Research - (2021) Volume 9, Issue 7
Immediate and Long Term Gingival Marginal Leakage of Two Bioactive Bulk Fill Restorative Materials (A Comparative in vitro Study)
Shelan Sadeq Jumaah, and Abdulla MW Al-Shamma*
*Correspondence: Abdulla MW Al-Shamma, Department of Restorative and Esthetic Dentistry, College of Dentistry, Baghdad University, Iraq, Email:
Abstract
Objective: The aim of this study was to examine Immediate and long term gingival marginal leakage of two bioactive restorative materials in cl II cavity preparations. Materials and methods: Forty eight maxillary first premolar teeth of comparable sizes were collected and allocated into three main groups according to the restorative materials used (n=16): Group (A): Filtek™ Bulk Fill, Group (B): Predicta™bulk bioactive composite, Group (C): ACTIVA™ bioactive composite. Two slot cavities, with standardized dimensions, were prepared in each tooth (3mm buccolingual, 2mm mesiodistal, and mesial gingival margin located 1mm coronal to CEJ and distal gingival margin located 1mm apical to CEJ (.All groups were further divided into two subgroups according to the storage periods: subgroup1 (n=8) the teeth were stored for 24 hours, while in subgroup2 (n=8) for 90 days in SBF as storage medium. The restored samples were thermo cycled and then immersed in methylene blue dye (2%) for 24 hours. Dye diffusion was evaluated by inspect the sectioned samples using digital microscope at 40× magnification. Statistical Analysis: The data were analyzed using Kruskal-Wallis test and Mann-Whitney U-test. Results: The results showed statistically insignificant differences among the restorative materials at 24 hours. However, after 90 days storage the differences were statistically significant, Predicta™ showed lowest microleakage followed by Filtek™ bulk fill while ACTIVA™ showed the highest microleakage. Conclusions: all tested restorative materials showed increase microleakage after aging, dentin margin revealed greater microleakage than enamel.
Keywords
Microleakage, Predicta, Bioactive.
Introduction
In recent decades, esthetic dentistry has made significant progress, subsequent in the development of a variety of restorative materials that have vastly improved. Currently, these materials' performance in terms of marginal sealing integrity and durability is a disturbing factor, particularly in cavities involving the cementum region, where clinical problems are exacerbated [1].
Marginal integrity is essential to increase the longevity of any restoration; the major cause of losing marginal integrity is the Polymerization shrinkage leading to microleakage and thus failure of class II composite restorations. This occurred because monomer molecules are converted into a polymer network, which exchanges Van der Wall’s spaces for covalent bond spaces, creating contraction stresses and microleakage [2].
In spite of the advantages and current enhancements within composite resin for dental requirements, an ambition for the improvement of substitute, smart restorative materials is perceived [3]. Bioactive material is demarcated as one that forms a surface layer of an appetite-like material in contact with saliva or a saliva substitute. These materials deliver minerals that are valuable to the tooth structure that aid and stimulate mineralization and the creation of chemical bonds that benefit to seal the tooth and avoid microleakage [4].
ACTIVA™ bioactive composites (Pulpdent, USA), patented bioactive ionic resin, patented rubberized resin, and bioactive ionomer glass are the main components of ACTIVA™. Bioactive ionic resin contains water with high release and recharge of calcium, phosphate, and fluoride ions. ACTIVA™ bioactive composite mimics the physical and chemical properties of natural teeth by combining the strength and esthetics of composites with the benefits of glass ionomer [5].
A rather recent improvement is Predicta™ bioactive Bulk materials (Parkell, USA), it’s bioactive that stimulate mineral apatite formation and remineralization at the material-tooth interface by releasing calcium and phosphate ions as claimed by manufacturer instruction.
Many question are raised regarding the ability of these bioactive materials, owing to their assumed bioactive properties, to improve marginal adaptation and prevent or reduce marginal leakage when compared to available bulk composite restoration materials. This study is performed in an attempt to answer some of such questions. the aim of this study was to measure and compare the microleakage of two bioactive restorative materials (Predicta™ and ACTIVA™) with standardized cl II slot preparation at two storage periods (24 hours, and 90 days). The null hypothesis was that there were no significant differences between three restorative materials (Predicta™, ACTIVA™ and Filtek™ Bulk Fill restorative materials) regarding gingival marginal leakage at different storage periods (24 hours, and 90 days).
Materials and Methods
Forty eight maxillary sound first premolar teeth with comparable sizes, extracted for orthodontic purpose were included in this study according to a protocol that has been accepted by The Research Ethics Committee of the College of Dentistry, University of Baghdad (no. 228520). The teeth were cleaned and preserved in thymol solution (0.1%) for 2 days to prevent bacterial and fungal growth [6]. After that the samples allocated into three main groups according to the restorative materials used (n=16): group A: (control group) Filtek™ Bulk Fill, group B: Predicta™ bulk bioactive composite, group C: ACTIVA™ bioactive composite.
Cavity preparation
A dental manikin (Maxilla) was used to mimic the clinical situation during restoration placement. each tooth received two standardized Class II proximal box cavities (on mesial surface located 1mm coronal to CEJ while on distal surfaces located 1mm apical to CEJ with mesiodistal width: 2 mm, buccolingual width: 3 mm) were prepared using parallel sided diamond fissure bur of 1.2 mm diameter (Komet, Germany) at high-speed with air/water spray. To standardize cavity preparation, a modified dental surveyor was used. To preserve the cutting efficiency, each new bur was used to prepare four cavities and then discarded [7]. After cavity preparation, all the dimensions were checked using a digital vernier.
Restorative procedure
For each group, the restorative techniques were performed following the company’s instructions of their restorative material. Thus in group A: the cavities received etching ,bonding and restoration with Filtek bulk fill™ (3M,USA), in group B: the cavities received etching ,bonding and restoration with Predicta™ bioactive bulk fill (Parkell, USA) and group C: the cavities received etching only and restoration with ACTIVA™ bioactive bulk fill (Pulpdent, USA). Etching step was performed using phosphoric acid 37 %( super etch) placed for 15 sec and then washed and dried with gentle air. In groups (A and B) drops of Universal adhesive bond was spreading in the mixing well, and a disposable bond brush was used to apply the adhesive to the full cavity, rubbed for 20 seconds.
Subsequently, a calm stream of air was dedicated over the adhesive for about 5 seconds until complete vaporization of the solvent agent, a LED light (Elipar™ Deep Cure-L LED Curing Light) was used for curing the adhesive for 10 seconds according to the manufacturer's instructions.
Each prepared tooth was secured by sectional matrix band to establish the proper proximal anatomic contour. On the mesial surface (enamel), one increment of 4 mm in thickness was inserted, and on the distal surface, two horizontal increments were inserted (dentin). Each bulk fill composite restorations were irradiated for 20 seconds from the occlusal, buccal, and palatal surfaces, and then finished and polished using the EVE twist system.
Thermo cycling
The samples in each subgroup 2 (90 days) storage period were subjected to 500 thermal cycles between 5° and 55°C with a dwell period of 30 sec in an effort to induce the temperature changes that occur in the oral cavity [8]. After that all samples were stored in an incubator for (24hours) in subgroup 1 and (90 days) in subgroup 2 in simulated body fluid.
Microleakage test
The root apices were sealed with sticky wax and the entire tooth surface was coated with two coats of nail varnish except 1 mm cavosurface margin around the restoration.
The specimens were soaked in a 2%methylene blue dye solution for 24 hours at 37â?? before being rinsed thoroughly to eliminate extra dye. The samples were fixed in self-curing epoxy resin (Henkel polybit, UAE) and allowed to set for 24 hours.
Then one section longitudinally was made in restoration from mesial margin to distal margin to obtain two similar dental fragment by using XP sectioning saw with diamond abrasive blade 0.03mm. The sectioned samples were examined under a digital microscope (Dino-Lite capture 2.0, version 1.3.6., Taiwan) at (40X) magnification (Figure 1).
Figure 1: Microleakage scores, (A) Score 0, (B) Score 1, (C) Score 2, (D) Score 3.
Results
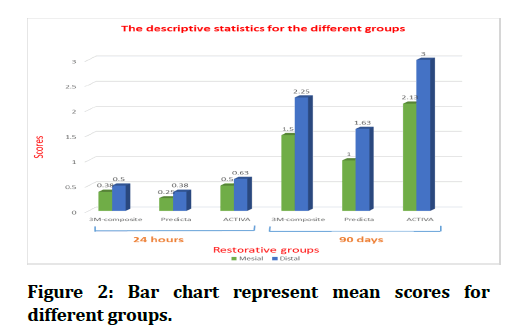
Collected data were analyzed using SPSS (Statistical Package for the Social Science) (version 21). Descriptive statistics which include Statistical tables and graphical presentation by (Bar-Charts) and Arithmetic mean, Standard deviation (SD), Minimum value and Maximum value of the present study are shown in (Table 1 and Figure 2). Inferential statistics which comprise: the Kruskal–Wallis test was used to differentiate between nonparametric data from more than two different groups, while the Mann–Whitney U test was used to compare nonparametric data from two different groups. A p-value of < 0.05 was used to determine statistical significance.
Table 1: Descriptive statistics for the different groups.
| N | Minimum | Maximum | Mean | Standard Deviation | |
|---|---|---|---|---|---|
| A1-M | 8 | 0 | 1 | 0.38 | 0.518 |
| A1-D | 8 | 0 | 1 | 0.5 | 0.535 |
| B1-M | 8 | 0 | 1 | 0.25 | 0.463 |
| B1-D | 8 | 0 | 1 | 0.38 | 0.518 |
| C1-M | 8 | 0 | 1 | 0.5 | 0.535 |
| C1-D | 8 | 0 | 1 | 0.63 | 0.518 |
| A2-M | 8 | 1 | 2 | 1.5 | 0.535 |
| A2-D | 8 | 2 | 3 | 2.25 | 0.463 |
| B2-M | 8 | 0 | 2 | 1 | 0.756 |
| B2-D | 8 | 1 | 3 | 1.63 | 0.744 |
| C2-M | 8 | 1 | 3 | 2.13 | 0.641 |
| C2-D | 8 | 3 | 3 | 3 | 0 |
Abbreviation: M: Mesial gingival margin. D: Distal gingival margin
Figure 2: Bar chart represent mean scores for different groups.
Kruskal-Wallis test was used in the present study showed statistically insignificant differences in the mean microleakage scores between the restorative groups at 24h on both mesial and distal margins. However, at 90d storage the differences were statistically significant in the mean microleakage scores on mesial margin (p<0.05) and highly significant on the distal margin among the restorative groups (P=0.01) (Table 2).For intragroup comparison between mesial and distal margins, the result revealed insignificant difference at 24h storage period among all groups manifested with Mann–Whitney U test. However, after 90d storage the distal cavity (dentin) resulted in a statistical significant increase in microleakage scores related to mesial cavity(enamel )in Filtek bulk fill™ (significant)and ACTIVA™ (highly significant),although no difference was noticed for Predicta™ group (Table 3). The result displayed highly significant difference in all restorative groups between two storage periods (24h and 90d) on the mesial and distal margins manifested with Mann– Whitney U test (Table 4).
Table 2: Kruskal-Wallis test for comparison among different materials.
| Storage | Margin | Groups | Mean Rank | p-value | Significance |
|---|---|---|---|---|---|
| 24 Hours |
Mesial (coronal to CEJ) |
A1 | 12.5 | 0.6 | NS |
| B1 | 11 | ||||
| C1 | 14 | ||||
| Distal (apical to CEJ) |
A1 | 12.5 | 0.619 | NS | |
| B1 | 11 | ||||
| C1 | 14 | ||||
| 90 Days |
Mesial (coronal to CEJ) |
A2 | 12 | 0.017 | S |
| B2 | 8.13 | ||||
| C2 | 17.38 | ||||
| Distal (apical to CEJ) |
A2 | 11.5 | 0.001 | HS | |
| B2 | 7 | ||||
| C2 | 19 |
Table 3: Mann-Whitney U test for comparison between mesial and distal leakage for each material.
|
Groups |
Margins |
Mean Rank |
p-value |
Significance |
|
|---|---|---|---|---|---|
| 24 Hours |
A1 | Mesial | 8 | 0.626 | NS |
| Distal | 9 | ||||
| B1 | Mesial | 8 | 0.602 | NS | |
| Distal | 9 | ||||
| C1 | Mesial | 8 | 0.626 | NS | |
| Distal | 9 | ||||
| 90 Days |
A2 | Mesial | 6 | 0.015 | S |
| Distal | 11 | ||||
| B2 | Mesial | 6.88 | 0.138 | NS | |
| Distal | 10.13 | ||||
| C2 | Mesial | 5.5 | 0.003 | HS | |
| Distal | 11.5 |
Abbreviation: NS: Non-significant, S: Significant, HS: Highly significant
Table 4: Mann-Whitney U test for comparison of the leakage of 24 hours and 90 days aging for each material.
| Groups | Storage periods | Mean Rank | p-value | Significance | |
|---|---|---|---|---|---|
| Mesial (coronal to CEJ) |
A | 24 hours | 5.25 | 0.003 | HS |
| 90 days | 11.75 | ||||
| B | 24 hours | 6.25 | 0.037 | S | |
| 90 days | 10.75 | ||||
| C | 24 hours | 4.75 | 0.001 | HS | |
| 90 days | 12.25 | ||||
| Distal (apical to CEJ) |
A | 24 hours | 4.5 | 0.000 | HS |
| 90 days | 12.5 | ||||
| B | 24 hours | 5.25 | 0.005 | HS | |
| 90 days | 11.75 | ||||
| C | 24 hours | 4.5 | 0.000 | HS | |
| 90 days | 12.5 |
Discussion
Microleakage at the tooth structure–material interface has been related to whole restorations [9]. Microleakage is defined as the “...clinically undetectable passage of bacteria, fluids, molecules, or ions between a cavity wall and the restorative material applied to it.”
A variety of factors can contribute to microleakage. These factors include, but are not limited to the material's physicochemical properties, the polymerization process, and the outline and form of the cavity preparation. Microleakage may also be influenced by operator (technique) variables such as material manipulation, insertion procedures, isolation limits, and adherence to the fundamental standards of dental adhesive and composite resin technology [10].
Based on the findings of the study, the null hypothesis which stated that marginal microleakage was unaffected by restoration type at different storage times was accepted. At 24 hours, there were no significant differences between the three restorative materials. This result in agreement with Khosravi et al. [11] who found that water storage (24 hours) had insignificant effect on gingival microleakage of class II cavities restored with composite resins. Results of the present study are supported by Cannavo et al. [12] who found that the marginal seal of Activa bioactive was at equivalence with the Filtek™ Supreme Ultra, SonicFill™, TetricEvoCeram® composites.
The reasons for low microleakage at 24hrs may be due to the restorations' flowability in (ACTIVA™ and Predicta™), which allows for better wetting along cavity walls, enhancing dental restorations' adaptation to cavity walls, also Filtek bulk fill™ was used with a single-bond universal adhesive system containing 10 methacryloxydecyl-phosphate (MDP) which is responsible for forming a good micromechanical interlocking bond between the adhesive and the dentin [13]. Furthermore during this storage period there was no enough time to give significant difference between all restorative groups.
However after artificial aging for 90 days, the microleakage scores for all tested restorative materials increased significantly. This result may be due to the effect of aging and thermocycling which has been proved to be the most effective factors in increasing the microleakage process. Since restorative materials have a higher thermal expansion coefficient than dental tissue, thermal stresses are produced frequently at the toothrestoration interface. These stresses can cause cracks to form in the bonding region [14]. This is supported by Jaffer et al. [15] who observed that thermo cycling leads to a contraction/expansion stress combined with an increase in chemical degradation.
Furthermore, incomplete penetration of collagen fibers by the dental adhesive exposes the fibers to MMPs' collagen lytic action, which can be activated by low pH values during dentin etching. As a result, the hybrid layer degrades, the bond strength deteriorates over time, and the composite restoration fails [16].
According to the results, ACTIVA™ showed highest microleakage followed by Filtek bulk fill™ and Predicta™ scheduled lowest microleakage.
Predicta™ bioactive composite, revealed the lowest microleakage after 90d storage which may be due to releasing calcium and phosphate ions that may be stimulate mineral apatite formation and remineralization at the material-tooth interface. Such bioactivity is known in the field to equate to stronger bonds between the restoration and tooth and sealing of margins against microleakage. In addition Predicta™ was used with Parkell® Universal dental adhesive that uses a unique blend of 4-methacryloyloxyethy trimellitate anhydride (4-META) and methacryloyloxydecyl dihydrogen phosphate (MDP) monomers that may enhance surface penetration and promote strong, long-lasting dental bonds.
Such bioactivity supported with in vitro study performed by Luong et al. (2020), who found that during simulated body fluid storage, the newly developed predicta dentin desensitizer demonstrated effective dentinal tubule sealing ability and stimulated mineral crystal growth over dentin and into the tubules [17].
The result in agreements with McCabe et al. and Hamdy et al. [18,19] they demonstrated that bioactive materials can precipitate an appetite-like substance on their surface when immersed in physiological body fluid for a period of time, in addition to enhancing remineralization by adding minerals to tooth structure, such as calcium aluminates, they are effective in decreasing matrix metalloproteinase formation, thereby reducing collagen degradation, and they are provided by mineral saturation, which protects the tooth structure from the harmful effects of all acids.
The highest microleakage after 90 days aging recorded by ACTIVA™. Its bioactive material that can reseal its marginal interface with mineral crystal growth that provide greater safety and efficacy against secondary caries, and prevention of bacterial access to dentinal tubules and ultimately the pulp itself [4].
This may be because ACTIVA's coefficient of thermal expansion differs from that of the tooth structure. Differences in polymerization shrinkage and coefficient of thermal expansion that occurred in the ACTIVA™ structure as a result of rising resin content to 44.6 % [20].
Furthermore, ACTIVA™ was used without bonding agent that may influence the marginal integrity and increased microleakage. However, due to clinical evidence of this material's lack of self-adhesive properties, the most recent ACTIVA™ directions for use now prescribe the use of a dental adhesive for clinical placement [21].
The results in agreement with and Kaushik et al. [22], who utilize microleakage as a means of assessing marginal integrity and cavity seal. In this previous study, substantially higher dye penetration was perceived when no etching and bonding were used with ACTIVA™.
The results in contrast with study performed by Amaireh et al. [23] who concluded that microleakage of ACTIVA™ without an adhesive agent and with an intermediate adhesive, was comparable to that observed with composites.
In spite of their findings, in this study it is assumed that mineral deposition on the surface of ACTIVA™ might be weak and poorly crystalline. This assumption is supported by Nourmohammadi et al. who noticed poorly crystalline carbonate apatite on the entire resin modified glass ionomers cement soaked in SBF solution [24].
Abdulla and Majeed, (2020) found through their SEM study that after immersion in SBF, there were some calcium phosphate deposits on ACTIVA™ surface, as well as a small increase in the density of Ca+2 and PO43– through EDX, and this accused to the chemical affinity of silanol and carboxyl groups for forming apatite nuclei resulted in primary heterogeneous calcium phosphate nucleation [25].
Filtek bulk fill™ showed less microleakage compared to ACTIVA™ which may due to its chemical composition which is mainly based on UDMA that have a higher molecular weight , that decreased the overall polymerization shrinkage and thus decreased the interfacial stresses and the microleakage [26]. Moreover, Filtek bulk fill™ was combined with a single-bond universal adhesive system containing MDP, which is responsible for forming a good micromechanical interlocking bond between the adhesive and the dentin [13].
For intra group comparison, result of the current study showed no significant differences between mesial margin (enamel) and distal margin (dentin) at 24h storage in all studied groups. These results were in accordance with previous findings that aimed at RMGI and ACTIVA™ hybridization in enamel and dentin and how it improved the resin interaction with tooth minerals, resulting in a strong resin–hydroxy apatite complex and a positive marginal seal in enamel and dentin [27, 28].
However, after 90d storage the microleakage scores for both mesial and distal margins increased significantly compared to 24h scores and this may be due to same reasons discussed previously (coefficient of thermal expansion and thermo cycling, interface hydrolysis). Dentin margin revealed highest microleakage compared to enamel in all studied restorative materials. These findings are supported by the findings of Benetti et al. [29] who observed large gaps in dentin margins when a bulk-fill composite resin was used compared to enamel. This may be due to the adhesive's higher bond strength to etched enamel compared to etched dentin resulting in greater resistance to thermal stress at the enamel margin. Another reason for enamel's lower microleakage relative to dentin may be the use of an etch-and-rinse adhesive system of 37% phosphoric acid etching. This etching technique is very effective in increasing enamel bond strength compared to self-etch technique [30].
Other factors which increased microleakage at the dentinal margin as compared to enamel margin may be the organic content of dentin substrate and outward movement of dentinal tubular fluids and due to the complex and changing physiologic processes involved with dentin substructure. When the distance between the light-curing tip and the resin surface is >2 mm, the light intensity is significantly reduced. This might prevent adequate polymerization of resin composite materials. As a result, the composite resin conversion degree at the dentinal margin is expected to be lower than at the enamel margin, which received the curing light directly.
One of the limitation of this in vitro study is the Predicta™ bioactive composite, its novel material and there is limited information about physical, and chemical properties so it need further investigations.
Conclusion
Within the limitations of the present study, the conclusions include:
At 24 hours there were no differences in microleakage among the restorative materials.
After 3 months storage all tested restorative materials showed increase microleakage, the ACTIVA™ had the most microleakage, followed by Filtek bulk fill™ and Predicta™, which had the least microleakage.
In intragroup comparisons, each groups had more leakage at the apical (dentin) margin than the coronal (enamel) margin. Aging had significant impact on microleakage.
Author Info
Shelan Sadeq Jumaah, and Abdulla MW Al-Shamma*
Department of Restorative and Esthetic Dentistry, College of Dentistry, Baghdad University, IraqCitation: Shelan Sadeq Jumaah, Abdulla MW Al-Shamma,Immediate and Long Term Gingival Marginal Leakage of Two Bioactive Bulk Fill Restorative Materials (A Comparative in vitro Study), J Res Med Dent Sci, 2021, 9(7): 120-126
Received: 05-Jun-2021 Accepted: 08-Jul-2021