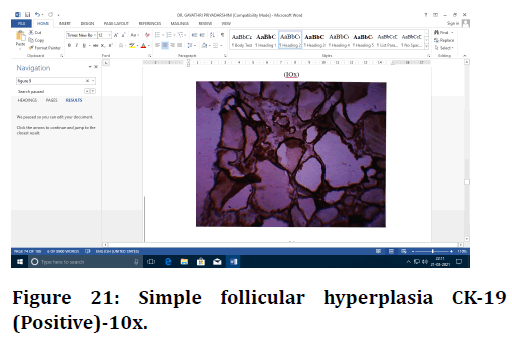
Figure 21. Simple follicular hyperplasia CK-19 (Positive)-10x.
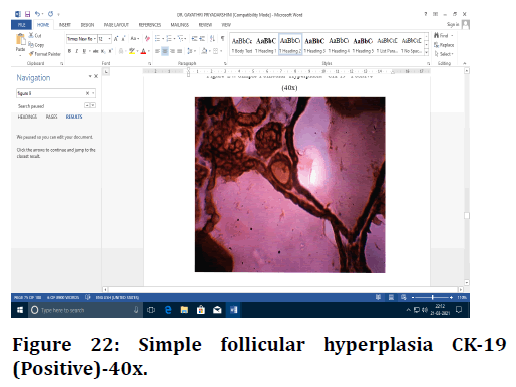
Figure 22. Simple follicular hyperplasia CK-19 (Positive)-40x.
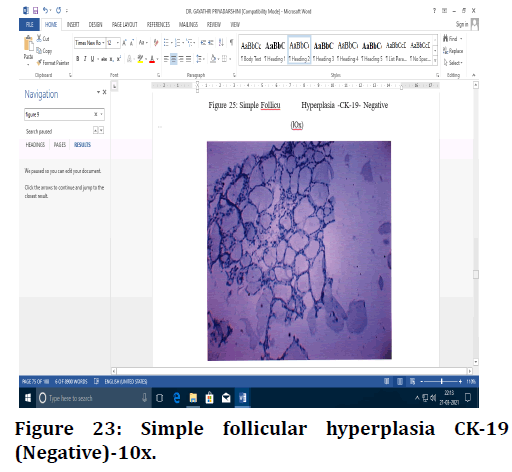
Figure 23. Simple follicular hyperplasia CK-19 (Negative)-10x.
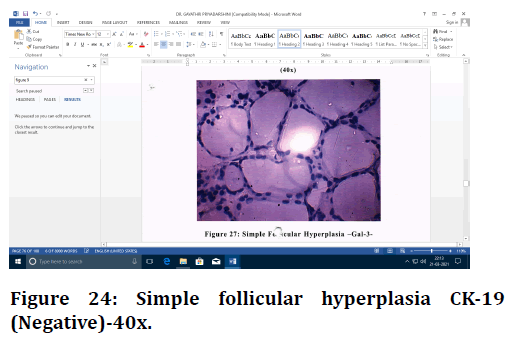
Figure 24. Simple follicular hyperplasia CK-19 (Negative)-40x.
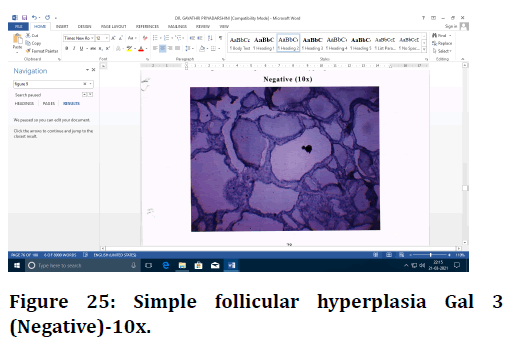
Figure 25. Simple follicular hyperplasia Gal 3 (Negative)-10x.
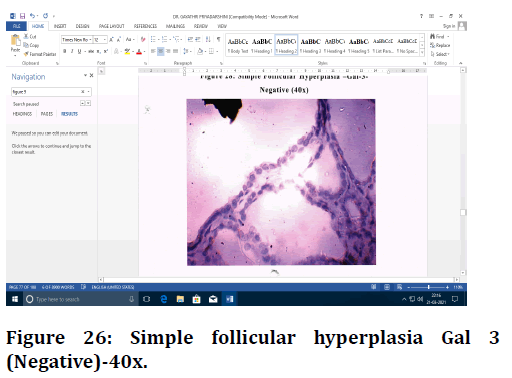
Figure 26. Simple follicular hyperplasia Gal 3 (Negative)-40x.
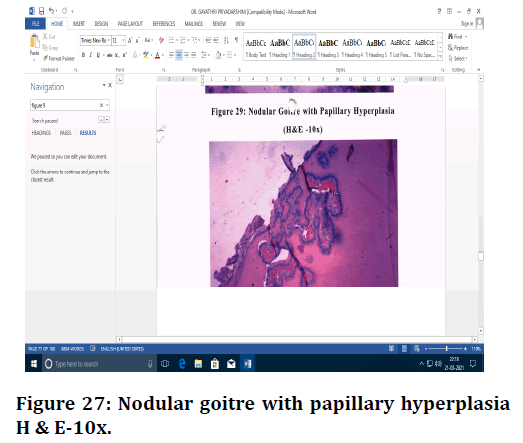
Figure 27. Nodular goitre with papillary hyperplasia H & E-10x.
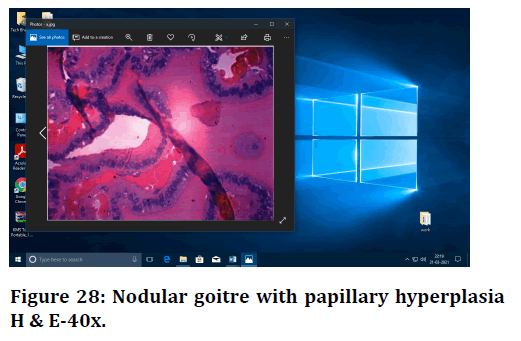
Figure 28. Nodular goitre with papillary hyperplasia H & E-40x.
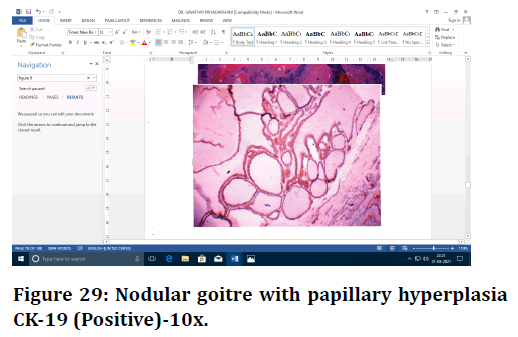
Figure 29. Nodular goitre with papillary hyperplasia CK-19 (Positive)-10x.
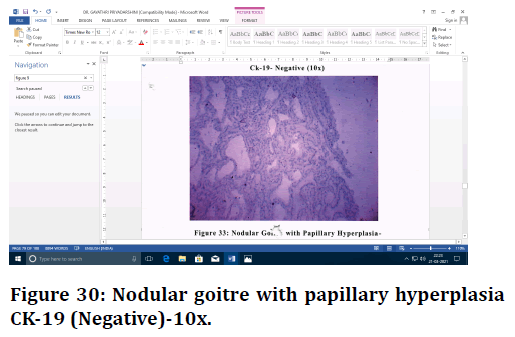
Figure 30. Nodular goitre with papillary hyperplasia CK-19 (Negative)-10x.
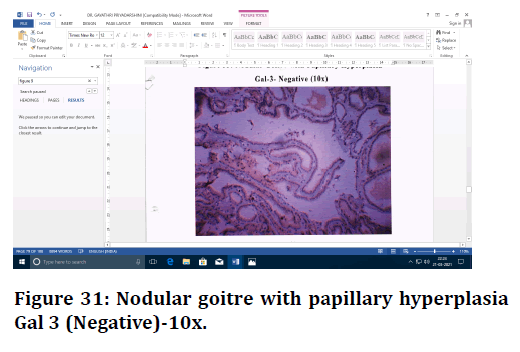
Figure 31. Nodular goitre with papillary hyperplasia Gal 3 (Negative)-10x.
Discussion
Thyroid gland lesions are common worldwide and are discovered during routine medical care. Even though carcinoma of thyroid is not that common, it is the most Gayathri Priyadarshini RS, et al. J Res Med Dent Sci, 2021, 9 (6):439-449 Journal of common malignancy of the endocrine system. A survey sponsored by the World Health Organization (WHO) in 2010 revealed that there are around 44,670 new cases and 1,690 deaths caused by this disease every year [10]. Our study was performed with 122 cases of thyroid lesions received in Department of Pathology, Sree Balaji Medical College and Hospital. These thyroid lesion includes 30 cases of Papillary carcinoma of Thyroid, 32 cases of Hashimoto's Thyroiditis, 32 cases of Nodular hyperplasia, 16 cases of Simple follicular Hyperplasia and 12 cases of Nodular goitre with Papillary Hyperplasia, for which expression of cytokeratin-19 and Galectin-3 were studied.
All 30 cases of PTC in the present study were positive for CK-19 and Galectin-3. CK-19 showed cytoplasmic 3+ positivity in all the 30 cases and Galectin-3 showed cytoplasmic and nucleus positivity ranging from 2+ to 3+ in 14 and 16 cases respectively. This clearly established the fact that CK-19 and Galectin-3 are fully expressed in PTC. Among 92 cases of non-neoplastic lesions, Gal-3 showed negativity in 90 cases and 2 cases of NH showed positivity weakly. CK-19 was positive in all (30) cases of PTC, all (32) cases of HT, 30 out of 32 cases of NH, 14 out of 16 cases of SFH and 8 out of 12 cases of NGPH.
CK-19 In thyroid lesions
In the current study, CK-19 was diffusely and strongly positive in all cases of PTC and positive with variable intensity in most of non-plastic cases. Therefore, CK-l9 staining lacks specificity for PTC, but is a sensitive marker in thyroid lesion. Overexpression of CK-19 favours a diagnosis of PTC if the histomorphology is in agreement. So, Cytokeratin 19 may have added value as part of a panel of immunomarkers in the diagnosis of PTC.
In a study, Miettinen [11] (1997) underscored that poorer staining was seen with CK-19 in most follicular carcinomas, although strong staining was seen in papillary carcinomas and this finding was important in the differential diagnosis. Many studies reported that although diffuse staining with CK-19 was seen in most cases of papillary carcinoma and follicular variant of papillary carcinoma, variable staining of other malignant and benign lesions could provide differential diagnosis. In a study by, Young Joo et al CK-19 has a low specificity with response to diagnosis of malignant thyroid tumors. There was a statistically significant difference between malignant and benign lesions in terms of intensity of staining with CK19, with ck-19 showing +3 staining in 66. 7% of malignant lesions and +3 staining in 41.7% of benign lesions [13]. The present study correlates well with this study showing still greater positivity in PTC (100% compared to 66.7%). Our study indicates that CK - l9 cannot be considered as a marker for malignancy as we did not take up follicular carcinomas in our study, we can't comment on its expression in follicular carcinomas.
Thus, in spite of the immunoreactivity for CK-19 is more frequent and more diffuse in papillary carcinoma, its immunoreactivity in other lesions may limit its utility as a diagnostic marker.
Galectin-3 in thyroid lesions
In a current study, Gal-3 showed positivity in all 30 cases of papillary carcinoma of thyroid. Gal-3 expression is absent in all cases (100%) of non-neoplastic lesions except 2 cases of NH which showed positivity (6.25%). Therefore there is significant difference between nonneoplastic lesions of thyroid and PTC. According to the study by Park et al.Gal-3 positivity is highly in favour of a malignant tumor of thyroid [13]. A vast study by Bartolazzi et al. [14], showed that, the sensitivity and the specificity of galectin-3 immunodetection in the differential diagnosis of benign and malignant thyroid lesions were higher than 99% and 98%, respectively. Also Mataraci Emine Aycan et al. [12] said that cytoplasmic (+) staining of galectin-3 should be taken as a warning and a great number of samples should be made for malignancy criteria. There was a statistically significant difference between malignant and benign lesions in terms of percentage of staining with galectin-3.
In Rajesh Kumar et al. study [6], staining with galectin-3 was present in 70-73% of malignant lesions and 34% of benign lesions. Pisani et al [7] exclusively suggests galectin-3 as a marker of malignancy. Ina study [14,15] it is demonstrated that galectin-3 is highly expressed in benign thyroid lesions and normal thyroid tissue. The discrepancies in the frequency of galectin-3 immunoreactivity in benign lesions may be related to the different antibody detection systems and the cut-off values for positive and negative staining. In the thyroid gland, endogenous biotin is invariably expressed in thyrocytes, mostly in Hurthle cells. Thus, a biotin-based detection system may provide false positive results. It has been suggested that galectin-3 immunodetection may be a useful adjunct in the distinction between benign and malignant thyroid tumors, only if performed in a biotinfree detection system. So we used biotin free detection system to overcome this defect. In a study by Weinberger et al. cytoplasmic and nuclear staining with galectin -3 was seen in malignant neoplasms and no staining with galectin -3 was observed in benign thyroid lesions [16].
Our study is similar to the last study with 100% galactin-3 positivity with minimal (62.5%) positivity in other lesions which could be easily grouped by histomorphology as non PTC. Only one study reports a higher percentage of positivity of galactin -3 in benign thyroid lesions which is not in correlation with our study.
Conclusion
In the present study, Cytokeratin-19 and Galectin-3 Immunohistochemical markers used. It is clear in the present study that CK-19 is expressed in all papillary carcinoma of thyroid and also in non-neoplastic lesion with variable degrees of intensity. Hence, CK-19 lacks the specificity even though it has sensitivity. Galectin-3 is expressed in all Papillary carcinoma of thyroid showing strong positivity, other cases such as Hashimoto's Thyroiditis, simple follicular hyperplasia, nodular goitre and most of nodular hyperplasia shows negativity to this marker. So, it can be concluded from the current study that Galectin-3 maybe a useful specific marker in confirming the diagnosis of PTC.
Funding
No funding sources.
Ethical Approval
The study was approved by the Institutional Ethics Committee.
Conflict of Interest
The authors declare no conflict of interest.
Acknowledegements
The encouragement and support from Bharath University, Chennai is gratefully acknowledged. For provided the laboratory facilities to carry out the research work.
References
- Brown LM. Helicobacter pylori: Epidemiology and routes of transmission. Epidemiol Rev 2000; 22:283–297.
- Anderson J, Anderson JV, Baker LRI, et al. Gastrointestinal disease. In: Kumar and Clark Clinical medicine: 5th ed. Philadelphia: WB Saunders; 2002; 272.
- Minhas KZ, Goraya F, Javid S, et al. Endoscopic and Histopathological evaluation of 306 dyspepsic patients. Pak J Gastroentrol 2003; 17:4-7.
- Kaore NM, Nagdeo NV, Thombare VR. Comparative evaluation of the diagnostic tests for Helicobacter pylori and dietary influence for its acquisition in dyspeptic patients: A rural hospital based study in central India. JCDR 2012; 6:63 6-41.
- Salih BA. Helicobacter pylori infection in developing countries: The burden for how long?. Saudi J Gastroenterol 2009; 15):201-207.
- Kumar R, Bano G, Kapoor B, et al. Clinical profile in H. pylori positive patients in Jammu. Prevalence 2006; 92:34-71.
- Pisani T, Vecchione A, Giovagnoli MR. Galectin-3 immunodetection may improve cytological diagnosis of occult papillary thyroid carcinoma. Anticancer Res 2004; 24:1111-2.
- Mohammadi ASLJ, Dinarvand G, Golchin N, et al. The diagnostic value of gene expression of FHL1 in the differential diagnosis of papillary thyroid carcinoma and benign tumors. J Isfahan Med School 2014; 31:2113-2121.
- Fonseca E, Nesland J, Hoie J, et al. Pattern of expression of intermediate cytokeratin filaments in the thyroid gland: An immunohistochemical study of simple and stratified epithelial-type cytokeratins. Virchows Arch 1997; 430:239–245.
- Jemal A, Siegel R, Xu J, et al. Cancer statistics, 2010. CA Cancer J Clin 2010; 60:277-300.
- Miettinen M, Kovatich AJ, Karkkainen P. Keratin subsets in papillary and follicular thyroid lesions: A paraffin section analysis with diagnostic implications. Virchows Arch 1997; 431:407-413.
- MataracI EA, Özgüven BY, Kabukçuoglu F. Expression of cytokeratin 19, HBME-1 and galectin-3 in neoplastic and nonneoplastic thyroid lesions. Polish J Pathol 2012; 63:58.
- Park YJ, Kwak SH, Kim DC, et al. Diagnostic value of galectin-3, HBME-1, cytokeratin 19, high molecular weight cytokeratin, cyclin D1 and p27(kip1) in the differential diagnosis of thyroid nodules. J Korean Med Sci 2007; 22:621-8.
- Bartolazzi A, Papotti M, Orlandi F. Methodological considerations regarding the use of galectin-3 expression analysis in preoperative evaluation of thyroid nodules. J Clin Endocrinol Metab 2003; 88:950.
- de Matos LL, Del Giglio AB, Matsubayashi CO, et al. Expression of CK-19, galectin-3 and HBME-1 in the differentiation of thyroid lesions: systematic review and diagnostic meta-analysis. Diagnostic Pathol 2012; 7:1.
- Weinberger PM, Adam B, Gourin CG, et al. Association of nuclear, cytoplasmic expression of galectin-3 with β-catenin/wnt-pathway activation in thyroid carcinoma. Arch Otolaryngol Head Neck Surg 2007; 133:503–510.
Author Info
Gayathri Priyadarshini RS and Ponnuswamy Karkuzhali*
Sree Balaji Medical College & Hospital Affiliated to Bharath Institute of Higher Education and Research, IndiaCitation: Gayathri Priyadarshini RS, Ponnuswamy Karkuzhali, Expression of Immunohistochemical Markers in Papillary Carcinoma Thyroid and Non-Neoplastic Lesions of Thyroid , J Res Med Dent Sci, 2021, 9(6): 439-449
Received: 08-May-2021 Accepted: 23-Jun-2021
